Abstract
Background: Crohn’s disease (CD) and ulcerative colitis (UC) are main inflammatory bowel diseases (IBD) which show progression with remissions and exacerbations. Mean platelet volume (MPV) and inflammatory markers are affected in chronic inflammatory diseases. In this study we aimed to investigate MPV in patients with IBD.
Methods: A total of 200 subjects were enrolled. The study group consisted of 100 patients with IBD (UC: 50 and CD:50) and the control group included 100 healthy subjects. Groups were compared regarding MPV and CRP levels. The correlation between MPV and CRP was assessed.
Results: Groups were similar in terms of age, sex and MPV levels (p=0.09, 0.08, 0.459, respectively). CRP levels were higher in patients with CD (p<0.001). A significant correlation was found between MPV and CRP only in active CD patients (r=-0,527; p=0,009).
Conclusion: Although MPV was found to be associated with chronic inflammatory conditions, we did not show any association between inflammatory bowel disease.
Key words
Mean platelet volume, Ulcerative colitis, Crohn’s disease
Introduction
Ulcerative colitis (UC) and Crohn’s disease(CD) are inflammatory bowel diseases (IBD) that affect different regions of gastrointestinal tract [1]. Genetic, environmental and immunological factors are associated with the pathogenesis of both cases. The assessment of IBD is based on a clinical symptoms, physical examination, laboratory tests, radiology and endoscopy with histology. The clear distinction between the two diseases is established by only histopathologic examination [2]. However, pathologic evaluation of the disease activity may not be correlated with clinical and endoscopic findings.
Clinical activities of both diseases are assessed by specific activity indices [3,4,5]. Increased acute phase reactants like C-reactive protein (CRP), fibrinogen and ferritin are important parameters indicating the activity of disease as well as increased erythrocyte sedimentation rate (ESR), thrombocytosis and leukocytosis. Platelets are mainly involved in homeostasis but recent studies have shown that they also have an important role in inflammatory response [6,7,8].
There is no any gold standard test or examination for to determine the type, disease activity and prognosis of inflammatory bowel diseases. Therefore, a non-invasive biomarker for IBD has been a focus in IBD researches.
In case of an inflammation, platelets undergo structural modification and secrete some cytokins which result with a decrease in mean platelet volume [9]. Recent studies reported different results about the correlation between MPV and other inflammatory markers in inflammatory bowel diseases [10,11]. In this study we aimed to investigate MPV levels in patients with CD or UC.
Materials and methods
This retrospective study was carried out in the internal medicine and gastroenterology outpatient clinics of a tertiary hospital in Istanbul from 01 January 2010 to 01 July 2012. The institutional review board of the hospital approved this experiment (IRB number: 14.04.2012/63), and informed consent was obtained from all subjects. All procedures were followed in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008.
A total of 200 subjects from both genders, with a minimum age of 18 years old, were included. The study group was comprised of 100 patients with IBD and the control group was comprised of 100 healthy subjects. The study group was divided into two subgroups. One of the subgroup was comprised of 50 patients with UC and the other one comprised of 50 patients with CD.
Diagnosis of IBD was mainly done according to clinical, endoscopic and pathologic criteria. The BMIs were achieved from the records which had been calculated according to height and weight measurements for each individual at the time of admission. The blood sample results were recorded concurrently at the time when clinical activity indices of CD and UC patients were calculated. Control group was collected among healthy subjects who did not have a history of acute or chronic infection, endocrinological or hematological disease, heart failure, hepatic and renal disorder, cancer and peripheral vascular disease. None of the enrolled subjects had received any medication influencing biochemical tests.
Crohn’s Disease Activity Index (CDAI) and Modified Truelove Witts Activity Index (MTWAI) were used for evaluating clinical activities of CD and UC, respectively [12,13]. Complete blood counts were measured with the Sysmex XE 2100i (Japan) by fluorescence flow cytometry, ESR and CRP levels were determined using the Westergreen method and immunoturbidimetry, respectively. Body mass index was calculated according to the medical records achieved on admission for each individual. Disease Activity Index scores, hemoglobin, hematocrite, platelet count, MPV and CRP levels were recorded.
All analyses were performed using NCSS ( Number Cruncer Statistical System) 2007 & PASS (Power Analysis and Sample Size) 2008 Statistical Software (Utah, USA). Data are shown as mean ± standard deviation (SD). Besides descriptive analysis ( mean, Standard error, frequency, ratio) ANOVA or Kruskal-Wallis tests were used to compare the quantitative measurements between the three groups. Students’ t test was used to compare variance between groups with normal distribution and Mann Whitney U test was used for comparing groups without normal distribution. Pearson or Spearman correlation analysis were used to show the correlation between MPV and other inflammatory markers. The probability of making a Type I error (alpha, significance) is 0.05 in all tests.
Results
Groups were similar in terms of age and sex (p=0.09 and 0.08, respectively). There were 26 women (52%) and 24 men (48%) in the CD group. The study group of patients with UC consisted of 19 women (38%) and 31 men (62%), while the control group of healthy participants contained 57 women (57%) and 43 men (43%). Both of the subgroups were comparable according to the frequency of active disease. Twenty-three out of 50 CD and 24 out of UC patients were at active disease period (p=0.842) (Table 1).
|
|
Crohn’s Disease
(N=50)
|
Ulcerative colitis
(N=50)
|
Control
(N=100)
|
p
|
|
Age (years)
|
36.48 ± 11.41
|
40.84 ± 12.93
|
37.52± 8.54
|
0.09
|
|
Body mass Index (kg/m2)
|
24.64 ± 6.12
|
24.88 ± 4.33
|
23.42± 2.84
|
0.083
|
|
Female (%)
|
26(52%)
|
19(38%)
|
57(%57)
|
0.08
|
|
Active Disease
|
23(46%)
|
24(48%)
|
---
|
0.842
|
|
Platelet (103/µL)
|
316.66 ± 92.84
|
298.76 ± 76.17
|
265.68 ± 58.42
|
0.001
|
|
MPV(fL)
|
7.76 ± 0.95
|
7.76 ± 1.37
|
7.94 ± 0.82
|
0.459
|
|
CRP (mg/dL)
|
1.58 ± 3. 37
|
0.69 ± 0.87
|
0.33 ± 0.03
|
0.001
|
|
Hemoglobin (g/dL)
|
13.0 ± 2.1
|
13.2 ± 1.1
|
13.9 ± 1.2
|
0.001
|
|
Hemotocrit (%)
|
39.2 ± 5.9
|
39.6 ± 4.7
|
41.5 ± 3.7
|
0.006
|
Table 1. The demographic and clinical features of the patients and controls.
The MPV levels of the groups were statistically similar. The MPV levels of patients with CD, UC and healthy subjects were 7.76 ± 0.95, 7.76 ± 1.37 and 7.94 ± 0.82, respectively (p=0.459, Table 1). The serum CRP levels of the groups were statistically different. Patients with CD had highest CRP levels. The CRP levels of the patients with CD, UC and healthy subjects were 1.58 ± 3. 37, 0.69 ± 0.87 and 0.33 ± 0.03, respectively (p<0.001) (Table 1). The blood hemoglobin levels, hemotocrit percentages and platelet counts of the groups were also statistically different (p<0.001, <0.006, <0.001, respectively, Table 1).
The comparison of MPV and CRP values of the active and inactive CD patients did not show any significant difference (7.86 ± 0.92 vs. 7.64 ± 098, p=0.426, 0.68 ± 0.65 vs. 2.65 ± 4.76, p=0.126, respectively, Table 2). Platelet level of patients with active CD was higher than patients with inactive CD (p=0.012). The comparison of MPV values of the active and inactive UC patients also did not show any significant difference (8.07 ± 1.65 vs. 7.43 ± 0.91, p=0.101). On the other hand, there was a statistically significant difference between active and inactive UC patients according to the CRP levels (0.45 ± 0.37 vs. 0.96 ± 1.15, p= 0.018, Table 3).
|
|
Crohn’s disease (inactive)
N=27
|
Crohn’s disease (active)
N=23
|
p
|
|
Platelet (103/µL)
|
285.78 ± 71.51
|
352.91 ± 103.00
|
0.012
|
|
MPV (fL)
|
7.86 ± 0.92
|
7.64 ± 098
|
0.426
|
|
CRP (mg/dL)
|
0.68 ± 0.65
|
2.65 ± 4.76
|
0.126
|
Table 2. Platelet, MPV and CRP levels of active and inactive CD patients
According to the Pearson correlation analyses; an inverse correlation was found between MPV and CRP (r = -0.527, p = 0.009, Table 4, Figure 1) in patients with CD. CRP levels were positively correlated with CDAI in patients with CD (r = 0.477, p = 0.004, Table 5, Figure 2). Similarly, a positive correlation was found between CRP levels and MTWAI (r = 0.405, p = 0.003, Table 5) in patients with UC.
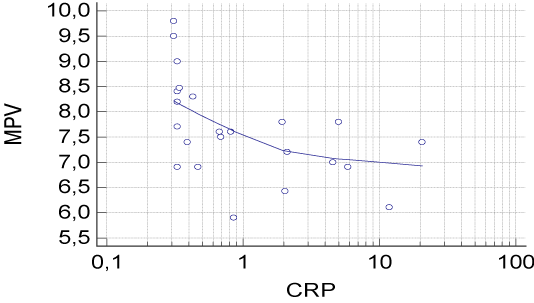
Figure 1. A scatter diagram shows the correlation between MPV and CRP in patients with CD.
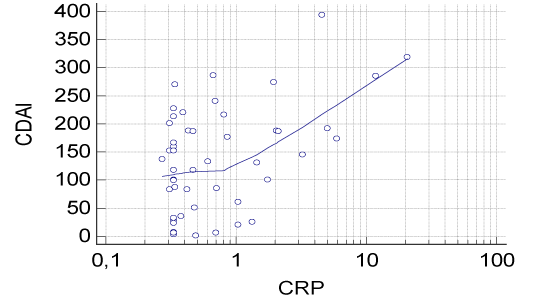
Figure 2. A scatter diagram shows the correlation between CDAI and CRP in patients with CD.
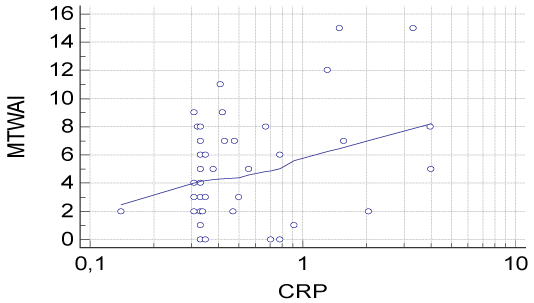
Figure 3. A scatter diagram shows the correlation between MTWAI and CRP in patients with UC.
|
|
Ulcerative colitis (active)
N=26
|
Ulcerative colitis (inactive)
N=24
|
p
|
|
Platelet (103/µL)
|
291.77± 69.44
|
306.33 ± 83.69
|
0.505
|
|
MPV (fL)
|
8.07 ± 1.65
|
7.43 ± 0.91
|
0.101
|
|
CRP (mg/dL)
|
0.45 ± 0.37
|
0.96 ± 1.15
|
0.018
|
Table 3. Platelet, MPV and CRP levels of active and inactive UC patients
|
|
CRP
|
|
MPV
|
(CD)
r=-0.527
p=0.009
|
|
|
(UC)
r=0.043
p=0.766
|
Table 4. Pearson Correlation analyses tests, an inverse correlation was found between MPV and CRP in patients with CD.
|
|
CDAI
|
MTWAI
|
|
MPV
|
r=-0.182
p=0.204
|
r=-0.292
p=0.059
|
|
CRP
|
r=0.477
p=0.004
|
r=0.405
p=0.003
|
2021 Copyright OAT. All rights reserv
Table 5. Pearson Correlation analyses tests, The correlation between CDAI and MPV, CRP in patients with CD and he correlation between MTWAI and MPV, CRP in patients with UC.
Discussion
In this study we investigated the MPV levels in patients with IBD. UC and CD are two main inflammatory bowel diseases. While UC is limited to the colon, CD can involve any segment of the gastrointestinal tract. The clinical course of diseases is characterized by remission and relapse which may develop spontaneously or in response to medical treatment. Early diagnosis and treatment of active disease are important for reducing morbidity and mortality [14]. Many non-invasive tests have been studied for diagnosis and determining the activation degree of inflammatory bowel disease. Nevertheless, an ideal test has not been found yet. MPV is a measurement of the average size of platelets. MPVcorrelates with platelet function and activation. It can be influenced by the inflammation. Larger platelets which are metabolically and enzymatically more active used in inflammatory process [15].
We have shown that MPV levels are not affected by active and inactive CD and UC. We have also shown high CRP levels in patients with CD. Our results are in accordance with some of previous studies while there are also inconsistent results. Douda et al compared MPV levels of active and inactive 56 CD patients and found that active CD patients had significantly lower MPV levels than inactive ones [16]. Zubcevic et al studied on 36 CD patients and reported that MPV levels were associated with mild and moderate disease activity. In addition they also reported high CRP levels in CD patients [17].
We did not find any significant difference among MPV and CRP levels of active and inactive CD patients. Song Liu et al. demonstrated lower MPV levels in CD patients in their study that was conducted with 61 CD patients and 50 healthy controls in 2011 (12). However, when CD patients were classified into two groups as active and inactive patients, the MPV levels were comparable with healthy controls. This study failed to demonstrate any correlation between MPV levels and other activity indices in CD patients as well, similar to our study.
In present study we have not found any difference between active and inactive UC patients according to the MPV levels. Conversely, CRP levels were high in patients with active UC. In addition no correlation was found between MPV and CRP in these patients. Kayhan et al reported similar MPV levels in active and inactive UC patients [18]. On the other part, some of previous studies showed that active UC patients had lower MPV values than inactive ones and healthy controls [18-20]. We have found an inverse correlation between MPV and MTWAI in the current study. In accordance with this link Yuksel et al showed a correlation between MPV and MTWAI in their study [18].
The present study had some limitations. First, it would have been beneficial if the sample size had been larger. Second, MPV and CRP levels could be compared with other inflammatory cytokins. Thirth, this is a retrospective study. The result of a prospective study with larger sample size may be more helpful.
In conclusion, new biomarkers are needed and searched for diagnosing and predicting active disease in many inflammatory diseases. Chronic inflammation in IBD leads to alterations in platelet number and morphology [21]. Being an inexpensive and feasible marker, studies have focused specifically on MPV [22]. Although most of the studies show that MPV changes in case of inflammation, it is still not accepted as a valid biomarker for diagnosis or follow ups of any inflammatory disease. According to the result of the current study we suggest that MPV could be hardly used as a marker in determination disease activity for both diseases.
Acknowledgements and conflict of interest
The authors declare that they have no conflict of interest.
Contribution details
T.S. (initials) contributed to concept, discussion and wrote manuscript. Ş.Ö.K. contributed to concept, design, discussion, analyzed data, edited and wrote the manuscript. C.E. researched data and contributed to discussion, concept and design. S.A. contributed to discussion, Z.S. contributed to discussion and wrote manuscript.
References
- Montgomery SM, Ekbom A (2002) Epidemiology of inflammatory bowel disease. Curr Opin Gastroenterol 18: 416-420. [Crossref]
- StensonWF (2006) Inflamatuar Barsak Hastaliklari. In: Goldman Lee, Ausiello D. Eds. Cecil Textbook of Medicine. Ankara: Günes Kitapevi 861-869.
- Harvey RF, Bradshaw JM (1980) A simple index of Crohn’s disease Activity. Lancet 1: 514. [Crossref]
- Gasche C, Scholmerich J, Brynskov J, D'Haens G, Hanauer SB, et al. (2000) A simple classification of Crohn's disease: report of the Working Party for the World Congresses of Gastroenterology, Vienna 1998. Inflamm Bowel Dis 6: 8-15. [Crossref]
- Seo M, Okada M, Yao T, Ueki M, Arima S, et al. (1992) An index of disease activity in patients with ulcerative colitis. Am J Gastroenterol 87: 971-976. [Crossref]
- Elzey BD, Tian J, Jensen RJ, Swanson AK, Lees JR, et al. (2003) Platelet-mediated modulation of adaptive immunity. A communication link between innate and adaptive immune compartments. Immunity 19: 9-19. [Crossref]
- Klinger MH (1997) Platelets and inflammation. Anat Embryol (Berl) 196: 1-11. [Crossref]
- Bout D, Joseph M, Pontet M, Vorng H, Deslée D, et al. (1986) Rat resistance to schistosomiasis: platelet-mediated cytotoxicity induced by C-reactive protein. Science 231: 153-156. [Crossref]
- Brandt E, Ludwig A, Petersen F, Flad HD (2000) Platelet-derived CXC chemokines: old players in new games. Immunol Rev 177: 204-216. [Crossref]
- Kapsoritakis AN, Koukourakis MI, Sfiridaki A, Potamianos SP, Kosmadaki MG, et al. (2001) Mean platelet volume: a useful marker of inflammatory bowel disease activity. Am J Gastroenterol 96: 776-781. [Crossref]
- Liu S, Ren J, Han G, Wang G, Gu G, Xia Q, Li J.,2012. Mean platelet volume: a controversial marker of disease activity in Crohn's disease. Eur J Med Res 17: 27. [Crossref]
- Best WR, Becktel JM, Singleton JW, Kern F Jr (1976) Development of a Crohn's disease activity index. National Cooperative Crohn's Disease Study. Gastroenterology 70: 439-444. [Crossref]
- Friedman S, Blumberg SR (2015) Inflammatory bowel disease. In: Longo DL et al (eds). Harrison’s principles of internal medicine. New York: Mc Graw Hill 1947-1965.
- Threatte GA (1993) Usefulness of the mean platelet volume. Clin Lab Med 13: 937-950. [Crossref]
- Douda T, Bures J, Rejchrt S, Kopácová M, Pecka M, et al. (2006) [Mean platelet volume (MPV) in Crohn's disease patients]. Cas Lek Cesk 145: 870-873. [Crossref]
- Zubcevic N, Mesihovic R, Zubcevic S (2010) Usefulness of laboratory data in estimation of Crohn's disease activity. Med Arh 64: 33-36. [Crossref]
- Kayahan H, Akarsu M, Ozcan MA, Demir S, Ates H, et al. (2007) Reticulated platelet levels in patients with ulcerative colitis. Int J Colorectal Dis 22: 1429-1435. [Crossref]
- Yüksel O, Helvaci K, Başar O, Köklü S, Caner S, et al. (2009) An overlooked indicator of disease activity in ulcerative colitis: mean platelet volume. Platelets 20: 277-281. [Crossref]
- Polińska B, Matowicka-Karna J, Kemona H (2009) [The cytokines in inflammatory bowel disease]. Postepy Hig Med Dosw (Online) 63: 389-394. [Crossref]
- Järemo P, Sandberg-Gertzen H (1996) Platelet density and size in inflammatory bowel disease. Thromb Haemost 75: 560-561. [Crossref]
- Tang J, Gao X, Zhi M, Zhou HM, Zhang M, et al. (2015) Plateletcrit: a sensitive biomarker for evaluating disease activity in Crohn's disease with low hs-CRP. J Dig Dis 16: 118-124. [Crossref]
- Danese S, Scaldaferri F, Papa A, Pola R, Sans M, et al. (2004) Platelets: new players in the mucosal scenario of inflammatory bowel disease. Eur Rev Med Pharmacol Sci 8: 193-198. [Crossref]



