Abstract
Cystic adenomyosis, a cystic lesion in the myometrium, is a rare disease that is characterized by intense dysmenorrhea. Here we report a case of a woman diagnosed with adnexa chocolate cyst that was found to be cystic adenomyosis during laparoscopic surgery. The case is of a 37-year-old woman, gravida 0 and para 0. When she was 32 years old, she visited a nearby hospital for dysmenorrhea. She was diagnosed with adnexa chocolate cyst in both sides and was followed up with oral low dose of estrogen-progestin (LEP). Five years later, she was suggested to undergo surgery because of the increasing size of the cysts. During the laparoscopic surgery, we found that the cystic lesion was not typical, and the connection with the uterus was clear. The pathological findings were consistent with the diagnosis of cystic adenomyoma. We suggest that when cystic lesions are identified with severe dysmenorrhea, the connection with the uterus and the possibility of cystic adenomyoma should be considered.
Key words
cystic adenomyosis, cystic lesions, adenomyoma, leiomyoma
Introduction
Cystic adenomyosis, a cystic lesion in the myometrium, is a rare disease characterized by intense dysmenorrhea and chronic recurrent pelvic pain. Here we report a case of a patient diagnosed with adnexa chocolate cyst before surgery, which was found to be a cystic adenomyoma during the surgery.
Case report
The case was of a 37-year-old woman, gravida 0 and para 0, with no unusual personal or family history. She underwent menarche at the age of 14, and her menstrual cycle was regular with 28-day cycle. She was experiencing progressively worsening dysmenorrhea at around the age of 20 years. When she was 32 years old, she went to a nearby hospital for dysmenorrhea. She was diagnosed with adnexa chocolate cyst in both sides, and low dose of estrogen-progestin (LEP) was prescribed. During the follow up period, she was suggested to undergo surgery because of the increasing size of the cysts.
The patient`s tumor markers CA125 and CA19-9 were 16 U/ml and 31 U/ml, respectively. A pelvis magnetic resonance imaging (MRI) was scheduled (Figure 1). Axial and sagittal images showed hemorrhagic masses on both sides of the ovaries. They were 10 × 7.5 × 8 cm in size and adhered with each other. High signal intensity on T1-weighted images and low to non-uniform signal intensity on T2-weighted images were present. The ovaries were clearly identified along with several follicles. The MRI suggested presence of endometrial cysts. However, a line-like signal-lessness area was regarded as a flow void in the cyst on the left side, which was shown to continue with the uterine bottom (Figure 1e). Therefore, cystic degeneration of leiomyoma was considered as a differential diagnosis.
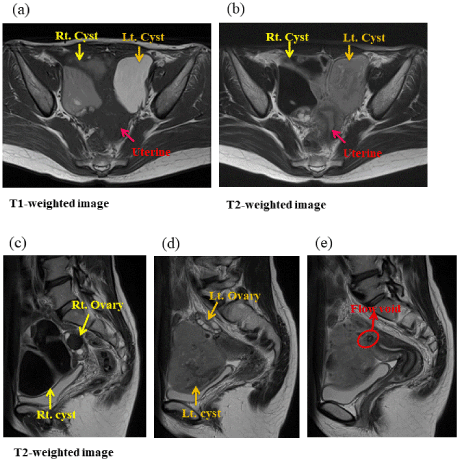
Figure 1. Pelvis magnetic resonance imaging (MRI). Axial and sagittal images showed hemorrhagic masses on both sides of the ovaries. They were 10 × 7.5 × 8 cm in size and adhered with each other. (a) T1-weighted image shows high signal intensity. (b~d) T2-weighted images present low to non-uniform signal intensity. The ovaries were clearly identified along with several follicles. (e) a line-like signal-lessness area was regarded as a flow void in the cyst on the left side.
Based on the clinical characteristics of dysmenorrhea, the patient was diagnosed with endometrial cyst of both ovaries, and laparoscopic surgery for cystic extractions was performed (Figure 2). During surgery, we found that the uterus, both sides of the ovaries, and some intestinal tract were firmly adhered (Figure 2a). Douglas' pouch was perfectly closed, and r-ASRM classification was Stage IV with 112 points. Dark-brown content flowed from the cyst when the incision reached the cystic cavity (Figure 2b). The cyst wall was thick. After the reduction of the tumor size by removal of the content, the connections of the masses with uterus were well defined (Figure 2c). Additionally, the cysts, which had no communication with the endometrial cavity, were removed. Right ovary cystectomy was performed at the same time. The surgery time was 2 hours and 40 minutes, and the patient lost 300 ml of blood.
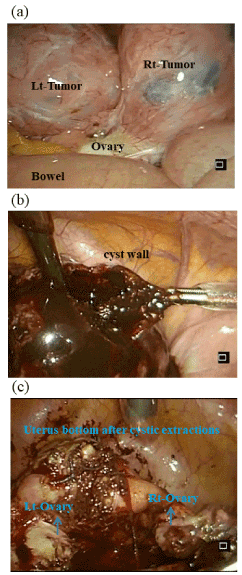
Figure 2. Intraoperative findings. (a) both sides of the ovaries, and some intestinal tract were firmly adhered. Douglas' pouch was perfectly closed, and r-ASRM classification was Stage IV with 112 points. (b) Dark-brown content flowed from the cyst when the incision reached the cystic cavity. The cyst wall was thick. (c) After the reduction of the tumor size by removal of the content, the connections of the masses with uterus were well defined.
The patient recovered well and was discharged according to the clinical pass. To prevent recurrence, oral Dienogest, a selective progesterone receptor agonist, was prescribed. Defecation pain and menstrual pain improved significantly. There was no recurrence 6 months after the surgery. Histological studies showed that endometrial glands and stroma existed in the cystic lesion and they were clearly different from the surrounding muscular layer. In the serosa layer, endometrium organization was also defined (Figure 3). Pathological findings were consistent with that of cystic adenomyoma.
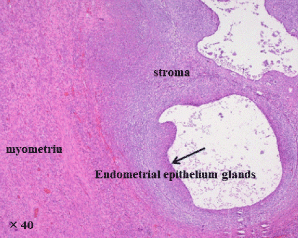
Figure 3. Pathological findings. Histological studies showed that endometrial glands and stroma existed in the cystic lesion and they were clearly different from the surrounding muscular layer. In the serosa layer, endometrium organization was also defined.
Discussion
Cystic adenomyoma is a rare disease resulting from an extensive hemorrhage within ectopic glands in the myometrium. It is characterized by well-circumscribed cavitated endometrial gland and stroma located within the myometrium. Cysts usually contain a chocolate-like fluid [1]. Depending on clinical characteristics and the age of onset, cystic adenomyoma is classified as either adult or juvenile type (Table 1). Adult cystic adenomyoma is a special type of adenomyosis and occurs among parous women older than 30 years. The cystic mass may be found in any part of the uterus, including myometrial-, mucosal-, and serosal-layers. In addition, ectopic endometrial glands also existed in the myometrium, with no clear lines between normal myometrium and cystic adenomyoma. On the other hand, the juvenile type is suggestive of a new type of Mullerian ducts anomaly, which is found in any nulliparous woman younger than 30 years. The mass is mostly located in the uterine attachment of the right round ligament of the normal uterus in the presence of adenomyosis [2,3]. Acien et al. [4]suggested that fallopian tubes and ovaries should be normal. In our case, dysmenorrhea occurred before the age of 30 years, the uterine endometrium and myometrium were normal with no other associated uterine anomalies. According to our patient’s history, images, and pathological findings, we considered that this case was a juvenile cystic adenomyoma. However, the mass was not on the uterine ligament, and the right ovary was abnormal, which was consistent with a chocolate cyst.
Cystic adenomyoma |
|
Adult |
Juvenile |
Age of onset |
Older than 30 years |
Younger than 30 yeras |
|
|
|
Delivery history |
(+) |
(-) |
Development |
A special type of adenomyosis |
Anomaly of Mullerian tube |
|
|
Parts |
In any part of the uterus, myometrial-, mucosal-, and serosal-layer. |
Most of the mass at the attachment level of the round ligament. |
|
|
Besides cystic adenomyoma, ectopic endometrial glands also exist in myometrium;
there is no clear lines between normal myometrium and cystic adenomyoma; |
|
there is no ademomyosis besides cystic adenomyoma;
with normal Fallopian tubes and ovaries;
|
Characters |
|
Content |
Chocolate-like fluid |
Pathology |
Endometrial glands and stroma exist in cystic lesion |
Table 1. Depending on clinical characteristics and the age of onset, cystic adenomyoma is classified as either adult or juvenile type.
Conclusions
We reported a case with cystic adenomyotic lesions that was treated with laparoscopic surgery. In our case, cyst adenomyoma was difficult to determine before surgery. A line-like signal-lessness area was regarded as flow void in the left side cyst, which continues with the uterine bottom was showed in MRI, and cystic degeneration of leiomyoma was considered as a differential diagnosis. Therefore, when cystic lesions are identified with severe dysmenorrhea, the connection with uterus and the presence of cystic adenomyoma should be considered and distinguished from cystic degeneration of leiomyoma.
References
- Calagna G, Cucinella G, Tonni G, Gregorio RD, Triolo O, et al. (2015) Cystic adenomyosis spreading into subserosal-peduncolated myoma:How to explan it. Int J Surg Case Rep 8: 29-31. [Crossref]
- Acien P, Asien M, Fernandez F, Mayol MJ, Aranda I (2010) The cavitated accessory uterine mass: a mullerian anormaly in women with an otherwise normal uterus. Obstet Gynecol 117: 1101-1109. [Crossref]
- Demir H, Scoccia B (2010) Diagnosis, laparoscopic management, and histopathologic findings of Juvenile cystic adenomyoma: a review of nine cases. Fertil Steril 94: 862-868. [Crossref]
- Acien P, Bataller A, Fernandez F, Acien MI, Rodriguez JM, et al. (2012) New cases of accessory and cavitated uterine masses (ACUM): a significant cause of severe dysmenorrhea and recurrent pelvic pain in young womem. Hum Reprod 27: 683-694. [Crossref]



