Abstract
Over the past twenty years gynecologic surgery has evolved from primarily abdominal approach to the current focus on minimally invasive surgical techniques. Minimally invasive techniques include vaginal and laparoscopic techniques. Evolution in laparoscopic technology and equipment has exploded to include multiple vessel sealing instruments of varying modalities, instruments with “wristed” capabilities and robotic assisted technology. Single port laparoscopy and natural orifice transluminal endoscopic surgery are other variations of laparoscopic technology.
Vaginal surgery is still touted as the “ultimate” minimally invasive surgery by ACOG; however, its use has not grown over this time. Many surgeons have had limited training in vaginal surgery and are not as comfortable with this approach.
What really is the best approach? Why does it matter what surgical approach is chosen? How are physicians able to gain competency and proficiency in this ever changing environment? How do we improve patient safety and outcomes in gynecologic surgery?
Objectives for Attendees:
- Understand past and current trends in gynecologic surgery
- Understand evidence techniques and technology in gynecology surgery
- Explain benefits to patient safety and cost relating to gynecologic surgery
- Understand training techniques to improve competency in gynecologic surgery
Introduction
Hysterectomies are now performed using several different techniques. These include abdominal, vaginal, laparoscopic, laparoscopic assisted vaginal hysterectomy and now the addition of robotic assisted laparoscopic hysterectomy. These various techniques give both the surgeon and patient options to choose the most beneficial and optimal approach to surgery. It creates added difficulties in structuring gynecologic surgical education programs. These difficulties may cause shifts in surgical exposure for residents away from both abdominal and vaginal approaches [1].
Newer innovations in laparoscopy have helped decrease the numbers of hysterectomies from the abdominal approach. In 2003 hysterectomies were still being performed abdominally in over 70% of the time [2]. In 2005 abdominal hysterectomies were performed at approximately 64%. Fourteen percent were laparoscopic and twenty-two percent were vaginal [3].
The significant current trend in gynecologic surgery is for a more minimally invasive surgical approach. Vaginal and laparoscopic, as well as the added robotic assisted surgery, are all consistent with shorter hospital stays, fasted patient recovery, less blood loss, fewer infection, and increased patient satisfaction. Surgical training for gynecological surgeons should be to produce confident, well-trained physicians with a broad surgical experience consistent with the surgical advances.
History
Past major surgical options for gynecology were limited to abdominal and vaginal surgery. Successful surgery was improved with the development of sterile surgical technique and antibiotics. Hysterectomy is the most common major gynecologic surgery performed in United States with over 600,000 annually. By historical reports, the first successful abdominal hysterectomy was performed in 1843 by Charles Clay (England). In the United States, Edward Richardson is credited with the first abdominal Hysterectomy in 1929 [4]. Vaginal hysterectomy has also been performed dating back to 120 AD by Soranus of Ephesus. Vaginal surgery and hysterectomy have been performed by many in Europe over 17th and18th centuries. In the United States, in 1861 Choppin, of New Orleans, is credited for performing successful vaginal hysterectomy for uterine prolapse [5].
These two methods of gynecologic surgery stayed in place for the majority of the 20th century with abdominal hysterectomy as the most favored procedure at 75% compared to vaginal hysterectomy at 25% in the early 1990’s. Vaginal surgery was limited to prolapse while fibroids, bleeding, endometriosis, malignancy, and prior surgery indicated abdominal approach.
Abdominal surgery provided access to the entire pelvis and abdomen allowing both visual and tactile sensation through a larger incision. Surgeon training at this time was preferred since it allowed teaching of anatomy and assistance by a mentor [6]. Fewer surgeons perform vaginal surgery. Vaginal surgery avoids an abdominal incision and allows direct access to repair vaginal wall defects. Vaginal surgery may have limited visualization, space for surgeon and assistant, and access if complications. Hysterectomy complication rates for abdominal procedures were 1.7 times overall, 1.9 times higher for febrile morbidity and 2.1 times higher for blood transfusion when compared to vaginal surgery [7].
Traditional guidelines for hysterectomy [7]
Abdominal
- Uterus “Too Big”
- Vagina “Too Narrow” (Arch <90deg., Bituberus diameter <8.0cm
- Uterus “Too High” (no descent)
- Intra-Abdominal issues
- -Adhesions, endo, adenexal disease, prev. pelvic surgery, CPP, prev. Cesarean
Vaginal
Less serious disease, mainly prolapse. In relation to complications form surgical approaches, abdominal surgery has the greatest complication rate with higher cost and vaginal surgery continues to have the lowest cost and complications [8].
The laparoscope
In the 1940’s Palmer (France) developed a surgical evaluation device using a camera device called endoscopy. Laparoscopy, endoscopy in the abdomen, was further developed in the 1970’s and 1980’s operative gynecology began. The laparoscope allowed visualization of the abdominal cavity through small incisions. This new approach was associated with faster recovery and fewer wound complications versus open procedures. While the laparoscopic had some advantages, it had a steep learning curve and not all gynecologic surgeons had access or training [9].
In 1988 Harry Reich performed the first hysterectomy using the assistance of the laparoscope. The laparoscope assisted the surgeon in evaluation of the abdomen and pelvis through smaller incisions and the uterus was removed through the vagina. This surgical combination was associated with less pain, less blood loss and shorter patient hospitalization and recovery. Still the laparoscope added cost and OR time, in addition to the learning curve.
Robotics
Within gynecology surgery, one of the more significant recent advances came with the FDA approval of the DaVinci robotic system in 2005. Robotic assisted surgery is still considered a laparoscopic surgical approach but adds three-dimensional camera, improved physician ergonomics, seven degree of freedom similar to a surgeon hand and provides precise, accurate instrument control. Robotics main defect in surgery is loss of haptics and increased costs [10]. A DaVinci robotic system costs approximately 1.6 million dollars plus yearly maintance and surgical instrument cost of two hundred and fifty to five hundred dollars. Robotics, however, removes many of the negative effects of laparoscopic surgery like lack of ergonomics, amplified tremor by surgeon, fulcrum, two-dimensional camera and limited range of motion of four-degrees of freedom. While proper training with robotics is necessary, the above benefits enable a decreased learning curve compared to straight-stick laparoscopy.
Robotic vs. Laparoscopic
Robotic
- FDA approved April, 2005
- Only current system
- Three components
- Surgeon console
- Insite 3D vision system
- Patient-side cart with EndoWrist Instruments
- 3D high Definition Camera
- 7 degrees of freedom similar to full ROM of surgeon’s hand
- Precise and Accurate instrument control while eliminating tremors
- Robotic system Si $1.6 million. Maintenance $100,000/yr.
- Dual console $600,000
- Instruments $2,000 each
- (10 uses=200 ea).
Laparoscopic
- 2D camera
- 4 degrees of freedom
- Fulcrum effect, non-intuitive ROM
- Tremor amplified
- Lack of ergonomics
Local research trends in gynecologic surgery
Our study shows how numbers and types of hysterectomy changed at our institution with additional data from the graduating resident physicians classes prior and 5 years following the advent of the robot surgery. Our institution is a large community-based hospital with academic affiliation to train both medical students and resident physicians. A total of 845 hysterectomies were performed in 2004. This included 475 abdominal hysterectomies (56.2), 238 total vaginal hysterectomies (28.2), and 132 laparoscopic-assisted vaginal hysterectomies (15.6). Between 2004 and 2009 the total number of hysterectomies performed increased by 20% to 1010 total (Figure 2). The largest increase in cases came from robotic-assisted hysterectomies, accounting for 383 (37.9). The number of total abdominal hysterectomies decreased to 277 (27.4). Total vaginal hysterectomies decreased to 154 (15), while LAVH cases increased to 153 (15.1). Total laparoscopic hysterectomies also increased in 2009, with 43 cases performed (4.3).
Current national (U.S.) trends (Figure 1)
- 1991 75% TAH, 25% Vaginal
- 2005 64% TAH, 21% Laparoscopic, 15% Vaginal (Jacoby et al. 2007)
- 2009 Robotic 9.5% (Manoucheri et al. 2014
- 2010 Laparoscopic 29% (Lee et al. 2014)
- Local 2009 26.3% TAH, 15.2% Vaginal, 15.1% LAVH, 37.9% Robotic, 4.3% TLH
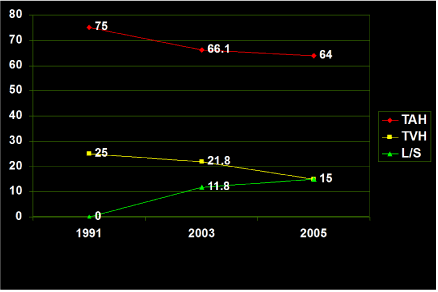
Figure 1: Hysterectomy trends United States 1991, 2003, 2005.
Advantages
- Laparotomy – Visual Depth, tactile sense, access
- Vaginal – No abdominal incision, direct access to defects, Ultimate MIS!
- Laparoscopic - visualization, small incision, shorter stay, less pain, faster recovery, less blood loss
Disadvantages
2021 Copyright OAT. All rights reserv
- Laparotomy – longer stay, more pain, longer recovery, higher morbidity
- Vaginal – less visual, tight space both team and surgeon, access if complications
- Laparoscopic – increase cost, increase learning curve, access if complications
Training surgeons
Almost immediately following introduction of robotic surgery came questions regarding its impact on resident education and training. These questions have pertained both to how best to train residents in these new technologies and if these technologies will ultimately be a detriment to resident training in traditional gynecologic surgery approaches. While minimally invasive techniques have increased now and limited abdominal approach to all-time low numbers by nearly 30% compared to early 1990’s, we must continue to train new surgeons with multiple techniques. The past mentoring of surgical education with the “See One, Do One, Teach One” methodology surgical simulation has an important function [11].
Surgical simulation
- Animate - Pig or cadaver
- Inanimate (“Dry Lab”) – skill modelsà dexterity, needle manipulation, camera and clutch control, suturing
- Computer generated systems
Currently, gynecologic surgeons are typically trained post residency using animated type labs. This training usually is approximately eight hours with a significant portion involving the animal labs. There have been residency programs that also provide training in robotic surgery, however, most of this training has been limited and involves no direct formal or simulated surgical education [12]. The Residency Training Network is an Internet based program to assist in providing a curriculum for training resident physicians [13].
When performing a hysterectomy which is the most important factor in determining route?
- Patient desires
- Diagnosis
- Uterine size
- Previous pelvic surgery
- Surgeons ability & comfort
Discussion
So what is the definitive approach to major gynecologic surgery and hysterectomy? What factors are most important to surgical approach? Which factor(s) associated with surgical choice is most important? The trend for surgery is minimally invasive approaches that focus on shorter recovery and improved patient outcomes that offset surgical costs. It has been reported that costs of surgery is lowest with vaginal hysterectomy followed by laparoscopy, abdominal and greatest cost robotic surgery. Also with regard to complications and patient benefit vaginal is again the lowest followed by laparoscopic, robotic and greatest with abdominal approach.
The American College of Obstetrics and Gynecology (ACOG) states that vaginal surgery is the approach of choice whenever feasible due to well –documented advantages and lowest complication rates [14]. The American Association of Gynecologic Laparoscopists (AAGL) states that minimally invasive techniques provide significant advantages to patients and both vaginal and laparoscopic approaches should be considered [15].
Another question still remains whether this shift in numbers negatively impacts a resident physician training. It is difficult to argue that open abdominal surgery is the necessary route for emergency cases, as well as laparoscopic or vaginal cases in which complications or unexpected findings are encountered. If residents are leaving residency with fewer laparotomies, are they less qualified to deal with emergencies or complications than gynecologists who trained before the robot [16]?
While minimally invasive techniques have provided an overall effect to decrease abdominal surgery, vaginal surgery, the recommended approach, is still performed the least. Desired metrics, decrease in cost of care and lower complications, may be limited by the increase in cost associated with laparoscopic surgery and, more so with, robotic assisted surgery. Comparison of various approaches shows vaginal surgery is more cost efficient (Figure 3). Surgical cost must be considered when multiple surgical options are available [17]. Improved surgical training in vaginal surgery to resident physicians has been advocated to achieve the desired metric outcomes.
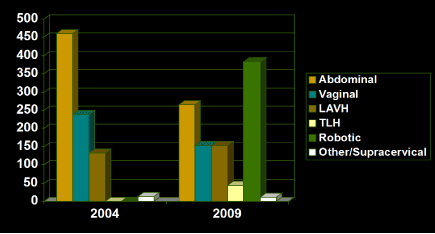
Figure 2: Local surgical approach trends 2004-2009.
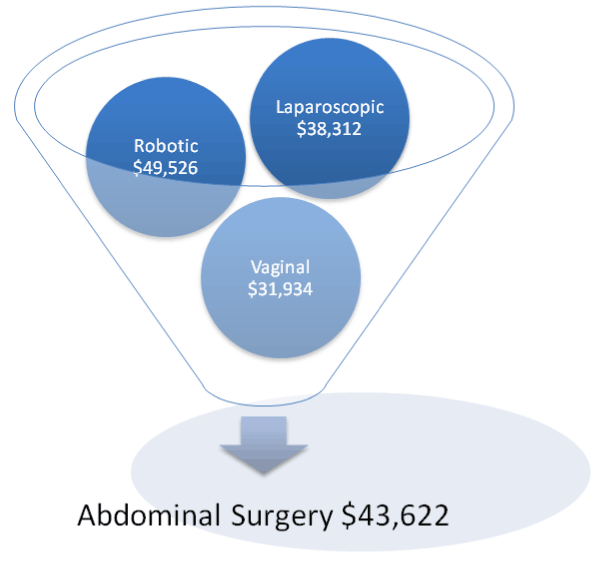
Figure 3: Cost comparison of various routes of hysterectomy [17].
References:
- Pulliam SJ, Burkewitz LR (2009) Smaller Pieces of the Hysterectomy Pie: Current Challenges in resident surgical Education. Obstet Gynecol 113 (2A1): 395-398. [Crossref]
- Wu JM, Wechter ME, Geller EJ, Nguyen TV, Visco AG (2007) Hysterectomy rates in the United States, 2003. Obstet Gynecol 110: 1091-1095. [Crossref]
- Jacoby VL, Autry A, Jacobson G, Domush R, Nakagawa S, et al. (2009) Nationwide use of laparoscopic hysterectomy compared with abdominal and vaginal approaches. Obstet Gynecol 114: 1041-1048. [Crossref]
- Sutton C (1997) Hysterectomy: a historical perspective. Baillieres Clin Obstet Gynaecol 11: 1-22. [Crossref]
- Downing KT (2012) Uterine prolapse: from antiquity to today. Obstet Gynecol Int 2012: 649459. [Crossref]
- Julian TM, Rogers RM Jr (2006) Changing the way we train gynecologic surgeons. Obstet Gynecol Clin North Am 33: 237-246, vii-viii. [Crossref]
- Kovac SR, Barhan S, Lister M, Tucker L, Bishop M, et al. (2002) Guidelines for the selection of the route of hysterectomy: application in a resident clinic population. Am J Obstet Gynecol 187: 1521-1527. [Crossref]
- Nieboer TE, Johnson N, Lethaby A, Tavender E, Curr E, et al. (2009) Surgical approach to hysterectomyfor benign gynaecological disease. Cochrane Database Syst Rev.
- Starr RA, Wagstaff NV (2006) Implementing a surgical skills training program. Obstet Gynecol Clin North Am 33: 247-258, viii. [Crossref]
- Vislo AG, Advincula AP (2008) Robotic Gynecologic Surgery. Obstet Gynecol 112: 1369.
- Walter AJ (2006) Surgical education for the twenty-first century: beyond the apprentice model. Obstet Gynecol Clin North Am 33: 233-236, vii. [Crossref]
- Galloway ML, Dhanraj D, Ventolini, G (2012) Robotic Assisted Gynecologic Surgery. J Gynecologic Surgery 28: 192-196.
- Robotic Training Network [1/12/2014]. Available from: http://www.robotictraining.org.
- [No authors listed] (2009) ACOG Committee Opinion No. 444: choosing the route of hysterectomy for benign disease. Obstet Gynecol 114: 1156-1158. [Crossref]
- AAGL Advancing Minimally Invasive Gynecology Worldwide (2011) AAGL position statement: route of hysterectomy to treat benign uterine disease. J Minim Invasive Gynecol 18: 1-3. [Crossref]
- Woodman PJ, Nager CW (2006) From the simple to the sublime: incorporating surgical models into your surgical curriculum. Obstet Gynecol Clin North Am 33: 267-281, viii. [Crossref]
- Wright KN, Jonsdottir GM, Jorgensen S, Shah N, Einarsson JI (2012) Costs and outcomes of abdominal, vaginal, laparoscopic and robotic hysterectomies. JSLS 16: 519-524. [Crossref]



