Abstract
Introduction: Bangladesh’s growing population negatively affects its economic growth. As such, reproductive health programs are critical. Fieldworkers play a critical role in providing family planning services in Bangladesh, and require up-to-date knowledge to counsel their clients to improve family planning outcomes. This study examines the effects of a fieldworker digital health training package on family planning client knowledge and behaviors in Bangladesh through a two-step diffusion model.
Methods: This study was part of a knowledge management intervention that sought to improve fieldworkers’ access, comprehension, and application of health resources. Mothers with a child under the age of two (n= 651) reported receiving a home visit from a fieldworker who had a netbook with the package (low exposure); reported receiving a home visit from a fieldworker who had a netbook with the package and were shown a digital resource (high exposure); or reported no home visit from a fieldworker who had a netbook (no exposure).
Results: Both levels of exposure were associated with higher odds of mothers reporting that the fieldworker discussed contraceptive choice, contraceptive side effects, and contraceptive side effects management compared to unexposed mothers. Mothers in the high exposure group had higher odds of contraceptive use compared to unexposed mothers (aOR: 1.85).
Discussion: The knowledge a fieldworker gains through a digital health training package can be diffused to clients, positively affecting client knowledge and behaviors. Such interventions can empower fieldworkers by providing them relevant information at the point of care, which can enhance their credibility among the communities they serve.
Key words
Bangladesh, contraceptive use, counseling, fieldworker
Introduction
Bangladesh has made remarkable progress in many of its health and development indicators, placing it among one of the few lower-income countries that potentially could reach its Millennium Development Goals (MDGs) targets related to health [1]. However, the population of Bangladesh is on the rise, and predictions suggest that the population will grow another 100 million before stabilizing unless fertility drops below replacement level [2]. As Bangladesh faces numerous issues related to its rapid population growth, including food and housing shortages, for example, reproductive health programming, including family planning, is crucial in managing unchecked population growth and its various deleterious effects.
After independence in 1971 until the mid-1990s, the government of Bangladesh invested primarily in vertical family planning services, including recruiting family planning caregivers at the community level to deliver contraceptives to women in their homes, as well as providing family planning services in primary health centers [3]. During this period, the contraceptive prevalence rate (CPR) increased from 8% to 45%, and the total fertility rate (TFR) declined from 6.3 to 3.3 [4,5]. As a result, Bangladesh has widely been lauded for its success in reducing unmet need for contraception (currently 11%) [6]. Yet, the use of skilled birth attendants is still low (31.7%), progress on anemia and under-nutrition is stagnant, and adolescent marriage and pregnancy remain high [6]. Additionally, the TFR has remained relatively constant, ranging from 3.0-3.4 across four Demographic Health Surveys and then ranging between 2.3-2.7 from 2007-2011 [4-8]. Preliminary results from the 2014 survey indicate that the TFR is 2.3 [9].
There are two cadres of fieldworkers that could have impacted outcomes related to family planning in Bangladesh. Family Welfare Assistants (FWAs) are primarily responsible for delivering family planning information and some commodities at the household and community level. Health Assistants (HAs) may also provide some services related to reproductive health. The influence of FWAs is quite relevant to contraceptive use in Bangladesh, as Andaleeb et al. [10] found that women were more likely to use contraception in areas where there was a low population-to-FWA ratio, and when they received more visits from the FWA. Lack of supervision and training for FWAs were also hypothesized to contribute to low contraceptive uptake.
Community-based fieldworkers such as FWAs and HAs are particularly important within the context of Bangladesh, as one study has indicated that few children attending government health facilities were fully examined or correctly diagnosed, and few providers were given advice on how to continue care at home, while health caregivers that work at the community level did better than health facility workers in providing care [11]. A large evidence base suggests that health caregivers at the community level have the potential to play a key role in increasing coverage of essential interventions related to child survival [12].
As fieldworkers, such as FWAs and HAs provide vital services to communities that tend to have irregular access to health services, human resources for health is a challenge [13]. The global health care worker shortage, coupled with a lack of access to continuing professional development (CPD) opportunities [14], results in a health care workforce ill-equipped to prevent, treat, and manage disease.
Many resource-poor settings are starting to explore the use of digital health tools for data collection, supply chain management, and surveillance, as well as utilization for health professional training [13]. Defined in numerous ways, digital health broadly encompasses the communication of health information through computer technology and the Internet [15] and is increasingly becoming a critical tool in delivering effective global health programs specifically in low and middle-income countries, including capacity building assistance and training [13]. The potential to leverage digital health for economic growth has fueled access to information through various communication channels within the developing country context [16]. The need for rapid access to information to support critical decisions in public health is paramount [17], and universal access to information for health professionals is critical to ensure the highest delivery of health care, and subsequent health outcomes [18].
Digital health is particularly relevant within a training context. In fact, conventional training programs often do not focus on skills building within the context of health systems strengthening, nor do they focus on the practical aspects of health care delivery [19]. Health caregivers who work at the community level are typically brought to centralized locations for training, which, in turn, can cause serious disruptions in service delivery [20]. As a result, programmers are exploring other ways to ensure that health caregivers at the community level are being provided with the right training to deliver effective health care, including digital health through the use of knowledge management approaches such as eLearning and eToolkits. eLearning can broadly be defined as the use of network technology to deliver training [21], and eToolkits are digital libraries that compile relevant information into an easy-to-use interface [22]. These approaches to managing knowledge, including exploring what it is and how to create, transfer, and use it more effectively, are the essence of knowledge management [23], and these specific knowledge management approaches, digital libraries with synthesized content and e-learning systems, are both considered important enabling technologies for the knowledge supply chain [24]. Finally, within a training context, digital health training methods such as digital libraries and e-learning systems provide a flexible and sustainable way to provide continuous learning yielding improvements in in health worker knowledge and skills [25].
Digital health can enhance the health knowledge and skills of caregivers [26,27]. For example, digital health can play a powerful role at the point of care when a health caregiver is with a client and needs to provide accurate and relevant information on a range of health issues, including family planning and reproductive health. Digital health solutions provide ready access to needed information empowering the health worker and in turn satisfying the needs of the client [27,28]. Health knowledge is a critical factor that enables women to be aware of their rights and health status in order to seek appropriate health services. As Family Planning 2020 seeks to support the rights of women and girls to decide freely whether, when, and how many children they wish to have [29], there is a need to ensure that women have access to the right information to make choices regarding their reproductive health. FWAs and HAs play an important role in helping FP2020 reach its ultimate goal of enabling 120 million more women and girls to use contraceptives by 2020. Particularly in a country such as a Bangladesh, where 67% of the population lives in a rural setting [30], FWAs and HAs play a crucial role in communicating information about and motivating women and girls to use modern contraceptive methods [31].
Behaviors related to family planning are complex. An individual’s family planning behavior is influenced by many factors, including social norms, attitudes, and motivational factors, to name a few, and exposure to family planning services is a critical influence [32]. From a theoretical perspective, the provision of family planning services affects reproductive health behavior by facilitating the diffusion of new ideas about reproduction [33]. In this view, fieldworkers such as FWAs and HAs are agents of change who introduce new ideas and capabilities related to reproductive health to rural communities. Outreach programs, through the use of health caregivers at the community level, have fostered ideational change and increased demand for contraceptives [33].
Diffusion of innovations theory suggests that although external influences are generally responsible for making individuals aware of an innovation such as a practice or idea, interpersonal influence - or the interaction with friends and neighbors - is what leads to adoption [34,35]. This idea - that individuals may receive information about a practice or idea through a two-step diffusion process, with opinion leaders obtaining information from a wide-reaching channel such as the media, and then passing on the information to others - is called the two-step hypothesis. Articulated by Katz [36], this hypothesis was thus created to explain how diffusion of an idea or practice flowed from media to opinion leaders, to better understand how information flows. Within the context of Bangladesh, we suggest that this hypothesis can be applied to understanding how the knowledge an FWA or HA gains through digital training methods can be diffused to the client with regard to family planning ideational behaviors, including knowledge about issues related to family planning as well as family planning behaviors themselves. For the purposes of this study, we suggest that the FWAs and HAs obtain knowledge through a digital training package - that consists of eLearning courses as well as an eToolkit - and then pass on the information to their clients. In this study, we sought to test this two-step diffusion process by examining how a digital health training package geared toward improving knowledge related to reproductive health among FWAs and HAs affected client knowledge and behaviors related to reproductive health. Clients included mothers with a child less than two years old in two low-performing districts, Sylhet and Chittagong, which have been identified as priority areas for promoting modern contraception by the government of Bangladesh [9].
Methodology
This cross-sectional study was part of a larger knowledge management intervention conducted by the Bangladesh Knowledge Management Initiative project, called the eHealth pilot. One of the project’s objectives was to improve FWAs and HAs’ access and comprehension, as well as application, of integrated, coordinated and harmonized behavior change communication knowledge and resources for health, population and nutrition.
An objective related to this study focused on an eHealth pilot, which sought to use innovative technology to improve the knowledge and counseling skills of FWAs and HAs, with the intent of improving client knowledge and behaviors. Netbook computers were given to 153 FWAs and 151 HAs. District-level government officials purposively chose these fieldworkers. Prior to the pilot’s implementation, fieldworkers received a two-day hands-on training on how to use the netbook, and an orientation to the digital resources contained in the netbook. For the purpose of simplification, FWAs and HAs will be referred to broadly as fieldworkers for this study.
Netbooks contained two distinct offline digital health training resources:
- Eight video-based eLearning courses on topics related to maternal health, family planning, nutrition, interpersonal communication and integrated messaging.
- An eToolkit containing more than 100 printed and audio-visual materials for fieldworkers to use as counseling tools on health, family planning and nutrition topics during their regular counseling activities. The eToolkit was also designed to supplement and refresh fieldworker knowledge.
While the intervention focused on integration of health, nutrition, and family planning, this study examined family planning-related outcomes only. The intervention lasted for four months (May to August 2013). As this study was interested in understanding client behaviors in relation to fieldworker use (or non-use) of a package of digital resources, we were interested in comparing varying exposure of mothers who had a child under the age of two:
- Mothers who reported that they did not receive a home visit from a fieldworker who had a netbook (no exposure);
- Mothers who reported receiving a home visit from a fieldworker who had a netbook with the digital health training package (low exposure); and
- Mothers who reporting receiving a home visit from a fieldworker who had a netbook with the digital health training package and were shown a digital family planning resource on the netbook (high exposure).
The study was conducted in two low-performing districts in the context of uptake of family planning services: Sylhet and Chittagong. Multistage sampling was used to select study participants. Six upazilas (sub-districts) were randomly selected from each of two districts. Two unions (villages) were randomly selected from each sub-district, yielding a total of twelve unions per district. A household mapping exercise was undertaken in twelve unions in each district to prepare a sampling frame of mothers with children under two years. A random start was used in each union to begin the systematic random sampling process. Ethical approval was obtained by the Bangladesh Medical Research Council in Bangladesh and the Johns Hopkins Bloomberg School of Public Health Institutional Review Board in the United States.
Outcome variables
We were interested in a total of four outcomes. The primary outcome of interest was mothers’ current contraceptive use. Secondary outcomes included three fieldworker behaviors through the mothers perceptions of information provided or discussed with the fieldworker, including (1) whether or not the fieldworker provided information about possible side effects due to method choice, (2) whether or not the fieldworker provided information about actions to take in case side effects were experienced, and (3) whether or not the fieldworker provided information about the various methods of family planning options available.
Our primary outcome variable was current contraceptive use. All mothers were questioned about whether or not they were currently using any contraceptive method (both modern and traditional). They were asked: “Are you currently doing something or using any method to delay or avoid getting pregnant?” This outcome indicator is a dichotomous variable (yes or no).
All mothers were questioned about whether or not a fieldworker provided information regarding side effects or problems with their contraceptive method. They were asked: “In the past 3 months, were you ever told by a health and/or family planning worker about side effects or problems you might have with the method?” This outcome indicator is a dichotomous variable (yes or no).
In addition to asking mothers if a fieldworker provided information regarding side effects related to contraceptive method, they were questioned about whether or not a fieldworker provided information about the actions to take if side effects were experienced. They were asked: “Were you ever told by a health and/or family planning worker what to do if you experienced side effects with the method?” This outcome indicator was also a dichotomous variable (yes or no).
These three questions related to fieldworker behavior were asked to ascertain whether the information provided by a fieldworker was actionable, implying the usability and relevance of the information for the client [37]. Previous research indicates that actionable knowledge related to family planning method side effects is one of the most critical factors in decreasing morbidity related to family planning method use [38].
All mothers were questioned about whether or not a fieldworker provided information about the various contraceptive methods available. They were asked: “Were you ever told by a health and/or family planning worker about other methods of family planning that you could use?” This outcome indicator was a dichotomous variable (yes or no).
Independent variables
The exposure variable consisted of three categories. The first category was mothers who reported that they did not receive a home visit from a fieldworker who had a netbook (no exposure) during the pilot intervention (from May to August 2013). The second category was mothers who reported receiving a home visit from a fieldworker who had a netbook with the digital health training package (low exposure). The third category was mothers who reported receiving a visit from a fieldworker who had a netbook with the digital health training package and who were shown a digital family planning resource on the netbook (high exposure).
Our analysis controlled for a number of factors, including age, education and household assets. Age is a dichotomous variable with younger women in the 15 to 29 years category and older women being 30-43 years. Three education categories include non-literate (unable to read or write), primary (grades 1-4) and some secondary education or more (grades 5-8 or more). A household asset index consisting of electricity, radio, TV, mobile or landline phone, and refrigerator, was created with mothers, with four or more assets being categorized as “high” and mothers with three or less assets as “low”.
Results
Socio-demographic characteristics from the sample of mothers by digital health pilot intervention exposure are listed in Table 1. There was no statistically significant difference in each of the socio-demographic variables (age, education level, and household assets index) between the three groups. Approximately three-fourths of all mothers reported less than three household assets and were 15-29 years old. Regarding education level, half of the mothers reported that they had at least completed some secondary schooling or more.
Table 1. Background characteristics of mothers' (child<2 years) by digital health pilot intervention exposure.
|
No exposure
(N = 248) |
Low exposure
(N=145)
|
High exposure
(N=258)
|
Total
(N=651)
|
Chi-square |
Age (years) |
N (Percent) |
N (Percent) |
N (Percent) |
N (Percent) |
5.48
p=0.06 |
15-29 |
203 (81.9) |
104 (71.7) |
200 (77.5) |
507 (77.8) |
|
30-43 |
45 (18.2) |
41 (28.3) |
58 (22.5) |
144 (22.2) |
|
Education Level |
N (Percent) |
N (Percent) |
N (Percent) |
N (Percent) |
4.93
p=0.29 |
Non-Literate |
38 (15.3) |
16 (11.0) |
24 (9.3) |
78 (12.0) |
|
Primary |
95 (38.3) |
55 (37.9) |
99 (38.3) |
249 (38.2) |
|
Some secondary or more |
115 (46.3) |
74 (51.1) |
135 (52.3) |
324(49.7) |
|
Household Assets+ |
N (Percent) |
N (Percent) |
N (Percent) |
N (Percent) |
1.14
p=0.56
|
Low (<=3 assets) |
196 (79.0) |
117 (80.7) |
197 (76.3) |
510 (78.3) |
|
High (>=4 assets) |
52 (21.0) |
28 (19.3) |
61 (23.6) |
141 (21.7) |
|
+ Household assets =Electricity, radio, TV, mobile, telephone, refrigerator
Figure 1 displays the percentage of mothers who were exposed to the digital pilot intervention. Of the 651 respondents, data indicate digital pilot intervention exposure of 62 percent with 22 percent of the mothers receiving a home visit from a fieldworker who had a netbook with the digital health training package, and another 40 percent of the mothers receiving a visit from a fieldworker who had a netbook with the digital health training package and who were shown a digital family planning resource on the netbook. Approximately 38 percent of mothers did not receive a home visit from a fieldworker who had a netbook during the pilot intervention period.
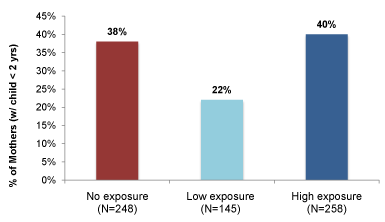
Figure 1. Exposure to digital health pilot intervention (n=651).
Figure 2 displays the various contraceptive methods of the sample. The current use of family planning methods in the sample was 69.3 percent. Of those users that currently used family planning methods (n=451), 31.1 percent reported using oral pills and another 17.5 percent reported using injectables. Condom use was reported by 10 percent and the rhythm method was practiced by 3.3 percent of users. Use of terminal methods like female sterilization (3 percent) and male sterilization (0.1 percent) was low as was the use of lactational amenorrhea.
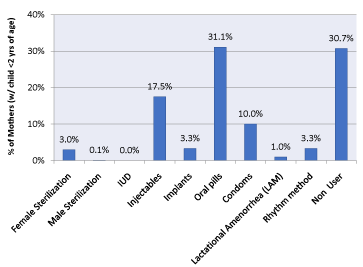
Figure 2. Family Planning Method Mix Among Mothers (N= 651).
Actionable knowledge related to family planning has been identified as information that can enable couples to make decisions and take action related to those decisions [37]. In this pilot intervention, resources included in the digital health training package included ways in which fieldworkers could provide actionable information related to family planning. Table 2 examines fieldworker behavior regarding three variables focused on actionable information: whether or not the mother reported that the fieldworker offered a choice of contraceptives during the home visit, whether or not the mother reported that the fieldworker discussed side effects associated with contraceptive methods, and whether or not the mother reported that the fieldworker discussed what to do if side effects related to contraceptive use were experienced.
Table 2. Odds ratios from logistic regression analysis measuring effects of mothers’ (child<2 years) exposure to a digital health pilot intervention on fieldworkers’ behavior (n=651).
|
Fieldworker offered a choice of contraceptives during home visit
|
Fieldworker discussed side effects of contraceptives during home visit
|
Fieldworker discussed what to for side effects during home visit |
Independent
Variables |
Adjusted
Odds Ratio [CI] |
Adjusted
Odds Ratio [CI] |
Adjusted
Odds Ratio [CI] |
Digital health pilot intervention exposure
No exposure (r)
Low exposure
High exposure |
1.00
3.18*** [2.06-4.91]
2.73***[1.90-3.93] |
1.00
3.22*** [2.09-4.96]
3.29*** [2.27-4.75] |
1.00
3.21*** [2.09-4.95]
3.23***[2.23-4.66] |
Age
< 30 years
30-43 years |
1.00
1.12 [0.75-1.66] |
1.00
1.08 [0.72-1.60] |
1.00
1.09 [0.73-1.62] |
Education
Non-literate
Primary (1-4 grade)
Some secondary or more |
1.00
1.57 [0.92-2.68]
1.49 [0.87-2.57] |
1.00
1.46 [0.85-2.50]
1.57 [0.91-2.72] |
1.00
1.52 [0.87-2.62]
1.61 [0.93-2.79] |
Household assets+
Low (0-3)
High (4-6) |
1.00
0.91 [0.60-1.37] |
1.00
1.01 [0.68-1.53] |
1.00
0.98 [0.65-1.48] |
District
Sylhet
Chittagong |
1.00
1.56** [1.12-2.16] |
1.00
1.46* [1.05-2.03] |
1.00
1.37 [0.99-1.91] |
* Significant at p <= 0.05; ** p<=0.01; *** p<=0.001
+ Household assets: electricity, radio, television, mobile phone, landline phone, refrigerator
Using logistic regression modeling and adjusting for age, education, household assets and district, results indicate that both low and high levels of exposure to the pilot were associated with higher odds of mothers reporting that the fieldworker discussed all three items related to actionable knowledge. Mothers who received a home visit from a fieldworker who was given a netbook with the digital health training package were 3.18, 3.22 and 3.21 times more likely to report that the fieldworker discussed contraceptive choice, discussed side effects, and provided information regarding action the mother could take if she experienced side effects related to contraceptive use, respectively, compared to mothers who received no home visit from a fieldworker who had a netbook. Similarly, odds of mothers reporting that the fieldworker discussed/provided information on all three topics in the group that received a home visit from a fieldworker who was given a netbook with the digital health training package and were shown a digital family planning resource on the netbook were 2.73, 3.29, and 3.23, respectively, compared to mothers who received no home visit from a fieldworker who had a netbook.
Table 3 presents results from logistic regression analysis to assess if exposure to the digital pilot intervention was associated with current contraceptive use among mothers. The model indicates that mothers who received a home visit from a fieldworker who was given a netbook with the digital health training package and were shown a digital family planning resource on the netbook were 1.85 times more likely to currently use contraceptives compared to mothers who received no home visit from a fieldworker who had a netbook, after adjusting for age, education, household assets and district. However, mothers who received a home visit from a fieldworker who was given a netbook with the digital health training package did not have higher odds of current contraceptive use compared to mothers who received no home visit from a fieldworker who had a netbook. This finding indicates that current contraceptive use behavior is more heavily influenced by home visits by a fieldworker that not only had a netbook with the digital resources, but also used the netbook as a teaching tool with the mother.
Table 3. Odds ratios from logistic regression analysis measuring effects of mothers’ (child < 2 years) exposure to a digital health pilot intervention on current contraceptive use (n=651).
Independent Variables |
Current Contraceptive Use
Adjusted Odds Ratio [CI] |
Digital health pilot intervention exposure
No exposure (r)
Low exposure
High exposure |
1.00
1.30 [0.83-2.03]
1.85* [1.25-2.74] |
Age
< 30 years
30-43 years
|
1.00
0.97 [0.64-1.48] |
Education
Non-literate
Primary (1-4 grade)
Some secondary or more |
1.00
1.73 [1.00-3.01]
1.52 [0.87-2.64] |
Household assets+
Low (0-3)
High (4-6) |
1.00
0.44*** [0.29-0.67] |
District
Sylhet
Chittagong
|
1.00
0.83 [0.59-1.17]
|
* Significant at p <= 0.05; ** p<=0.01; ***p<=0.001
+ Household assets: electricity, radio, television, mobile phone, landline phone, refrigerator
Exploring current contraceptive use further, Figure 3 indicates a dose response relationship between exposure to the digital health pilot intervention and current contraceptive use (p<0.01). Of mothers who had no exposure, 62.5 percent reported current contraceptive use. Of mothers who received a home visit from a fieldworker who was given a netbook with the digital health training package, 69.0 percent reported current contraceptive use. Of mothers who received a home visit from a fieldworker who was given a netbook with the digital health training package and were shown a digital family planning resource on the netbook, 75.2 percent reported current contraceptive use.
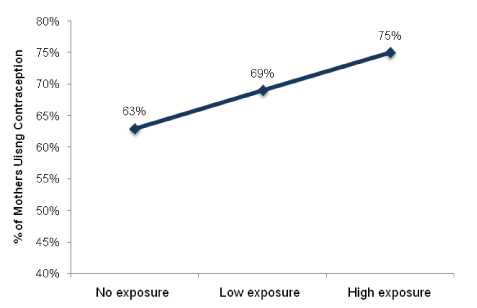
Figure 3. Percent current contraceptive use by digital health pilot intervention exposure (N=651; p<0.01).
Discussion
The past decade has ushered in two important changes in the delivery of family planning and other health services. One change is the acceptance and promotion of community-level fieldworkers as important players within the delivery of health services; another is the rapid expansion and use of digital health solutions to improve delivery of health services. In Bangladesh, a country with a large rural community and stagnating fertility rates, fieldworkers such as family welfare assistants and health assistants play a vital role in providing health information on a range of topics to their clients. However, fieldworkers must have up-to-date information in order to deliver the best service. Knowledge management methods such as eLearning courses and Toolkits provide curated and synthesized collections of selected health information that fieldworkers can easily access and apply in their daily work, and then diffuse this knowledge and learning to their clients. This study indicates that fieldworker use of these knowledge management methods proved to be a crucial factor that strengthened their actionable knowledge and skills to the extent that they were not only able to transfer the knowledge to their clients, they were also able to persuade clients who expressed a need for family planning to initiate contraceptive use.
This study provides evidence for the differential effects of a digital intervention. Although even low exposure to the intervention was associated with fieldworkers more likely to offer a choice of contraceptives, discuss side effects, and discuss the possible actions to take experiencing side effects, contraceptive use was associated only with mothers who reported receiving a home visit from a fieldworker who had a netbook with the digital health training package and were shown a digital family planning resource on the netbook (high exposure). This indicates that behavior change requires interpersonal persuasion, and that while digital resources are an effective, appropriate tool to facilitate counseling, technology alone may fall short with regard to client behavior change.
We speculate that using the netbook with the client lead to more questions and discussions between the fieldworker and the client, and perhaps this may explain why those mothers that were shown a resource on the netbook during a home visit were more likely to report using contraceptives. Previously, mothers would have no option but to trust the fieldworker, but with the addition of the netbook with vetted resources, mothers may have felt more confident in the information that was provided to them. Additionally, prior to using the netbooks, fieldworkers indicated that they had few visual aids to use during home visits, and the use of technology during the home visit may have aided in mothers seeing the fieldworker as a more credible family planning resource, as anecdotally, fieldworkers also indicated that they felt more confident about the information they provided because they could refer to the netbook. In this way, fieldworkers’ confidence and self-efficacy to provide accurate family planning information may have indirectly impacted mothers’ perceptions of their credibility, and in turn, their knowledge and behavior.
In addition to providing gains in skills and knowledge, digital health interventions can empower field workers as these interventions provide them with the knowledge they need at the point of care thus improving their self-efficacy and credibility in the communities in which they work [28]. These benefits of empowerment, self-efficacy, and credibility add value beyond what one might find in a traditional capacity strengthening and training methods, which may increase knowledge and skills but not have an impact on fieldworkers’ sense of agency. Others studies conducted among community health workers who have received a digital health intervention have found that digital health interventions impact fieldworker empowerment and motivation [39-41]. In addition, possessing and harnessing the knowledge housed on digital technologies translates into greater field worker authority and increased trust [27] and greater respect from the community [42]. Finally, digital health interventions may be more cost effective because they are able to reach more fieldworkers more quickly, result in fewer service disruptions, are more timely than traditional trainings, and reduce travel costs [43].
Finally, the role of fieldworkers in diffusing knowledge related to reproductive health should not be overlooked. A recent study indicated that within Bangladesh, rural women had less knowledge on family planning than urban women [44]. As fieldworkers provide essential health services to primarily rural populations in Bangladesh, they serve an important function in synthesizing knowledge and subsequent behaviors related to family planning [45]. Additionally, a key component to minimizing the knowledge gap is the use of knowledge generation to improve, develop, and evaluate training models to improve tacit skills and improve capacity across all levels of the health system [46]. Results from this study indicate that fieldworkers were able to glean knowledge related to reproductive health from the digital health training package, and were then able to transfer this knowledge onto their clients, supporting our two-step diffusion hypothesis.
This study has several2021 Copyright OAT. All rights reservs is likely, as this study relied on self-reporting. However, because this study asked mothers to report on fieldworker behavior instead of asking the fieldworkers about their own behaviors, our results may be more valid compared to a typical self-report. Recall bias is also likely, as mothers may not have remembered if a fieldworker had a netbook or used the netbook with them during the home visit. We were also unable to control for other potentially confounding factors, such as exposure to other health interventions related to family planning. Additionally, because this is a cross-sectional study, it is not possible to establish a temporal relationship between exposure and outcomes. Finally, it is likely that the fieldworkers that were given the netbooks were more enthusiastic and motivated than those that were not. We were also unable to take into account fieldworkers’ abilities to counsel clients on issues related to family planning prior to being trained on the netbook.
Despite these limitations, this study makes several unique contributions to the field. First, this is one of the only community-based studies that provide evidence regarding the effect of a knowledge management digital health intervention on clients. Other community-based studies have stopped short of measuring variables at the client-level, instead focusing on changes at the provider level and the implications of those changes on health system improvement (for example, see [27]. In addition, this study contributes to the body of literature that supports the use of digital training methods as a viable (and possibly preferable) means to improve fieldworker knowledge and skill. Digital health training addresses the drawbacks of other training methods, as fieldworkers can remain at their sites to continue providing services, are able to take courses and access materials at critical decision-making time points, and are cost-effective as there is no need for travel or to hire trainers. Finally, we introduce the idea of and test a two-step diffusion process whereby fieldworkers obtain new knowledge and skill from a digital health training package and in turn diffuse that new knowledge to their clients. Results imply that this two-step diffusion process occurred—as study participants had improved knowledge that translated in increased client knowledge and contraceptive uptake.
Building on the success of the pilot, the Bangladesh Knowledge Management Initiative project is currently in the process of scaling up the digital health training package for fieldworkers in Bangladesh. The eToolkit is being updated annually, with new content being added and outdated or redundant items being removed and an application of the digital health training package is under development. Nearly 24,000 Health Assistants have received Android-based tablets from the Directorate General of Health Services of the Ministry of Health and Family Welfare, and the project is advocating that the Directorate General of Family Planning also purchase tablets for its nearly 24,000 Family Welfare Assistants. As considerable resources are being utilized to scale up this digital health training package, an important next step is rigorous research to be able to best assess the impact of this scale-up on fieldworkers, clients, and health outcomes.
Funding information
This article was supported by the Knowledge for Health-II Project, funded by the Office of Population and Reproductive Health, Bureau for Global Health, US Agency for International Development, Cooperative Agreement No. AID-OAA-A-13-00068. The views expressed in this document do not necessarily reflect those of the US Agency for International Development or of the US government.
Competing interest
No author has any competing interests.
References:
- Zere E, Suehiro Y, Arifeen A, Moonesinghe L, Chanda SK, et al. (2013) Equity in reproductive and maternal health services in Bangladesh. Int J Equity Health 12: 90. [Crossref]
- Streatfield PK, Karar ZA (2008) Population challenges for Bangladesh in the coming decades. J Health Popul Nutr 26: 261-272. [Crossref]
- Johnston HB, Oliveras E, Akhter S, Walker DG (2010) Health system costs of menstrual regulation and care for abortion complications in Bangladesh. Int Perspect Sex Reprod Health 36: 197-204. [Crossref]
- Training N.I. of P.R. and 1994. Bangladesh demographic and health survey, 1993–1994, Calverton.
- Training N.I. of P.R. and 1997. Bangladesh demographic and health survey 1996–1997, Dhaka & Calverton.
- Training N.I. of P.R. and 2013. Bangladesh demographic and health survey 2011, Dhaka & Calverton.
- Training N.I. of P.R. and Associates M. and & Macro O, 2005. Bangladesh Demographic and Health Survey 2004. Available at: http://www.measuredhs.com/pubs/pdf/FR165/FR-BD04[FR165].pdf.
- Training N.I. of P.R. and 2007. Bangladesh Demographic and Health Survey 2007.
- Training N.I. of P.R. and 2015. Bangladesh Demographic and Health Survey 2014, Dhaka & Rockville.
- Andaleeb S.S. and Ph D (2003) Family Planning Field Workers In Bangladesh as Influence Agents: Some Policy Implications Family Planning Field Workers In Bangladesh as Influence Agents: Some Policy Implications.
- Arifeen SE, Bryce J, Gouws E, Baqui AH, Black RE, et al. (2005) Quality of care for under-fives in first-level health facilities in one district of Bangladesh. Bull World Health Organ 83: 260-267. [Crossref]
- Haines A, Sanders D, Lehmann U, Rowe AK, Lawn JE, et al. (2007) Achieving child survival goals: potential contribution of community health workers. Lancet 369: 2121-2131. [Crossref]
- Aluttis C, Bishaw T, Frank MW (2014) The workforce for health in a globalized context - global shortages and international migration. Glob Health Action 7: 10. [Crossref]
- Nartker AJ, Stevens L, Shumays A, Kalowela M, Kisimbo D, et al. (2010) Increasing health worker capacity through distance learning: a comprehensive review of programmes in Tanzania. Hum Resour Health 8: 30. [Crossref]
- Brodie M, Flournoy RE, Altman DE, Blendon RJ, Benson JM, et al. (2000) Health information, the Internet, and the digital divide. Health Aff 19: 255-265. [Crossref]
- Lustria ML, Smith SA, Hinnant CC (2011) Exploring digital divides: An examination of eHealth technology use in health information seeking, communication and personal health information management in the USA. Health Informatics J 17: 224-243. [Crossref]
- Revere D, Turner AM, Madhavan A, Rambo N, Bugni PF, et al. (2007) Understanding the information needs of public health practitioners: A literature review to inform design of an interactive digital knowledge management system. J Biomed Inform 40: 410-421. [Crossref]
- Godlee F, Pakenham-Walsh N, Ncayiyana D, Cohen B, Packer A (2004) Can we achieve health information for all by 2015? Lancet 364: 295-300. [Crossref]
- Ajuwon GA, Rhine L (2008) The level of Internet access and ICT training for health information professionals in sub-Saharan Africa. Health Info Libr J 25: 175-185. [Crossref]
- Gaye PA, Nelson D (2009) Effective scale-up: avoiding the same old traps. Hum Resour Health 7: 2. [Crossref]
- Welsh ET, Wenberg CR, Brown KG, Simmering MJ (2003) E-learning: emerging uses, empirical results and future directions. Int J Train Dev7: 245-258.
- Hanson RF, Gros KS, Davidson TM, Barr S, Cohen J, et al. (2014) National trainers’ perspectives on challenges to implementation of an empirically-supported mental health treatment. Adm Policy Ment Health 41: 522-534. [Crossref]
- Davenport TH, De Long DW, Beers MC (1998) Successful Knowledge Management Projects. Sloan Manag Rev 39: 43-57.
- Fuchs M, Muscogiuri C, Niederée C, Hemmje M (2004) Digital libraries in knowledge management: an e-learning case study. Int J Digital Libr 4.
- George PP, Papachristou N, Belisario JM, Wang W, Wark PA, et al. (2014) Online eLearning for undergraduates in health professions: A systematic review of the impact on knowledge, skills, attitudes and satisfaction. J Glob Health 4: 010406. [Crossref]
- Wutoh R, Boren SA, Balas EA (2004) eLearning: a review of Internet-based continuing medical education. J Contin Educ Health Prof 24: 20-30. [Crossref]
- Campbell N, Schiffer E, Buxbaum A, McLean E, Perry C, et al. (2014) Taking knowledge for health the extra mile: participatory evaluation of a mobile phone intervention for community health workers in Malawi. Glob Health Sci Pract 2: 23-34. [Crossref]
- Sullivan TM, Limaye RJ, Mitchell V, D'Adamo M, Baquet Z (2015) Leveraging the Power of Knowledge Management to Transform Global Health and Development. Glob Health Sci Pract 3:150-162. [Crossref]
- Brown W, Druce N, Bunting J, Radloff S, Koroma D, et al. (2014) Developing the “120 by 20” goal for the global FP2020 initiative. Stud Fam Plann 45: 73-84. [Crossref]
- World Bank 2014. World Development Indicators 2014.
- Gayen K, Raeside R (2010) Social networks and contraception practice of women in rural Bangladesh. Soc Sci Med 71: 1584-1592. [Crossref]
- Joshi S, Schultz TP (2007) Family Planning as an Investment in Development: Evaluation of a Program’s Consequences in Matlab, Bangladesh.
- Murphy E (2004) Diffusion of innovations: family planning in developing countries. J Health Commun 9 Suppl 1 123-129. [Crossref]
- Rogers EM (1995) Diffusion of Innovations. In Elements of Diffusion. 1-20.
- Valente TW (1996) Social network thresholds in the diffusion of innovations. Social Networks 18: 69-89.
- Katz E, Katz E (1957) The Two-Step Flow of Communication: An Up-To-Date Report on an Hypothesis. Public Opinion Quarterly 21: 61.
- Kapadia-Kundu N, Sullivan TM, Safi B, Trivedi G, Velu S (2012) Understanding Health Information Needs and Gaps in the Health Care System in Uttar Pradesh, India. J Health Commun 17: 30-45. [Crossref]
- Bloom SS, Tsui AO, Plotkin M, Bassett S (2000) What husbands in northern India know about reproductive health: correlates of knowledge about pregnancy and maternal and sexual health. J Biosoc Sci 32: 237-251. [Crossref]
- Chang LW, Kagaayi J, Arem H, Nakigozi G, Ssempijja V, et al. (2011) Impact of a mhealth intervention for peer health workers on AIDS care in rural Uganda: A mixed methods evaluation of a cluster-randomized trial. AIDS Behav 15: 1776-1784. [Crossref]
- Little A, Medhanyie A, Yebyo H, Spigt M, Dinant GJ, et al. (2013) Meeting Community Health Worker Needs for Maternal Health Care Service Delivery Using Appropriate Mobile Technologies in Ethiopia. Plos One 8: e77563. [Crossref]
- Madon, S, Amaguru JO, Malecela MN, Michael E (2014) Can mobile phones help control neglected tropical diseases? Experiences from Tanzania. Social Sci Med 102: 103-110.
- Chib A, Chen VH (2011) Midwives with mobiles: A dialectical perspective on gender arising from technology introduction in rural Indonesia. New Media & Society 13: 486-501.
- Guri-rosenblit S (2009) Distance Education in the Digital Age : Common Misconceptions and Challenging Tasks. Distance Education 23: 105-122.
- Haque M, Hossain S, Rumana Ahmed K, Sultana T, Chowdhury HA, et al. (2015) A Comparative Study on Knowledge about Reproductive Health among Urban and Rural Women of Bangladesh. J Family Reprod Health 9: 35-40. [Crossref]
- Kabir H, Saha NC, Oliveras E, Gazi R (2013) Association of programmatic factors with low contraceptive prevalence rates in a rural area of Bangladesh. Reprod Health 10: 31. [Crossref]
- Kendall T, Langer A (2015) Critical maternal health knowledge gaps in low- and middle-income countries for the post-2015 era. Reprod Health 12: 55. [Crossref]



