Purpose: To determine if a didactic workshop can be an effective means of increasing physical medicine and rehabilitation (PM&R) residents’ general knowledge of billing and coding as well as residents’ ability to code accurately.
Method: This is a pre-test/post-test study. Fifty-four PM&R residents ranging from post-graduate year 2 (PGY-2) to PGY-4 at three different institutions in the northeastern United States participated in an approximately 2-hour workshop focused on billing and coding. The workshop was preceded by a 20-30 minute pre-test and was followed by a 20-30 minute-long post-test. The test included 34 questions on the topics of general billing and coding knowledge, evaluation and management (E+M) coding, and basic procedural and electrodiagnostic (EDx) coding.
Results: The mean score for the pre-test was 26.2+/-11.4% and for the post-test was 55.1+/-12.6%. The mean improvement was 28.9 and was significant (p < 0.01). Test results improved to a significant degree in all question sub-types (information recall, E+M coding, and EDx coding).
Conclusions: A 2-hour didactic workshop on the basics of billing and coding increases residents’ knowledge of general billing and coding concepts as well as their ability to code accurately.
Resident education, systems-based-practice, billing, coding, rehabilitation, core competencies, PM&R, Physiatry.
The complexity of medical billing, coding, and practice management has increased dramatically over the last 25 years. In 1992, the Current Procedural Terminology (CPT) Editorial Panel defined criteria to standardize the reporting of physician-patient encounters. The first version of the “Documentation Guidelines for Evaluation and Management Services” was introduced in 1995 and revised in 1997. The ninth version of the International Classification of Diseases (ICD-9), first introduced in 1979 and comprising 13,000 codes, has now been supplanted by ICD-10 in October 2015 with approximately 68,000 codes. In 2011, the first phase of Meaningful Use was implemented, soon followed by phases 2 and 3. The Physician Quality Reporting System (PQRS) began applying negative payment systems in 2015 to those physicians and group practices that did not report data on quality measures [1]. Recognizing the importance of educating residents about the changing nature of health care delivery, in 1999 the ACGME defined six core competencies, one of which is “systems-based practice,” defined as “actions that demonstrate an awareness of and responsiveness to the larger context and system of health care and the ability to effectively call on system resources to provide care that is of optimal value ” [2].”
Despite initiatives such as the ACGME systems-based practice core competency, real world training in billing, coding, and practice management has been lacking. Williford et al. in 1999 surveyed medical school obstetrics and gynecology department executives, residents, and former residents from 171 programs. Only 9 of 171 institutions had a formal program and only 2 offered 10 or more hours of training per year. Of the residents surveyed, 68% indicated that they had "minimal" or "not at all" confidence in their ability to code accurately [3]. In 2006 Agida et al. showed that 133 second-year internal medicine residents had low levels of knowledge about Medicare [4]. A study by Fakhry et al. in 2007 found that 85% of 60 surgical residents perceived themselves as novices in billing and coding [5]. Despite this lack of knowledge, regardless of specialty, residents largely desire more training in systems-based practice [3,6].
From a practical standpoint, properly coding an encounter provides a standardized diagnosis that is linked to the charges incurred as well as a rationale for obtaining medical authorization for procedures and tests. Proper coding is needed to generate a level of service and bill. Billing is required to reimburse a physician for his or her service and provides revenue to maintain practice operations. Accurate coding and billing is not only important for generating income, it is also used for research purposes, to track disease prevalence, to track productivity, and to make staffing decisions. Over and under-billing, whether intentional or otherwise, is illegal and ignorance cannot be claimed as an excuse. Even when outside billing companies are used, the physician is ultimately responsible for any of the legal or financial ramifications of miscoding.
There have been very few studies that have examined systems-based practice knowledge in Physical Medicine & Rehabilitation (PM&R) residents. In 2009 Elwood et al. showed that residents in three large PM&R residency programs in the northeastern United States, "admit to being unaware of how to document procedural and progress notes, billing forms, and other forms integral to reimbursement effectively or how reimbursement varies in different practice settings." Despite this, residents felt that training in billing and coding was important to residents' future careers [7].
This study seeks to determine if a 2-hour didactic workshop on billing and coding can effectively teach PM&R residents the basics of outpatient billing and coding terminology while giving them the tools to effectively code outpatient E+M or procedure encounters. Secondary goals were to determine deficiencies in the areas of terminology, E+M coding, procedural coding, and to focus further didactic efforts.
A didactic workshop was performed at three large PM&R residency programs in the northeastern United States. Four workshops in total (twice at one institution) were conducted between 2013 and 2015. The workshop consisted of a 2-hour long presentation on the basics of billing and coding. The goal was to provide PM&R residents with the necessary tools to properly code an outpatient E+M or procedure-only visit. All workshops were conducted by the first author. Topics discussed included: basic definitions, coding terminology, determination of appropriate E+M levels, basic procedural coding (joint and soft tissue injections), and EDx coding. A significant portion of the workshop was dedicated to helping residents practice determining the E+M level of mock charts according to the history, physical exam, and medical decision making (MDM). The determinants of medical decision making, the 1995 and 1997 physical exam coding guidelines, and required aspects of past, family and social history (PFSH) were reviewed in-depth using a “backwards” approach. The focus was on determining the level of MDM and then working backwards to make sure the relevant physical exam and PFSH levels matched the necessary level of coding. The idea was to teach residents to tailor their documentation to meet the needs of the patient and MDM without being excessive. The authors felt this was an important concept in this era of electronic medical records, where it is easy to “over document” and dilute the medical record with information that may not have clinical or billing relevance. The seemingly ubiquitous copying forward of previous data from the medical record can lead to extraneous and erroneous information and is a potential source of fraud and abuse.
The workshop was preceded by a 34-question pre-test and was followed by an identical 34-question post-test. Approximately 20 to 30 minutes were allotted for the pre and post-tests. Whatever time was taken for the pre-test was attempted for the post-test. Three of the workshops were performed as a part of required didactic sessions and one workshop was voluntary. A total of 54 residents participated in the workshops. The project was submitted to the institutional review board (IRB) and was deemed to be exempt.
The 34-question pre and post-tests consisted of 31 short answer questions and 3 true or false questions. Questions were organized into three categories: information recall (8 questions), evaluation and management (E+M) coding (20 questions), and EDx coding (6 questions). Correct, incorrect, and answers left blank were tabulated and recorded.
A paired t-test was used to compare the pre and post-tests. On a percent basis, the mean score was 26.2+/-11.4% for the pre-test and 55.1+/-12.6% for the post-test (Figure 1). The mean improvement was 28.9% and was significant (p < 0.01). The mean score for the recall type questions was 43.8 +/- 28% on the pre-test and 79.2 +/- 19.7% on the post-test (Figure 2). The mean improvement was 35.4% and was significant (p < 0.01). The mean score for E&M coding questions was 31.76 +/- 14.7% on the pre-test and 61.9 +/- 15.6% on the post-test (Figure 3). The mean improvement was 30.2% and was significant (p < 0.01). The mean score for the EDx questions was 5.86 +/- 14.9% on the pre-test and 46 +/- 32.2% on the post-test (Figure 4). The mean improvement was 40.1% and was significant (p < 0.01).
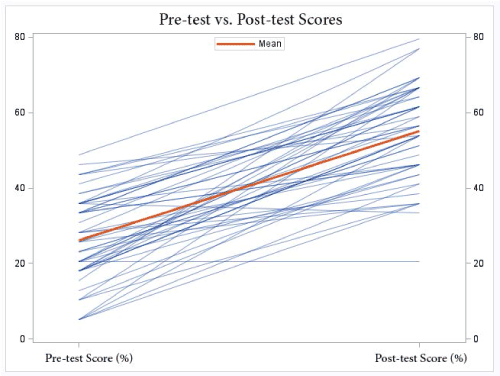
Figure 1. Pre-test vs. post-test scores (for all questions). The mean improvement was 28.9%.
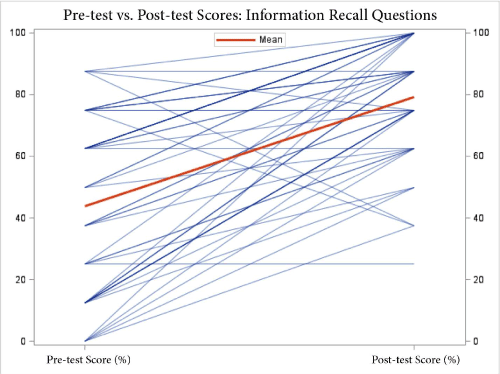
Figure 2. Pre-test vs. post-test scores for information recall type questions. The mean improvement was 35.4%.
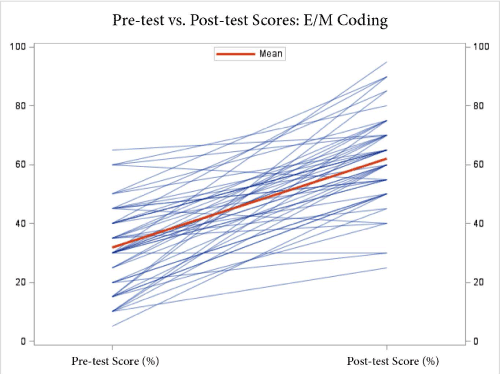
Figure 3. Pre-test vs. post-test scores for E+M coding type questions. The mean improvement was 30.2%.
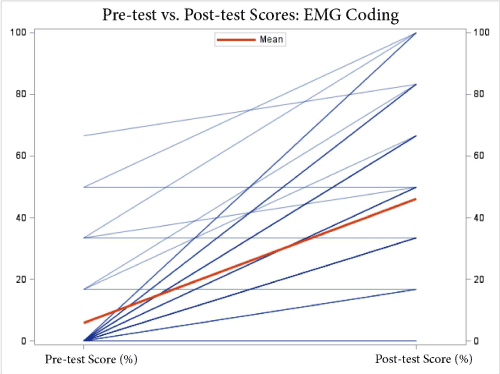
Figure 4. Pre-test vs. post-test scores for EDx coding type questions. The mean improvement was 40.1%.
While systems-based practice has been identified as an ACGME core competency, there is currently no standard method of teaching this competency. Many systems-based issues cross specialty lines, such as patient safety, inter-disciplinary teamwork, cost-effective care, and documentation accuracy. Others are specialty specific, such as documentation of specific procedures (e.g. EDx procedures) that only a few specialties perform. Research into systems-based practice has been largely confined to single specialties; however, many of the techniques investigated can be applied to resident education more broadly. Some progress has been made towards assessing residents’ mastery of systems-based practice with the institution of specialty-specific milestones in 2015. The milestones outline more concrete descriptions of deficiency and mastery; however, upon reviewing the “milestone projects” of general surgery, otolaryngology, obstetrics and gynecology, internal medicine, pediatrics, neurology, and PM&R, only PM&R includes language specifically addressing residents’ ability to code. An “aspirational” PM&R resident: “Maintains regulatory compliance, including accurate coding and billing [8].”
Methods of teaching systems-based practice are varied and range from simple to complex. Since this study was initiated, other studies have demonstrated that educational sessions improve residents’ ability to bill and code accurately [9]. Electronic, web-based, and year-long curricula have been trialed with promising results [10-12]. Some studies have taken more objective approaches such as quantifying actual lost revenue due to inaccurate resident billing [5], requiring residents to complete mock bills for outpatient clinic visits [13], and by simulating a third-party payer audit and comparing the quality of billing of actual charts before and after a series of seminars [14-17]. Some have suggested even giving residents virtual paychecks [18].
Ng and Lawless found that residents tended to underbill, leading to $43,676 in unrealized reimbursements [13]. Hirsch et al. found that an additional $34,342 was billed in a 10-month period after house staff were provided with a brief lecture and an educational sheet on billing [16]. Interestingly, Gala et al. found a significant reduction in the number of undercoded charts, but also found that billing seminars can lead to overbilling as well (this was attributed to resident overconfidence) [14]. Kikano et al. found that undercoding and overcoding occurred at a similar frequency (21% and 19% respectively) and that new patient visits were more likely to be inaccurately coded than established patient visits [19].
There is a paucity of data examining how systems-based practice is taught to PM&R residents. Elwood et al. found that residents become more involved as they progress through their training and suggested that more senior residents could be used to educate more junior residents [7]. They also found more interest in billing and coding as residents advance in their training, suggesting that teaching these concepts earlier in residency may not be as effective. It would be interesting to repeat our questionnaire after a delayed period of time, and see if there is a difference in adherence of the billing and coding concepts among the different PGY levels.
In this study, post-test scores were improved to a statistically significant degree after a 2-hour workshop. This improvement was observed with all question types (information recall, E+M coding, and EDx coding). To the knowledge of the authors, this study is the first to examine the effect of a didactic workshop on billing and coding in the PM&R resident population.
There are several limitations to our study. This survey has not been validated and was not stratified by PGY year. While we received much positive feedback after these educational workshops, there was no formal evaluation of residents’ perceived usefulness of this exercise. Some of the questions included on the pre and post-tests asked residents to evaluate charting. These were simulated charts and not actual encounters. It is possible that residents' coding accuracy would change when coding actual charts. The pre and post-tests were based on ICD-9 principles (since ICD-10 had not been implemented when our study started), but the overall concepts can be applied to ICD-10 as well. The CPT code for ultrasound guidance was modified in between administration of the workshops, changing one of the answers on the tests. This question was omitted. Due to this, we were unable to assess residents’ ability to accurately code for soft-tissue injections. In addition, the small number of questions concerning EDx coding (6) limits the ability to draw strong conclusions about the effects of this workshop on residents’ ability to accurately code EDx procedures. This study emphasized billing and coding as it pertains to outpatient encounters and is not generalizable to the inpatient setting. This was a multi-center study; however, all of the programs were in the northeastern United States, and therefore may reflect certain regional billing practices.
A 2-hour didactic workshop on billing and coding improved PM&R residents’ knowledge of billing and coding and their ability to accurately bill and code outpatient charts. Areas for future study include auditing of PM&R residents’ actual charts before and after an educational seminar to examine the trend in billing accuracy. In addition, it is thought that residents spend too much time on documentation [20]. In theory, a greater amount of billing and coding knowledge could lead to greater efficiency with documentation. This is an additional area for future examination.
The authors wish to thank Hilary Armstrong for her assistance in preparing the statistics for this article. The authors would also like to thank Franklin and Joseph Flahive for their assistance in optimizing article graphics.
1) No funding or grants or equipment were provided for the project from any source.
2) This study confers no financial benefits to the authors.
3) A very basic version of this study was presented as part of the Association of Academic Physiatrists Program for Academic Leadership. The presentation and results were not published or presented in poster form.
- Quality Measures Summary. Centers for Disease Control and Prevention website. https://www.cdc.gov/asthma/pdfs/quality_measures_summary_3_18_15.pdf. Updated March 18, 2015. Accessed September 8, 2016.
- Kavic MS (2002) Competency and the six core competencies. JSLS 6: 95-7. The Physical Medicine and Rehabilitation Milestone Project. ACGME website. https://www.acgme.org/Portals/0/PDFs/Milestones/PMRMilestones.pdf. Updated July 2015. Accessed September 8, 2016.
- Williford LE, Ling FW, Summitt RL, Stovall TG (1999) Practice management in obstetrics and gynecology residency curriculuma. Obstet Gynecol 94: 476-9. [Crossref]
- Adiga K, Buss M, Beasley BW (2006) Perceived, actual, and desired knowledge regarding Medicare billing and reimbursement. A national needs assessment survey of internal medicine residents. J Gen Intern Med 21: 466-70. [Crossref]
2021 Copyright OAT. All rights reserv
- Fakhry SM, Robinson L, Hendershot K, Reines HD (2007) Surgical residents' knowledge of documentation and coding for professional services: an opportunity for a focused educational offering. Am J Surg 194: 263-7. [Crossref]
- Andreae MC, Dunham K, Freed GL (2009) Inadequate training in billing and coding as perceived by recent pediatric graduates. Clin Pediatr (Phila) 48: 939-44. [Crossref]
- Elwood D, Kirschner JS, Moroz A, Berliner J (2009) Exploring systems-based practice in a sample of physical medicine and rehabilitation residency programs. PM R 1: 223-8. [Crossref]
- The Physical Medicine and Rehabilitation Milestone Project. ACGME website. https://www.acgme.org/Portals/0/PDFs/Milestones/PMRMilestones.pdf. Updated July 2015. Accessed September 8, 2016.
- Benke JR, Lin SY, Ishman SL (2013) Directed educational training improves coding and billing skills for residents. Int J Pediatr Otorhinolaryngol 77: 399-401. [Crossref]
- Lemen PM (2005) Development and assessment of a Web-based evaluation and management coding curriculum for residents. Am J Obstet Gynecol 193: 1785-9. [Crossref]
- Kuiken T, Prather H (1998) A computer education program to improve physician awareness of rehabilitation hospital charges. Arch Phys Med Rehabil 79: 910-4. [Crossref]
- Babitch LA (2006) Teaching practice management skills to pediatric residents. Clin Pediatr (Phila) 45: 846-9. [Crossref]
- Ng M, Lawless ST (2001) What if pediatric residents could bill for their outpatient services?. Pediatrics 108: 827-34. [Crossref]
- Gala RB, Chiang S (2012) The impact of a documentation and coding curriculum in an obstetrics and gynecology continuity clinic. Ochsner J 12: 354-8. [Crossref]
- As-sanie S, Zolnoun D, Wechter ME, Lamvu G, Tu F, et al. (2005) Teaching residents coding and documentation: effectiveness of a problem-oriented approach. Am J Obstet Gynecol 193: 1790-3. [Crossref]
- Hirsh JM, Collier DH, Boyle DJ, Gardner EM (2010) A concise evaluation and management curriculum for physicians in training improved billing at an outpatient academic rheumatology clinic. J Clin Rheumatol 16: 148-50. [Crossref]
- Kapa S, Beckman TJ, Cha SS, et al. A reliable billing method for internal medicine resident clinics: financial implications for an academic medical center. J Grad Med Educ 2: 181-7. [Crossref]
- O'Neil T, Heidelbaugh J, Riley M (2011) Resident Virtual Paychecks: A Model to Teach Proper Billing and Coding Methods. Poster presented at: the 44th Society of Teachers of Family Medicine annual spring conference; 2011 April 27-May 1; New Orleans, Louisiana.
- Kikano GE, Goodwin MA, Stange KC (2000) Evaluation and management services. A comparison of medical record documentation with actual billing in community family practice. Arch Fam Med 9: 68-71. [Crossref]
- Oxentenko AS, West CP, Popkave C, Weinberger SE, Kolars JC (2010) Time Spent on Clinical Documentation: A Survey of Internal Medicine Residents and Program Directors. Arch Intern Med 170: 377-80. [Crossref]




