Atrial myxoma, Hemorrhagic stroke; Intracranial aneurysm
Myxomas have been implicated in embolic etiologies of ischemic and have also been noted to have a role in intracranial aneurysmal formation with subsequent bleeding [1,2]. We present a case of a 57 year old woman who presents with a right frontal parietal intraparenchymal hemorrhage. Further stroke workup was never pursued as the etiology was of her bleed was thought to be secondary to hypertension. A few years later, she presented back with symptoms concerning for Transient Ischemic Attack (TIA). A Transthoracic Echocardiogram (TTE) done as part of TIA work uprevealed a large left atrial myxoma.
A 57-year-old right-handed female with a past medical history of hypertension presented with acute onset left sided weakness. Her vital signs were significant for a blood pressure of 160/71 with all other vitals stable. She had a right sided gaze preference, left facial palsy and 3/5 strength and diminished sensation to pin prick over the left upper and lower extremity. Non-contrasted CT of the head showed a large 5.6 cm right frontal parietal intraparenchymal hemorrhage (Figure 1A). A CT angiogram (CTA) head and neck was negative for a malformation related to the bleed, but showedan incidental small 25 x 13 mm aneurysm at the right A1-A2 junction (Figures 1B and 1C). The patient was admitted to the neurological intensive care unit (NICU) where she was quickly transitioned to an oral anti-hypertensive. Further imaging such as MRI brain and a TTE were not pursued as hemorrhage was thought to be secondary to hypertension. A year later, the patient returned with a 5 minute episode of dysarthria, worsened left-sided weakness concerning for a TIA. Her work up included a MRI brain with and without contrast which did not show signs of acute stroke and magnetic resonance angiogram (MRA) of head and neck showed a stable A1 aneurysm. TTE showed amass on the left atrium attached to the intra-atrial septum. A transesophageal echocardiogram (TEE) confirmed a large heterogeneous mass seen adherent to inter-atrial septum within the left atrium. Cardiac MRI further classified a 1.5 cm x 1.5 cm X 1.0 cm mass attached to the interatrial septum (Figure 1D). The patient underwent cardiothoracic surgery for removal of her atrial myxoma. Follow-up TTE showed no evidence of atrial myxoma recurrence.
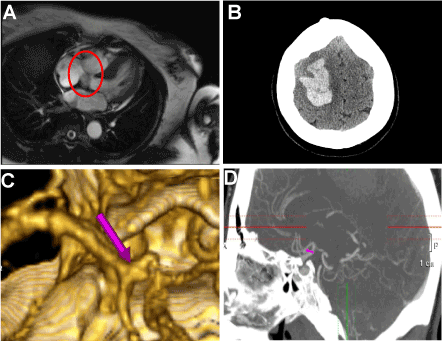
Figure 1. A.Non-contrasted CT of the head showed a large 5.6 cm right frontal parietal intraparenchymal hemorrhage, B. CTA head and neck 25 x 13 mm broad-based aneurysm at the right A1-A2 junction, C. Reconstructions of the CTA head and neck showing 25 x 13 mm broad-based aneurysm at the right A1-A2 junction, D. 1.5 cm x 1.5 cm X 1.0 cm left atrial myxoma as seen on cardiac MRI
Atrial myxomas are the etiology of stroke or TIA in 1 in 250 adults. The annual incidence is 0.5 per million with 75% of cases occurring in the left atrium [2,3]. Thereis a 2:1 female preponderance, and the age at onset is usually between 30 and 60 years. Neurologic manifestations of atrial myxomas have been reported in 25-45% of cases [2,3]. Emboli are most often myxomatous but may also arise from thrombus adherent to the tumor and have been reported to cause cerebral infarction in 27% of cases [4]. Less common are presentations of intracranial aneurysms secondary to myxomas3-5. Several possible mechanisms of aneurysm formation have been proposed. One method is that of tumor cells infiltrating cerebral vessels via vasa vasorum destroying the architecture of arterial walls. Alternatively, perivascular damage may be due to vascular occlusion by tumor material with subsequent scarring and pseudoaneurysm formation. Another proposed mechanism is the direct transendothelial invasion of tumor cells into the arterial wall causing destruction of its architecture and subsequent aneurysm dilatation [5]. TTE remains the most frequently used imaging method to detect atrial myxomas. TTE has a sensitivity of around 90% in the detection with TEE offering higher sensitivity [5]. Additionally, the presentation of atrial myxoma often comprises of an elevation of ESR and C-reactive protein, hyperglobulinemia and anemia. Constitutional symptoms such as fever, night sweats and weight loss can be due to interleukin-6, produced by the myxoma. All of these symptoms were absent in our patient [6].
Our patient initially presented with a large cortical hemorrhage in the setting of slightly elevated blood pressures. The etiology of her hemorrhage was not identified at time of discharge and most likely was secondary to a friable aneurysm due to intracranial involvement of her tumor or due to a hemorrhagic conversion of an ischemic infarction with cardio-embolic etiology. This case highlights the importance of a thorough stroke work up of all cryptogenic strokes in any young person with a high cortical infarction. Without obvious physical findings on admission, this is a diagnosis that would have otherwise been missed if it were not for a TTE as part of the stroke work up.
- Colucci V, Alberti A, Bonacina E, Gordini V (1995) Papillary fibroelastoma of the mitral valve. A rare cause of embolic events. Tex Heart Inst J 22: 327–331. [Crossref]
- O'Rourke F, Dean N, Mourandian MS, Akhtar N, Shuaib A (2003) Atrial myxoma as a cause of stroke: case report and discussion. Can Med Assoc J 169: 1049–1051. [Crossref]
- Herbst M, Wattjes MP, Urbach H, Inhetvin-Hutter C, Becker D, et al. (2005) Cerebral embolism from left atrial myxoma leading to cerebral and retinal aneurysms: A case report. AM J Neuroradiol 26: 666-669. [Crossref]
- De Marco A, La Tessa G, De Falco A, De Falco FA, Merola A, et al. (2010) Multiple Cerebral Aneurysms Associated with Atrial Myxoma. Neuroradiology Journal 23: 62-68.
- Markel, ML, Waller BF, Armstrong WF (1987) Cardiac myxoma: A review. Medicine 66: 114-125. [Crossref]
- Kirschner LS, Carney JA, Pack SD, Taymans SE, Giatzakis C, et al. (2000) Mutations of the gene encoding the protein kinase type I-alpha regulatory subunit in patients with the Carney complex. Nat Genet 26: 89-92. [Crossref]
Editorial Information
Editor-in-Chief
Massimo Fioranelli
2021 Copyright OAT. All rights reserv
Guglielmo Marconi University
Article Type
Case Report
Publication history
Received: January 01, 2015
Accepted: January 12, 2015
Published: January 16, 2015
Copyright
©2015 Billakota S. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation
Billakota S (2015) Atrial myxoma leading to intraparenchymal hemorrhage 1: DOI: 10.15761/JIC.1000106
Corresponding author
Santoshi Billakota
Duke University Medical Center, PO Box 2905, 27710, Durham, NC, USA, Tel: (310) 699-1921; Fax: (919) 684-0131.

