Diaphragmatic hernias are commonly classified as either congenital or acquired and traumatic or non-traumatic. Non-traumatic diaphragmatic hernia with liver herniation is extremely rare. In view of the rarity of this lesion and its likely confusion with other diagnosis like pulmonary or cardiac lesions, we present a case of non-traumatic liver herniation in a 55-year-old female patient. She presented with worsening breathlessness over a 5-day period. Chest x-ray revealed a large right homogenous paracardiac mass. Computed tomography of thorax with abdomen revealed a defect in the diaphragm through which liver segments were seen herniating into the thoracic cavity (cottage loaf sign). She was managed symptomatically and at present, she is awaiting surgical management of the liver herniation. Though non-traumatic diaphragmatic herniation is extremely rare, clinicians should be aware of this condition and should consider it among the differentials of chest x-ray abnormalities.
Liver, hernia, diaphragm, spontaneous
Diaphragmatic hernias are commonly classified as either congenital or acquired and traumatic or non-traumatic. Although several cases have been reported, non-traumatic liver herniation into the thoracic cavity is extremely rare [1,2]. In view of the rarity of the lesion and its likely confusion with other diagnosis like a pulmonary or cardiac lesion, we present a case of non-traumatic liver herniation in a 55-year-old female patient whose chest x-ray showed a right homogenous paracardiac lesion.
A 55-year-old female presented with worsening breathlessness over a 5-day period. She also gave history of low grade fever and cough for the same duration. Her past medical history was remarkable for bronchial asthma. On examination, patient had decreased breath sounds in right mammary, infra-axillary and infra-scapular area and dull note on percussion in the same areas. Patient was clinically suspected to have right side pleural effusion. Chest x-ray revealed a large right homogenous paracardiac mass (Figure 1). CT thorax with abdomen revealed a defect in the diaphragm through which segments 8 and 4a of the liver were seen herniating into the thoracic cavity (Figures 2 & 3). The herniated liver was seen constricted by the diaphragm at the rupture site giving rise to the classical “cottage loaf sign”. She was managed with conservative measures and at present, she is awaiting surgical management of the liver herniation.
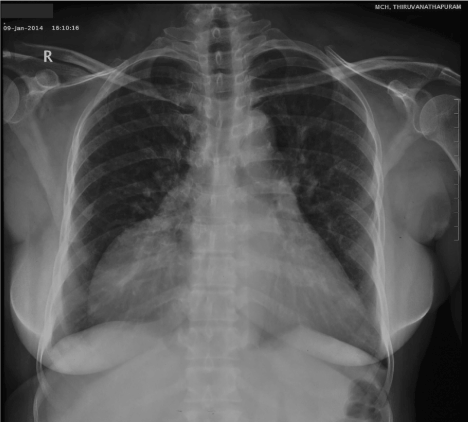
Figure 1. Chest X-ray showed a large right cardiophrenic homogenous mass.
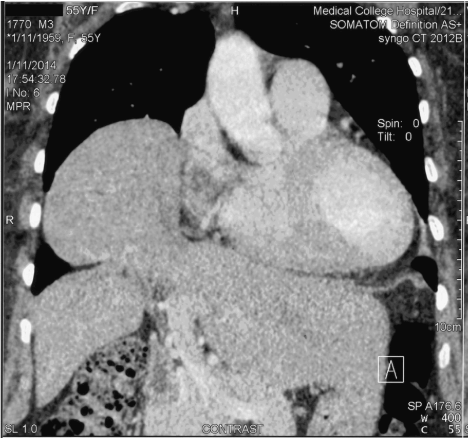
Figure 2. CT chest (coronal) showed the diaphragm defect through which the liver is seen herniating into the thoracic cavity (Cottage loaf sign).
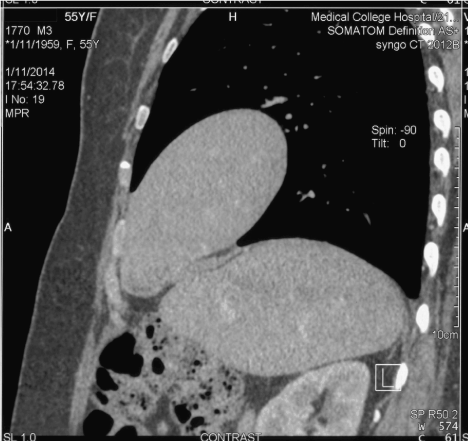
Figure 3. CT chest (sagittal) showed the diaphragm defect through which the liver is seen herniating into the thoracic cavity (Cottage loaf sign).
Diaphragmatic hernias can be divided into two categories namely congenital and acquired defects. Trauma is the leading cause of acquired diaphragmatic hernias. Spontaneous diaphragmatic rupture describes the rupture of the diaphragm due to increasing pressure in the abdominal cavity and chest wall without any direct trauma [3]. The most common reasons for non-traumatic diaphragmatic herniation are coughing, physical exercise, and vaginal child birth.4 Our patient had history of chronic cough which could have possibly caused the diaphragmatic rupture in our patient. In a study by Losanoff and colleagues,4 spontaneous rupture of the diaphragm was predominantly seen on the left (68%). Right sided diaphragmatic hernias are very rare because of the protective effect of liver. In our patient, herniation was on the right which further added to the diagnostic dilemma.
The commonly herniating organs in spontaneous diaphragmatic rupture are the stomach, colon and omentum [4]. The only organ which herniated through the diaphragmatic defect in our patient was the liver. The most common symptoms of diaphragmatic rupture are abdominal or thoraco-abdominal pain, nausea, vomiting, and dyspnoea [4]. Though our patient presented with breathlessness, the possibility of diaphragmatic hernia was initially not considered, because she had an underlying respiratory condition (bronchiectasis).
Single or serial plain chest radiographs are diagnostic in most cases of diaphragmatic rupture. The computed tomography of the thorax is the imaging modality of choice in these patients but the sensitivity varies between 71% and 90% [5,6]. The diagnosis of diaphragmatic hernia with liver herniation was confirmed with computed tomography in our patient. The characteristic “cottage loaf” sign was seen in the computed tomographic images, confirming the diagnosis of liver herniation through a diaphragmatic defect. A cottage loaf sign, occurs as a result of partial herniation of liver through a diaphragmatic defect. The herniated component is separated by a waist at the diaphragm from the larger intra-abdominal component. This shape resembles cottage loaf, a particular shape of bread in which larger and smaller spherical structures are squashed together, forming a cottage shape [7].
Definitive treatment of diaphragmatic rupture is surgery and the surgical approach is determined by the location and duration of the diaphragmatic rupture. The transthoracic approach is the most appropriate way of removing adhesions in the absence of any abdominal pathology or in delayed cases. The defect may be repaired primarily or by using prosthetic mesh
Non-traumatic diaphragmatic hernia of the liver in an adult is an extremely rare right-sided diaphragmatic hernia. A high index of suspicion is needed to diagnose diaphragmatic rupture and should be distinguished from other conditions like pulmonary and cardiac lesions. The computed tomography of the thorax is the imaging modality of choice in these patients. The diagnosis and evaluation of non-traumatic diaphragmatic hernia of the liver can help optimize surgical management.
- Pataka A, Paspala A, Sourla E, Bagalas V, Argyropoulou P (2013) Non traumatic liver herniation due to persistent cough mimicking a pulmonary mass. Hippokratia 17: 376-377. [Crossref]
- Luo HF, Lei T, Wang HJ, Tan G, Wang ZY (2007) Non-traumatic diaphragmatic hernia of the liver in an adult: a case report. Hepatobiliary Pancreat Dis Int 6: 219-221. [Crossref]
- Akbar A, Parikh DH, Alton H, Clarke JR, Weller PH, et al. (1999) Spontaneous rupture of the diaphragm. Arch Dis Child 81: 341-342. [Crossref]
- Losanoff JE, Edelman DA, Salwen WA, Basson MD (2010) Spontaneous rupture of the diaphragm: case report and comprehensive review of the world literature. J Thorac Cardiovasc Surg 139: e127-128. [Crossref]
- Matsevych OY (2008) Blunt diaphragmatic rupture: four year's experience. Hernia 12: 73-78. [Crossref]
- Iochum S, Ludig T, Walter F, Sebbag H, Grosdidier G, et al. (2002) Imaging of diaphragmatic injury: a diagnostic challenge? Radiographics 22 Spec No: S103-116. [Crossref]
- Roche CJ, O'Keeffe DP, Lee WK, Duddalwar VA, Torreggiani WC, et al. (2002) Selections from the buffet of food signs in radiology. Radiographics 22: 1369-1384. [Crossref]
2021 Copyright OAT. All rights reserv



