Abstract
The prevalence of obesity in the United States has increased rapidly over the past few decades and has become a major public health concern. Childhood obesity is a risk factor for the development of several chronic physical and mental health conditions. Studies suggest that children in the rural areas are at a higher risk for obesity. Thus, there is a need to have effective interventions to prevent childhood obesity. The objective of this systematic review and meta-evaluation is to identify existing interventions for prevention of obesity and evaluate quality and applicability of these interventions in different populations. We conducted a systematic search for studies published in electronic databases from 1980 to 2014. Intervention studies with a focus on prevention of obesity in children ages 2-20 years, residing in rural or Appalachian region of the United States were included. The selection process identified 21 eligible studies for inclusion. A majority of the studies used quasi-experimental design (N = 9) and mostly targeted children from the ages of 8-11 years. Outcome measures included attitude and knowledge of healthy lifestyle, change in diet and physical activity, and body mass index. A large variation in meta-evaluation score was obtained (15-29). Overall, studies reported positive changes in healthy behaviors, suggesting the importance and effectiveness of these interventions in the prevention of obesity. These findings provide insight for designing effective future interventions for obesity prevention.
Key words
appalachia, childhood obesity, intervention, meta-evaluation, prevention of obesity, rural
Introduction
The prevalence of obesity among children in the United States has increased rapidly over the past three decades to a point where pediatric obesity is now considered a public health threat [1,2]. According to the 2009-2010 National Health and Nutrition Evaluation Survey results, approximately 17% of children and adolescents (ages 2-19 years) in the U.S. are obese and about 32% are overweight or obese [3]. Further, economic costs of obesity impact the entire nation, with childhood obesity-related medical costs estimated at $14 billion annually [4]. Childhood obesity has been identified as a risk factor for the development of chronic diseases, including depression, anxiety, hypertension, insulin resistance, dyslipidemia, metabolic syndrome, and type II diabetes [5,6]. This dramatic increase in the rate of obesity is adversely affecting the health of pediatric population. In addition to the physiological complications, psychological issues such as low self-esteem, depression, and social isolation are also highly prevalent in overweight and obese children, resulting in poor quality of life [7].
Previous research suggests that children in rural-dwelling areas are at a disproportionately higher risk for overweight and obesity compared to their peers in urban and suburban settings [8]. In addition, Appalachian areas have the highest prevalence rates of obesity among the rural areas in the U.S [9]. Reasons for these higher rates of obesity in rural and Appalachian children may be related to several factors, including poverty [10,11], inadequate access to healthcare and preventive health, low levels of physical activity [12], poor nutrition practices [12], and lack of supportive environments [11]. For children of these rural areas, obesity education and prevention is of particular importance due to the lack of medical and health-related formal communication.
Childhood obesity is problematic because it is resistant to treatment once established and increases the likelihood of adult obesity, which is associated with several health risks [13]. Furthermore, cultural, economic and geographical characteristics of Appalachian and rural communities make it challenging to reduce childhood obesity [9]. Thus, prevention is the major focus of public health authorities. One of the goals of Healthy People 2020 is to reduce the proportion of children and adolescents aged 2 to 19 years who are considered obese (Objective NWS-10.4) [14]. This systematic review and meta-evaluation focuses on intervention studies for the prevention of childhood obesity, conducted in rural-dwelling areas.
Methods
Literature search process
A systematic literature search was conducted, for studies published from January 1, 1980 to October 31, 2014, in electronic databases including Academic Search Premiere, CINAHL, ERIC, PubMed, and psychINFO. The search strategy included a combination of keywords related to obesity and interventions such as overweight, obesity, program, prevention, intervention, treatment, rural, and Appalachia.
According to Appalachian Regional Commission, Appalachia consists of the area following the Appalachian Mountains which includes all of West Virginia and portions of 12 other states: Alabama, Georgia, Kentucky, Maryland, Mississippi, New York, North Carolina, Ohio, Pennsylvania, South Carolina, Tennessee, and Virginia [15]. A large portion of this Appalachian region is rural. According to the U.S. Census Bureau, rural region is considered anything not urban, or a population smaller than 2,500 people [16].
Initial screening identified titles or abstracts related to interventions for childhood obesity. Furthermore, bibliographies of those selected articles were screened for additional studies of relevance. Titles, abstracts or full-texts reviewed were screened against the inclusion criteria described below. Articles that met the inclusion criteria were then subjected to meta-evaluation. The selection criterion is shown in Figure 1.
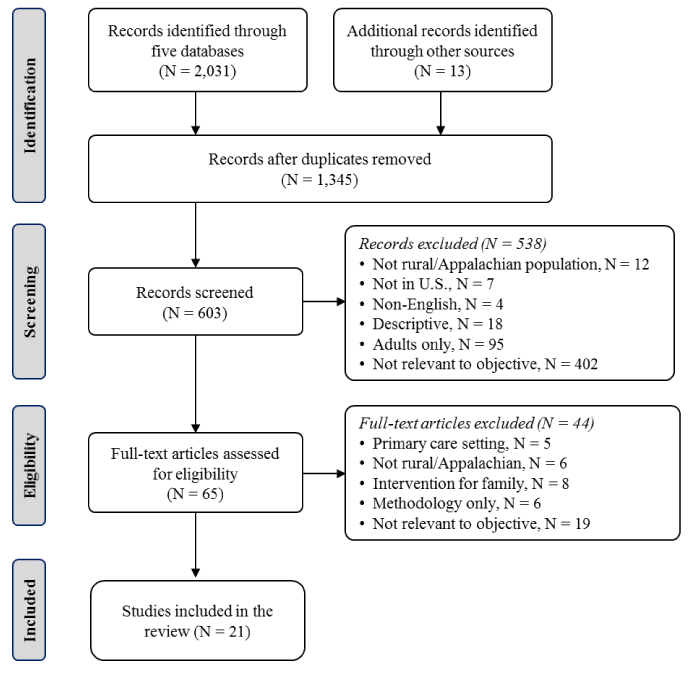
Figure 1. Schematic representation of selection process (PRISMA).
Study inclusion criteria
The search was limited to studies in English, published in peer-reviewed journals, and those with original research findings for the interventions being evaluated. Studies focusing on interventions in children ages 2-20 years, residing in rural or Appalachian region of the United States were included. Further, most of the studies included assessed school-based interventions. For the purpose of this meta-evaluation, only those studies focusing on preventive interventions were included; interventions with a focus on treatment of obesity were excluded. Furthermore, studies were included if they focused on either promotion of physical activity and/or nutrition along with any other educational interventions. The studies included either used pre-experimental, experimental or quasi-experimental study design. The other requirements for inclusion were use of appropriate statistical techniques and large enough sample size (≥ 30) for meaningful analyses.
Description of meta-evaluation approach
The purpose of this meta-evaluation of intervention studies is to provide a useful evaluation of the overall validity of the research focusing on prevention of childhood obesity. The basic methodological approach for meta-evaluation comprises of a systematic review of research studies using a standardized set of design followed by evaluating studies against a methodological criteria to estimate the relative degree and strength of the internal and external validity of the studies reviewed. In the meta-evaluation approach, a specified number of points are assigned to each study based on the characteristics of each study corresponding to the criteria designed for evaluation. The higher the number of total points, the greater the likelihood of internal and external validity, and therefore the greater the significance of the research findings [17].
The methodological criteria used included the areas of research design, sample size, length of observation period, quality of measurements used, outcome measures considered in the intervention (such as physical activity, dietary intake, health knowledge, body mass index, and sedentary activity), experimental time period, and quality of methodology used (description of setting, population characteristics, theoretical basis, intervention, and statistical analysis). The scoring strategy based on the methodological criteria is listed in Table 1.
|
Points
|
Meta-evaluation criteria subcomponents
|
|
Criterion #1 Research Design (e.g., “Design”)
|
|
5
|
Randomized pretest and posttest, plus matched control group with multiple replications
|
|
4
|
Equivalent control group design, with pretest and posttest with multiple replications
|
|
3
|
Nonequivalent control group design, with pretest and posttest with multiple replications
|
|
2
|
Subjects as own controls, with pretest and posttest with multiple replications
|
|
1
|
Subjects as own controls, with pretest and posttest with single replication
|
|
Criterion #2 Sample size (e.g., “Sample”)
|
|
5
|
Sample size >1500
|
|
4
|
Sample size from 1000 to 1499
|
|
3
|
Sample size from 500 to 999
|
|
2
|
Sample size from 100 to 499
|
|
1
|
Sample size <100
|
|
Criterion #3 Length of observation period (e.g., “Length”)
|
|
5
|
Observation period >12 months
|
|
4
|
Observation period from 10 to 12 months
|
|
3
|
Observation period from 7 to 9 months
|
|
2
|
Observation period from 4 to 6 months
|
|
1
|
Observation period ≤ 3 months
|
|
Criterion #4 Quality of Measurements Used (e.g., ‘‘Measurements’’)
|
|
5
|
Self-report with independent objective verification for all measures, with use of standard measures
|
|
4
|
Self-report with independent objective verification for most measures
|
|
3
|
Self-report or independent objective verification for selected measures
|
|
2
|
Self-report only on risk factors and biometric measures
|
|
1
|
Limited consistency in measurement methodology
|
|
Criterion #5 Outcome measures considered in the intervention, such as physical activity, dietary intake, health knowledge, body mass index, and sedentary activity (e.g., “Outcomes”)
|
|
5
|
Number of outcomes evaluated ≥ 5
|
|
4
|
Number of outcomes evaluated = 4
|
|
3
|
Number of outcomes evaluated = 3
|
|
2
|
Number of outcomes evaluated = 2
|
|
1
|
Number of outcomes evaluated = 1
|
|
Criterion #6 Experimental time period (e.g., “Recentness”)
|
|
5
|
Last year of intervention conducted after 2010
|
|
4
|
Last year of intervention conducted from 2006 to 2010
|
|
3
|
Last year of intervention conducted from 2001 to 2005
|
|
2
|
Last year of intervention conducted from 1990 to 2000
|
|
1
|
Last year of intervention conducted prior to 1990
|
|
Criterion #7 Quality of methodology used, such as description of setting, population characteristics, theoretical basis, intervention, and statistical analysis (e.g., “Methodology”)
|
|
5
|
Number of methodology components described in detail = 5
|
|
4
|
Number of methodology components described in detail = 4
|
|
3
|
Number of methodology components described in detail = 3
|
|
2
|
Number of methodology components described in detail = 2
|
|
1
|
Number of methodology components described in detail = 1
|
Table 1. Meta-evaluation criteria
Results
Study selection and description
Approximately 2,000 articles were identified for the review process. The selection process resulted in 21 studies eligible for inclusion (Figure 1). The studies included are summarized in Table 2. The table provides brief description of the target population, intervention, duration of intervention, theoretical framework, outcome measures, and relevant findings [18-39].
|
Author/
Year
|
Study design
|
Population
|
Region
|
Intervention
|
Intervention duration
|
Theory-based
|
Outcome measures
|
Summarized findings
|
|
Ling et al. (2014) [29]
|
Quasi-experimental
|
K to 5th graders
Age = 6-12 years
N = 1,508
|
Rural KY
|
School-based healthy lifestyle intervention
|
5 months
|
No
|
Health education (nutrition and physical activity)
|
Significant increase in percentage of children met physical activity (1% vs. 5%, P < 0.01) and nutrition (15% vs. 26%, P < 0.01) recommendations after intervention.
|
|
Morgan et al. (2014) [30]
|
Quasi-experimental
|
4th graders
Age = 9-11 years
N = 105
|
Rural AL
|
CATCH nutrition curriculum
|
2.5 months
|
Social Cognitive Theory
|
Nutrition education, physical activity, motivation
|
Significant improvement in nutrition knowledge and healthy food choices (P < 0.05) in intervention group.
|
|
Smith and Holloman (2014) [37]
|
Experimental
|
9th to 12th graders
Age = 14-20 years
N = 186
|
Rural Appalachia
|
School-based intervention
|
1 month
|
No
|
Consumption of sugar-sweetened drinks, water consumption
|
Daily servings of sugar-sweetened beverages significantly decreased (2.32 to 1.32, P < 0.001), and water consumption increased by 19% post-intervention.
|
|
Struempler et al. (2014) [38]
|
Quasi-experimental
|
3rd graders
N = 2,477
|
Rural AL
|
School-based nutrition program
|
4 months
|
Experiential Learning Theory
|
Nutrition
|
Moderate, but significant increase in food/vegetable consumption in intervention group (P < 0.01)
|
|
Cohen et al. (2013) [21]
|
Experimental
RCT
|
1st to 6th graders
Mean age = 8.65 ± 1.6 years
N = 432
|
Rural communities in CA, KY, MS, SC
|
CHANGE - community and school-based intervention
|
12 months
|
No
|
Fruits and vegetables intake and other diet
|
Students enrolled in the intervention consumed significantly more fruits/vegetables and showed a reduction in the average daily dietary glycemic index (P < 0.05).
|
|
Puma et al. (2013) [33]
|
Quasi-experimental
|
2nd graders
N = 363
|
South-central CO
|
Integrated Nutrition and Physical Activity Program (INPAP)
|
3-6 years
|
Social Cognitive Theory
|
Nutrition and physical activity knowledge, self-efficacy, attitudes and behaviors, BMI
|
Long-term effects were observed in nutrition-related knowledge and attitudes, but these effects attenuated over time.
|
|
Williamson et al. (2012) [39]
|
Experimental; Longitudinal, cluster 3-arm RCT
|
4th to 6th graders
Mean age = 10.5 years
N = 2,060
|
Rural LA
|
Environmental School-based prevention program
|
28 months
|
No
|
Percent body fat, BMI, change in behavior
|
Decreased body fat, but no difference in physical activity in intervention group compared to control group.
|
|
Craven et al. (2011) [23]
|
Quasi-experimental
|
9th graders
Age = 13-19 years
N = 399
|
Rural Eastern NC
|
Nutrition Education Intervention
|
4 months
|
Social Cognitive Theory
|
BMI, diet intake
|
Greater decline in BMI along with fruit/vegetable intake in intervention group.
|
|
Greening et al. (2011) [26]
|
Experimental; RCT cluster by school
|
Age = 6-10 years
N = 450 (Control = 246, Intervention = 204)
|
Rural MS
|
TEAM Mississippi Project
|
8 months
|
Social Learning Theory
|
Nutrition, knowledge, health behavior, physical activity, percentage body fat
|
Significant decline in precent body fat (P = 0.02), greater engagement in physical activity (P = 0.04), and decline in dietary fat intake (P < 0.0005) in intervetnion group.
|
|
Smith et al. (2011) [36]
|
Pre-experimental
|
3rd and 4th graders who were overweight and obese
Age = 8-12 years
N = 72
|
Appalachia
|
Teen Mentoring Intervention - after-school program
|
2 months
|
Theory of Planned behavior
|
BMI, health behavior, nutritional knowledge, attitude towards healthy eating and physical activity
|
Significant increase in positive health behavior, i.e. healthy eating (P = 0.02), improvement in nutritional knowledge, and improved attitude towards healthy diet (P = 0.05). Significant reduction in BMI was also observed (P = 0.03).
|
|
Hovland et al. (2010) [28]
|
Quasi-experimental
|
3rd graders
Age = 6-11 years
N = 138
|
Appalachian OH
|
FoodMASTER curriculum delivered by teachers
|
9 months
|
No
|
Dietary intake
|
No significant differences in dietary intake.
|
|
Canavera et al. (2009) [18]
|
Pre-experimental
|
5th graders
Age = 10-12 years
N = 122
|
Rural KY
|
School-based teacher delivered intervention
|
3 months; 1 session per week
|
Social Cognitive Theory
|
Fruit and vegetable consumption, water consumption, television viewing time, physical activity
|
Intervention significantly improved consumption of water (P = 0.022) and reduced television viewing (P = 0.022).
|
|
Drummond et al. (2009) [24]
|
Pre-experimental
|
K to 12th graders
N = 1,876 (approx.)
|
Rural AZ
|
Steps to a Healthier Arizona - childcare setting
|
3 years; 7 workshops across 9 months
|
Community Change Model
|
Nutrition, physical activity
|
Significant increase in median total number of best practices from 36 to 44 (P = 0.0003). Significant increase in nutrition best practices from 25 to 30 (P = 0.0003).
|
|
Schetzina et al. (2009, 2011) [34, 35]
|
Pre-experimental
|
Age = 7-10 years
N = 114
|
Rural Appalachia
|
Winning with Wellness - school-based approach
|
18 months; 6 workshops
|
Coordinated School Health Model
|
BMI, physical activity, nutrition
|
Children were more active at school after program implementation, followed healthy food habits (P< 0.0001).
|
|
Muth et al. (2008) [31]
|
Experimental; RCT cluster by classrooms
|
4th graders
N = 75 (Control = 37, Intervention = 38)
|
Rural NC
|
IMPACT - integrated in-classroom curriculum
|
3 months
|
Social Cognitive Theory
|
Dietary intake
|
Significant increase in daily fruit/vegetable intake, calcium-rich foods, and grain intake (P < 0.05) in intervention group as well as Increase in diet knowledge (P = 0.01).
|
|
Gombosi et al. (2007) [25]
|
Pre-experimental
|
K to 8th graders
Age = 5-14 years
N = 4,241 (approx.)
|
Rural PA
|
Fit for Life - health education curriculum
|
5 years ( 1999 - 2004; during school year)
|
No
|
BMI, health education
|
Overall increase in overweight and obesity of children, indicating inadequate health education.
|
|
Cason et al. (2006) [20]
|
Quasi-experimental
|
4th graders
Age = 9-11 years
N = 130
|
Rural SC
|
Jump Into Foods and Fitness (JIFF) curriculum
|
5 months
|
No
|
Health knowledge and behavior (diet and physical activity)
|
Significant improvement in health-related behavior after the completion of intervention program. (P < 0.005).
|
|
Carrel et al. (2005) [19]
|
Experimental; RCT
|
Children with BMI > 95th percentile for age
Mean age = 12 ± 0.5 years
N = 53
|
Rural WI
|
School-based fitness program
|
9 months
|
No
|
BMI, percentage body fat, cardiovascular fitness
|
Significantly greater loss of body fat, greater increase in cardiovascular fitness, and greater improvement in fasting insulin level (P < 0.05).
|
|
Cottrell et al. (2005) [22]
|
Experimental; RCT cluster by school
|
Kindergarten
Age = 4-6 years
N = 50 (Control = 26, Intervention = 24)
|
WV
|
CARDIAC-Kinder Care
|
1 month
|
No
|
Physical activity, child diet
|
Significantly greater consumption of fruits/vegetables and fewer sweets among children in intervention group (P < 0.05).
|
|
Harrell et al. (2005) [27]
|
Quasi-experimental
|
5th graders
Mean age = 11.9 ± 0.06 years
N = 205
|
Rural MS
|
Cardiovascular health in children - school-wide program
|
4 months
|
No
|
Fruit and vegetable intake, health knowledge
|
Significant increase in health knowledge (P < 0.0001), increase in vegetable consumption (P < 0.05), and decrease in sugar-sweetened drinks (P < 0.05) in intervention group.
|
|
Pate et al. (2003) [32]
|
Quasi-experimental
|
5th graders
Mean age = 10.8 ± 0.7 years
N = 436
|
Rural SC
|
Community-based after-school program
|
18 months
|
No
|
Physical activity
|
No significant differences in physical activity.
|
Table 2. Summary of interventions for prevention of childhood obesity
Study characteristics
Studies were carried out in rural regions of 13 different states, with most of them conducted in Kentucky [18,21,29], Mississippi [21,26,27], and South Carolina [20,21,32] (N = 3 each). Studies included in this review were conducted either in a school-based or child care setting. Most of the studies were published after 2008 (N = 14) [18,21,23,24,26,28,30,33-39]. Further, a majority of the studies used quasi-experimental design (N = 9) [20,23,27-30,32,33,38]; study design in which a control group is used, however, the design doesn’t account for randomization, followed by randomized control trials (N = 7) [19,21,22,26,31,37,39]. For the studies utilizing randomized control design, randomization occurred at the individual, school or classroom level.
The sample size for these intervention studies ranged from 50 to 4,241. Five studies had an adequate sample size of greater than 500 [24,25,29,38,39] and only two studies had a small sample size of less than 100 [31,36].
Population characteristics
Children from ages 4-20 years (kindergarten through 12th grade) were targeted for intervention, with most of the children in the age group of 8-11 years (N = 15). Consistently, most of the students were in 3rd to 5th grade (N=15). Sex distribution of the participants was included in all of the studies reported in this review. At-risk participants, i.e. those who were overweight or obese, were specifically targeted for intervention in only two studies [19,36].
Theoretical framework
Ten intervention studies used theoretical framework for design of the program and implementation [18,23,24,26,30,31,33-36,38]. Among these studies, five of the interventions were based on Social Cognitive Theory [18,23,30,31,33]. Studies that utilized theoretical framework either used quasi-experimental or pre-experimental design (N = 4 each).
Intervention evaluation
Twenty interventions were school-based and one was conducted in a child care setting [24]. Intervention programs ranged in duration from 1 month to 6 years. Many of the programs in school setting implemented intervention as a part of the school curriculum and teaching staff helped in the implementation of program. Interestingly, one of the studies had teen mentors for program implementation [36]. The programs utilized educational, behavioral, environmental, and social strategies with the focus being either improving knowledge of health behavior or improving health behavior. The health behaviors targeted included fruit and vegetable consumption, consumption of sugar-sweetened beverages, water, type of dietary foods, and physical activity. Almost all of the studies, included in this review, indicated a significant improvement in knowledge or health behavior. Interestingly, one of the studies indicated that improvement in health knowledge faded away over a period of time.
Meta-evaluation of intervention studies
The results of meta-evaluation are shown in Table 3. Overall total score for the studies ranged from 15-29. A majority of studies had a total score above 20 [21-26,28,29,31,33-36,38,39], with only six studies having higher total score equal to or greater than 25 [21,26,33-35,38,39]. Studies with better study design, large sample size, longer observation period, standard measurement methods, higher number of outcomes, and comprehensive methodology scored higher for the corresponding criterion (Table 1). The points obtained by each study varied corresponding to each criterion.
|
Author, Year
|
Design
|
Sample
|
Length
|
Measurements
|
Outcomes
|
Recentness
|
Methodology
|
Total
|
|
Ling et al. 2014 [29]
|
3
|
5
|
2
|
4
|
2
|
4
|
5
|
25
|
|
Morgan et al. 2014 [30]
|
3
|
2
|
1
|
3
|
2
|
5
|
4
|
20
|
|
Smith and Holloman, 2014 [37]
|
2
|
2
|
1
|
1
|
1
|
5
|
3
|
15
|
|
Struempler et al. 2014 [38]
|
3
|
5
|
2
|
5
|
1
|
5
|
5
|
26
|
|
Cohen et al. 2009 [21]
|
5
|
2
|
5
|
4
|
1
|
4
|
5
|
26
|
|
Puma et al. 2013 [33]
|
3
|
2
|
5
|
4
|
4
|
5
|
3
|
26
|
|
Williamson et al. 2012 [39]
|
5
|
5
|
5
|
2
|
2
|
5
|
5
|
29
|
|
Craven et al. 2011 [23]
|
3
|
3
|
2
|
5
|
3
|
4
|
5
|
25
|
|
Greening et al. 2011 [26]
|
5
|
3
|
3
|
4
|
3
|
4
|
5
|
27
|
|
Smith et al. 2011 [36]
|
5
|
2
|
1
|
5
|
3
|
4
|
4
|
24
|
|
Hovland et al. 2010 [28]
|
3
|
2
|
3
|
5
|
2
|
4
|
5
|
24
|
|
Canavera et al. 2009 [18]
|
2
|
2
|
1
|
3
|
3
|
4
|
4
|
19
|
|
Drummond et al. 2009 [24]
|
1
|
5
|
5
|
2
|
2
|
4
|
3
|
22
|
|
Schetzina et al. 2009, 2011 [34, 35]
|
2
|
2
|
5
|
4
|
4
|
4
|
5
|
26
|
|
Muth et al. 2008 [31]
|
5
|
1
|
1
|
4
|
2
|
4
|
5
|
22
|
|
Gombosi et al. 2007 [25]
|
1
|
2
|
5
|
4
|
2
|
3
|
4
|
21
|
|
Cason et al. 2006 [20]
|
3
|
2
|
3
|
2
|
2
|
3
|
3
|
18
|
|
Carrel et al. 2005 [19]
|
5
|
1
|
3
|
3
|
1
|
3
|
3
|
19
|
|
Cottrell et al. 2005 [22]
|
5
|
1
|
2
|
4
|
3
|
3
|
5
|
23
|
|
Harrell et al. 2005 [27]
|
3
|
2
|
2
|
4
|
2
|
3
|
4
|
20
|
|
Pate et al. 2003 [32]
|
3
|
2
|
4
|
3
|
1
|
3
|
4
|
20
|
Table 3. Summary of meta-evaluation scores
Scores were assigned based on criteria specified in Table 1.
Discussion
The prevalence of obesity among children in the U.S. has increased rapidly over the past several decades, becoming a leading nationwide concern. The estimates for childhood obesity in rural-dwelling areas exceed the averages by as much as double, with Appalachian areas having the highest prevalence rates among the rural areas of the U.S. [1,2,9]. Further, current strategies for preventing childhood obesity have not shown promising results in rural Appalachia [9].
School-based interventions provide opportunities for researchers and program planners to target larger population of children efficiently and effectively. With existing resources already available in schools, interventions can be conducted for a longer duration of time. Further, children spend a majority of time in school and thus, successful school-based programs can be integrated into the curriculum. Improving attitude and knowledge regarding diet and physical activity can help children implement positive health behaviors in their everyday life. Content of the program and adequate training of teachers and staff can result in implementation of successful obesity prevention interventions. Further, existing evidence-based guidelines can be used as the foundation for developing, implementing, and evaluating obesity prevention interventions.
This meta-evaluation study provides insight into the quality of existing school-based intervention study evaluated on the selected criteria for evaluation. The studies included in this meta-evaluation varied in terms of design, sample size, observation period, outcomes considered, measurements, methodology, and recentness of the study. All of these criteria discussed here are helpful in evaluating an intervention for its replicability and applicability to other populations.
The studies selected for meta-evaluation used different study designs-experimental, pre-experimental, and quasi-experimental. The experimental studies obtained more points for their design, followed by quasi-experimental study design, suggesting robustness of these studies in terms of their design. For interventions focusing on preventive strategies, the purpose was to design an intervention strategy which is effective in the population being tested as well as generalizable to other populations. Thus, both experimental and quasi-experimental designs seem to be appropriate for the interventions focusing on prevention.
A large sample size is more representative of a population and limits the effect of outliers or extreme observations. Most of the studies included had sample size less than 500, which is adequate for statistical analyses, but not for generalization. However, sample sizes above 1000 are more feasible and large sample sizes were used by only three studies with either experimental or quasi-experimental design. Studies with large sample size are warranted for to evaluate generalizability of these interventions. Overall, lowest points were assigned for sample size for most of the studies.
Regarding observation period, most of the studies scored lower points, i.e., they had a shorter observation period, either ≤ 3 months, 4-6 months or 7-9 months. All the studies included focused on change in behavior, i.e. nutrition and/or physical activity, as one of the primary outcome. Furthermore, it is also important to assess the duration for which individuals retain the change in behavior. Thus, longer duration of observation period is more effective at assessing post-intervention change in the outcome. Most of the pre-experimental studies had longer observation period compared to experimental or quasi-experimental studies.
Almost all of the studies used self-reported standard measures;a few studies provided objective verification for all the measures used. This suggests that the interventions were assessed with appropriate measurement of outcomes and can be used effectively and reliably. Experimental studies had higher points for quality of measurement followed by pre-experimental studies.
Physical activity and dietary intake are the most important outcomes that are often assessed for obesity interventions. A majority of studies evaluated both change in physical activity and dietary intake as a primary outcome. All of the intervention studies showed positive change in these outcomes, which suggests that these interventions were effective in promoting change in behavior. In addition, some of the interventions were theory-based, whereas others did not use any theory for designing intervention. Theory enhances understanding of complex situations and is important for identifying the range of factors that might modify the situation. Furthermore, theory provides a basis for evaluating elements of a program and further improvement of existing programs.
2021 Copyright OAT. All rights reserv
All the studies provided comprehensive description of the methodology, including description of setting, population characteristics, intervention, and statistical analyses. Furthermore, all intervention studies reviewed were conducted after 2001, with most of them being very recent (i.e., after 2008). The more recent the study, the more relevant it is because these studies tend to use newer prevention strategies and technologies. With time, there are changes in demographics, socioeconomic status, lifestyle, etc., which warrants newer interventions. Since the studies are recent, the interventions assessed can be used in other populations-children and adolescents for prevention of obesity.
Schools can promote a sense of community and support for children. Further, schools can also involve parents or families in childhood obesity prevention programs, which can further influence a child’s behavior. Few studies demonstrated success of after school-based programs. These programs can involve parents or families in the intervention. In addition, programs that use teen or peer mentoring might provide inexpensive and effective strategies for motivating children for a healthier lifestyle. Children often look up to their peers often look up others in their community and are motivated to adopt healthy lifestyle behaviors. This strategy is specifically beneficial in rural areas, where there is a lack of formal health education programs. Another important aspect is duration of these intervention programs. A school-based setting offers opportunities for longer duration of these interventions. Having a program integrated into curriculum and providing health-related knowledge over a period of time may help children adopt these healthier habits and retain it in their life.
The search strategy included only published literature; this may have excluded some of the effective interventions. Further, we included interventions targeting rural and Appalachian children. Studies with no clear specification of interventions in rural population were, thus, excluded. Despite these limitations, this review provides insights into the existing interventions for prevention of obesity. Further, this review examines the quality and applicability of interventions.
Conclusion
The meta-evaluation of the intervention studies provided a meaningful evaluation of the quality of the research focusing on interventions for prevention of obesity in rural-dwelling children. Overall, studies reported positive change in behavior regarding physical activity and dietary intake, suggesting the importance and effectiveness of these interventions in prevention of obesity. Further, the variation in scores suggests wide range of quality and rigor in the design and implementation of these interventions.
References
- (2014) Centers for Disease Control and Prevention. Overweight and obesity: childhood obesity facts.
- Reilly JJ (2006) Obesity in childhood and adolescence: evidence based clinical and public health perspectives. Postgrad Med J 82: 429-437. [Crossref]
- Ogden CL, Carroll MD, Kit BK, Flegal KM (2012) Prevalence of obesity and trends in body mass index among US children and adolescents, 1999-2010. JAMA 307: 483-490. [Crossref]
- (2009) Robert Wood Johnson Foundation. Facts about childhood obesity.
- (2012) Centers for Disease Control and Prevention. Overweight and obesity: basics about childhood obesity. Centers for Disease Control and Prevention.
- Washington RL (2008) Metabolic syndrome – No longer an adult only disease. The Journal of Pediatrics 152: A1.
- Daniels SR (2005) Regulation of body mass and management of childhood overweight. Pediatr Blood Cancer 44: 589-594. [Crossref]
- Patterson PD, Moore CG, Probst JC, Shinogle JA (2004) Obesity and physical inactivity in rural America. J Rural Health 20: 151-159. [Crossref]
- (2010) Robert Wood Johnson Foundation. F as in fat: How obesity policies are failing in America, Washington, DC: Trust for America’s Health.
- Horodynski MA, Hoerr S, Coleman G (2004) Nutrition education aimed at toddlers: a pilot program for rural, low-income families. Fam Community Health 27: 103-113. [Crossref]
- Wood D (2003) Effect of child and family poverty on child health in the United States. Pediatrics 112: 707-711. [Crossref]
- Lutfiyya MN, Lipsky MS, Wisdom-Behounek J, Inpanbutr-Martinkus M (2007) Is rural residency a risk factor for overweight and obesity for U.S. children? Obesity (Silver Spring) 15: 2348-2356. [Crossref]
- (2013) Effective Health Care Program. Childhood obesity prevention programs: Comparative effectiveness review and meta-analysis.
- (2014) Office of Disease Prevention and Health Promotion. Healthy People 2020.
- (2014) Appalachian Regional Commission. The Appalachian Region.
- Health Resources and Services Administration. Defining the rural population.
- Chapman LS; American Journal of Health Promotion Inc (2005) Meta-evaluation of worksite health promotion economic return studies: 2005 update. Am J Health Promot 19: 1-11. [Crossref]
- Canavera M, Sharma M, Murnan J (2008) Development and pilot testing a social cognitive theory-based intervention to prevent childhood obesity among elementary students in rural Kentucky. Int Q Community Health Educ 29: 57-70. [Crossref]
- Carrel AL, Clark RR, Peterson SE, Nemeth BA, Sullivan J, et al. (2005) Improvement of fitness, body composition, and insulin sensitivity in overweight children in a school-based exercise program: a randomized, controlled study. Arch Pediatr Adolesc Med 159: 963-968. [Crossref]
- Cason KLL, B.N. (2006) Educational Intervention Improves 4th-Grade Schoolchildren's Nutrition and Physical Activity Knowledge and Behaviors. Top Clin Nutr 21: 234-240.
- Cohen JF, Kraak VI, Choumenkovitch SF, Hyatt RR, Economos CD (2014) The CHANGE study: a healthy-lifestyles intervention to improve rural children's diet quality. J Acad Nutr Diet 114: 48-53. [Crossref]
- Cottrell L, Spangler-Murphy E, Minor V, Downes A, Nicholson P, et al. (2005) A kindergarten cardiovascular risk surveillance study: CARDIAC-Kinder. Am J Health Behav 29: 595-606. [Crossref]
- Craven KW, Moore JB, Swart AS, et al. (2011) School-based nutrition education intervention: effect on achieving a healthy weight among overweight ninth-grade students. J Public Health Manag Pract 17: 141-146. [Crossref]
- Drummond RL, Staten LK, Sanford MR, et al. (2009) A pebble in the pond: the ripple effect of an obesity prevention intervention targeting the child care environment. Health Promot Pract 10: 156S-167S. [Crossref]
- Gombosi RL, Olasin RM, Bittle JL (2007) Tioga County Fit for Life: a primary obesity prevention project. Clin Pediatr (Phila) 46: 592-600. [Crossref]
- Greening L, Harrell KT, Low AK, Fielder CE (2011) Efficacy of a school-based childhood obesity intervention program in a rural southern community: TEAM Mississippi Project. Obesity (Silver Spring) 19: 1213-1219. [Crossref]
- Harrell TK, Davy BM, Stewart JL, et al. (2005) Effectiveness of a school-based intervention to increase health knowledge of cardiovascular disease risk factors among rural Mississippi middle school children. South Med J 98: 1173-1180. [Crossref]
- Hovland JA, McLeod SM, Duffrin MW, Johanson G, Berryman DE (2010) School-based screening of the dietary intakes of third graders in rural Appalachian Ohio. J Sch Health 80: 536-543. [Crossref]
- Ling J, King KM, Speck BJ, Kim S, Wu D (2014) Preliminary assessment of a school-based healthy lifestyle intervention among rural elementary school children. J Sch Health 84: 247-255. [Crossref]
- Morgan AZ, Ulrich P, Simmons KP, et al. (2014) Effectiveness of a multi-faceted, school-based health intervention program with 4th graders in Alabama. Children and Youth Services Review 37: 46-54.
- Muth ND, Chatterjee A, Williams D, Cross A, Flower K (2008) Making an IMPACT: effect of a school-based pilot intervention. N C Med J 69: 432-440. [Crossref]
- Pate RR, Saunders RP, Ward DS, Felton G, Trost SG, et al. (2003) Evaluation of a community-based intervention to promote physical activity in youth: lessons from Active Winners. Am J Health Promot 17: 171-182. [Crossref]
- Puma J, Romaniello C, Crane L, Scarbro S, Belansky E, et al. (2013) Long-term student outcomes of the Integrated Nutrition and Physical Activity Program. J Nutr Educ Behav 45: 635-642. [Crossref]
- Schetzina KE, Dalton WT 3rd, Lowe EF, Azzazy N, VonWerssowetz KM, et al. (2009) A coordinated school health approach to obesity prevention among Appalachian youth: the Winning with Wellness Pilot Project. Fam Community Health 32: 271-285. [Crossref]
- Schetzina KE, Dalton WT, 3rd, Pfortmiller DT, et al. (2011) The Winning with Wellness pilot project: rural Appalachian elementary student physical activity and eating behaviors and program implementation 4 years later. Fam Community Health 34: 154-162. [Crossref]
- Smith LH1 (2011) Piloting the use of teen mentors to promote a healthy diet and physical activity among children in Appalachia. J Spec Pediatr Nurs 16: 16-26. [Crossref]
- Smith LH, Holloman C (2014) Piloting "sodabriety": a school-based intervention to impact sugar-sweetened beverage consumption in rural Appalachian high schools. J Sch Health 84: 177-184. [Crossref]
- Struempler BJ, Parmer SM, Mastropietro LM, et al. (2014) Changes in fruit and vegetable consumption of third-grade students in body quest: food of the warrior, a 17-class childhood obesity prevention program. J Nutr Educ Behav 46: 286-292. [Crossref]
- Williamson DA, Champagne CM, Harsha DW, Han H, Martin CK, et al. (2012) Effect of an environmental school-based obesity prevention program on changes in body fat and body weight: a randomized trial. Obesity (Silver Spring) 20: 1653-1661. [Crossref]

