Ochronosis is an uncommon condition characterized by the deposition of an ochre-colored pigment within the skin, cartilage, and other connective tissues [1]. There are two types of ochronosis: endogenous and exogenous. Alkaptonuria (endogenous ochronosis), is a rare metabolic disorder characterized by a triad of homogentisic aciduria, cutaneous hyperpigmentation, and arthropathy. It is due to the deficiency of the enzyme homogentisic acid oxidase, which catalyzes the conversion of homogentisic acid to maleylacetoacetic acid in the catabolism of tyrosine. Exogenous ochronosis is a cutaneous disorder characterized by the bluish-black hyperpigmentation on the skin due to chronic use of chemical preparation and oral administration of a specific medication [2]. We present an overlap case of exogenous and endogenous ochronosis.
Coined by Virchow in 1866, ochronosis refers to the brownish-yellow or ochre-colored accumulation of pigment found in the connective tissue of patients with the disease. There are two types of ochronosis: endogenous and exogenous [3].
Endogenous ochronosis or alkaptonuria is an autosomal recessive disease caused by a deficiency of the enzyme homogentisic oxidase, which oxidizes homogentisic acid, a metabolite of tyrosine and phenylalanine. The deficiency of this enzyme leads to an accumulation of homogentisic acid in the connective tissues [4]. This metabolic disorder has recently been attributed to the gene locus (AKU) on chromosome 4q234 [5]. The patient is usually asymptomatic until the third and fourth decade of life [4]. Clinically, endogenous ochronosis presents with a triad of homogentisic aciduria, arthropathy, and cutaneous hyperpigmentation. The most disabling manifestation of disease is ochronotic arthropathy, which affects mainly the large joints and the intervertebral disks. The hands and feet are usually spared or rarely affected [6]. Bluish to brownish hyperpigmentation on the medial and lateral aspect of sclera (Osler’s sign) are also observed in patients but their vision is not impaired [7]. Bluish pigmentation of the auricles where the skin is thin, with discoloration of the cartilage is also a significant clinical feature [6,8].
On the other hand, exogenous ochronosis manifests as asymptomatic hyperpigmentation in photo-exposed region [9]. It occurs over sites of chemical contact, like the osseous surfaces of the zygomatic areas of the face, side and back of the neck as well as the extensor aspects of extremities, usually in a symmetrical pattern. The lesions are grey brown or blue-blackmacules and usually with hyperchromic, pinpoint, caviar-like papules [9]. Exogenous ochronosis can be secondary to the topical application of hydroquinone, resorcinol, or oral administration of antimalarials or mercury [5].
Ochronosis secondary to hydroquinone was first described in 1975 by Findlay [10] in patients who regularly applied this topical bleaching agent for a long period. It occurs almost exclusively in patients with a high phototype (Fitzpatrick's classification IV to VI).
A 68-year- old female with skin Fitzpatrick phototype IV, presented with a history of facial hyperpigmentation. She self-medicated with a commercialized solution containing hydroquinone 2% and tretinoin 0.025% which was available over the counter, for 5 years without using a sunscreen. She also started having mild pain and stiffness on the lower back for three years. She was then treated for osteoarthritis and degenerative lumbar osteoarthropathy.
On physical examination, patient had blue-black patches with caviar-like, hyperchromic, pinpoint papules with round depigmented macules (confetti-like depigmentation), symmetrically, distributed over the frontal, zygomatic, mandibular, upper lip, chin, and lateral regions of face (Figure 1a and 1b). Obvious bluish-brown pigmentation on sclerae (Figure 2a), ears (Figure 2b), and nails (Figure 2c) were confirmed.
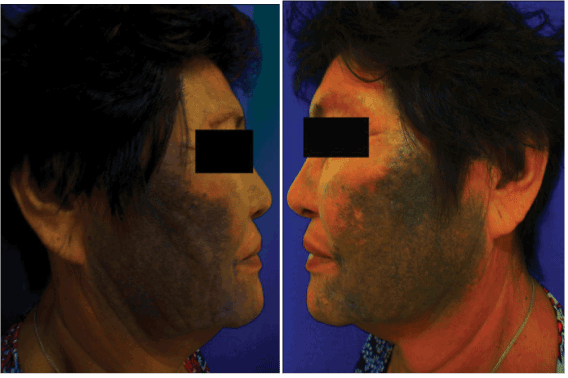
Figure 1a-b. Fuliginous blue-black patches with caviar-like, hyperchromic, pinpoint papules with round depigmented macules (confetti-like depigmentation), symmetrical, and distributed over the zygomatic, mandibular regions, lateral region of face.
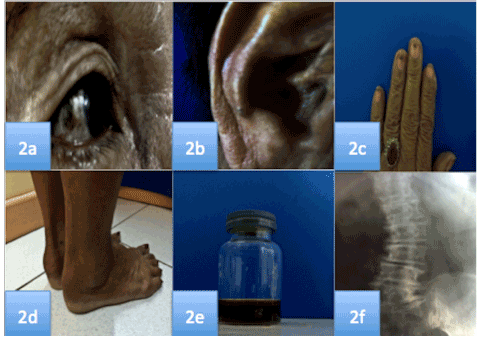
Figure 2a-f. Pigmentation on the sclerae, conchae, and nails, bilateral thickening of Achilles tendon, black urine on Ferric chloride test, and lumbosacral x-ray abnormalities
Bilateral thickening of Achilles tendon was also observed (Figure 2d). Urine had normal color, however through ferric chloride test it turned black (Figure 2e).
Radiological evaluation of lumbosacral joint revealed axial osteoarticular degeneration, calcification on intervertebral disk and mild scoliosis (Figure 2f).
Routine laboratory analysis including complete blood count, urinalysis, BUN/creatinine, liver function test, uric acid, and electrocardiography were within normal range. Histologic examination of skin specimen from her left cheek revealed the presence of ochronotic ‘banana shaped’ pigments in the dermis confirming the diagnosis of exogenous ochronosis (Figure 3).
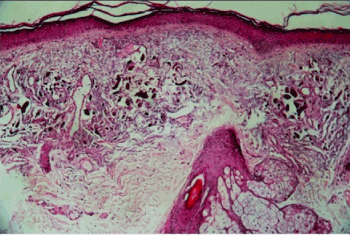
Figure 3. Histopathology of the lesion, showing atrophy of epidermis, and brownish-yellow (ochre) “banana shaped” fibers in the papillary dermis (H&E stain 10x)
Patient was treated with oral antioxidant containing glutathione, N-acetyl cysteine, and high dose vitamin C, glycolic soap, tretinoin cream 0.1%, Rumex cream, sunscreen, chemical peel using trichloroacetic acid once a month, restricted protein and phenylalanine diet with partial improvement of the lesions.
Our patient presented with Fitzpatrick skin phototype type IV, similar to the cases of exogenous ochronosis described in the literature. Exogenous ochronosis presents as a bluish black discoloration on the site of application of hydroquinone. With respect to the concentrations of hydroquinone applied, the patient used relatively low concentrations (2%) but for a long time (5 years). This is similar to the study by Gandhi where ochronosis was observed in chronic use of hydroquinone and not necessarily due to high concentrations [11].
Prolonged use of hydroquinone, without sunscreen could accelerate the appearance of ochronosis.
On further examination, the patient was noted to have endogenous ochronosis as well. She presented with the triad of cutaneous hyperpigmentation, arthropathy and homogentisic urine. Osler's sign as illustrated in our patient is due to deposition of ochronotic pigment in the sclera. There were also noted pigmentation on the ears and nails.
Histopathology revealed many ochre pigments in the dermis. Patient also experienced non-radiating low back pain for three years, described as mild scoliosis with calcification on the lumbosacral joint on radiograph. Aside from these, there are also tangible thickening of both Achilles tendons. Furthermore, positive result in urine ferric chloride test was observed.
In this case, what was initially thought of as a classic case of exogenous ochonosis secondary to hydroquinone, turned out to be an overlap case of exogenous and endogenous ochronosis.
2021 Copyright OAT. All rights reserv
Various theories explain the pathogenesis of ochronosis. In the exogenous type, the pattern and areas of predilection show similarity to that of photoallergic dermatitis, and the strong absorption by hydroquinone of the sunburn waveband of ultraviolet light (peak 293nm) has led many to believe that exogenous ochronosis is photoactivated [10]. In endogenous ochronosis, there is accumulation of homogentisic acid that polymerizes to form ochre pigments in the papillary dermis [12].
On histopathology, early lesions show basophilic and swollen collagen fibers before developing the characteristic yellow ochronotic morphology. Fully developed lesions of ochronosis are characterized by focal collections of yellow-brown (ochre), ‘banana-shaped’ fiber in the superficial dermis, often coexisting with mild solar elastosis [12]. Occasionally, colloid milium and/or granulomas are detected [13].
Various treatments have been used for exogenous ochronosis, but usually produce mediocre results [10,11]. Satisfactory results have been described with retinoic acid, cryotherapy, CO2 laser Q-switched ruby laser [14], Q-switched alexandrine 755 laser, and Nd Yag 1064 laser [15].
On the other hand, the following treatment options are recommended for endogenous ochronosis: restricting protein intake, with low phenylalanine and tyrosine in diet. Long-term ascorbic acid can reduce late sequences by diminishing serum concentration of the metabolite benzoquinone acetic acid. It inhibits oxidation and polymeration. The drug 2 –nitro-4-Trifuor-methyl benzoyl-1, 3-cyclohexanedione (NTBC), which is a potent inhibitor of p-hydroxyphenyl-pyruvate dioxygenase to catalyze the formation of homogentisic acid can be beneficial. It inhibits oxide oxidation and polymerization [5]. Systemic steroids may be given in arthritic patients. In advanced cases surgical operation for disk herniation and valve replacement may be warranted [8].
Cutaneous bluish-brown hyperpigmentation is the hallmark of exogenous ochronosis. But clinicians must also look for involvement of other vital organs. Patients with endogenous ochronosis usually present with typical signs and symptoms, such as homogentisic aciduria, cutaneous hyperpigmentation, and arthropathy. However they are often treated under a wrong diagnosis. Early diagnosis and appropriate symptomatic treatment may significantly improve quality of life of the patient.
- Ribas J, Schettini AP, Cavalcante Mde S (2010) Exogenous ochronosis hydroquinone induced: a report of four cases. An Bras Dermatol 85: 699-703. [Crossref]
- Charlín R, Barcaui CB, Kac BK, Soares DB, Rabello-Fonseca R, et al. (2008) Hydroquinone-induced exogenous ochronosis: a report of four cases and usefulness of dermoscopy. Int J Dermatol 47: 19-23. [Crossref]
- Goldsmith LA, Katz SI, Gilchrest BA, Paller AS, Leffell DJ, et al. (2012) Fitzpatrick 8thEd: Dermatology in General Medicine. McGraw Hill Company, USA 822
- Odabas AR, Karakuzu A, Selcuk Y, Erdem T, Cetinkaya R (2001) Alkaptonuria: a case report. J Dermatol 28: 158-160. [Crossref]
- Ibrahim FA, El-din Selim MM, Al-Ansari H (2002) Ochronosis. J Dermatol Venereol 9: 1-5.
- Ngcelwane MV, Mandaba M, Bam TQ (2013) Multiple tendon ruptures in ochronosis: case report and review of prophylactic therapy. SA Orthop J 12: 55-57.
- Masood Q, Hassan I, Majid I, Khan D, Manzooi S, et al. (2003) Dexamethasone cyclophosphamide pulse therapy in pemphigus: experience in Kashmir valley. Indian J Dermatol Venereol Leprol 69: 97-99. [Crossref]
- Lubics A, Schneider I, Sebök B, Havass Z (2000) Extensive bluish gray skin pigmentation and severe arthropathy. Endogenous ochronosis (alkaptonuria). Arch Dermatol 136: 548-549, 551-2. [Crossref]
- Kramer KE, Lopez A, Stefanato CM, Phillips TJ (2000) Exogenous ochronosis. J Am Acad Dermatol 42: 869-871. [Crossref]
- Levin CY, Maibach H (2001) Exogenous ochronosis. An update on clinical features, causative agents and treatment options. Am J Clin Dermatol 2: 213-217. [Crossref]
- Gandhi V, Verma P, Naik G (2012) Exogenous ochronosis After Prolonged Use of Topical Hydroquinone (2%) in a 50-Year-Old Indian Female. Indian J Dermatol 57: 394-395. [Crossref]
- Charlín R, Barcaui CB, Kac BK, Soares DB, Rabello-Fonseca R, et al. (2008) Hydroquinone-induced exogenous ochronosis: a report of four cases and usefulness of dermoscopy. Int J Dermatol 47: 19-23. [Crossref]
- Jain A, Pai SB, Shenoi SD (2013) Exogenous ochronosis. Indian J Dermatol Venereol Leprol 79: 522-523. [Crossref]
- Bellew SG, Alster TS (2004) Treatment of exogenous ochronosis with a Q-switched alexandrite (755 nm) laser. Dermatol Surg 30: 555-558. [Crossref]
- Kanechorn-Na-Ayuthaya P, Niumphradit N, Aunhachoke K, Nakakes A, Sittiwangkul R, et al. (2013) Effect of combination of 1064 nm Q-switched Nd:YAG and fractional carbon dioxide lasers for treating exogenous ochronosis. J Cosmet Laser Ther 15: 42-45. [Crossref]



