A female patient of 89 years (born in 1927), in a good health condition, living on her own in a house suffered a stroke in 2001, and in 2010 she was diagnosed with an inoperable brain tumour (meningioma). Apart from occasional memory loss and short term nausea she had no difficulties and could take care of herself. Following a visit by her relatives in December 2013 she suddenly lost consciousness, collapsed, and was lying on a stone floor until her relatives found her after the following two days. She developed an extensive pressure ulcer on her shoulder blades and on the occipital and parietal bone on her skull, accompanied by loss of hair, skin, and subcutaneous tissue up to the bone in the extent of 10 x 12 cm. After two months of hospitalisation at the Department of Neurology her general condition stabilised, she could communicate, but her mobility was limited. The pressure ulcer on her shoulder blade healed quite effectively, the manifestations on the cranium were stagnant, the pressure ulcer showed callous margins, and the bone was coloured dark brown to black. Since March 2014 the therapy included gel preparations, In May 2014 we commenced therapy using stem cells-fibroblasts, on a culture medium-cellulose wound dressing Hcel®NaT. The application of fibroblasts was concluded in July 2015. Until January 2016 Hcel®NaT was applied moistened only with the culture medium-a Nutrient Mixture F-12 Ham Formulation until the defect healed completely.
pressure ulcer on the occipital and parietal bone, stem cell therapy
Despite all the progress made in the field of medicine, pressure ulcers (bedsores) still are a problem in hospitalised patients as well as the patients in home care. The patients suffer and their life is at risk, the healthcare workers therefore see the management of pressure ulcers as one of their priorities. There are many specialised congresses dedicated to this topic. The aetiology of pressure ulcers is influenced by internal and external factors. There are more male tan female sufferers and the group at greatest risk are senior patients but also young patients after severe traumas.
The management of pressure ulcers includes complex measures (depending on the overall condition of the patient and local finding). What also is important is the therapy of underlying disease and the management of their overall physical condition. Therapeutic procedures include conservative therapy and surgery, depending on the stage of pressure ulcers. Topical therapy includes lavage with antiseptic solutions, ointments, moulds, modern dressing materials, (such as foam or silicone dressings, alginates, carbon dressings, modified cellulose, i.e. carboxymethyl cellulose, etc. Many dressing materials are combined with silver to potentiate antimicrobial properties). Innovative procedures include stem cell therapy using autologous or donor fibroblasts [1-4].
Preventive measures include active and passive mattresses, patient positioning, and measures to counteract infection, antibiotics, improved patient comfort, supported granulation and epithelisation. What is discussed at the moment is proper diet and nutrition of the patient [5-10].
Despite long term experience there are cases that can surprise physicians and traditional treatment methods need to be revaluated. When deciding about therapy to increase the quality of life of the patient, their age must not play a role.
A lively female patient of 89 years (born in 1927) lived alone in her house. She suffered as stroke in 2001, and in 2010 she was diagnosed with an inoperable brain tumour-meningioma. Apart from episodic memory loss and transient nausea she did not have any problems and was able to take care of herself. At the beginning of December 2013 after her relatives who visited her left, she lost consciousness and was lying on a stone floor until they came by two days after that. After two months of hospitalisation at the Department of Neurology her condition stabilised, she could communicate, but was left in a wheelchair. At the end of February 2014 she was released into home care. On her skin there were two extensive pressure ulcers that were only treated with greasy tulle due to her severe underlying condition. Considering her condition and her high age, surgery was ruled out. She was admitted to our clinic towards the end of March with an extensive pressure ulcer between the shoulder blades and in the occipital and parietal area on the head, with skin and subcutaneous tissue missing up to the bone in the extent of 10 x 12 cm.
Status localis at the first visit-partial healing of the pressure ulcer between the shoulder blades, on the head the defect is stagnant, with thickened margins, blackish brown bone colour (Figures 1). Since the beginning of April 2014 the therapy included thin hydrocolloids and polyurethane foam (Figure 2) on the back, the defect healed completely at the end of July 2015. The defect on the head was first treated with hydrogel preparations; there was improved blood supply to the margins, epithelisation, and change in the colour of the bone (Figure 3). After considering several therapeutic possibilities we decided to commence stem cell therapy (Figure 4).
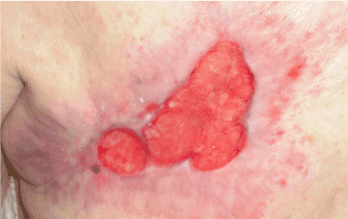
Figure 1. Pressure ulcer on the left shoulder blade in March 2014
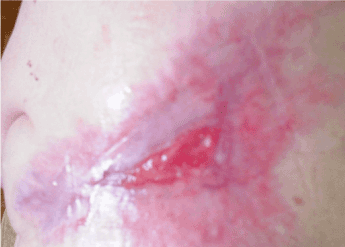
Figure 2. Pressure ulcer on the back after 2 months of wet therapy
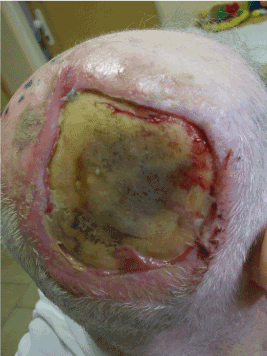
Figure 3. Hydrogel preparations used in therapy, improved blood supply to the margins, pithelisation from the margins, change in bone colour (April 2014)
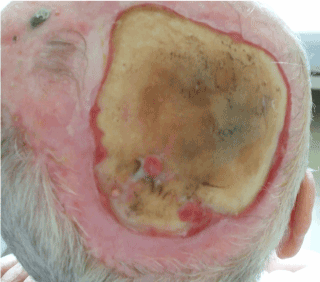
Figure 4. Local finding before the application of stem cells – fibroblasts
We harvested skin material from the right armpit (punch 1 mm), and sent it to the laboratory in a transport culture medium (Ringer solution + Gentamycin) where it was processed within 2 hours.
Skin biopsy taken from the axila is placed in transport solution (Ringer´s solution with Gentamycin 50 ug/ml). Transport of the biopsy to the tissue bank is realized under controlled conditions at the temperature 4-8° C.
Skin tissue is processed in laminar flow cabinet (class II B) situated in a clean room. The skin tissue is cleaned and cut into small pieces (size 1-2 mm). The fragments of the tissue are treated with collagenase II (concentration 0.1-0.2%) at the temperature 37°C.
The fibroblasts released after digestion of matrix are isolated and suspended in culture medium DMEM supplemented with fetal bovine serum (10%) and Gentamycin (50 ug/ml). The fibroblasts are inoculated in the plastic flasks and cultured at the temperature 37°C in CO2 atmosphere (5%). The culture medium is changed every 2 days.
During successful cultivation a cell mono-layer is formed. The number of cells required by physician is obtained via subcultivation of the primoculture. Proliferation of the fibroblasts is monitored using phase contrast inverted microscopy. Quality control of the process is done periodically and includes control of fibroblasts morphology and viability and microbiological and biochemical controls of the culture medium. The time needed for cultivation of fibroblasts is 3-4 weeks on the average.
In the final product the cultivated autologous fibroblasts (cca 107cells/ml) are suspended in Ringer’s solution and transported to the health care facility under controlled conditions at the temperature 25°C
After four weeks (first week of May 2014) the solution with fibroblasts was ready to be applied to the pressure ulcer on the head.
The stem cells culture medium was Hcel®NaT, (wound dressing from modified cellulose) that stimulates a physiological condition. Hcel®NaT absorbs the exudate and turns it into a gel that keeps the wound wet. The dressing adheres to the wound perfectly and is easily removable [11].
The defect is washed with F1/1. Hcel®NaT is moistened with stem cell solution and applied onto the defect (Figure 5). The dressing was at first changed every other day, after a month, it was changed every third or every fourth day. Within 5 weeks healing was observable, with slow gradual epithelisation starting from the margins. There was also epithelisation observable on the bone, and the defect was getting smaller. (Figures 6 and 7)
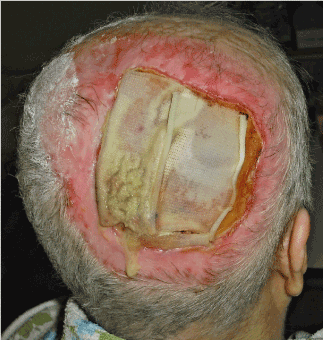
Figure 5. Hcel®NaT dressing moistened with stem cell solution
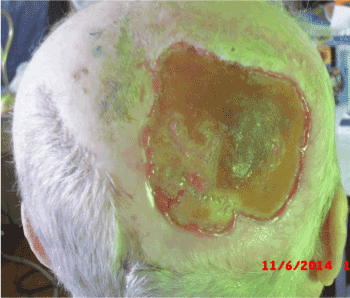
Figure 6. November 2014 – epithelisation from the margins and the centre, the defect decreased in size
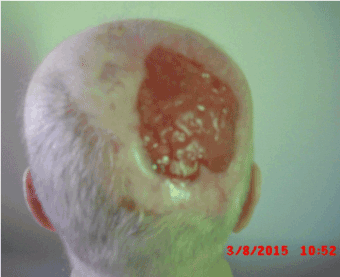
Figure 7. . March 2015 – the bone is completely covered with granulations, and there is epithelisation from the margins
The treatment continued until 2015 (Figure 8). At that time the defect was covered with granulations and the size of the defect was reduced by more than 60%. In July 2015 we started moistening the dressing material Hcel®NaT with the culture medium-Nutrient Mixture F-12 Ham Formulation (Annex 1). Topical therapy continued and the dressing was changed once in four days.
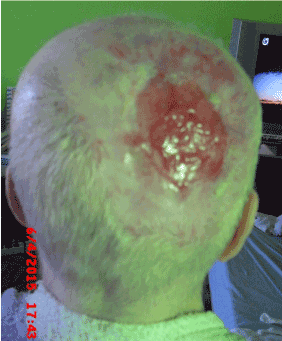
Figure 8. June 2015 – Hcel®NaT is moistened only with the culture medium Nutrient Mixture F-12 Ham Formulation
Despite the fact that fibroblasts were no longer applied, the healing continued at a satisfactory pace and according to documentation from January 2016 there were only small residual areas undergoing the process of epithelisation (Figure 9).
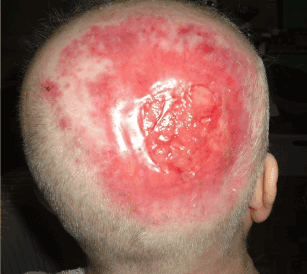
Figure 9. Local finding in January 2016 – the defect on the head is almost healed
The application of stem cells-fibroblasts processed using bioengineering technologies represent one of the most progressive types of cell therapy without any undesired effects. The final effect of application includes the formation of new skin cells, better skin appearance and elasticity due to the synthesis of collagen, elastin, and other ECM (extracellular matrix-protein and saccharide) components. This method is money and time consuming and requires perfect cooperation and coordination between the physician, the laboratory, and the patient, however, it brings excellent final effects. It is very comfortable for the patient and not demanding for the staff.
The presented case very well documents the good therapeutic effect of fibroblasts applied on a pressure ulcer on the head that was considered unsuitable to be covered with a transplant or treated with VAC therapy by the surgeons (due to age and underlying diagnosis of the patient). Healing with stem cells may be slow, but it has improved the quality of life and the overall condition of the patient (Figures 10 and 11)
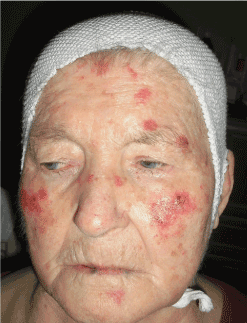
Figure 10. The patient in April 2013

Figure 11. The patient in January 2016
What is also very interesting is the fact that once the processes of epithelisation and granulation started in the defect (due to the application of fibroblasts), the patient continued applying the Hcel®NaT wound dressing moistened only with the culture medium Nutrient Mixture F-12 Ham Formulation, but the haling was not decelerated.
It is therefore questionable what is responsible for the final effect:
- the dressing material,
- the combination of the dressing material and the culture medium
- or both factors plus the renewed regenerative properties of the skin
The future will show w2021 Copyright OAT. All rights reserv(pressure ulcers, lower leg ulcers of varying aetiology) will take advantage of stem cells also in cases where manifestations are considered unsuitable to be treated by transplantation or VAC therapy (due to age and underlying diagnosis of the patient). The healing may seem slow, and require patience on the part of the patient and medical staff as well, but it will without any doubt improve the overall condition and the quality of life of the patient affected. What should also be mentioned is the fact that cellulose materials and their derivates show numerous excellent properties suitable in wound healing, as demonstrated in the case report. Carboxymethyl cellulose is used in moist wound healing, oxidised cellulose is used as a resorbable surgical haemostatic material. Hcel®NaT (sodium carboxymethyl cellulose) is a new cellulose dressing material that differs from other materials, as it is made of non-woven (fibrous) textiles by (spun-laced technology) [11-13].
View supplementary data
- Thangapazham RL, Darling TN, Meyerle J (2014) Alteration of Skin Properties with Autologous Dermal Fibroblasts. Int J Mol Sci 15: 8407-8427. [Crossref]
- Munavalli GS (2011) Autologous Living Cell Therapy for Facial Rejuvenation. Practical Dermatology 45-48.
- Watson D, Keller GS, Lacombe V (1999) Autologous Fibroblasts for Treatment of Facial Rhytids and Dermal Deppressions. Arch Facial Plast Surg 1: 165-170. [Crossref]
- Smith S, Munavalli GS, Weiss R (2012) Multicenter, Double-blind, Placebo-controlled Trial of Autologous Fibroblasts Therapy for the Treatment of Nasolabial Fold Wrinkles. Dermatol Surg 38: 1234-1244. [Crossref]
- European Pressure Ulcer Advisory Panel-Independent Expert Panel; National Pressure Ulcer Advisory Panel-Independent Expert Panel; Pan Pacific Pressure Injury Alliance-Professional Association. Interventions for prevention and treatment of pressure ulcers. In: Prevention and treatment of pressure ulcers: clinical practice guideline. 2009 (revised 2014). NGC: 010604
- European Pressure Ulcer Advisory Panel-Independent Expert Panel; National Pressure Ulcer Advisory Panel-Independent Expert Panel; Pan Pacific Pressure Injury Alliance-Professional Association: Prevention of pressure ulcers. In: Prevention and treatment of pressure ulcers: clinical practice guideline. 2009 (revised 2014). NGC:010603
- Breslow RA, Hallfrisch J, Guy DG, Crawley B, Goldberg AP (1993) The importance of dietary protein in healing pressure ulcers. J Am Geriatr Soc 41: 357–362. [Crossref]
- Langer G, Schloemer G, Knerr A, Kuss O, Behrens J (2003) Nutritional interventions for preventing and treating pressure ulcers (Cochrane Review). Cochrane Database Syst Rev CD003216. [Crossref]
- Riebelová V, Válka J, Francú M (2000) Trendy soudobé chirurgie 3-Dekubity, Prevence, konzervativní a chirurgická terapie. Vydavateľstvo: Galén.
- Stryja J (2008) Repetitorium hojení ran. Geum.
- Sopuch T, Drahovzalov R, Rýdl J, Bureš I, Milichovský M, et al. (2013) Celulózové materiály v ošetřování ran. HOJENÍ RAN 7: 14-20.
- Queen D (2009) Technology update: Understanding hydrocolloids. Wounds international 1: 2-7.
- Queen D (2010) Technology update: Understanding Hydrofiber® Technology. Wounds international 1: 29–32
- Czech Pharmacopoeia.
- Uzun M, Anand SC, Shah T (2013) In Vitro Characterisation and Evaluation of Different Types of Wound Dressing Materials. Journal of Biomedical Engineering and Technology 1: 1-7.
- BS EN 13726-1:2002, Test methods for primary wound dressing, Aspects of Absorbency, BSI, ISBN 0 580 39510 3, British Standard Institute 2002.











