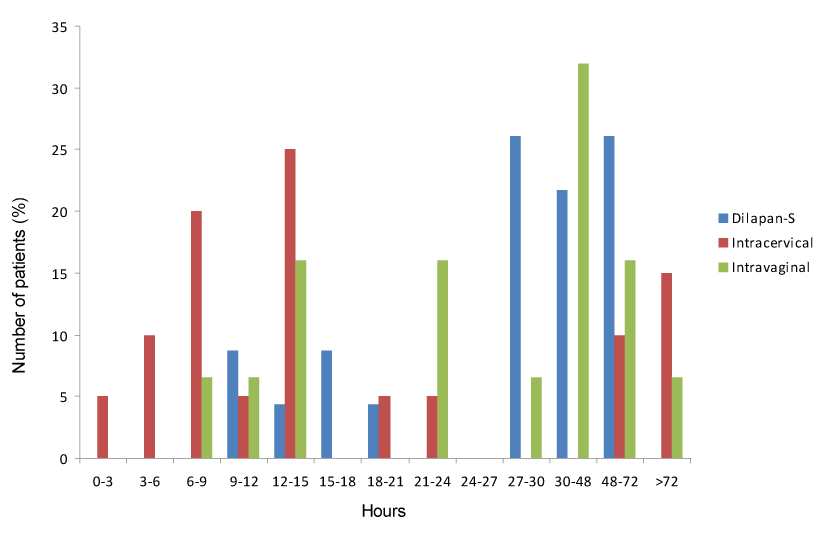Abstract
Aim: To compare the efficacy & safety of hygroscopic cervical dilator versus two prostaglandin E2 application methods for term induction of labour.
Method: Above 36th weeks of gestation, all women, who were admitted to hospital for induction of labour, were labour induced either with the hygroscopic cervical dilator between February till May 2015 versus intravaginal 1 mg or intracervical 0.5 mg prostaglandin E2 between March 2013 to August 2013 irrespective of cervical Bishop score. The main outcome variables were induction-to-delivery interval, number of foetal blood samples, PDA rate, rate of oxytocin augmentation and rate of vaginal delivery.
Results: Sixty-three patients were enrolled in this study (Dilapan-S n=26, intracervical n=20, intravaginal n=19). There were no differences between the three groups in respect to maternal age, gravity, parity, gestational diabetes, previous conisation of the cervix, previous caesarean section rate, reason for labour induction, gestational age and Bishop score. Outcome parameters showed that the induction-to-delivery was statistically significantly shorter in the intracervical compared to the Dilapan-S or the intravaginal group (median 12.8 h (intracervical) versus 31.7 h (Dilapan-S) or 29.9 h (intravaginal); p=0.03). No difference in induction-to-delivery time was found between Dilapan-S and intravaginal PGE2 (p>0.05).
Summary: The intracervical PEG2 had the shortest induction-to-delivery time in comparison to intravaginal PEG2 and mechanical induction with Dilapan-S. With intracervical PEG2 high levels of uterine hyper stimulation (25%) were detected which all required pharmacological intervention with Ferenterol. Intravaginal PEG2 only rarely caused uterine hyper stimulation, whereas Dilapan-S showed no hyper stimulation at all.
Introduction
The oldest reported method for induction of labour is mechanical dilation by insertion of a foreign body into the cervix, which is widely used today [1]. The use of mammary stimulation and manual dilation of the cervical canal to produce uterine contraction where first described by Hippocrates [1,2]. Till the mid-20th century similar methods were used for labour induction like balloon-tipped catheters, Laminaria tents or pressurised douches [1]. With the discovery of oxytocin in the early 1900s [3] and in the 1960s that exogenously applied prostaglandins can efface and dilate the uterine cervix [4] obstetricians have two options of induction of labour: mechanical and pharmacological methods.
Mechanical methods include osmotic dilators, for example luminaria tents, which are derived from seaweed, and 2 synthetic variants: Dilapan-S (Medicem international GmbH, Switzland) and Lamicel. Lamicel is a combination pharmaceutical containing up to 500 mg of magnesium and mechanical dilator. Several studies demonstrated some efficacy of labour induction without increased maternal or neonatal morbidity [5-7], however due to lack of large-scale trials there are insufficient data regarding safety of induction at term. Dilapan-S is composed of polyacrylonitrile and exerts clinical effects in 2 to 4 hours [8]. Early versions of Dilapan-S had concerns regarding infection. These concerns were partly due to the potential for introducing genital microorganisms [9] as well as device fragmentation requiring removal under ultrasound guidance [10]. These concerns have largely been eliminated due to improved advances in technology; however, data on the efficacy of these devices of labour induction at term are missing.
The alternative mechanical dilators are balloon catheters, which currently can be used for term cervical ripening and labour induction. The Foley catheter [11,12] is commonly used and an intracervical double-balloon catheter has recently been introduced [13,14].
Various pharmacological prostaglandin E2 (PGE2) preparations are available, which have been used by various routes, including local (intracervical (Pfizer Pharma) and intravaginal (Pfizer Pharma)) and general administration (oral, intramuscular, and intravenous) [15].
This study was carried out to examine whether at term Dilapan-S versus PGE2 administration has a different induction time and maternal as well as foetal outcome.
Materials and methods
All women, who were admitted to hospital for labour induction with a singleton foetus in vertex presentation, at or above 36 + 1 gestation age and absence of active labour, were enrolled for this study from January to May 2015 for Dilapan-S and March 2013 to August 2013 for PEG2. Exclusion criteria were multiple pregnancies and previous caesarean section. This cohort analysis was done to assess safety and efficacy of newly available Dilapan induction. All patients gave their informed consent. After Dilapan-S induction intravaginally PEG2 (Minprostin) was carried out irrespective of the Bishop score.
The patient’s baseline characteristics and reasons for induction are presented in Table 1 and 2.
Table 1. Baseline characteristics of the study population of mean (M), ± standard deviation (SD), and median [n. s. = non-significant difference, p > 0.05].
|
Dilapan-S (n = 24)
M ± SD (median) |
Cervical (n = 20)
M ± SD (median) |
Intravaginal (n = 19)
M ± SD (median) |
p value |
Maternal age (years) |
33.9 ± 2.4 (35) |
34.2 ± 4.5 (34) |
32.5 ± 3.9 (32) |
n. s. |
Gravity |
1.7 ± 0.8 (2) |
2.2 ± 1.3 (2) |
1.8 ± 1.8 (1) |
n. s. |
Parity |
0.4 ± 0.6 (0) |
0.7 ± 0.7 (1) |
0.3 ± 0.6 (0) |
n. s. |
Gestational age (weeks) |
39.8 ± 1.4 (40) |
39.6 ± 1.5 (40) |
39.7 ± 1.1 (40) |
n. s. |
Bishop score |
2.9 ± 1.5 (3) |
3.8 ± 1.3 (4) |
3.5 ± 1.3 (3) |
n. s. |
BMI (kg/m2) |
23.2 ± 5.8 (22.0) |
23.8 ± 4.6 (23.1) |
23.4 ± 3.4 (22.7) |
n. s. |
Number of Dilapan-S rods |
4.0 ± 1.1 (4) |
- |
- |
- |
New-born birth weight (kg) |
3470 ± 606 (3370) |
3640 ± 401 (3685) |
3556 ± 479 (3600) |
n. s. |
Table 2. Reason for induction of labour and outcome after induction of labour with either Dilapan-S, intracervical or intravaginal PGE2 [n. s.= non-significant difference, p > 0.05].
|
Dilapan-S (n =24)
n (%) |
Cervical (n=20)
n (%) |
Intravaginal (n=19)
n (%) |
p value |
Reason for induction of labour |
|
n. s. |
Post date |
9 (43) |
6 (30) |
7 (37) |
Premature rupture of membranes |
4 (19) |
4 (20) |
5 (26) |
Preeclampsia |
2 (10) |
3 (15) |
2 (11) |
On request |
4 (19) |
4 (20) |
1 (5) |
Other |
0 (0) |
3 (15) |
1 (5) |
Gestational diabetes |
1 (5) |
0 (0) |
1 (5) |
IUGR |
1 (5) |
0 (0) |
1 (5) |
Macrosomia |
0 (0) |
0 (0) |
1 (5) |
Peridural anesthesia |
8 (38) |
9 (45) |
10 (53) |
n. s. |
Oxytocin augmentation |
8 (38) |
8 (40) |
9 (47) |
n. s. |
Mode of delivery |
|
n. s. |
Vaginal birth (without operative delivery) |
15 (71) |
13 (65) |
9 (47) |
Vacuum extraction / forceps |
0 (0) |
2 (10) |
2 (11) |
Caesarean section |
6 (29) |
5 (25) |
8 (42) |
Number of fetal blood sampling (n) |
|
n. s. |
0 |
19 (90) |
14 (70) |
15 (79) |
1 |
1 (5) |
4 (20) |
1 (5) |
2 |
1 (5) |
1 (5) |
1 (5) |
3 |
0 (0) |
1 (5) |
1 (5) |
All patients in the Dilapan-S group were placed in the lithotomy position and a speculum examination was done to identify the cervix. The insertions of the Dilapan-S rods were done under visual control. The maximum of rods without causing discomfort were noted. The maximum numbers of Dilapan-S rods were 5. The inserted rods were removed when the patient was in active labour or on the next day (< 24 hours). After removing of the rods and if the patient was not in active labour all patients received intravaginal PGE2 1 mg (Minprostin©).
Similarly, all patients in the intracervical PGE2 group were placed in the lithotomy position and a speculum examination was done to identify the cervix. The insertion of a cannula in the cervix and application of the 0.5 mg PEG2 gel (Pepidil©) were carried out whilst viewing the cervix. In the absence of regular contraction, another 0.5 mg gel was applied into the cervix using the same procedure.
All patients in the intravaginal PGE2 group received first 1 mg (Minprostin©) and in the absence of regular contraction another 2 mg was applied after 6 to 8 hours. On the 2nd day of induction, initially 2 mg and after 6 to 8 hours another 1 mg were applied if no regular contraction was felt by the patient.
All patients had fetal electrocardiography and electrohysterogram (Monica AN24) controls half an hour before Dilapan-S or gel application and half an hour after Dilapan-S or one hour after gel application whilst lying on the right or left side. No further intervention was carried out if contractions exceeded 2 per 10 minutes. Dilapan-S was removed the next morning after 16-24 hours or when the patient was in labour with cervical dilatation. After one day of three or more Dilapan-S rods a switch to intravaginal PEG2 gel (Minprostin©) was carried out. For gel application a switch of gel was allowed after three days of failed induction. In the presence of > 2 contractions per 10 minutes, failure of cervical dilatation (>1 cm/h) or failure to progress during the active first (cervix dilation >3 cm) and second stages of labour, management required initiation of intravenous oxytocin by infusion was started >6 h after the last dose of gel. Electrocardiotocography was intermittent during active phase of labour (cervical dilatation >3 cm) and continuous if in the active phase of labour the foetal heart rate was suspect or pathological. During 2nd stage of labour, continuous foetal monitoring was carried out.
The outcome parameters were the induction-to-delivery interval (from insertion of first rods or gel to birth), number of foetal blood samples, PDA rate, rate of oxytocin augmentation, 5 min and 10 min Apgar score, and arterial pH value.
The data analysis used SPSS (Version 21, IBM© SPSS© Statistics). Differences between groups were tested by a nonparametric Kruskal-Wallis-Test. Two-side p values were reported for all tests and a value < 0.05 was regarded as significant.
Results
Sixty-three patients were enrolled in this study. Twenty-four were in the Dilapan-S group, 20 patients in the cervical group and 19 in the intravaginal group. There were no differences between the three groups in respect to maternal age, gravity, parity, gestational diabetes, previous conisation of the cervix, pervious caesarean section rate, reason for labour induction, gestational age and Bishop score (Tables 1 and 2; Figure 1).
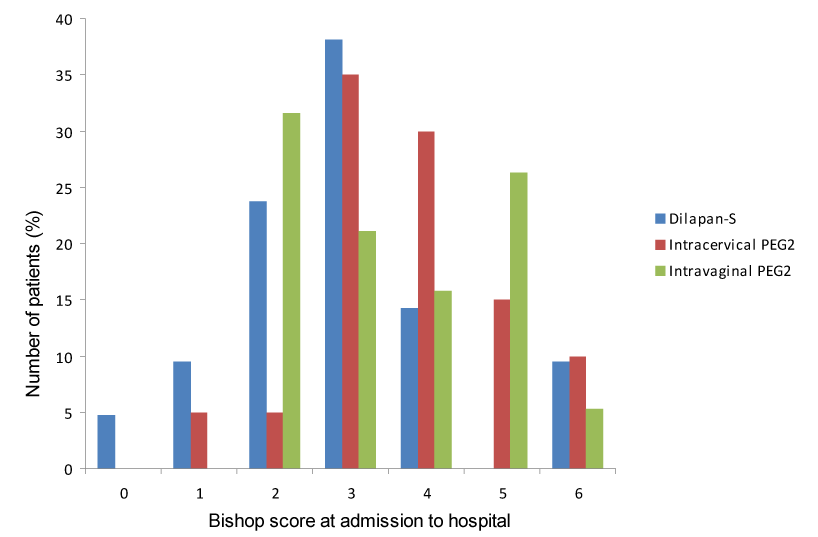
Figure 1. Bishop score at admission to hospital.
Outcome parameters (Table 2 & 3) showed that the induction-to delivery was statistically significantly shorter in the intracervical compared to the Dilapan-S or the intravaginal group (median 12.8 h (intracervical) versus 31.7 h (Dilapan-S) or 29.9 h (intravaginal); p = 0.03; Figure 2). No difference in induction-to-delivery time was found between Dilapan-S and intravaginal PGE2 (p>0.05).
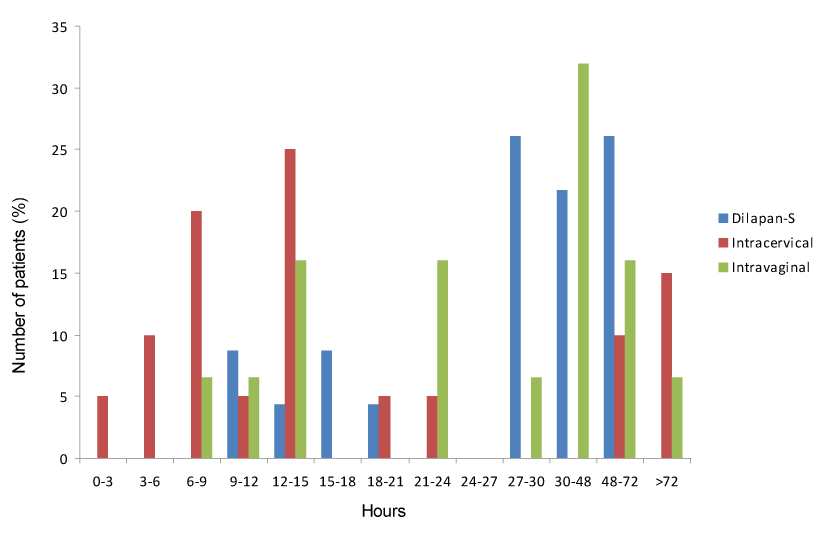
Figure 2. Induction-to-delivery time (h) of the three study groups.
Table 3. Outcome after induction of labour of mean (M), ± standard deviation (SD), and median [n. s.: non-significant difference, p > 0.05].
|
Dilapan-S (n=24)
M ± SD (median) |
Cervical (n=20)
M ± SD (median) |
Intravaginal (n=19)
M ± SD (median) |
p value |
Induction-to-delivery (hours) |
35 ± 18 (31.7) |
38 ± 63 (12.8) |
42 ± 12 (29.9) |
0.03 |
Hypertstimulation (n (%)) |
0 (0) |
6 (25.0) |
1 (5.3) |
n. s. |
Arterial pH value |
7.23 ± 0.08 (7.21) |
7.20 ± 0.08 (7.22) |
7.23 ± 0.07 (7.22) |
2021 Copyright OAT. All rights reserv
n. s. |
5 min Apgar |
9.8 ± 0.5 (10) |
9.8 ± 0.5 (10) |
9.8 ± 0.1 (10) |
n. s. |
10 min Apgar |
10 ± 0 (10) |
10 ± 0 (10) |
10 ± 0.2 (10) |
n. s. |
Number of induction |
2.1 ± 1.2 (2) |
2.4 ± 2.2 (1) |
2.0 ± 0.9 (2) |
n. s. |
With intracervical PEG2 high levels of uterine hyper stimulation (25%) were detected which all required pharmacological intervention with ferenterol. Intravaginal PEG2 only rarely (5%) caused uterine hyper stimulation, whereas Dilapan-S showed not hyper stimulation at all.
Discussion
Our results show that intracervical PGE2 administration had a shorter induction-to-delivery time in comparison to mechanical induction rods (Dilapan-S) and intravaginal PGE2. This result is contrary to the current Cochrane database review, which included 11 trials [16]. This difference might be partially explained due to the fact that previous studies inserted the cannula into the cervix during a vaginal examination and not under direct visual control as in our study [15]. Insertion of the cannula into the cervix during a vaginal examination is very difficult if the cervix is unripe (low Bishop score).
In women with low Bishop scores several research studies tried to define the most efficacious method of labour induction. Morzurkewich et al. [17] evaluated current modes of labour induction, giving particular attention to a subgroup of women with unfavourable cervices. Mechanical methods resulted in higher vaginal delivery rates than the use of oxytocin alone in the low Bishop score group (3 studies, 178 women; RR 0.50; 95% CI, 0.29-0.87) [17,18,16]. A recent Cochrane database review on mechanical induction [18] had difficulties to generalise study results due to the lack of standardisation in the dosing regimens in the pharmaceutical arms. No difference in caesarean delivery rate was identified when comparing mechanical induction methods to pharmacologic induction methods [17,18,16], however mechanical methods were associated with a significantly lower rate of uterine hyper stimulation, with and without fetal heart rate changes, when compared with prostaglandin preparations [19-21]. No hyper stimulation was seen in our Dilapan-S study group, whereas in the intracervical study group several patients (n=5, 25%) required intravenous Fenoterol for uterine hyper stimulation. In the intravaginal study group two patients also had uterine hyper stimulation for a short duration, but no Fenoterol was required.
Mechanical methods demonstrated a lower rate of operative vaginal delivery rate [17,18], however no difference were detected in our study due to the small sample size.
In Germany for unripe cervical scores and trial of labour after caesarean section mechanical device is the only allowed induction method since all pharmacological agents are “off label” use with known legal implications. With 1 prior caesarean birth Bujold et al. [22] described no significant differences in rates of uterine rupture when comparing women who received Foley catheter for labour induction with women who laboured spontaneously. Two further retrospective studies reported similar results [23,24], but one retrospective study showed an increase [25]. Hoffman et al. commented that causation for this risk increase is difficult. Currently, strong evidence for an increased rupture rate in the women after caesarean section are rare, and ACOG currently states that cervical ripening with Foley catheter may be an option of women with unfavourable cervix desiring trial of labour after caesarean section [26].
Most studies have excluded women with ruptured membranes due to the concern for increased infectious morbidity when a foreign body is introduced into the cervix [27]. Four patients with premature rupture of membranes where in included in the Dilapan-S study group and all had no neonatal or maternal infections. Further studies are required to test whether mechanical induction in women with premature rupture of membranes and unfavourable cervices could decrease length of labour and thereby decrease infection rates.
The major limitation of this study is the study design (cohort group analysis) and small sample size.
Conclusion
The intracervical PEG2 had the shortest induction-to-delivery time in comparison to intravaginal PEG2 and mechanical induction with Dilapan-S. With intracervical PEG2 high levels of uterine hyper stimulation (25%) were detected which all required pharmacological intervention with ferenterol. Intravaginal PEG2 only rarely (5%) caused uterine hyper stimulation, whereas Dilapan-S showed not hyper stimulation at all. Dilapan-S is an ideal candidate for women with a prior caesarean section due to the current contraindications of the pharmacological induction agents. Potentially, for outpatient cervical ripening Dilapan-S might also be a candidate [28]. Further prospective randomised trials are required to test the preliminary pilot trial results.
References
- Sciscione AC (2014) Methods of cervical ripening and labor induction: mechanical. Clin Obstet Gynecol 57: 369-376. [Crossref]
- Mackenzie IZ (2006) Induction of labour at the start of the new millennium. Reproduction 131: 989-998. [Crossref]
- Bell WB (1909) The pituitary body and the therapeutic value of the infundibular extract in shock, uterine atony, and intestinal paresis. Br Med J 2: 1609-1613. [Crossref]
- Karim SM, Trussell RR, Patel RC, Hillier K (1968) Response of pregnant human uterus to prostaglandin-F2-alpha-induction of labour. Br Med J 4: 621-623. [Crossref]
- Bagratee JS, Moodley J (1990) Synthetic laminaria tent for cervical ripening. S Afr Med J 78: 738-741. [Crossref]
- Berkus MD, Laufe LE, Castillo M (1990) Lamicel for induction of labor. J Reprod Med 35: 219-221. [Crossref]
- Johnson IR, Macpherson MB, Welch CC, Filshie GM (1985) A comparison of Lamicel and prostaglandin E2 vaginal gel for cervical ripening before induction of labor. Am J Obstet Gynecol 151: 604-607. [Crossref]
- Chambers DG, Willcourt RJ, Laver AR, Baird JK, Herbert WY (2011) Comparison of Dilapan-S and laminaria for cervical priming before surgical pregnancy termination at 17-22 weeks’ gestation. Int J Womens Health 3: 347-52. [Crossref]
- Evaldson GR, Fianu S, Jonasson A, Larsson B, Nord CE, et al. (1986) Does the hygroscopic property of the laminaria tent imply a risk for ascending infection in legal abortions? A microbiological study. Acta Obstet Gynecol Scand 65: 257-261. [Crossref]
- Lichtenberg ES (2004) Complications of osmotic dilators. Obstet Gynecol Surv 59: 528-536. [Crossref]
- Gibson KS, Mercer BM, Louis JM (2013) Inner thigh taping vs traction for cervical ripening with a Foley catheter: a randomized controlled trial. Am J Obstet Gynecol 209: 272. [Crossref]
- Delaney S, Shaffer BL, Cheng YW, Vargas J, Sparks TN, et al. (2010) Labor induction with a Foley balloon inflated to 30 mL compared with 60 mL: a randomized controlled trial. Obstet Gynecol 115: 1239-1245. [Crossref]
- Atad J, Hallak M, Ben-David Y, Auslender R, Abramovici H (1997) Ripening and dilatation of the unfavourable cervix for induction of labour by a double balloon device: experience with 250 cases. Br J Obstet Gynaecol 104: 29-32. [Crossref]
- Salim R, Zafran N, Nachum Z, Garmi G, Kraiem N, et al. (2011) Single-balloon compared with double-balloon catheters for induction of labor: a randomized controlled trial. Obstet Gynecol 118: 79-86. [Crossref]
- Reinhard J, Rösler R, Yuan J, Schiermeieret S, Herrmann E, et al. (2014) Prostaglandin E2 labour induction with intravaginal (Minprostin) versus intracervical (Prepidil) administration at term: randomized study of maternal and neonatal outcome and patient’s perception using the Osgood semantic differential scales. BioMed Research International.
- Boulvain M, Kelly A, Irion O. Intracervical prostaglandins for induction of labour. The Cohrane Database of Systematic Reviews; 1, Article ID CD006971, 2008.
- Mozurkewich EL, Chilimigras JL, Berman DR, Perni UC, Romero VC, et al. (2011) Methods of induction of labour: a systematic review. BMC Pregnancy Childbirth 11: 84. [Crossref]
- Jozwiak M, Bloemenkamp KW, Kelly AJ, Mol BW, Irion O, et al. (2012) Mechanical methods for induction of labour. Cochrane Database Syst Rev 3: CD001233. [Crossref]
- Sciscione AC, Nguyen L, Manley J, Pollock M, Maas B, et al. (2001) A randomized comparison of transcervical Foley catheter to intravaginal misoprostol for preinduction cervical ripening. Obstet Gynecol 97: 603-607. [Crossref]
- Fox NS, Saltzman DH, Roman AS, Klauser CK, Moshier E, et al. (2011) Intravaginal misoprostol versus Foley catheter for labour induction: a meta-analysis. BJOG 118: 647-654. [Crossref]
- Jagielska I, Kazdepka-ZiemiÅska A, Janicki R, Fórmaniak J, Walentowicz-SadÅ‚ecka M, et al. (2013) [Evaluation of the efficacy and safety of Foley catheter pre-induction of labor]. Ginekol Pol 84: 180-185. [Crossref]
- Bujold E, Blackwell SC, Gauthier RJ (2004) Cervical ripening with transcervical foley catheter and the risk of uterine rupture. Obstet Gynecol 103: 18-23. [Crossref]
- Ben-Aroya Z, Hallak M, Segal D, Friger M, Katz M, et al. (2002) Ripening of the uterine cervix in a post-cesarean parturient: prostaglandin E2 versus Foley catheter. J Matern Fetal Neonatal Med 12: 42-45. [Crossref]
- Ravasia DJ, Wood SL, Pollard JK (2000) Uterine rupture during induced trial of labor among women with previous cesarean delivery. Am J Obstet Gynecol 183: 1176-1179. [Crossref]
- Hoffman MK, Sciscione A, Srinivasana M, Shackelford DP, Ekbladh L (2004) Uterine rupture in patients with a prior cesarean delivery: the impact of cervical ripening. Am J Perinatol 21: 217-222. [Crossref]
- American College of Obstetricians and Gynecologists (2010) ACOG Practice bulletin no. 115: Vaginal birth after previous cesarean delivery. Obstet Gynecol 116: 450-463. [Crossref]
- Heinemann J, Gillen G, Sanchez-Ramos L, Kaunitz AM (2008) Do mechanical methods of cervical ripening increase infectious morbidity? A systematic review. Am J Obstet Gynecol 199: 177-187. [Crossref]
- Sciscione AC, Muench M, Pollock M, Jenkins TM, Tildon-Burton J, et al. (2001) Transcervical Foley catheter for preinduction cervical ripening in an outpatient versus inpatient setting. Obstet Gynecol 98: 751-756. [Crossref]