Psammomatoid ossifying fibromas (POF) represent a rare and unique subtype of fibro-osseous lesions with predilection for the paranasal sinuses and orbits. They have specific histopatholgic features with tendency toward local aggressive behavior with invasion and destruction of adjacent anatomic structures. Symptoms include proptosis, facial swelling, nasal obstruction, pain, sinusitis and headaches, depending on the location of the lesion [1]. Secondary extension to the skull or cranial fossa can occur from a sinonasal origin, but a primary location within the cranium is rare [2]. We describe a case of POF involving primarily the right frontal bone of a 10 year-old boy.
The patient is a 10-year-old boy who has a retracted multiyear history of regular right-sided temporal headaches. The patient uses his single index finger to point to the same region of his right temple and states that he experiences this perhaps twice a week. He describes it as a burning sensation that occasionally produces enough discomfort to give him an upset stomach. He had no history of trauma. He was brought to an outside emergency room where a head CT scan was obtained. The study demonstrates an expansile oval shape soft tissue lesion centered in the right frontal bone diploe, bulging into the inner table. There was no significant invasion into the intracranial content.
Given the symptomatic nature of the lesion and its resistance to medical treatment, it was surgically resected. Histological examination revealed a psammomatoid ossifying fibroma.
Psammomatoid ossifying fibroma (POF) is a benign fibroosseous lesion predominantly involving the paranasal sinuses and orbits, with predilection for the children and young adults [1,3]. Multiple synonyms have been used, including juvenile POF (JPOF), given their predilection for this age group, aggressive POF (APOF), indicating their clinical behavior, psammoma-osteoid fibroma, psammous desmo-osteoblastoma and cementifying or cemento-ossifying fibroma [4,5].
The fibroosseous lesions of the sinunasal region include a variety of nonneoplastic and neoplastic entities. The nonneoplastic group includes fibrous dysplasia, aneurismal bone cysts and giant cell granuloma. The neoplastic category includes ossifying fibroma, giant cell tumor, fibromyxoma, osteoblastoma and osteosarcoma [6,7].
From the neoplastic group, POF are unique lesions, considered a subtype of ossifying fibroma, that have predilection to supraorbital locations, the ethmoid sinus, and the maxillary sinus. These lesions are slowly progressive lesions with potential to create sizable defects [1,6,7]. They can, and usually do, occupy multiple, separate anatomic sites. This indicates their aggressive behavior and represents a unique feature compared to the other fibroosseous lesions [8]. Their invasive growth may be extensive involving several paranasal sinuses, the nasal cavity, nasopharynx or palate and cranial cavity. Symptoms include proptosis, facial swelling, nasal obstruction, pain, sinusitis and headaches [6].
They have specific histological features that allow their differentiation from the other groups. The lesion appears as a benign fibroosseous proliferation composed of bony spicules and spherules, admixed with a fibrous stroma. The most distinctive pattern is the presence of mineralized or calcified “psammomatoid” bodies or ossicles. They varies in appearance from small with a round to oval shape, to a larger irregularly shaped ossicles pattern, and they had concentric layering similar to that of pasammoma bodies [2,6].
These ossicles are identified within the bony trabecules as well as within adjacent cellular stoma [6].
The nonosseous component includes a cellular stroma with a fascicular to storiform growth, composed of round to polyhedral to spindle-shaped cells, with prominent basophilic nuclei and inapparent cytoplasmic borders. Within the cellular stroma were mitotic figures, but without mitotic activity or atypical mitoses. There could be cellular polymorphism but anaplasia and necrosis are usually not identified [6].
Radiographic studies are invaluable in diagnosis and in determining the extent of growth. On CT, the lesions are expansile and circumscribed by a thick shell of bone density with a multiloculated, bone density, internal appearance and a content of varying density [3,5,6,8]. Psammomatoid bodies appear radiolucent or like ground glass [8]. Some lesions show aggressive behavior with displacement, bulging or bowing of adjacent bone structures or invasion into adjacent anatomic compartment, including the calvarium and anterior cranial fossa [6,8]. On MRI, APOF are hypointense on T1 and T2 weighted sequences. The bony walls show gadolinium enhancement, suggesting not a reactive hyperostosis, but tumor tissue [3,5].
The differential diagnosis includes mainly fibrous dysplasia, giant cell tumors, aneurysmal bone cysts and cementum producing lesions [6,7].
POF has been also related to fibrous dysplasia, in which calcifications may occur, however, POF is usually well demarcated from surrounding bone, presenting as expansive but circumscribed lesion, whereas fibrous dysplasia is poor delineated osseous expansion that may appear radiolucent, sclerotic or ground glass. In the other hand, mutation of GNAS1 gene has been described in virtually all cases of fibrous dysplasia and their absent in the cases of POF [2,6].
Giant cell tumors are uncommon, and their most common site is sphenoid and ethmoid bone. In these sites, they have no distinctive radiographic features but most of them are lytic and may or not invade adjacent structures. Histologically, they are dominated by multinucleated giant cells that are evenly distributed throughout the lesion. POF may have giant cells but they are usually focally seen and do not represent the dominant cell. Besides, the presence of psammoma bodies separates those two entities [6].
Aneurysmal bone cysts are usually seen in metaphysis of long bones, less than 5% occur in craniofacial bones. They are uncommon in nasal cavity and paranasal sinuses. Radiographically, they are expansile multilocularity radiolucent lesions measuring from 1 to 10 cm. Histologically, they are multicystic lesions filled with blood and lined by fibrous tissue, multinucleated giant cells, or granulation tissue. They have no psammoma bodies [6].
Cementum-producing lesions originate from periodontal and contain structures called cementum “droplets” or cementicles that may resemble the psammomatoid spherules [6]. Because of this similarity, APOF were referred sometimes to cemento-ossifying fibroma. Given real difficulty differentiating them by light microscopy, some authors consider ossifying fibroma and cemento-ossifying fibroma as same lesion. Distinguishing them by imminureactivity and by monoclonal antibody markers and is possible [6].
POF in a neurocranial location has been only rarely reported, and most of reported cases were discovered incidentally while investing for other head and neck or neurological complaint [2]. Our study is special by the POF lesion being the main symptomatic lesion, causing chronic and resistant headaches that lead to medical attention.
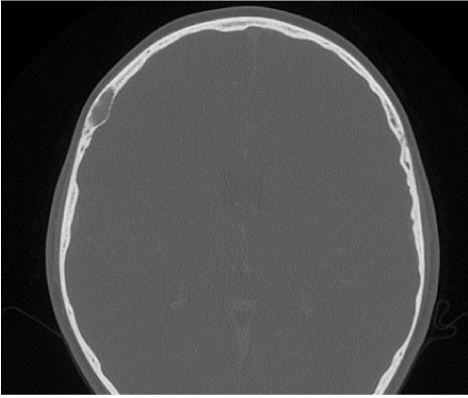
Figure 1. CT scan in reconstructed bone window demonstrates an expansible oval shape soft tissue lesion located in the right frontal bone diploe. No significant invasion was identified into the intracranial content.
In this location a JPOF can be easily mistaken with an intradiploic meningioma, especially that clinical and radiological finding might be strongly similar. POF may be distinguished by the absence of distinct epithelial membrane antigen imminureactivity [2]. Differentiating those two entities may also be impossible by immunohistochemical profile alone, and the diagnosis should then be made with combination with clinical and radiographic findings [4].
Treatment of choice is surgery, and complete resection should be the goal [2,3,6,8]. Incomplete resection leaves a tendency to local invasion and recurrence and can cause significant morbidity. Radiation therapy did not prove efficacy and thus regular radiological follow-up is recommended for incomplete resections [2,3]. Metastases or malignant transformation have not been described.
The prognosis associated with POF is considered good. But their extensive invasion, particularly in the orbits, may result in facial deformity requiring equally extensive surgical intervention [6]. Meningitis secondary to invasion into cranial cavity has been reported. Rarely, death has been reported, whether from secondary infection or direct destruction of vital structures [6]. Malignant behavior has not been reported [4].
In this article we presented a rare location for a rare entity, the psammomatoid ossifying fibromas (POF), which is a rare and unique subtype of fibro-osseous lesions with usual location in the paranasal sinuses and orbits. These lesions, even though benign, have tendency toward local aggressive behavior with invasion and destruction of adjacent anatomic structures, thus the importance of accurate diagnosis and appropriate treatment.
- Pirana S, Zerati F, Voegels R, Maia R (2003) Psammomatoid ossifying fibroma. Rhinology 41: 250-252. [Crossref]
- Hasselblatt M, Jundt G, Greiner C, Rama B, Schmäl F, et al. (2005) Juvenile psammomatoid ossifying fibroma of the neurocranium. Report of four cases. J Neurosurg 102: 1151-4. [Crossref]
- Martínez-Mañas RM, Rey MJ, Gastón F (2002) Aggressive psammomatoid ossifying fibroma. Ann Otol Rhinol Laryngol 111: 466-468. [Crossref]
- Granados R, Carrillo R, Nájera L, García-Villanueva M, Patrón M (2006) Psammomatoid ossifying fibromas: immunohistochemical analysis and differential diagnosis with psammomatous meningiomas of craniofacial bones. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 101: 614-619. [Crossref]
- Affleck BD, Malis DJ, Whittemore DE, Torgerson SJ (2002) Psammomatoid ossifying fibroma of the temporal bone. Otolaryngol Head Neck Surg 126: 585-587. [Crossref]
- Wenig B, Vinh T, Smirniotopoulos J, Fowler C, Houston G, et al. (1999) Aggressive psammomatoid ossifying fibromas of the sinonasal region. A clinicopathologic study of a distinct group of fibro-osseous lesions. Cancer 76: 1155-65. [Crossref]
- Slootweg PJ, Panders AK, Nikkels PG (1993) Psammomatoid ossifying fibroma of the paranasal sinuses. An extragnathic variant of cemento-ossifying fibroma. Report of three cases. J Craniomaxillofac Surg 21: 294-7. [Crossref]
- Khademi B, Niknejad N, Mahmoudi J (2007) An aggressive psammomatoid ossifying fibroma of the sinonasal tract: report of a case. Ear Nose Throat J 86: 400-401. [Crossref]
2021 Copyright OAT. All rights reserv

