As adults with cerebral palsy (CP) age, they are likely to be susceptible to lung infections and reflux illness, resulting in poor respiration and deterioration in walking distance and speed. The purpose of this pilot study was to test the short-term effectiveness of increasing the lung function of adults with CP by the introduction of a wind musical instrument. Eight adults with CP were given a Kazoo, a low cost portable musical instrument to participated in a one hour daily musical session for two weeks. Their lung function measures of peak expiratory flow rate were measured before and after the intervention. Results revealed a 50.42% increase in lung function which was also significant (t = 2.430, p = 0.045) over a short interventional period. This is the first study to evaluate using a musical instrument to improve lung function of adults with cerebral palsy. A follow-up large study is recommended.
adults with cerebral palsy, lung function, musical instrument
Cerebral palsy (CP) is a non-progressive permanent brain disorder which occurs at birth. and lead to disturbances of sensation, perception, cognition, communication, behavior, and musculoskeletal problem [1]. Children with CP also have poor chest mobility, trunk extensibility, and weak respiratory muscle strength [2]. Due to these physiological changes, they are at risk of reduction in lung volume and lung diseases such as pneumonia, atelectasis, bronchiectasis and chronic obstructive lung diseases.
One way to improve lung function is for children with CP to participate in Respiratory Muscle Training (RMT) using an incentive spirometer [2]. RMT reported improved respiratory muscle strength, increased trunk control and functional exercise capacity, enhanced participation in daily living activities, and improvement in the quality of life among children with CP [3]. However, a recent Cochrane Review of six randomized control trials comprising 195 multiple sclerosis participants found RMT had no significant effects to improve respiratory function [4].
Playing a wind instrument can be joyful, socially accepted while mimic inspiration and expiration to achieve deeper breathing, aid in excreting mucus, and higher lung function parameters [5-7]. A study of wind musical instrument players found they had higher lung function compared to health non-players [8]. Kazoo, a lightweight and low-cost acoustic instrument requires one to inhale deeply and exhale to produce sound. Using the Kazoo produced positive change in lung function when tested with individuals with Chronic Obstructive Pulmonary Disease (FEV1 and FVC score increased by 0.09 to 0.1 scores and FEV1% increased by 3.1.%) [9].
Studies to identify the major motor disorder of children with CP moving through adolescence and young adulthood has been sparse and not well understood [10]. What is known is low respiratory muscle strength in children with CP implies decreased capability levels of daily living self-care and social function [11]. The interest in adults with CP is because with increasing age they may be susceptible to lung infections and reflux illness, resulting in poor respiration and deterioration in walking distance and speed [3,12]. Furthermore, many adults with CP do social enterprise work activities to fulfil their desire for self-development, self-esteem and provide an avenue for them to reach out socially to the public. However, a Japanese study of 686 adults with CP working work at sheltered workshops found functional among 35% of them had motor deterioration over 5 years [13]. This was probably due to them sitting down for long period of time while at the sheltered workshops.
The purpose of this pilot study was to test the short-term effectiveness of increasing the lung function of adults with CP when they were introduction of a wind musical instrument.
Subjects
Eight adults with CP (5 males and 3 females) age above 18 years old (18-55 years of age) were recruited from the Cerebral Palsy Association of Singapore (CPAS). All participants attend CPAS Goodwill, Rehabilitation and Occupational Workshop daily from 9am to 4 pm. They had Gross Motor Functional Classification System (GMFCS) of level 2 to 4. All participants were keen to learn to use a Kazoo to improve lung function. They also had good understand and follow instruction for pulmonary function measurement (Table 1). Verbal and written consent was obtained from the participating adults with CP.
Table 1. Particulars of adults with CP participants
Coded names |
Race |
Sex |
GMFCS score |
| CTM |
Chinese |
F |
2 |
| DBMS |
Malay |
M |
2 |
| EN |
Chinese |
M |
3 |
| ECMT |
Chinese |
M |
2 |
| LCY |
Chinese |
F |
3 |
| LZD |
Chinese |
M |
2 |
| MHK |
Chinese |
F |
2 |
| OZRD |
Chinese |
M |
2 |
Experimental procedure
Experimental quantitative design was adopted for the pilot study. This convenience sample study introduced participants to Kazoo to play a variety of musical songs for two weeks (Figure 1). Participants were required to inhale deeply and exhale to produce sound from the Kazoo.

Figure 1. Kazoo, a lightweight and low-cost acoustic instrument.
The instrument used to measure the lung capacity was a portable Mini-Wright Peak Flow meter, which measures peak expiratory flow rate (PEF). It was found to be highly repeatable at a 95% confidence limit, on average across the range of flows, ±8.5 1iters/min [14]. Participants PEF was measurement before the introduction of Kazoo and measured again after 2 weeks of daily one hour of practice sessions. They were also encouraged to practice the Kazoo more frequently at home over the 2 weeks period to exercise their respiratory muscles to increase their lung function and improve their awareness of the breathing pattern (Figure 2).
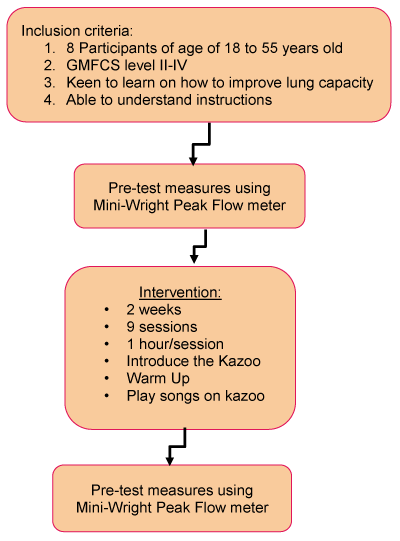
Figure 2. Consort flow chart of methodology.
The above protocol was approved by the Research and Projects Committee of School of Health Sciences, Nanyang Polytechnic, Singapore as ethically sound and safe to conduct.
Statistical analysis
Differences of pre and post PEF rate was determined by the parametric T-tests. All statistical tests were performed using the Student Version of SPSS 20.0 for Windows, with the level of significance set at p < 0.05.
Mean pre-PEF rate was 240 liters/min while post-PEF rate was 362.6 liters/mins. There was an increase of 50.75% of lung function achieved over the 2 weeks period of 9 interventions of 1 hour each (Figure 3). T-test revealed statically significance (t = 2.430 at p = 0.045).
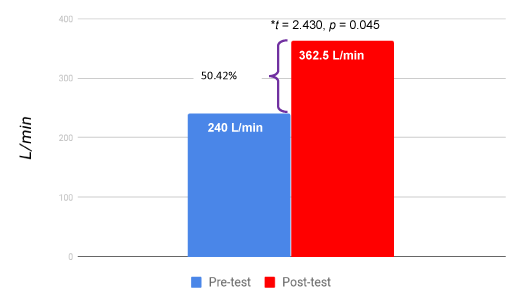
Figure 3. Mean pre and post-Test test values.
This pilot study found that introducing Kazoo, an acoustic instrument to adults with CP improved their ability to inhale deeply and exhale to produce an increase sound by using 50.42% more expiratory flow rate. This improvement was achieved over 2 weeks of 9 face-to-face sessions only. The results were also statistically significant.
To the best of the authors’ knowledge, this is the first study to evaluate the effectiveness of using low cost portable musical instruments to improve the lung function of adults with CP. Wade introduced Kazoo to patients with Chronic Obstructive Pulmonary Function (COPD) for 5 minutes sessions and also found positive improvements [9].
Our results concur with Wade results but on different population of diseases. Cumulatively both studies support the use of Kazoo as a simple and portable device that improved lung function of adults with CP who have good oral motor skills. The introduction of a musical instrument to therapy sessions can create greater compliance by clients to regular lung functional exercises therapy.
We could have use more details lung function instrument to measure both inspiration and expiration factors. We recommend using Spirometry for future studies.
Future studies should also evaluate lower limb function and specifically walking distance and speed and correlated with improvement in lung function of this targeted population. A strong correlation between walking ability and lung function has been reported in the past.
Healthcare professional should explore introducing simple musical devices to adults with CP for them to use regularly to maintain their functional ability. Large scale studies should be conducted on adults with CP to better understand how we can improve the lives of this population as they move through adult to middle and older age.
- Anonymous (2007) The definition and classification of cerebral palsy. Dev Med Child Neurol 49: 1–44. [Crossref]
- Seddon PC, Khan Y (2003) Respiratory problems in children with neurological impairment. Arch Dis Child 88: 75-78. [Crossref]
- Keles MN, Elbasan B, Apaydin U, Aribas Z, Bakirtas A, et al. (2018) Effects of inspiratory muscle training in children with cerebral palsy: a randomized controlled trial. Braz J Phys Ther [In Press]. [Crossref]
- Rietberg MB, Veerbeek JM, Gosselink R, Kwakkel G, van Wegen EEH (2017) Respiratory muscle training for multiple sclerosis (Review). Cochrane Database Syst Rev 12: CD009424. [Crossref]
- Low V (2015) Bottom line health. Play the harmonica to strength your lungs. https://bottomlineinc.com/health/respiratory/play-the-harmonica-to-strengthen-your-lungs.
- Dhule SS, Sunita BN, Gawali SR (2013) Pulmonary function tests in wind instrument player. International Journal of Science and Research 2: 384-386.
- Zuskin E, Mustajbegovic J, Schachter EN, Kern J, Vitale K, et al. (2009) Respiratory function in wind instrument players. Med Lav 100: 133-1341. [Crossref]
- Wade LM (2017) A pilot study of pursed lip breathing, singing and kazoo playing on lung function and perceived exertion of participants who smoked. Thesis for Doctor of Philosophy (Music Therapy) .
- Haak P, Lenski M, Hidecker MJC, Li M, Paneth N (2009) Cerebral palsy and aging. Dev Med Child Neurol 51: 16–23.
- Wang HY, Chen CC, Hsiao SF (2012) Relationships between respiratory muscle strength and daily living function in children with cerebral palsy. Res Dev Disabil 33: 1176-1182. [Crossref]
- Lampe R, Blumenstein T, Turova V, Alves-Pinto A (2014) Lung vital capacity and oxygen saturation in adults with cerebral palsy. Patient Prefer Adherence 8: 1691-1697. [Crossref]
- Ando N, Ueda S (2000) Functional deterioration in adults with cerebral palsy. Clin Rehabil 14: 300–306. [Crossref]
- Miller MR, Dickinson SA, Hitchings DJ (1992) The accuracy of portable peak flow meters. Thorax 47: 904-909.



