Abstract
Objective: The aim of this study was to investigate the role of the ‘angle of progression’ (AOP) in the prediction of vaginal delivery and establish a cut-off value.
Method: 101 pregnant women were included in this prospective study. They were admitted in labor to our hospital and had singleton cephalic presentations and full-term pregnancies. AOP was measured at admission time. We analyzed the results of all the women included but also a subgroup of 66 singleton pregnant women whose assessment of the AOP was performed at the beginning of the second stage of labor.
Results: Ninety-one patients had a vaginal delivery (90%) and 19 a cesarean section (10%).The area under the curve was 0.85 (95% confidence interval [CI], 0.77–0.92)and the value of the AOP that optimizes the curve was 125º (S 67.1% E 100%). In the subgroup that was assessed at the second stage of labor, the area under the curve was 0.97 (95%CI,0.90–0.99) and a value of the AOP that optimizes the curve was also 125º (S 91.38% E 100%).
Conclusions: The angle of progression is a simple and reliable intrapartum ultrasound parameter for the evaluation of fetal head descent. Transperineal ultrasound assessment could help to decide the method of delivery. In our experience, the sensitivity of the ultrasound measurement increases when this is taken in the second stage of childbirth.
Key words
intrapartum ultrasound, transperineal ultrasound,angle of descent, angle of progression, sonopartogram, vaginal delivery
Introduction
To detect patients at risk of cesarean section is important to improve perinatal results, as well as the satisfaction of mothers in their childbirth experience [1]. As failure to progress during labor is one of the main causes of cesarean section, its accurate and reliable prediction will lead to a reduction of unplanned emergency cesarean. In the last years, the rate of cesarean section has increased and a common reason for its indication is the fetal head station during labor and the failure to progress in labor.
There is evidence that the subjective digital vaginal examination to determine the position, rotation and descent of the fetal head during delivery may not be accurate [2-4]. Recent studies show that ultrasonographical assessment of fetal head descent through use of intrapartum ultrasound can help to solve these limitations [5-7].
The angle of progression (AOP) is a simple and reliable ultrasound parameter for the assessment of the descent of the fetal head. A strong inverse correlation between the angle of progression and the head-perineum distance has been detected. The direction of the head was defined by Henrich et al. [8] as the angle between the infrapubic line of the pelvis (a line perpendicular to the longest diameter of the pubis from the lower border) and another line drawn perpendicular to the widest diameter of the fetal head. Ghi et al. [2] combined the direction of the fetal head with the degree of midline rotation of the fetal head to establish pelvic descent and vaginal delivery prognosis but It was Barbera [5] who described the angle of descent. This last parameter also allows us to evaluate the presence of caput succedaneum and the molding of the fetal head.
The aim of this study is to analyze this parameter (AOP), and to determine the angle of descent below which the vaginal delivery is not accomplished.
Materials and methods
Prospective observational study was carried out during 2015. The patients included in the study signed an informed consent. A single determination of the descent angle was performed.
To obtain the AOP, a transducer was covered with ultrasound gel and a latex glove and located between the labia below the pubic symphysis in a mid-sagittal position. A sagittal view of the long axis of the pubic symphysis was obtained by a small lateral movement of the transducer, at the same plane, and a sagittal view of the leading portion of the fetal head was discerned (Figure 1). A line was drawn between calipers placed at the two ends of the long axis of the pubic symphysis and a second line was drawn from the distal point of the pubic symphysis tangentially to the fetal skull contour. The angle between these two lines (AOP) was measured. This measurement is independent of the obstetrician's experience, based on the identification of two visible bone structures easily [9,10]. All ultrasound examinations were carried out by the authors using an Acuson Antares machine with a 2-3MHz convex transducer.
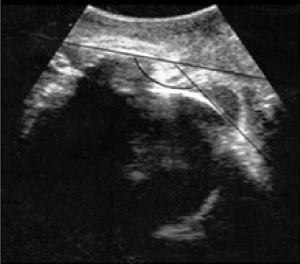
Figure 1. Angle of descent.
The inclusion criteria were: singleton pregnancy, at least 37 + 0 weeks of pregnancy and longitudinal cephalic fetus presentation. The exclusion criteria were: preterm delivery, other than longitudinal cephalic fetus presentation; multiple pregnancy, uterine abnormalities, condition after uterus surgery, pathological intrapartum cardiotocography and the refusal of the patient to participate in the study.
According to inclusion and exclusion criteria, 101 pregnant women were evaluated from the active phase of labor as demonstrated by regular uterine contractions and cervical dilatation ≥3 cm and were followed up until delivery. This study was approved by the Institutional Ethics Committee of our hospital. Subgroup analysis was performed by pregnant women with intrapartum ultrasound evaluation in the second stage of labor and the results of both groups have been compared.
The data has been analyzed with SPSS 17.0. A univariate descriptive analysis of the mean, the interval and the standard deviation for continuous variables, and of absolute frequency and percentages for the categorical variables has been performed. The results among groups (vaginal birth or cesarean section) have been related by t-Student (continuous variables) and the Chi-square test (categorical variables), establishing as a statistical significance a p <0.05. We have obtained a ROC curve and a table with the rate of vaginal delivery depending on the AOP.
Results
One hundred and one pregnancies were enrolled into the study. Comparing women who had vaginal deliveries to those who had a cesarean section, we did not observe significant differences in maternal age, maternal body mass index, gestational age at delivery, weight of newborns or neonatal outcomes (Table 1).
|
Media (DE or %) |
|
|
N=101 |
N=66 |
Maternal age (years) |
29,7 (5,7) |
30,1 (5,7) |
Gestational age (weeks) |
39,1 |
39,6 |
Maternal body mass index |
24,6 (5.2) |
24,3 |
Nulliparous (%) |
44,5 |
44,6 |
Multiparous (%) |
55,5 |
55,4 |
Birthweight (g) |
3349 (370) |
3391 (327) |
Adverse neonatal outcomes |
0 |
0 |
Table 1. Characteristics of the studied population.
Spontaneous vaginal delivery occurred in 72 (71%) women, instrumental delivery in 19 (19 %) and cesarean section in 10 (10%). The cesarean section deliveries were due to failures in the progression of labor in first or segon stage of labor. As expected, the lenght of labor and specifically the second stage of labor were significantly longer in the cesarean section group than in the vaginal delivery group (p <0.001).
We noticed an inverse and significant relationship between the angle of descent and the duration of the second stage of labor, so at a greater angle of descent, a shorter duration of the second stage was found (p = 0.01).
The average angle of progression was 129,4º(SD 19.9).In vaginal deliveries, it was 131.9º compared to 107.5º in cesarean sections (p<0.001). There were no differences between spontaneous vaginal delivery (141.4°, SD15.4) and assisted vaginal delivery (142.4 °, SD 13) (Figure 2).
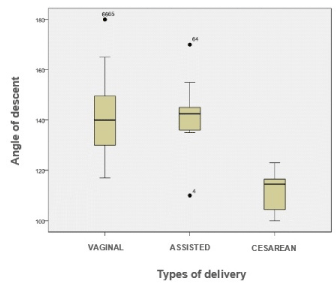
Figure 2. Comparison between the average angle of progression of vaginal, assisted and cesarean delivery.
The ROC curve for the descent angle for vaginal delivery showed an area under the curve (AUC) of 0.85 (95% confidence interval [CI], 0.77-0.92).The value of the angle of descent that optimizes the curve is 125º (S 67.1%, E 100%). There was not a cesarean section with an angle greater than 125° (Figure 3).
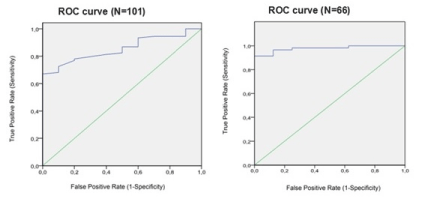
Figure 3. The ROC curve for the descent angle for vaginal delivery and the subgroup studied.
We decided to analyze a subgroup of 66 singleton pregnant women whose assessment of the AOP was performed at the beginning of the second stage of labor.The average angle of progression in this case was 138º (SD 17.2).
The ROC curve for the descent angle for vaginal delivery showed an area under the curve (AUC) of 0.97 (95% confidence interval [CI], 0.90-0.99).The value of the angle of descent that optimizes the curve is 125 º (S 91.38%, E 100%).
In this group, the average angle obtained in vaginal deliveries was 141.6º (SD 14.8, 110-180) compared to 111.8º (SD 8.3, 100-123) in cesarean section, a statistically significant difference. Nevertheless, 5 vaginal deliveries have presented angles of descent between 110-124º.
2021 Copyright OAT. All rights reserv
Discussion
Ultrasound can be used to assess the progress of labor. The use of the ecography allows to determine the position of the fetal head and improves the diagnosis, compare to the digital vaginal exam, in particular in cases of posterior and transverse presentations, in the presence of caput succedaneum and asynclitism [3,4]. They also improve the comfort of the pregnant woman, compared to digital exploration [11]. Souka noted that assessment of fetal head position by digital examination, wich is dependent and poorly reproducible by another operator, was not possible in 61% of cases in the first stage and 31% in the second stage of labor [12].
Molina et al. [7], among other authors [13,14], evaluated the reproducibility of the different ultrasound parameters used to assess the evolution of delivery and concluded that the angle of descent is the most reproducible parameter for measuring fetal head progression during labor, whereas Duckelmann et al. [10], showed that the determination of this ultrasound parameter is also independent of the professional's experience.
We agree with Zúñiga et al. [6], who found a negative correlation between the angle of descent and the duration of the expulsive period, and that a greater angle of descent during the second stage of labor was significantly associated with a shorter expulsion stage.
In the literatute, Kalache et al. [15], documents a strong relationship between the echographic measurement of the angle of descent and the type of delivery after a prolonged expulsive stage. For this, 41 women were evaluated at term and showed that at a progressive angle of 120°, the probability of a vaginal delivery was 90%. In our population, the value of the angle of descent was 125º with a 85 % probability of vaginal delivery but it improves up to 97% if we analyze it in the second stage of labor group.
Unlike Sainz et al. [16], who set the angle of progression for non-difficult instrumentalization at 128°, we found no difference in the mean fall angle between spontaneus vaginal delivery (141.4°) and forceps-assisted delivery (142.4º). We agree with the latter author when affirming that intrapartum ultrasound can be useful in assessing the performance of an instrumented delivery. Different authors have applied this tool to decrease the rate of failures in the instrumentation in a satisfactory way [15,17].
Conclusions
The use of ultrasound during delivery is a reality and it is increasing, but the application of this technology in the field of childbirth care has defenders and detractors. One concern is that advances in intrapartum ultrasound involve excessive reliance on technology. As long as there are no large prospective studies on the subject, the evidence for routine use remains under discussion.
Intrapartum ultrasound examination is a useful and objective tool to assess the progress of labor. During the second stage of labor may play a role in deciding how to end the pregnancy. The angle of descent is the most reproducible ultrasound parameter for the assessment of fetal head descent during labor and it is directly proportional to the probability of vaginal delivery.
In our experience, there has been no cesarean section with an angle of descent equal or greater than 125º. Furthermore, the sensitivity of the technical ultrasound increases when this is performed in second stage of labor.
References
- Yeo L, Romero R (2009) Sonographic evaluation in the second stage of labor to improve the assessment of labor progress and its outcome. Ultrasound Obstet Gynecol 33: 253-258. [Crossref]
- Ghi T, Farina A, Pedrazzi A, Rizzo N, Pelusi G, et al. (2009) Diagnosis of station and rotation of the fetal head in the second stage of labor with intrapartum translabial ultrasound. Ultrasound Obstet Gynecol 33: 331-336. [Crossref]
- Sherer DM, Abulafia O (2003) Intrapartum assessment of fetal head engagement: comparison between transvaginal digital and transabdominal ultrasound determinations. Ultrasound Obstet Gynecol 21: 430-436. [Crossref]
- Yuce T, Kalafat E, Koc A (2015) Transperineal ultrasonography for labor management: accuracy and reliability. Acta Obstet Gynecol Scand 94: 760-765. [Crossref]
- Barbera AF, Pombar X, Perugino G, Lezotte DC, Hobbins JC (2009) A new method to assess fetal head descent in labor with transperineal ultrasound. Ultrasound Obstet Gynecol 33: 313-319. [Crossref]
- Renato Zúñiga, John Apaza, Sergio Puma, Gustavo Chávez, Luis Cáceres (2013) Ecografía translabial intraparto en la determinación del tiempo de duración de período expulsivo. Rev Peru Gin Obs 59: 255-260.
- Molina FS, Terra R, Carrillo MP, Puertas A, Nicolaides KH (2010) What is the most reliable ultrasound parameter for assessment of fetal head descent? Ultrasound Obstet Gynecol 36: 493-499. [Crossref]
- Henrich W, Dudenhausen J, Fuchs I, Kamena A, Tutschek B (2006) Intrapartum translabial ultrasound (ITU): sonographic landmarks and correlation with successful vacuum extraction. Ultrasound Obstet Gynecol 28: 753-760. [Crossref]
- Hassan WA, Eggebø T, Ferguson M, Gillett A, Studd J, et al. (2014) The sonopartogram: a novel method for recording progress of labor by ultrasound. Ultrasound Obstet Gynecol 43: 189-194. [Crossref]
- Dückelmann AM, Bamberg C, Michaelis SA, Lange J, Nonnenmacher A, et al. (2010) Measurement of fetal head descent using the 'angle of progression' on transperineal ultrasound imaging is reliable regardless of fetal head station or ultrasound expertise. Ultrasound Obstet Gynecol 35: 216-222. [Crossref]
- Seval MM, Yuce T, Kalafat E, Duman B, Aker SS, et al. (2016) Comparison of effects of digital vaginal examination with transperineal ultrasound during labor on pain and anxiety levels: a randomized controlled trial. Ultrasound Obstet Gynecol 48: 695-700. [Crossref]
- Souka AP, Haritos T, Basayiannis K, Noikokyri N, Antsaklis A (2003) Intrapartum ultrasound for the examination of the fetal head position in normal and obstructed labor. J Matern Fetal Neonatal Med 13: 59-63. [Crossref]
- Tutschek B1, Braun T, Chantraine F, Henrich W (2011) A study of progress of labour using intrapartum translabial ultrasound, assessing head station, direction, and angle of descent. BJOG 118: 62-69. [Crossref]
- Dietz HP1, Lanzarone V, Simpson JM (2006) Predicting operative delivery. Ultrasound Obstet Gynecol 27: 409-415. [Crossref]
- Kalache KD, Duckelmann AM, Michaelis SA, Lange J, Cichon G, et al. (2009) Transperineal ultrasound imaging in prolonged second stage of labor with occipitoanterior presenting fetuses: How well does the ‘angle of progression’ predict the mode of delivery? Ultrasound Obstet Gynecol 33: 326-330. [Crossref]
- Antonio Sainz J, Borrero C, Aquise A, García-Mejido JA, Gutierrez L, et al. (2016) Intrapartum translabial ultrasound with pushing used to predict the difficulty in vacuum-assisted delivery of fetuses in non-occiput posterior position. J Matern Fetal Neonatal Med 29: 3400-3405. [Crossref]
- Barak O, Levy R, Flidel O, Zaks S, Gillor M, et al. (2017) The Routine Use of Intrapartum Ultrasound in Clinical Decision-Making during the Second Stage of Labor - Does It Have Any Impact on Delivery Outcomes? Gynecol Obstet Invest. [Crossref]



