Key words
hymenoplasty, vaginoplasty, revirgination
Introduction
Hymenoplasty is the procedure to restore the torn hymen intactness of which is presumed to be sign of virginity. Usual patient is an unmarried girl who had indulged in premarital sex and is going to be married. Academic literature is devoid of details about hymenoplasty procedures. We have found one report [1] which has just described, in not very descript manner and without photographs, the procedure of hymenoplasty. We have described a procedure for hymenoplasty by using the remnants of torn hymen [2]. However many a times our patients after hymenoplasty complained that though they bled but one or two drops only while they wanted more bleeding during first sexual act. For such patients we developed the technique of creating superhymen in which more bleeding is destined to occur on the eve of first sexual intercourse.
Material and method
We have done superhymenoplasty in thirty one patients over period of three years. Twenty females were unmarried and eleven were married or divorcee who came for hymenoplasty after which they expected enough bleeding during first sexual act. None of them were aware of two terms and difference between hymenoplasty and superhymenoplasty. Of thirty one females twenty were accompanied by their parents, five accompanied by their boyfriends and fiancée, while others were unaccompanied by anybody. Eleven females were going to be remarried because of divorce or death of their husbands and those were accompanied by parents. Four women were accompanied by their husbands who wanted restoration of hymen of their wives knowing well that they have lost hymen in premarital sexual intercourse.
The history was taken and all patients were explained that absence of hymen is not a sign of lost virginity; and same is true for bleeding on first night. But all were determined to get the procedure of superhymenoplasty. They were told that in superhymenoplasty more bleeding is destined. Whether to go for hymenoplasty or superhymenoplasty was their personal decision.
Technique
The procedure was done in local or general anaesthesia as per wishes of the patients. In 15 patients procedure was done in local anaesthesia and in remaining patients in general anaesthesia.
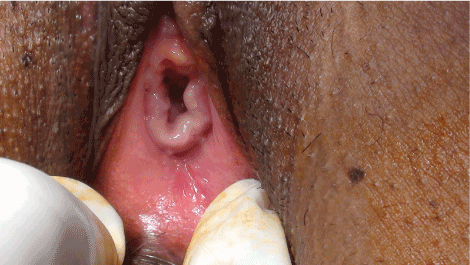
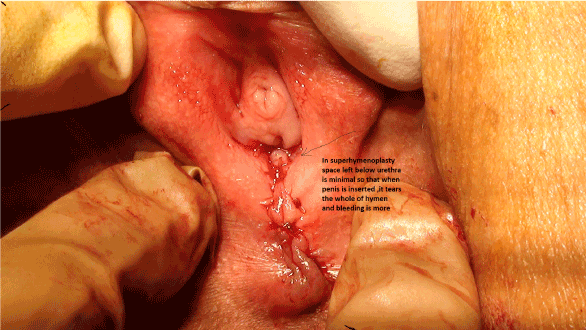
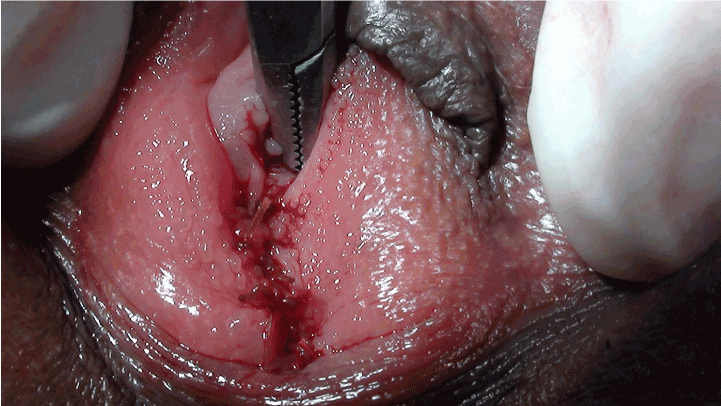
Patients were placed in lithotomy position. Area was prepared and draped. Torn pieces of hymen were incised and incision was continued in remnants up to just below the urethral orifice creating two layers –outer and inner. Inner layer was stitched using chromic catgut 4-0 and outer layer was also stitched using same catgut. When done finally, only small hole was left in hymen just below urethral orifice for menstrual blood and other vaginal secretions to come out. Neosporin ointment was applied over the suture line and no dressing was done. Post operatively patients were advised to clean the area with warm water and apply the ointment. No dressing was required. For pain, analgesic tablets were enough as there was not much pain. For five days combination of Metronidazole and Ofloxacine was given.
Result
During 7 days following operation patients complained of slight pain some times, and slight blood mixed discharge. After one week there was no complaint in any of the patients except in one who complained of pain for as long as one month .
All patients were contacted over phone for follow up afterwards but only 11 patients responded out of which ten expressed their satisfaction with the results on first night regarding bleeding and vaginal tightness. One patient said that she did not bled much except one or two drops but vaginal tightness was virginal as she had felt on the eve of first intercourse done for the first time.
Discussion
Genital plastic surgery for women has come under scrutiny and has been the topic of discussion in the news media, online and in medical journals. In the absence of measurable standards of care, lack of evidence-based outcome norms and little standardization either in nomenclature or training requirements, concern has been raised by both ethicists’ and specialty organizations [3].
The celebration of bloody sheet, portrayed in popular cinema, is based on strong religious and cultural beliefs. The religious books state that a bride has to be a virgin, and according to the custom a woman found on her wedding night to have been “Touched” brings shame to her family. Consequences include divorce to death [4-8].
So availability of facility of hymenoplasty to restore the torn hymen saves many young women from disgrace. However, many a times couples want more bleeding on the eve of first sexual intercourse. When interviewed about reason for wish of more bleeding on first sexual act women said they themselves wanted to feel thrill of gush of blood coming out. And for such couples and women superhymenoplasty procedure is boon.
The operation in no way cause female genital mutilation because only torn pieces of hymen are united after freshening the edges and superhymenoplasty did not cause long term complication in any of 31 patients followed for one year.
Superhymen is name given for the first time by us which simply means creating a hymen in a way that very small hole is left for menstrual blood to come out. When insertion of penis takes place hymen istotear and bleeding is destined to occur. As only left over pieces of hymen are stitched together, no injury to vaginal mucosa takes place. Need of creating superhymen may be questioned by many organizations. However we think that procedure is safe and without any associated complications gives extra satisfaction. So there should not be any objection to it. It is like cosmetic surgery of any part of body which is done just to increase the self-esteem, like augmentation mammoplasty is not necessity but only enhances self-esteem of the women.
Conclusion
A procedure of superhymenoplasty has been described in which superhymen is created which results more bleeding on the eve of first sexual act. It give more satisfaction to the couple. The procedure causes no complications as only torn pieces are used to create the superhymen.
References
- Longmans A, VerhoeffA (1998) who wants the procedure and why. BMJ 316: 459-460. [Crossref]
- Vishwa Prakash (2009) Hymenoplasty — how to do. Indian J Surg 71: 221-223. [Crossref]
- Goodman MP (2009) Female cosmetic genital surgery. ObstetGynecol 113: 154-159. [Crossref]
- Kandela P (1996) Egypt's trade in hymen repair. Lancet 347: 1615. [Crossref]
- O'Connor M (2008) Reconstructing the hymen: mutilation or restoration? J Law Med 16: 161-175. [Crossref]
- Vishwa Prakash (2015) VP, s Flap hymenoplasty. Plastic Surgery International.
2021 Copyright OAT. All rights reserv
- Ou MC, Lin CC, Pang CC, Ou D (2008) A cerclage method for hymenoplasty. Taiwan J ObstetGynecol 47: 355-356. [Crossref]
- Emans SJ, Woods ER, Allred EN, Grace E (1994) Hymenal findings in adolescent women: impact of tampon use and consensual sexual activity. J Pediatr 125: 153-160. [Crossref]