Abstract
Background
Venous thromboembolism is a leading cause of morbidity and mortality in the United States. Accurate and timely diagnosis may be confounded by its nonspecific clinical presentation. Wells Criteria is a reliable screening tool with high sensitivity; however, recent data suggest that D-dimer is increasingly used as a primary screening test. While the sensitivity of D-dimer is comparable to Wells Criteria, it lacks specificity and positive predictive value, thus resulting in increased hospitalizations, further testing and accompanied costs and complications.
Aims
Our goal was to assess utilization of D-dimer and Wells criteria in the emergency department as a screening tool for venous thromboembolism.
Materials and methods
This is a retrospective chart review conducted at a community hospital. All patients who had a D-dimer test at presentation to the emergency department were included in the study. Fishcer’s Exact was used for statistical analysis.
Results
Contrary to current recommendations, 15 patients (9.3%) with low Wells Score and negative D-dimer had further imaging studies. Increased use of imaging resulted in an increased cost of care and possible exposure to the procedure related complications.
Conclusions
A review of the literature and our study both conclude that adherence to current guidelines for evaluation of venous thromboembolism is less than optimal. Adherence to the guidelines in evaluating these patients would have several beneficial outcomes including reducing the need for further imaging studies thus reducing healthcare costs and decreasing possible patient complications associated with such procedures.
Key words
pulmonary embolism, D-dimer, deep venous thrombosis, wells criteria
Introduction
Venous thromboembolism (VTE) is a major cause of morbidity and mortality in United States [1]. It’s prevalence is one patient per thousand people per year and out of 100,000 hospital admissions, 239 are from VTE [2-4]. Current recommendations, based on cumulative data, suggest using a two-step approach of utilizing Wells Criteria (Figure 1) for its high sensitivity and D-dimer for its high negative predictive value to triage patients quickly and effectively in the emergency department [5,6]. However, D-dimer use along with pulmonary computed tomographic angiography has increased for varying reasons [7-9]. D-dimer has very low positive predictive value and can be elevated in many other conditions, thus is not specific to VTE [7-12]. The purpose of this retrospective study was to evaluate the use of guidelines for diagnosis of VTE in a community based emergency department.
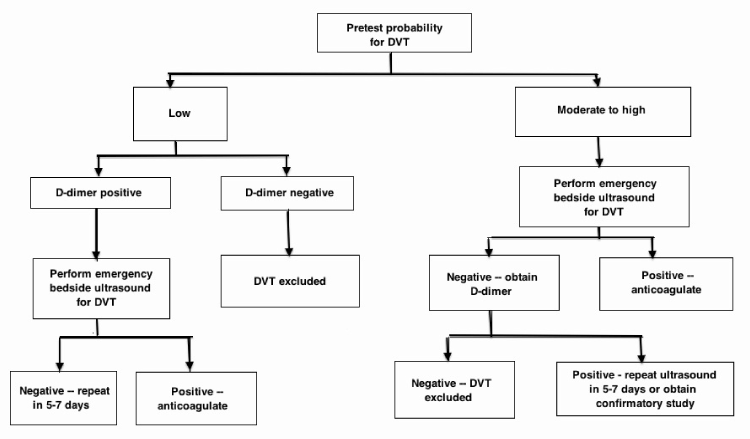
Figure 1. Deep Venous Thrombosis (DVT) Clinical Algorithm Suggested by the American College of Emergency Physicians (ACEP) [6].
Methods
This is an institutional review board approved retrospective study. All patients who presented to our emergency department during January through June 2010 were considered for inclusion in the study. Patient charts were reviewed by a team of physicians for D-dimer level, documentation for Wells Score, lower extremity venous ultrasound, computed tomography chest pulmonary embolism protocol, ventilation quotient scan and demographic information. If there was no Wells Score documentation in the chart, a score was calculated using available information in the medical record. Zero was assigned for any missing data needed to calculate Wells Score. Statistical analysis was done using Fisher’s Exact Test.
Results
During the study period 10,651 patients presented to our emergency department, 346 (3.2%) had symptoms suggestive of VTE and were screened using D-dimer testing. Sixteen of the 346 screened (4.6%) had documented thromboembolic events. Average age of the patients was 55.4 years (range of 18-96), 63% of them being females. Table 1 shows detailed demographics of the study population. The average annual rate of venous thromboembolism was 0.23% in hospitalized patients. Wells Score was not documented in any of the patients screened for VTE.
|
Total number of patients (N)
|
346
|
|
Age (years)
|
Range 18-96, average 55.4
|
|
Sex
|
Male - 37%, Female - 63%
|
|
D dimer
|
|
|
<0.51 %
|
170 (49%)
|
|
>0.51 %
|
176 (51%)
|
|
Wells score
|
|
|
Low probability
|
303 (88%)
|
|
Medium probability
|
38 (11%)
|
|
High probability
|
5 (1%)
|
|
Venous thromboembolic events
|
16 (4.6%)
|
|
Deep venous thromboembolism (DVT)
|
3 (.87%)
|
|
Pulmonary embolism (PE)
|
6 (1.7%)
|
|
DVT and PE
|
7 (2.0%)
|
Table 1. Demographics of study population.
A significantly higher percentage of patients with a D-dimer result ≥0.50 mg/dl had a confirmed venous thromboembolism compared to patients with a D-dimer result < 0.50 mg/dl (9% vs. 1%, p-value= 0.0004) (Table 2). Patients with a Wells Score that indicated a high or moderate probability of VTE had a much higher percentage of confirmed VTE than patients with a Wells score that indicated a low probability (20% vs. 18% vs. 2.6%, p=<0.0001) (Table 2). A vast majority, 87.5% (n=303), of the study population had low probability Wells Scores. Among them, 162 had negative D-dimers. Of the 162 patients, 15 (9.3%) had further imaging done (Figure 2)
| |
With VTE
|
Without VTE
|
|
|
D-dimer
|
|
|
|
|
< 0.51
|
1 (1%)
|
169 (99%)
|
p=0.0004
|
|
> 0.51
|
15 (9%)
|
161 (91%)
|
|
|
Wells Criteria
|
|
|
|
|
Low probability
|
8 (2.6%)
|
295 (97.4%)
|
p=<0.0001
|
|
Medium probability
|
7 (18%)
|
31 (82%)
|
|
|
High probability
|
1 (20%)
|
4 (80%)
|
|
Table 2. Analysis of data based on D-dimer and Wells probability score.
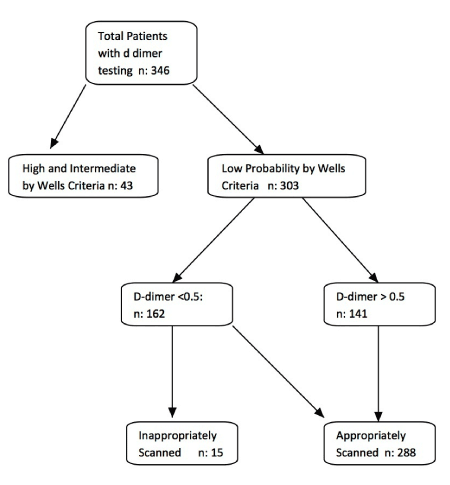
Figure 2. Patient Management Flowchart.
Discussion
VTE is a common condition (1:1,000 in general population) [2]. Pulmonary embolism is a common and potentially lethal disease accounting for more than 250,000 hospitalizations a year in the United States [1]. The incidence of deep venous thrombosis and pulmonary embolism is 20% or less among screened patients [13,14]. A missed diagnosis of VTE can lead to sudden death, chronic cardiopulmonary dysfunction, and impaired quality of life [4,15,16]. However, over testing increases costs and patients are exposed to undue risk with no added benefit. Diagnosing accurately avoids anticoagulation and its associated risk of bleeding in patients without disease [17].
There are multiple clinical prediction rules (in Table 3) available to predict likelihood of VTE [5, 18-20]. Patients are divided into high, moderate or low probability risk categories [4]. If likelihood is high or moderate, patients are scanned with computed tomography chest or lower extremity venous ultrasound directly. However, patients in the low risk group need further testing with D-dimer (Figure 1) to exclude the possibility of thromboembolic disease [6].
|
Test
|
Criteria
|
Points
|
Clinical Probability
|
|
Wells Score [17] for DVT
|
Cancer
|
1
|
Low probability: 0
Intermediate: 1-2
High probability: >=3
|
|
Paralysis or recent plaster cast
|
1
|
|
Bed rest >3days or surgery <4weeks
|
1
|
|
Pain on palpation of deep veins
|
1
|
|
Swelling of entire leg
|
1
|
|
Diameter difference on affected calf >3cm
|
1
|
|
Pitting edema (affected side only)
|
1
|
|
Dilated superficial veins (affected side)
|
1
|
|
Alternative diagnosis at least as possible as DVT
|
-2
|
|
|
|
|
|
|
Wells Score [18] for PE
|
Previous PE or DVT
|
1.5
|
Unlikely: <= 4
Likely: >4
|
|
Heart rate >100 BPM
|
1.5
|
|
Recent surgery or immobilization
|
1.5
|
|
Clinical signs of DVT
|
3
|
|
Alternative diagnosis less likely than PE
|
3
|
|
Hemoptysis
|
1
|
|
Cancer
|
1
|
|
|
|
|
|
|
Revised Geneva Score[19] for PE
|
Age >65years
|
1
|
Low: 0-3
Intermediate: 4-10
High: >=11
|
|
Previous DVT or PE
|
3
|
|
Surgery under general anesthesia or fracture of the lower limbs <1month
|
2
|
|
Active malignancy (solid or hematological malignancy, currently active or considered as cured for <1year
|
2
|
|
Unilateral lower limb pain
|
3
|
|
Hemoptysis
|
2
|
|
Heart rate 75-94 BPM
|
3
|
|
Heart rate >95 BPM
|
5
|
|
Pain lower limb deep vein palpation and unilateral edema
| 2021 Copyright OAT. All rights reserv
4
|
Table 3. Clinical prediction rules available to predict likelihood of venous thromboembolism.
The most commonly used clinical prediction rule is Wells Criteria. Prevalence of deep venous thrombosis based on pretest probability of low, intermediate and high (as estimated by Wells Criteria) is 5%, 15% and 70% respectively [18]. For suspected pulmonary embolism, Wells Score and Revised Geneva Score are also widely accepted as standard measurements of pretest probability [20,21]. Revised Geneva Score is entirely based on clinical variables and thus independent from physician judgment [20]. In our study, the prevalence of venous thromboembolism in patients with low, intermediate and high clinical probability groups, using retrospectively calculated Wells Criteria, was 3%, 18% and 20% respectively, which is different from historical data [18]. Retrospective calculation of the Wells Score most likely underestimated the score, which would explain this difference.
D-dimer testing is done for the exclusion of VTE in low risk patients. The sensitivity of D-dimer in low to medium probability groups (as per Wells Criteria) varies from 94-96% (95 % CI 0.88-1.00) in multiple meta-analyses [10,11]. D-dimer levels below 0.5 mg/dl in low and intermediate clinical probability have a high negative predictive value, essentially ruling out VTE and no further studies are needed [12,22-24]. In our study only one patient (~0.5%) had confirmed VTE with D-dimer less than 0.50 mg/dl and 99% of patients (n=169) with D-dimer <0.50 had no VTE upon further investigations, in line with the previous data.
Testing D-dimer in patients with high clinical probability should not alter further diagnostic pathways [18]. In our study each of the five patients with high probability had D-dimer above 0.50 mg/dl. The post-test probability of pulmonary embolism remains above 3% despite a normal D-dimer, rendering the test futile in this subgroup [13]. D-dimer level above 2 mg/dl was predictive of the presence of pulmonary embolism, independently of the clinical score, with an odds ratio of 6.9 [25].
The fact that none of our patients had documented Wells Scores is not unusual. In a recent survey on clinical prediction rules, 68% of respondents (physicians) reported being familiar with at least one clinical prediction rule for pulmonary embolism [26]. Surveyed physicians also identified reasons for not using the prediction rules [26]. The clinical prediction rules for VTE are grossly underused or under documented and thus diagnostic decisions made were in discordance with the established recommendations [27-29].
In our study fifteen patients with negative D-dimer and low probability Wells Score had further work up done. This is not in line with established guidelines. This resulted in additional imaging studies and associated cost to the healthcare. Imaging cost on average was $1,289 per image based on reported Centers for Medicare and Medicaid Services charges (lower extremity venous doppler: $727, computed tomography chest with contrast: $1,586).
Limitations: Our single center study is limited by its retrospective nature and calculation of Wells Criteria based on chart review, which could have underestimated the actual Wells Score.
Conclusions
Every effort should be made to apply the clinical probability rules for VTE in emergency department patients before testing for D-dimer. This will result in substantial cost savings to the healthcare system. Furthermore, emergency departments will benefit from establishing guidelines and monitoring the use of clinical prediction rules for consistency, similar to other commonly utilized protocols including acute coronary syndrome and stroke.
References
- Goldhaber SZ (1998) Pulmonary embolism. N Engl J Med 339: 93-104. [Crossref]
- Anderson FA Jr, Wheeler HB, Goldberg RJ, Hosmer DW, Patwardhan NA, et al. (1991) A population-based perspective of the hospital incidence and case-fatality rates of deep vein thrombosis and pulmonary embolism. The Worcester DVT Study. Arch Intern Med 151: 933-938. [Crossref]
- Yusuf HR, Tsai J, Atrash HK, Boulet S, Grosse SD (2012) Venous thromboembolism in adult hospitalizations - United States, 2007-2009. CDC Morbidity and Mortality Weekly Report 61: 401-404.
- Silverstein MD, Heit JA, Mohr DN, Petterson TM, O'Fallon WM, et al. (1998) Trends in the incidence of deep vein thrombosis and pulmonary embolism: a 25-year population-based study. Arch Intern Med 158: 585-593. [Crossref]
- Kearon C, Ginsberg JS, Douketis J, Crowther M, Brill-Edwards P, et al. (2001) Management of suspected deep venous thrombosis in outpatients by using clinical assessment and D-dimer testing. Ann Intern Med 135: 108-111. [Crossref]
- Del Rios M, Lewiss R, Saul T, 2014. Focus on: emergency ultrasound for deep vein thrombosis. American College of Emergency Physicians ACEP News.
- Kabrhel C, Matts C, McNamara M, Katz J, Ptak T (2006) A highly sensitive ELISA D-dimer increases testing but not diagnosis of pulmonary embolism. Acad Emerg Med 13: 519-524. [Crossref]
- Ota M, Nakamura M, Yamada N, Yazu T, Ishikura K, et al. (2002) Prognostic significance of early diagnosis in acute pulmonary thromboembolism with circulatory failure. Heart Vessels17: 7-11. [Crossref]
- Studdert DM, Mello MM, Sage WM, DesRoches CM, Peugh J, et al. (2005) Defensive medicine among high-risk specialist physicians in a volatile malpractice environment. JAMA 293: 2609-2617.[Crossref]
- Stein PD, Hull RD, Patel KC, Olson RE, Ghali WA, et al. (2004) D-dimer for the exclusion of acute venous thrombosis and pulmonary embolism: a systematic review. Ann Intern Med 140: 589-602. [Crossref]
- Brown MD, Rowe BH, Reeves MJ, Bermingham JM, Goldhaber SZ (2002) The accuracy of the enzyme-linked immunosorbent assay D-dimer test in the diagnosis of pulmonary embolism: a meta-analysis. Ann Emerg Med 40: 133-144. [Crossref]
- Anoop P, Chappell P, Kulkarni S, Shirley JA (2009) Evaluation of an immunoturbidimetric D-dimer assay and pretest probability score for suspected venous thromboembolism in a district hospital setting. Hematology 14: 305-310. [Crossref]
- Bounameaux H, Perrier A, Righini M (2010) Diagnosis of venous thromboembolism: an update. Vasc Med 15: 399-406. [Crossref]
- Anderson DR, Kovacs MJ, Kovacs G, Stiell I, Mitchell M, et al. (2003) Combined use of clinical assessment and d-dimer to improve the management of patients presenting to the emergency department with suspected deep vein thrombosis (the EDITED Study). J Thromb Haemost 1: 645-651. [Crossref]
- Cushman M, Tsai A, Heckbert SR, et al. (2001) Incidence rates, case fatality, and recurrence rates of deep vein thrombosis and pulmonary embolus: the Longitudinal Investigation of Thromboembolism Etiology (LITE). J Thromb Haemost 86: 2349.
- Murin S, Romano PS, White, RH (2002) Comparison of outcomes after hospitalization for deep venous thrombosis or pulmonary embolism. J Thromb Haemost 88: 407-414. [Crossref]
- Büller HR, Agnelli G, Hull RD, Hyers TM, Prins MH, et al. (2004) Antithrombotic therapy for venous thromboembolic disease: the Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy. Chest 126: 401S-428S. [Crossref]
- Wells PS, Anderson DR, Bormanis J, Guy F, Mitchell M, et al. (1997) Value of assessment of pretest probability of deep-vein thrombosis in clinical management. Lancet 350: 1795-1798. [Crossref]
- Wells PS, Anderson DR, Rodger M, Ginsberg JS, Kearon C, et al. (2000) Derivation of a simple clinical model to categorize patients probability of pulmonary embolism: increasing the models utility with the SimpliRED D-dimer. Thromb Haemost 83: 416-420. [Crossref]
- Le Gal G, Righini M, Roy PM, Sanchez O, Aujesky D, et al. (2006) Prediction of pulmonary embolism in the emergency department: the revised Geneva score. Ann Intern Med 144: 165-171. [Crossref]
- Klok FA, Kruisman E, Spaan J, Nijkeuter M, Righini M, et al. (2008) Comparison of the revised Geneva score with the Wells rule for assessing clinical probability of pulmonary embolism. J Thromb Haemost 6: 40-44. [Crossref]
- Righini M, Perrier A, De Moerloose P, Bounameaux H (2008) D-Dimer for venous thromboembolism diagnosis: 20 years later. J Thromb Haemost 6: 1059-1071. [Crossref]
- Taira T, Taira BR, Carmen M, Chohan J, Singer AJ (2010) Risk of venous thromboembolism in patients with borderline quantitative D-dimer levels. Am J Emerg Med 28: 450-453.[Crossref]
- van Belle, A., Buller, H.R., Huisman, M.V., et al., 2006. For the Christopher Study Writing Group. Effectiveness of managing suspected pulmonary embolism using an algorithm combining clinical probability, D-dimer testing and computed tomography. JAMA 295, p.172e9.
- Bosson JL, Barro C, Satger B, Carpentier PH, Polack B, et al.(2005) Quantitative high D-dimer value is predictive of pulmonary embolism occurrence independently of clinical score in a well-defined low risk factor population. J Thromb Haemost 3: 93-99. [Crossref]
- Runyon MS, Richman PB, Kline JA, Pulmonary Embolism Research Consortium Study Group (2007) Emergency medicine practitioner knowledge and use of decision rules for the evaluation of patients with suspected pulmonary embolism: variations by practice setting and training level. Acad Emerg Med 14: 53-57. [Crossref]
- Lee JA, Zierler BK (2011) The current state of practice in the diagnosis of venous thromboembolism at an academic medical center. Vasc Endovascular Surg 45: 22-27. [Crossref]
- Smith C, Mensah A, Mal S, Worster A (2008) Is pretest probability assessment on emergency department patients with suspected venous thromboembolism documented before SimpliRED D-dimer testing? CJEM 10: 519-523.
- Roy PM, Meyer G, Vielle B, Le Gall C, Verschuren F, et al. (2006) Appropriateness of diagnostic management and outcomes of suspected pulmonary embolism. Ann Intern Med 144: 157-164. [Crossref]


