Introduction
“The only source of knowledge is experience”: Albert Einstein.
It can be quite challenging and daunting to see a patient with wide complex tachycardia (WCT) in the emergency room and try to sort it out in terms of its diagnosis and treatment. A WCT is defined as a rhythm with a ventricular rate of more than 100 beats per minute and QRS duration of more than 120 msec.
By early 1980s, Adenosine had been accepted as an excellent mode of pharmacologic treatment of SVT (supraventricular tachycardia) [1-2]. It was being used in all scenarios: out of the hospital and the hospital settings, all age groups, pregnancy, pre-excitation syndromes and hemodynamic instability. By 1992, Adenosine had been accepted as the 1st line of agent for the treatment of hemodynamically stable SVT and incorporated into the American Heart Association (AHA) ACLS (Advanced Cardiac Life Support) protocol for its management [3].
To simplify the approach to this clinical scenario, the ER (Emergency Room) docs/health care providers will have to first and foremost decide if it is WCT. Once that decision is made, we will then proceed with the treatment keeping in mind the differential diagnosis of WCT: 1. VT. 2. SVT with aberrancy (existing Left or Right Bundle Branch Block) (LBBB or RBBB). 3. SVT with accessory pathways (eg WPW syndrome: Wolf-Parkinsons-White syndrome). 4. Drugs or electrolyte abnormalities (eg severe hyperkalemia). 5. Some cardiomyopathies with abnormal ECGs. 6. Ventricular pacing.
The pharmacologic management of wide complex tachycardia (WCT) is a different story altogether. It is so very critical to choose the right kind of medication once the decision is made to treat a patient with wide complex tachycardia. Calcium channel blockers (Diltiazem and verapamil) are strongly advised not to be used for fear of hemodynamic collapse, hypotension and cardiac arrest [4]. Digoxin should not be used for the same reasons as it may increase the conduction via the accessory pathway and thereby making the tachycardia uncontrollable and thus worsening the clinical scenario. Beta-blockers can affect the condition adversely by facilitating AV conduction via the accessory pathway and thus increasing the ventricular rate causing hypotension and hemodynamic collapse.
The Hippocratic Oath: “first, do no harm” (or “primum non nocere") is most applicable when it comes to taking care of patients with wide complex tachycardia. Not only you want to make the diagnosis as soon as possible (ASAP) but also the treatment is to be initiated as soon as possible to reduce the likelihood of any morbidity and mortality.
The classic teaching over the years has been that all cases of WCT are to be treated as Ventricular tachycardia (VT) until proven otherwise. Therefore, unless the provider is absolutely certain that the WCT is supraventricular in origin, the medications used for SVT protocol should not be used at all for the treatment of WCT [5].
As far as adenosine treatment as an IV bolus for the condition of WCT is concerned, it can work both as diagnostic as well as therapeutic option. If the WCT is with Aberrancy, it is likely to respond to IV Adenosine; likewise, a few idiopathic VT, for example fascicular VT is likely to respond to adenosine [6]. Regarding its diagnostic value, adenosine can help us diagnose the underlying rhythm/etiology of WCT by slowing the ventricular rate or unmasking the accessory pathway [7]. Because of continued concerns related to its potential side effects of worsening various tachycardias, causing atrial fibrillation and Torsade de pointes, in the past, Adenosine was recommended as per the AHA guidelines 2005 [5] to be used in case of WCT only if it was known to be a case of Aberrancy (that is patient is known to have underlying LBBB or RBBB).
However, based on our current knowledge this concept has been changing rapidly. Before I go on to discuss the current status of adenosine usage in WCT, let me present a case 1st:
Case presentation
An 87-year old pleasant retired nurse with history of hyperthyroidism, hypertension and arthritis developed palpitations, shortness of breath and dizziness. As the symptoms were not subsiding, paramedics were called in. A rhythm strip (Figure 1) showed a regular wide complex tachycardia with the ventricular rates of 140-165 beats per minute. She was hemodynamically stable and therefore paramedics decided to give her 6 mg of IV adenosine. She did not respond to that. Thereafter she was given 12 mg of IV adenosine with no response. At times, especially at the end of the strip, the rhythm appears being irregular. However, it could also be secondary to sinus arrhythmia due to all the stress and anxiety at the time!
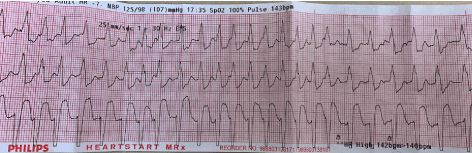
Figure1. WCT with stable hemodynamics
She continued to have palpitations and shortness of breath and her WCT persisted. Her systemic BP has dropped and she revealed significant bradycardia, pause and asystole (Figure 2). She also showed some changes suggestive of underlying atrial fibrillation! At that point, she was given IV 5 mg Verapamil.
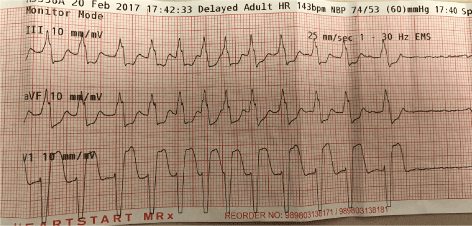
Figure 2. No response after 6 and 12 mg of IV adenosine
Her WCT did respond; she converted back to sinus and her hemodynamics came back to normal as well (Figure 3). She started to feel much better and she was brought to our local ER for further work up and evaluation (Figure 4).
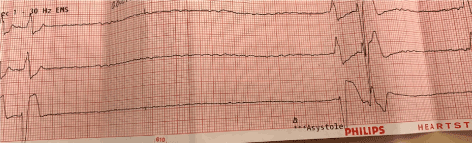
Figure 3. After 2 doses of Adenosine and IV Verapamil
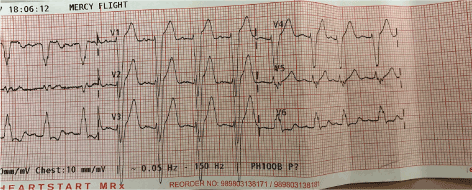
Figure 4. Responding to Rx with normal sinus and bundle branch block:
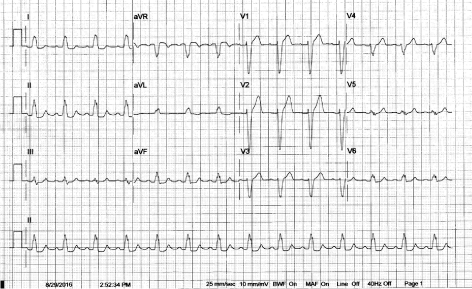
Figure 5. Baseline ECG: Known to have LBBB over the years:
She was admitted overnight. Her routine blood work was normal. Her troponins were unremarkable. Her recent 2D-Echocardiography was reported to be normal with preserved LV systolic function.
She was being treated with Methimazole by her endocrinologist for hyperthyroidism. A week before hospitalization, her Methimazole was reduced from 10mg to 5 mg a day. In the hospital, her TSH (thyroid-stimulating hormone) level was 21. She was discharged on Metoprolol 25 mg twice a day with follow-up plans with her endocrinologist and cardiology follow-up was set up in my office with possible EP evaluation thereafter if she would be willing.
Discussion
The traditional teaching has been that about 80% patients presenting with WCT are eventually diagnosed with VT and the rest 20% will have SVT with aberrancy and a few rare diagnoses as mentioned before. Based on that knowledge and patient’s clinical history, a regular WCT should be assumed to VT until proven otherwise. If the patient is hemodynamically stable, a trial of antiarrhythmic therapy (with Amiodarone, Procainamide or other antiarrhythmic agents) is warranted keeping in mind that in case the patient becomes unstable/decompensated, cardioversion must be carried out immediately [4].
With the availability and increasing experience with adenosine usage, it should certainly be tried in this case scenario. If a patient with WCT is a case of SVT with aberrancy, it might convert the rhythm to normal. Some cases of adenosine-sensitive VT, mostly originating from right ventricular outflow tract (RVOT) may respond to adenosine as well.
On the other hand, if it is truly a case of VT, adenosine might not help. However, because of its very short half-life (less than 9 seconds), the adverse side-effects, if any, will resolve quickly and therefore will not hurt the patient [8]. While this is perfectly right approach NOW as mentioned in the latest AHA ACLS guidelines of 2017 to use adenosine as the first line of treatment in stable WCT [9], this was NOT the case before due to fear of hypotension, hemodynamic collapse and cardiac arrest [5].
“Drugs are of priceless value when needed, but they are at best emergency measures of most temporary utility…… the more effective they are at the right place, the more harmful in the wrong one.”: Woods Hutchinson, MD (1862-1930). Civilization and Health. “Chapter II: The Dawn of the New Doctor.” 1914.
In the management of this patient, 2 doses of adenosine were given and that was perfectly right thing to do. However, at that point when the patient did not respond, she was given IV Verapamil. Knowing that she did not respond to adenosine and given that it was a case of WCT at her age of 87 (likely to have underlying CAD, history of MI etc), one could assume that WCT being more likely a case of VT (about 80% likelihood) and therefore Amiodarone should have been tried or cardioversion should have been considered and Verapamil should not have been given! However, Verapamil WAS given and she did respond to it favorably!
There is a Victorian expression: “The operation was a success but the patient died.” (Harvard death)
In our case, the opposite happened: ‘The patient outcome was successful in spite of ‘wrong’ approach!’
‘ONE MORE THING’:
One critical aspect of this WCT story that I have not mentioned so far is that the patient was known to have left bundle branch block (LBBB) over the years. She being a mentally sharp, retired nurse knew this about her ECG. However, in the current situation of undue shortness of breath, palpitations and dizziness, I am sure she did not remember to tell the paramedics that she is known to have LBBB. Moreover, I am quite certain that the paramedics would not have had time or thoughts to ask her if she was known to have an abnormal ECG (BBB).
“A doctor who cannot take a good history and a patient who cannot give one are in danger of giving and receiving bad treatment.”
Hindsight can always be 20/20 being aware that she was known to have LBBB on her ECG and therefore we could have easily concluded that her WCT was SVT with aberrancy and not VT! (Therefore, in hindsight it was not ‘wrong’ to give Verapamil after failed adenosine attempt in case the paramedics knew that she was known to have LBBB!)
“The fact that your patient gets well does not prove that your diagnosis was correct!”
“Patients pay the doctor for their troubles; for his kindness, they still remain in his debt.”
Update on this case
She underwent an EP st2021 Copyright OAT. All rights reservode-physiology SVT. She underwent slow pathway catheter ablation. Her SVT could be easily reproduced in the EP lab before the ablation but it could not be reproduced after the ablation. It goes to show that every case of wide complex tachycardia is not ventricular tachycardia!
Conclusion
Any symptomatic patient with WCT should receive adenosine as the first line of medication for diagnostic as well as for therapeutic reasons as long as the patient is hemodynamically stable. If adenosine fails, an antiarrhythmic agent (like amiodarone or procainamide) should be the next line of management if the patient is hemodynamically stable and cardioversion is to be carried out immediately if the patient becomes unstable.
References
- DiMarco JP, Sellers TD, Berne RM, West GA, Belardinelli L (1983) Adenosine: electrophysiologic effects and therapeutic use for terminating paroxysmal supraventricular tachycardia. Circulation 68: 1254-1263. [Crossref]
- Belhassen B, Pelleg A, Shoshani D, Geva B, Laniado S (1983) Electrophysiologic effects of adenosine 5'-triphosphate on atrioventricular reentrant tachycardia. Circulation 68: 827-833. [Crossref]
- (1992) Guidelines for cardiopulmonary resuscitation and emergency cardiac care. Emergency Cardiac Care Committee and Subcommittees, American Heart Association. Part III. Adult advanced cardiac life support. JAMA 268: 2199-2241. [Crossref]
- McGovern B, Garan H, Ruskin JN (1986) Precipitation of cardiac arrest by verapamil in patients with Wolff-Parkinson-White syndrome. Ann Intern Med 104: 791-794. [Crossref]
- (2005) AHA ACLS Guidelines (Tachycardia with pulses). Circulation 112: iv-70.
- Kassotis J, Slesinger T, Festic E, Voigt L, Reddy CV (2003) Adenosine-sensitive wide-complex tachycardia: an uncommon variant of idiopathic fascicular ventricular tachycardia--a case report. Angiology 54: 369-372. [Crossref]
- Ilkhanipour K, Berrol R, Yealy DM (1993) Therapeutic and diagnostic efficacy of adenosine in wide-complex tachycardia. Ann Emerg Med 22: 1360-1364. [Crossref]
- Schuller JL, Varosy PD, Nguyen DT (2013) Wide complex tachycardia and adenosine. JAMA Intern Med 173: 1644-1646. [Crossref]
- ACLS 2017 Guidelines; AHA 2015 ACLS Recommendations, published in Circulation 2015.





