Abstract
A 30-year-old male presented with a painful, 4 cm left plantar mass. Excisional biopsy revealed a multinodular dermal and subcutaneous neoplasm composed of uniform, basaloid cells at the periphery transitioning to oncocytic, epithelioid cells with focal clear cell change in the central portions of the nodules. Although the tumor showed remarkable similarity to an eccrine poroma and/or dermal duct tumor, no definitive duct differentiation was identified. Immunohistochemically, the tumor cells displayed focal but strong smooth muscle actin expression but were negative for cytokeratin (AE1/AE3) and S-100 protein. The immunophenotype confirmed the diagnosis of glomus tumor with oncocytic change. Re-excision showed no residual neoplasm. Oncocytic change in glomus tumors is a recognized but uncommon finding that often results in diagnostic confusion with cutaneous adnexal neoplasms. Clear cell change is an exceedingly rare finding in glomus tumor that has not been reported in the literature to our knowledge. The presence of these features in our case caused diagnostic confusion with an adnexal neoplasm. However, the absence of ducts prompted immunohistochemistry to differentiate between glomus tumor and an adnexal neoplasm. This case demonstrates that glomus tumors can show both oncocytic and clear cell change and bear a striking resemblance to cutaneous adnexal tumors.
Key words
glomus tumor, adnexal, eccrine, oncocytic, clear cell, hidradenoma, dermal duct, sweat gland
Introduction
Glomus tumors, also termed as Popoff tumors or Barre-Masson syndrome, are relatively rare and comprise less than 2% of soft tissue tumors [1-4]. The neoplasms are usually solitary and most commonly occur in the extremities with a predilection for the subungual region of the fingers [5,6]. They commonly produce a triad of symptoms, including pain, which may be paroxysmal, tenderness and temperature sensitivity [6,7]. Most solitary lesions occur in the third to fifth decades of life [8]. A minority of cases can occur in children with about 10% due to a congenital autosomal dominant inheritance pattern. Multiple familial glomus tumors have an autosomal dominant inheritance pattern linked to chromosome 1p21-22 [9].
Histologically, glomus tumors are composed of uniform round cells surrounding variably sized vascular spaces. The normal glomus cell is theorized to be a modified smooth muscle cell based on ultrastructural and immunohistochemical features. Although there are rare cases with atypical features and/or malignant behavior, the majority of glomus tumors are benign [10-12].
Case report
A 30-year-old male presents with a long-standing history of multiple pilar cysts and a painful, 4 cm mass on the left plantar foot that was clinically diagnosed as a cyst. The plantar foot mass was located at the instep-heel junction and restricted his mobility. Excisional biopsy revealed a tan, firm 3.6 x 3 x 1.7 cm circumscribed lesion that extended to within 0.1 cm of the deep and peripheral excision margins.
Histologic examination of the tumor demonstrated large, well-circumscribed nodules of relatively uniform, neoplastic cells involving the dermis and subcutis (Figure 1). The tumor cells exhibited uniform basaloid features at the periphery of the nodules with minimal cytologic atypia with a transition to oncocytic features in the central portion of the tumor nodules (Figure 2). Rare mitotic figures were seen (1 per 50 high power fields), but no atypical mitoses were identified. Additionally, occasional foci of clear to pale cells were present in the tumor (Figures 3-5).
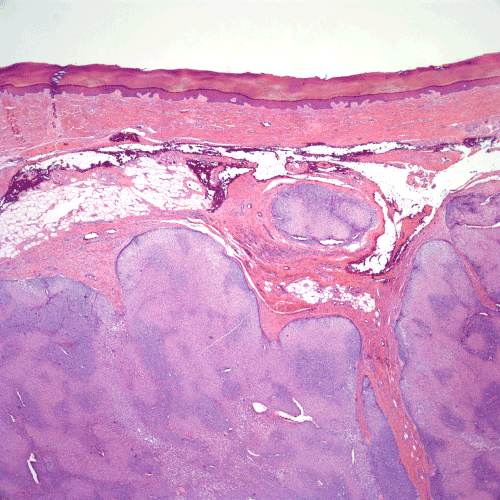
Figure 1. The tumor is composed of large, circumscribed nodules involving the dermis and subcutis of acral skin (H&E stain, 20x magnification).
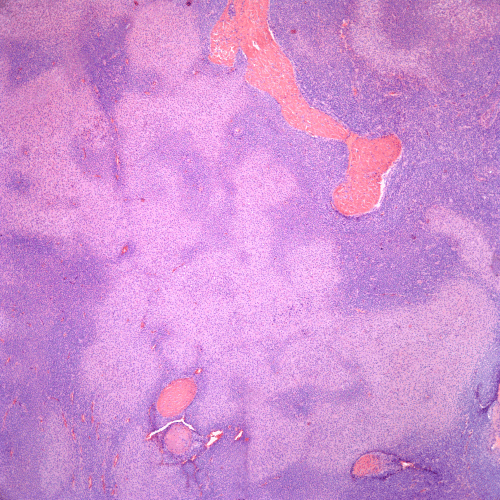
Figure 2. Uniform small round blue tumor cells with minimal cytoplasm are seen at the periphery of the nodules transitioning to central areas with more abundant pale eosinophilic cytoplasm (H&E stain, 40x magnification).
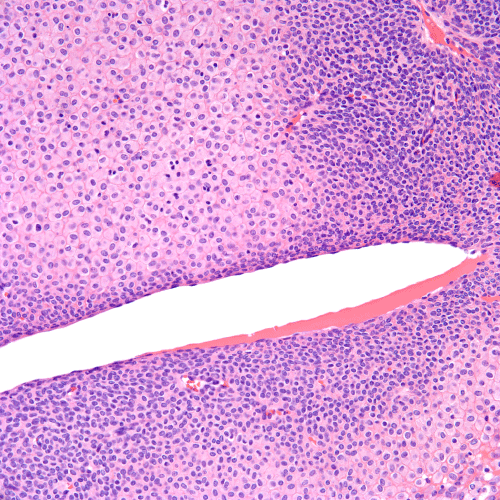
Figure 3. Both types of tumor cells display monotonous bland nuclei with minimal cytologic atypia. Dilated vessels are present in the midst of tumor cell sheets (H&E stain, 200x magnification).
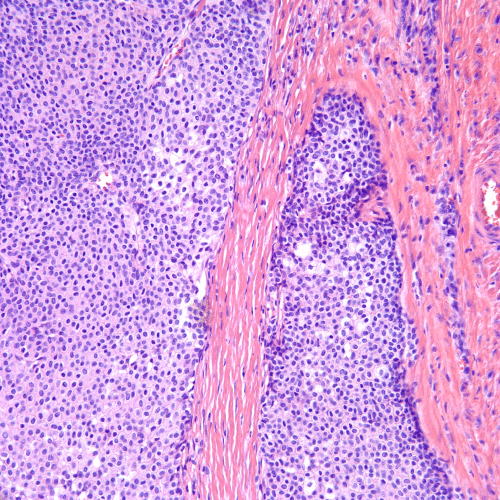
Figure 4. Focal areas display clear/pale cell change (H&E stain, 200x magnification).
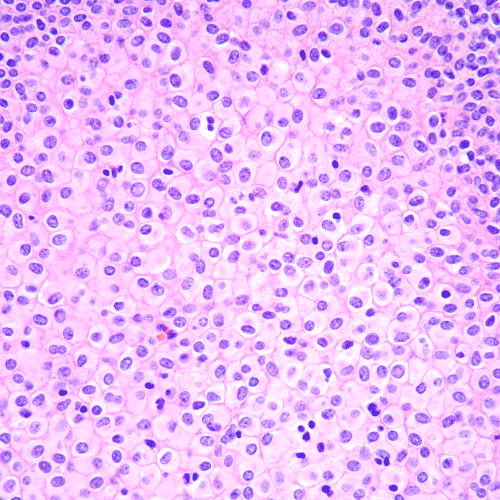
Figure 5. Other areas display abundant oncocytic pink cytoplasm (H&E stain, 400x magnification).
Immunohistochemistry for smooth muscle actin was positive in the tumor cells (Figure 6). The tumor cells were negative for cytokeratin (AE1/-AE3) and S-100 protein. Periodic acid Schiff (PAS) stain highlighted the basement membrane surrounding the neoplastic cells (Figure 7). The immunohistochemistry results established the diagnosis of a glomus tumor and essentially excluded a cutaneous adnexal tumor.
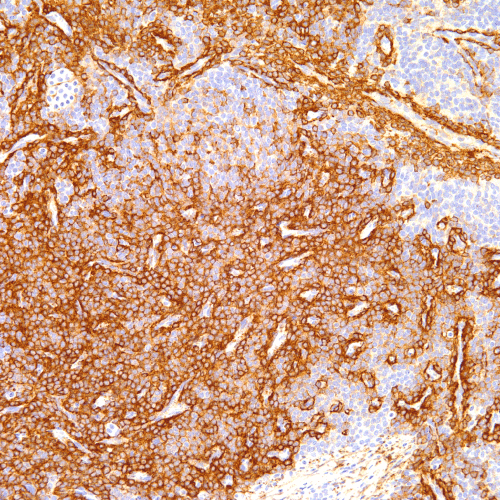
Figure 6. Smooth muscle actin immunostain displays strong cytoplasmic expression in the neoplastic cells (Smooth muscle actin immunohistochemical stain, 200x magnification).
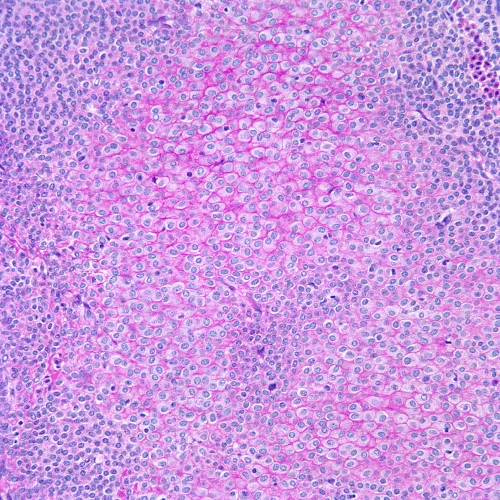
Figure 7. PAS stain highlights basement membrane investing individual oncocytic tumor cells (PAS stain, 200x magnification).
Re-excision demonstrated no residual neoplasm. No further follow up is available.
Discussion
Masson first histologically described glomus tumors in 1924 as a distinct perivascular neoplasm believed to have originated from modified smooth muscle cells within the walls of specialized arteriovenous shunts (Sucquet-Hoyer canals) responsible for thermoregulation [13].
Glomus tumors typically present as a firm, painful, violaceous, solitary nodule of the extremities, especially of the nail bed. Compared to solitary tumors, multiple glomus tumors are less common and are described as bluish nodules that are softer and more compressible than their solid counterparts [14].
Although they are most common in the subungual region of the finger, unusual anatomic sites have been reported including the stomach, rectum, cervix, vagina, mesentery, chest wall, bone, eyelid, and nose [15]. In a meta-analysis review of 127 references, lower extremity glomus tumors were found to have an average size of slightly greater than 2 cm compared to those found typically in the fingers which were rarely greater than 1 cm [4]. In another study, pedal tumors accounted for only 8.3% of the 48 patients diagnosed with a glomus tumor over a nine-year period [7].
Histologic features of a typical glomus tumor include uniform round to cuboidal cells with round, darkly staining nuclei and amphophilic to eosinophilic cytoplasm. The tumor cells are arranged into sheets punctuated by blood vessels around which the cells form perivascular collars composed of concentric rows of uniform tumor cells. [16]. Oncocytic changes characterized by an eosinophilic granular cytoplasm have been described in some glomus tumors [17,18].
In a minority of cases, glomus tumors display atypical features with potential for malignant behavior. These are usually greater than 2 cm, arise in deeper soft tissue, have atypical mitotic figures or a moderate to high nuclear grade and more than 5 mitotic figures per 50 high-power fields.
By immunohistochemistry, glomus tumors express vimentin, muscle actins, myosin, pericellular collagen type IV. They are usually negative for desmin and CD34. They are negative for von Willebrand factor, cytokeratin, and S-100 protein [19]. The immunohistochemical profile in our case (smooth muscle actin positive, cytokeratin negative, and S100 protein negative) supported the diagnosis of glomus tumor.
The differential diagnosis of glomus tumor includes cutaneous adnexal tumors. Histologic distinction between glomus tumor and poroma/dermal duct tumor can cause diagnostic difficulty. Both tumors show circumscribed aggregates of uniform basaloid cells and a predilection for acral sites. A useful feature in distinguishing glomus tumor from poroma/ dermal duct tumor is the absence of characteristic duct differentiation in the former. In our case, the glomus tumor exhibited clear cell change, a finding that may be present focally in dermal duct tumor and other cutaneous adnexal neoplasms. Due to these overlapping histologic features, immunohistochemistry may be critical in establishing the correct diagnosis of glomus tumor with oncocytic and/or clear cell change. Eccrine spiradenomas show nodules of uniform basaloid cells that resemble glomus cells but can be distinguished by duct differentiation and lack of the prominent vascularity seen in glomus tumors [20]. Another useful histologic feature is the intimate localization of glomus cells around blood vessels at the tumor periphery [21].
Conclusion
Glomus tumors of the foot are rare, benign neoplasms that are curable by simple surgical excision. Oncocytic change in glomus tumors is a recognized but uncommon finding that often results in diagnostic confusion with cutaneous adnexal neoplasms. The clear cell change exhibited in our case has not been reported in glomus tumors to our knowledge. As illustrated in our case, the presence of both oncocytic and clear cell features in a glomus tumor can histologically mimic cutaneous adnexal tumors requiring immunohistochemistry to establish a correct diagnosis.
References
- Fletcher D, Unni K, Mertens F (2002) World Health Organization Classification of Tumors. Pathology and Genetics of Tumors of Soft Tissue and Bone.
- Shugart RR, Soule EH, Johnson EW Jr (1963) Glomus tumor. Surg Gynecol Obstet 117: 334-340. [Crossref]
- Gaertner EM, Steinberg DM, Huber M, Hayashi T, Tsuda N, et al. (2000) Pulmonary and mediastinal glomus tumors--report of five cases including a pulmonary glomangiosarcoma: a clinicopathologic study with literature review. Am J Surg Pathol 24: 1105-1114. [Crossref]
- Luis LR Jr, Kaoru GR, Shemuel PB, Mills JL Sr (2008) Lower extremity glomus tumors: comprehensive review for surgeons. Vascular 16: 326-332. [Crossref]
- Herawi M, Parwani AV, Edlow D, Smolev JK, Epstein JI (2005) Glomus tumor of renal pelvis: a case report and review of the literature. Hum Pathol 36: 299-302. [Crossref]
- Moody GH, Myskow M, Musgrove C (1986) Glomus tumor of the lip. A case report and immunohistochemical study. Oral Surg Oral Med Oral Pathol 62: 312-318. [Crossref]
- Sun BG, Yun-tao W, Jia-zhen L (1996) Glomus tumours of the hand and foot. Int Orthop 20: 339-341. [Crossref]
- Conant MA, Wiesenfe2021 Copyright OAT. All rights reservf the skin. Arch Dermatol 103: 481-485. [Crossref]
- Weidner N (2009) Modern Surgical Pathology. Saunders/Elsevier, Philadelphia, PA, USA.
- Folpe AL, Fanburg-Smith JC, Miettinen M, Weiss SW (2001) Atypical and malignant glomus tumors: analysis of 52 cases, with a proposal for the reclassification of glomus tumors. Am J Surg Pathol 25: 1-12. [Crossref]
- Leu HJ (1981) [Glomus tumours: morbid-anatomical analysis of 58 cases, especially infiltrated forms (author's transl)]. Dtsch Med Wochenschr 106: 171-174. [Crossref]
- Gould EW, Manivel JC, Albores-Saavedra J, Monforte H, et al. (1990) Locally infiltrative glomus tumors and glomangiosarcomas. A clinical, ultrastructural, and immunohistochemical study. Cancer 65: 310-318. [Crossref]
- Masson P (1924) Le glomus neuro-myo-arteriel des regions tactiles et ses tumeurs. Lyon Chir 21: 257-280.
- Moor EV, Goldberg I, Westreich M (1999) Multiple glomus tumor: a case report and review of the literature. Ann Plast Surg 43: 436-438. [Crossref]
- Acebo E, Val-Bernal JF, Arce F (1997) Giant intravenous glomus tumor. J Cutan Pathol 24: 384-389. [Crossref]
- Weedon D, Strutton G, Rubin AI (2010) Weedon's Skin Pathology. Churchill Livingstone, Great Britain.
- Slater DN, Cotton DW, Azzopardi JG (1987) Oncocytic glomus tumour: a new variant. Histopathology 11: 523-531. [Crossref]
- Na-Rae K, Ro J, Dong-Hae C (2004) Oncocytic Glomus Tumor - A Case Report. The Korean Journal of Pathology 38: 268-269.
- Barnhill RL (2010) Dermatopathology. McGraw-Hill Medical, New York.
- 20. Rapini RP. Practical Dermatopathology. Philadelphia: Elsevier Mosby; 2005.
- Gombos Z, Zhang PJ (2008) Glomus tumor. Arch Pathol Lab Med 132: 1448-1452. [Crossref]







