Abstract
With worsening obesity epidemic, it has become an international health issue increasing not only morbidity and mortality, but also health care costs while decreasing the quality of life in general. Bariatric surgery has become a significant treatment for morbid obesity and patients with obesity who suffers from multiple medical comorbidities. Among the risks that bariatric surgery carries, intussusception is a rare long-term complication that may occur with gastric bypass, mostly described in case reports and small-scale retrospective study. These reported cases required operative reduction. Reports of spontaneous reduction are rarely reported. We present a patient who had
laparoscopic roux-en-y gastric bypass and presented with intussusception that spontaneous resolved within 24 hours. Diagnostic laparoscopy confirmed evidence of resolved intussusception and no further operative intervention was necessary. Bariatric surgeons should be vigilant of intussusception as a long-term complication, and may consider non-operative conservative management under certain presentation.
key words
intussusception, gastric bypass, spontaneous reduction
Introduction
In the United States, over 159 million adults and 37 million children are considered overweight or in obese category. The current obesity epidemic has become an international health issue with 1.46 billion adults falling into overweight or obese categories worldwide in 2008 [1]. In addition to the increasing health care costs and compromised quality of life, increased risks of associated illnesses such as metabolic disorders and hypertension, have caused significant morbidity and mortality. Roux-en-y gastric bypass is a highly successful approach for treating obesity with average loss of 60% to 70% of excess body weight [2]. Intussusception is an invagination of one segment of intestine into another, mostly seen in children. However, intussusception is very rare in adults, accounting for 1-5% of mechanical bowel obstruction [3], causes include malignancy, adhesions, and inflammatory bowel disease. There are rare reports of intussusception in post roux-en-y gastric bypass patients. Due to risk of bowel ischemia, all the diagnosed cases have been treated through immediate operative reduction of intussusception. However, operative intervention carries risks and depending on the presentation, conservative approach maybe considered. We present a patient with history of roux-en-y gastric bypass and now with retrograde intussusception that spontaneously reduced within 24 hours. She was managed mostly by clinical monitoring, supportive care, and repeat imaging. A non-emergent diagnostic laparoscopy was performed on the next day after spontaneous reduction was shown on CT scan. This case demonstrates the potential for conservative management based on clinical picture, and value of repeat imaging such as CT of abdomen for serial evaluation instead of emergent surgery.
Case
A 40 year-old woman with prior laparoscopic roux-en-y gastric bypass 3 years ago, presented with 1 day history of sharp left lateral abdominal pain that started suddenly, accompanied by nausea, vomiting, and obstipation. She denied any current medical conditions. Patient was hemodynamically stable and afebrile. On examination, her abdomen was tender in the left upper quadrant and epigastric area with radiation to back, but overall her abdomen was soft, non-distended, and non-peritoneal. Laboratory values were unremarkable except for a moderately elevated WBC at 12,900/µL. Otherwise; total bilirubin was 0.5 mg/dl, alkaline phosphatase 72 iu/L, AST 18 iu/L, ALT 22 iu/L, lipase 11 u/L and lactic acid 0.85 mml/L. She received a CT abdomen and pelvis with PO and IV contrast showing a small bowel intussusception jejunal-jejunal anastomosis site (Figure 1). No free air was visualized. Due to overall clinical stability, she was given IV hydration, placed on bowel rest, and monitored with serial abdominal exams. Over the next few hours, abdominal pain significantly improved. Subsequently, a repeat CT abdomen and pelvis was obtained, which showed a complete resolution of the small bowel intussusception with only residual edematous loops of small bowel at the initially involved section, and previous residual oral contrast had now passed through to the colon and rectum (Figure 2).
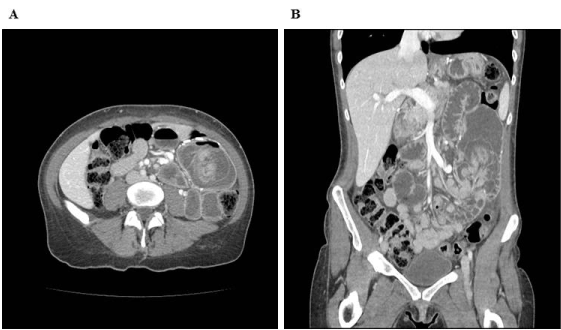
Figure 1: Dilated small bowel loop in the left midabdomen, receiving an extended segment of small bowel measuring 12cm in length, representing intussusception. A) Horizontal plane. B) Coronal plane.
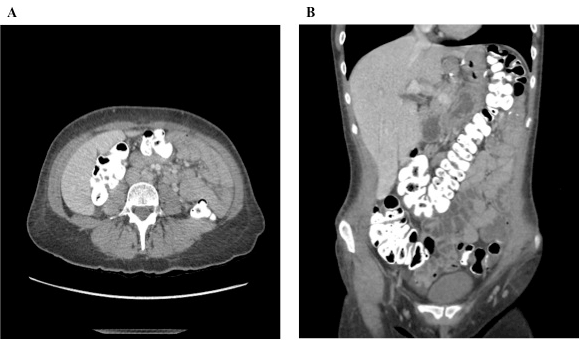
Figure 2: Resolution of the small bowel intussusception. Multiple small bowel loops appear edematous with mucosal enhancement at the site of previous intussusception within the left abdomen. There is passage of residual oral contrast given prior has passed through the colon and rectum. No evidence of obstruction or perforation was seen. A) Horizontal plane. B) Coronal plane.
Despite the resolution and improved clinical exam, her increasing leukocytosis with WBC of 15,500 /uL and persistent obstipation were concerning and a decision was made to proceed with an exploratory laparoscopy on the next day. Laparoscopy showed evidence of a previous intussusception that had spontaneous reduced with mild serosal erythema on the small intestine. There was no internal hernia or abnormal mass found. No intraoperative intervention was performed. The patient recovered well with resolution of her abdominal pain. She resumed normal bowel function and was able to tolerate a gastric bypass stage diet. Her leukocytosis resolved on the next day and she was discharged from hospital on postoperative day 1. At office follow up, she continued to do well with no further symptoms.
Discussion
More common among pediatric population, intussusception is an invagination of typically proximal segment of intestine into lumen of distal segment. Causes of intussusception in children are multiple including idiopathic, viral gastroenteritis, bacterial enteritis, Meckel diverticulum, tumor, hematoma, vascular malformations, cystic fibrosis, and celiac disease [4]. Causes are typically primary in nature and benign, and non-operative intervention pneumatic reduction is the first line of therapy. However, intussusception is rare in adults, accounting for 5% of all intussusceptions [3,5]. In adults, 90% of the intussusception is usually secondary to a pathologic process with malignancy accounting for majority of the cases, while 8-20% of cases are idiopathic. Other causes include adhesions, inflammatory bowel disease, and from jejunostomy feeding tubes.
In normal intussusception, the most likely involved segment involves junction between an intestinal segment that is freely moving and another that is adhered structure such as retroperitonium [4]. Intestinal lesions or irritants disrupt the normal peristaltic activity and lead to formation of intussusception. The exact etiology of intussusception after roux-en-y gastric bypass remains unclear and multiple etiologies have been proposed. Suggested causes include intestinal dysmotility, new lead point at suture/staple lines that may account for high incidence of intussusception at jejunal-jejunal anastomosis site, and change in composition of mesenteric fat secondary to weight loss that causes overall bowel instability and loss of cushion effect [6-8]. The etiology is most likely multifactorial and increasing awareness of this complication among physicians is critical to long-term management of bariatric patients.
Besides marginal ulcers, internal hernia, and malnutrition, intussusception has become recognized as a long-term complication of gastric bypass [9]. Among bariatric patients, current incidence of intussusception is 0.07-0.6%, but it was suggested the actual incidence may be higher due to potential for spontaneous reduction [10]. Common presenting symptoms are abdominal pain, nausea, vomiting, fever, constipation, and weight loss. Diagnosis is most often through CT of abdomen showing distended loop of bowel and characteristic “target sign” [11]. Most of the available literature is based on case reports [12-17]. Among the cases, most required an operative intervention, including direct reduction, reduction with plication, resection of bowel, and resection of bowel with revision of anastomosis. The largest review consisting of 71 patients, in which intussusception is found to be more common among female patients (98.6%) and most presented with abdominal pain and vomiting. Of these patients, 96% of patients required surgery, 70.6% of whom required anastomotic revision and 23.5% underwent reduction without resection [18]. However, cases of spontaneous reduction in post gastric bypass patients presenting with intussusception is rarely found. The review focused on 23 patients with gastric bypass and presented with intussusception, 9 of the patients were found to have spontaneous reduction, although some were reduced while running the bowel intraoperatively. All of these patients were operated upon and were found to have edema and hyperemia in the bowel segment involved [19]. Instead of immediate operative intervention often involving bowel resection and extended hospital stay along with risk of surgical complications, our case demonstrates the potential role of non-operative management. The patient had spontaneous reduction found on repeat CT scan 24 hours later before diagnostic laparoscopy without involvement of any resection. In selected patients, non-emergent, minimal intervention allows shorter hospital stay without potential risk of surgical complications.
In conclusion, we report the case of spontaneously reduced intussusception that did not require emergent operative intervention. Although a diagnostic laparoscopy was performed on the next day after intussusception was spontaneous reduced, no other operative interventions were required. Our patient did not show any signs of peritonitis and remained hemodynamically stable throughout the hospital course. In such case, potentially non-operative intervention may be applied in such case. Conservative treatment with careful observation, bowel rest, hydration, and repeat imaging 12-24 hours post-presentation maybe preferred in clinical stable patient without signs of peritonitis. Overall, clinicians should be aware of intussusception as a long-term complication of gastric bypass surgery, and instead of immediate surgical reduction, conservative treatment maybe an alternative management in selected patients.
References
- Go AS, Mozaffarian D, Roger VL, Benjamin EJ, Berry JD, et al. (2013) Heart disease and stroke statistics—2013 update: a report from the American Heart Association. Circulation 127: e6-e245. [Crossref]
- Buchwald H, Oien DM (2009) Metabolic/bariatric surgery Worldwide 2008. Obes Surg 19: 1605-1611. [Crossref]
- Koppman JS, Li C, Gandsas A (2008) Small bowel obstruction after laparoscopic Roux-en-Y gastric bypass: a review of 9,527 patients. J Am Coll Surg 206: 571-584. [Crossref]
- Paskauskas S, Pavalkis D (2012) Adult Intussusception. Current Concepts in Colonic Disorders. Dr. Lule G. (Edtr), ISBN: 978-953-307-957-8, InTech. [Available from: http://www.intechopen.com/books/current-concepts-in-colonic-disorders/adult-intussusception]. Accessed on October 17, 2016.
- Marinis A, Yiallourou A, Samanides L, Dafnios N, Anastasopoulos G, et al. (2009) Intussusception of the bowel in adults: a review. World J Gastroenterol 15: 407-411. [Crossref]
- Coster DD, Sundberg SM, Kermode DS, Beitzel DT, Noun SH, et al. (2008) Small bowel obstruction due to antegrade and retrograde intussusception after gastric bypass: three case reports in two patients, literature review, and recommendations for diagnosis and treatment. Surg Obes Relat Dis 4: 69-72. [Crossref]
- Duane TM, Wohlgemuth S, Ruffin K (2000) Intussusception after Roux-en-Y gastric bypass. Am Surg 66: 82-84. [Crossref]
- Zainabadi K, Ramanathan R (2007) Intussusception after laparoscopic Roux-en-Y gastric bypass. Obes Surg 17: 1619-1623. [Crossref]
- Schauer PR, Ikramuddin S, Gourash W, Ramanathan R, Luketich J (2000) Outcomes after laparoscopic Roux-en-Y gastric bypass for morbid obesity. Ann Surg 232: 515-529. [Crossref]
- Carilli S, Arisoy M2021 Copyright OAT. All rights reservfollowing laparoscopic Roux and Y gastric bypass: intussusception-case report. Springerplus 4: 603. [Crossref]
- Gayer G, Zissin R, Apter S, Papa M, Hertz M (2002) Pictorial review: adult intussusception--a CT diagnosis. Br J Radiol 75: 185-190. [Crossref]
- Wax JR, Wolff R, Cobean R, Pinette MG, Blackstone J, et al. (2007) Intussusception complicating pregnancy following laparoscopic Roux-en-Y gastric bypass. Obes Surg 17: 977-979. [Crossref]
- Al-Sabah S, Christou N (2008) Intussusception after laparoscopic Roux-en-Y gastric bypass. Surg Obes Relat Dis 4: 205-209. [Crossref]
- Tran D, Halmi D, Kolesnikov E (2009) Intussusception following Roux-en-Y gastric bypass: two case reports and literature review. Obes Surg 8: 1038.
- Sarhan M, Ahmed L, Miegge L (2010) Retrograde intussusception after Roux-en-Y gastric bypass. Am Surg 76: 454-456. [Crossref]
- Sanchez-Santos R, Gonzalez S, Lopez N (2009) Acute abdomen following laparoscopic Roux-en-Y gastric bypass: retrograde intussusception in jejunojejunostomy. Obes Surg 8: 1034.
- Shaw D, Huddleston S, Beilman G (2010) Anterograde intussusception following laparoscopic Roux-en-Y gastric bypass: a case report and review of the literature. Obes Surg 20: 1191-1194. [Crossref]
- Singla S, Guenthart BA, May L, Gaughan J, Meilahn JE (2012) Intussusception after laparoscopic gastric bypass surgery: an underrecognized complication. Minim Invasive Surg: 464853.
- Simper SC, Erzinger JM, McKinlay RD, Smith SC (2008) Retrograde (reverse) jejunal intussusception might not be such a rare problem: a single group’s experience of 23 cases. Surg Obes Relat Dis 4: 77–83.


