Abstract
Historical Vignette: Traumatic diaphragmatic hernia apparently was described by Sennertus, who in 1541 reported an instance of delayed herniation of viscera through an injured diaphragm [1]. The first two deaths were described by Ambrose Paré in 1578, one from strangulated bowel [2]. Ambroise Paré, in 1579, described the first case of diaphragmatic rupture diagnosed at autopsy. The patient was a French artillery captain who initially survived a gunshot wound of the abdomen, but died 8 months later of a strangulated gangrenous colon, herniating through a small diaphragmatic defect that would admit only the tip of the small finger. It was not until 1853 that ante mortem diagnosis of traumatic rupture of diaphragm was made by Bowditch. The first successful diaphragmatic repair was reported by Riolfi in 1886 in a patient with omental prolapse, and Naumann in 1888 repaired the defect with herniated stomach. The largest and the most comprehensive collective review was published by Hood in 1971, whereas the earliest review on this subject was by Carter andassociates in 1951 [3].
Key words
diaphragmatic injury, tear, intrathoracic pressure, intra-abdominal, diaphragm, musculotendinous
Introduction
Diaphragmatic rupture (also called diaphragmatic injury or tear). The diaphragm is the major muscle of respiration. Diaphragmatic excursion and chest wall expansion increase the negative intrathoracic pressure required for inhalation. The sequelae from diaphragmatic rupture and subsequent herniation of intra-abdominal contents are associated with significant morbility and mortality.
Anatomy
The diaphragm is a dome shaped, musculotendinous structure located at the bottom of the pleural cavity and at the top of the abdominal cavity. It consists of a central tendon, with right and left leaflets composed of striated muscles (Figure 1). Three large openings disrupt the continuity of the diaphragm: the aortic, esophageal, and inferior vena caval apertures. The diaphragm is covered by parietal pleura and peritoneum except for the bare area of the liver. Anatomically, the diaphragm is composed of two parts: the lumbar diaphragm and costal diaphragm [4].
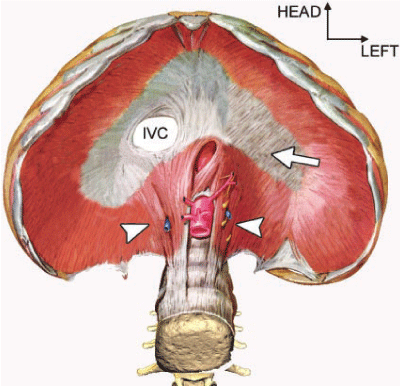
Figure 1. Central tendon (arrow), Crura (arrow heads)
Diaphragmatic hernias can be divided into two categories: congenital defects and acquired defects. Congenital diaphragmatic hernias (CDH) occur because of embryologic defects in the diaphragm. Most patients with CDH present early rather than late in life; however, a subset of adults may present with a congenital hernia that was undetected during childhood. Acquired diaphragmatic hernias stem from all types of trauma, with blunt forces accounting for the majority. Diaphragmatic hernias require a high level of suspicion to detect. Patients can be asymptomatic in up to 53% of hernias from blunt trauma and 44% from penetrating trauma. Routine chest x-ray detects only 33% of hernias when interpreted by the trauma team leader at initial evaluation. Missed injuries are associated with significant morbidity and mortality [5]. Traumatic rupture of the diaphragm is an uncommon condition. It occurs in 0.8 to 5% of patients admitted to hospital with thoracoabdominal trauma. The etiologic factors are blunt trauma (for example, in motor vehicle accidents) and penetrating trauma [6].
Spontaneous acquired diaphragmatic hernia without any apparent history of trauma is a very rare condition and is very difficult to diagnose (Figure 2). Diaphragmatic injuries are quite uncommon and often result from either blunt or penetrating trauma. Diaphragmatic rupture is a life-threatening condition. Diaphragmatic ruptures are usually associated with abdominal trauma however, it can occur in isolation. The organs most commonly involved in right-sided diaphragmatic hernias are the colon, omentum, small intestines and liver. Chest radiography and computerized tomography is the most effective method for diagnosis of traumatic diaphragmatic rupture [7]. Treatment is surgical, with reduction of the viscera and simple repair of the diaphragm with non-absorbable suture.
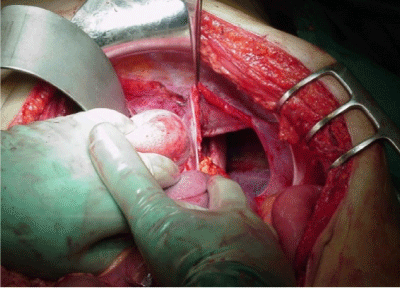
Figure 2. Traumatic Diaphragmatic Rupture
Pathophysiology
A sudden increase in the pressure gradient between the pleural and peritoneal cavities that occurs with high-speed blunt trauma will lead to disruptions of the diaphragm. This same pleuroperitoneal pressure gradient will also promote migration of intraperitoneal structures into the pleural space after disruption has occurred. Once the viscera have been displaced into the pleural space, both cardiovascular and respiratory functions are compromised [8] (Figure 3). The pathophysiologic effects of ruptured/ acquired diaphragm are on circulation and respiration. This is due to the impaired function of the diaphragm, compression of the lungs, and displacement of the mediastinum with impairment of the venous return to the heart. In cases of pericardial tear, the heart is compressed by the herniating viscera, and a clinical picture of cardiac tamponade may follow. Diaphragmatic action accounts for two thirds of the tidal volume when supine. Functional loss of one hemi-diaphragm results in 25% to 50% decrease in pulmonary function [9]. Smaller diaphragmatic hernias are often not found until months or years later when patients present with strangulation or dyspnea.
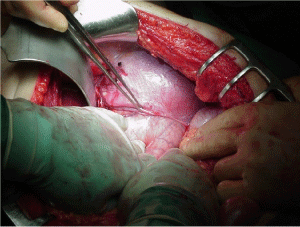
Figure 3. Disruptions of the diaphragm.
Clinical Presentation: Clinical findings include (1) marked respiratory distress, (2) decreased breath sounds on the affected side, (3) palpation of abdominal contents upon insertion of a chest tube, (4) auscultation of bowel sounds in the chest, (5) paradoxical movement of the abdomen with breathing, and/or (6) diffuse abdominal pain. Acute traumatic rupture of the diaphragm may go unnoticed and there is often a delay between the injury and the diagnosis. A comprehensive literature search was performed using the terms "delayed presentation of post traumatic diaphragmatic rupture" and "delayed diaphragmatic rupture". The diagnostic and management challenges encountered are discussed, together with strategies for dealing with them.
Review of Literature
A Pubmed search was conducted using the terms of post traumatic diaphragmatic rupture. Although quite a few articles were cited, the details of presentation, investigations and treatment discussed in each of these were not identical.
Mechanism of injury
These patients usually have multi system injuries because of the large force required to rupture the diaphragm [10]. Diaphragmatic injury is a recognised consequence of high velocity blunt and penetrating trauma to the abdomen and chest rather than from a trivial fall [11]. Traumatic diaphragmatic injuries occur in 0.8%–8% of patients who sustain blunt trauma. Up to 90% of diaphragmatic ruptures from blunt trauma occur in young men after motor vehicle accidents [12,13]. Injuries to the left hemidiaphragm occur three times more frequently than injuries to the right side following blunt trauma, possibly due to a buffering effect of the liver on the right hemidiaphragm [14]. However, the relative paucity of right-sided injuries may also have been associated with underdiagnosis [15]. Both bilateral tears and extension of tears into the central tendon are uncommon. They are reported in 2%–6% of patients with diaphragmatic injury [16]. Mechanisms of injuries include a lateral impact, which distorts the chest wall and shears the diaphragm, and a direct frontal impact, which leads to increased intraabdominal pressure [15]. Further ruptures of the diaphragm can occur in its central portion and at the costal attachment spreading in a transverse direction. Peripheral detachment is the least frequent type of rupture observed at surgery [17]. Penetrating injuries such as gunshot wounds or stab injuries are more random (2:1 ratio of penetrating vs blunt trauma) and produce small diaphragmatic holes (usually _1 cm in diameter), which are often overlooked [18].
Complications
A significant complication of diaphragmatic rupture is traumatic diaphragmatic herniation: organs such as the stomach that herniate into the chest cavity and may be strangulated, losing their blood supply. Herniation of abdominal organs is present in 3–4% of people with abdominal trauma who present to a trauma center.
Site of rupture
Between 50 and 80% of diaphragmatic ruptures occur on the left side. It is possible that the liver, which is situated in the right upper quadrant of the abdomen, cushions the diaphragm (Figure 4). However, injuries occurring on the left side are also easier to detect in X-ray films. Half of diaphragmatic ruptures that occur on the right side are associated with liver injury. Injuries occurring on the right side are associated with a higher rate of death and more numerous and serious accompanying injuries [19]. Bilateral diaphragmatic rupture, which occurs in 1–2% of ruptures, is associated with a much higher death rate (mortality) than injury that occurs on just one side.
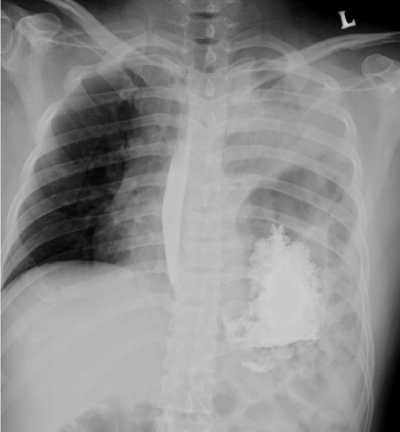
Figure 4. Site of rupture.
Diagnosis
Initially, diagnosis can be difficult, especially when other severe injuries are present; thus the condition is commonly diagnosed late. Chest X-ray is known to be unreliable in diagnosing diaphragmatic rupture; it has low sensitivity and specificity for the injury. Often another injury such as pulmonary contusion masks the injury on the X-ray film. Half the time, initial X-rays are normal; in most of those that are not, hemothorax or pneumothorax is present. However, there are signs detectable on X-ray films that indicate the injury. On an X-ray, the diaphragm may appear higher than normal. Gas bubbles may appear in the chest, and the mediastinum may appear shifted to the side [20]. A nasogastric tube from the stomach may appear on the film in the chest cavity; this sign is pathognomonic for diaphragmatic rupture, but it is rare. A contrast medium that shows up on X-ray can be inserted through the nasogastric tube to make a diagnosis. The X-ray is better able to detect the injury when taken from the back with the patient upright, but this is not usually possible because the patient is usually not stable enough; thus it is usually taken from the front with the patient lying supine. Positive pressure ventilation helps keep the abdominal organs from herniating into the chest cavity, but this also can prevent the injury from being discovered on an X-ray [20]. Over the past decade, conventional CT has benefited from two major advances: the introduction of helical CT in the early 1990s and the introduction of multi–detector row CT in 1998. Despite these advances, CT findings remain unchanged. Nevertheless, detection of diaphragmatic injuries has improved with helical CT and should further improve with multisection CT. Two major factors are mainly responsible for this improvement [21]. MR imaging with breath-hold acquisition permits good visualization of diaphragmatic abnormalities, but this technique cannot be performed in emergency situations [21].
Pitfalls of CT
2021 Copyright OAT. All rights reserv
False-Positive Findings: A diaphragmatic defect is not specific for a rupture. Posterolateral defects, which are detected at CT in approximately 6% of asymptomatic adults, may mimic diaphragmatic tears [4]. These defects occur more commonly on the left side and are thought to represent congenital asymptomatic Bochdalek hernias. Acquired diaphragmatic defects are seen more commonly in women, in patients with emphysema, and with increasing age. Some reports have supported the role of video assisted thoracoscopic surgery (VATS) in the management of diaphragmatic injury, with a sensitivity and specificity of 100% being quoted [22] (Figure 5).
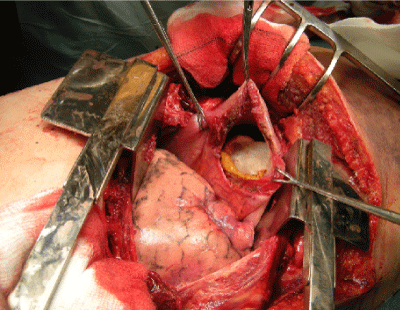
Figure 5. Videoassisted thoracoscopic surgery (VATS).
Repair of diaphragmatic rupture: Treatment of rupture is surgery. Generally the diaphragm is repaired by the transabdominal approach while complicated ruptures can be assessed with a lower thoracic incision [23]. Surgical exploration, however, is mandatory wherever diaphragmatic injury is suspected. Direct suture is effective in preventing future specific complications [24] (Figure 6).
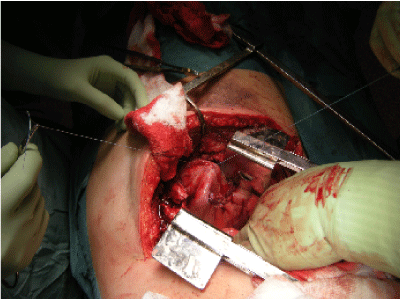
Figure 6. Surgical exploration.
Prognosis: In most cases, isolated diaphragmatic rupture is associated with good outcome if it is surgically repaired. The death rate (mortality) for diaphragmatic rupture after blunt and penetrating trauma is estimated to be 15–40% and 10–30% respectively, but other injuries play a large role in determining outcome [25]. Early deaths usually are a result of associated injuries not the diaphragmatic tear. Mortality rate ranges from 5-30%. Serious morbidity usually is related to re-expansion pulmonary edema or to the thoracotomy or laparotomy.
Competing Interest
A knowledge of diaphragmatic hernia is essential for both the physician and the surgeon in atypical abdominal and respiratory discomfort, especially when there is history of trauma. Paralysis or incoordination of the diaphragm is common, but more than 50% of these conditions resolve. The late complications of an undiagnosed traumatic hernia include all of the following: bowel herniation, incarceration, and strangulation; tension hemothorax secondary to massive bowel herniation; pericardial tamponade from herniation into the pericardial sac; and diaphragmatic paralysis that may recover after repair. Death and significant morbidity rarely are related to delayed diagnosis is however, incarceration of herniated abdominal contents can lead to infarction or rupture with disastrous consequences. The traumatic lesions of diaphragm are generally expressions of particularly severe trauma whose outcome is influenced by the associated organ injuries. High index of suspicion is required for diagnosis of diaphragmatic lesions. Preoperative diagnosis relies on the visceral dislocation both clinically and radiologically. In addition, the features highlighted above on chest skiagram and CT scan could add to confirm and support the diagnosis. To avoid missed injury thorough inspection of both hemidiaphragms should be done routinely on every trauma patient undergoing laparotomy [26].
References
- Shah R, Sabanathan S, Mearns AJ, Choudhury AK (1995) Traumatic rupture of diaphragm. Ann Thorac Surg 60: 1444-1449. [Crossref]
- Blaivas M, Brannam L, Hawkins M, Lyon M, Sriram K (2004) Bedside emergency ultrasonographic diagnosis of diaphragmatic rupture in blunt abdominal trauma. Am J Emerg Med Nov 22(7):601-4.
- Carter BN, Giuseffi J, Felson B (1951) Traumatic diaphragmatic hernia. Am J Roentgenol Radium Ther 65: 56-72. [Crossref]
- Caskey CI, Zerhouni EA, Fishman EK, Rahmouni AD (1989) Aging of the diaphragm: a CT study. Radiology 171: 385-389. [Crossref]
- Hanna WC, Ferri LE, Fata P, Razek T, Mulder DS (2008) The current status of traumatic diaphragmatic injury: lessons learned from 105 patients over 13 years. Ann Thorac Surg Mar 85(3):1044-1048.
- Rajesh S, Sabaratnam S, Alan JM, Amit KC (1995) Traumatic rupture of diaphragm. Ann Thorac Surg 60:1444-9.
- Athanassiadi K, Kalavrouziotis G, Athanassiou M, Vernikos P, Skrekas G, et al. (1999) Blunt diaphragmatic rupture. Eur J Cardiothorac Surg 15: 469-474. [Crossref]
- Karmy-Jones R, Jurkovich GJ (2004) "Blunt chest trauma". Current Problems in Surgery 41 (3): 211–380. doi:10.1016/j.cpsurg.2003.12.004. PMID 15097979.
- Rekha A, Vikram A (2010) Traumatic Diaphragmatic Hernia. Sri Ramachandra Journal of Medicine 3:2; 23-25.
- Meyers BF, McCabe CJ (1993) Traumatic diaphragmatic hernia. Occult marker of serious injury. Ann Surg 218:783-790. [Crossref]
- Goh BK, Wong AS, Tay KH, Hoe MN (2004) Delayed presentation of a patient with a ruptured diaphragm complicated by gastric incarceration and perforation after apparently minor blunt trauma. Canadian Journal of Emergency Medicine 6:277-280.
- Bergin D, Ennis R, Keogh C, Fenlon HM, Murray JG (2001) The "dependent viscera" sign in CT diagnosis of blunt traumatic diaphragmatic rupture. AJR Am J Roentgenol 177: 1137-1140. [Crossref]
- Van Hise ML, Primack SL, Israel RS, Müller NL (1998) CT in blunt chest trauma: indications and limitations. Radiographics 18: 1071-1084. [Crossref]
- Boulanger BR, Milzman DP, Rosati C, Rodriguez A (1993) A comparison of right and left blunt traumatic diaphragmatic rupture. J Trauma 35: 255-260. [Crossref]
- Killeen KL, Mirvis SE, Shanmuganathan K (1999) Helical CT of diaphragmatic rupture caused by blunt trauma. AJR Am J Roentgenol 173: 1611-1616. [Crossref]
- Shanmuganathan K, Killeen K, Mirvis SE, White CS (2000) Imaging of diaphragmatic injuries. J Thorac Imaging 15: 104-111. [Crossref]
- Schumpelick V, Steinau G, Schlüper I, Prescher A (2000) Surgical embryology and anatomy of the diaphragm with surgical applications. Surg Clin North Am 80: 213-239, xi. [Crossref]
- Shackleton KL, Stewart ET, Taylor AJ (1998) Traumatic diaphragmatic injuries: spectrum of radiographic findings. Radio Graphics 18:49-59.
- Hariharan D, Singhal R, Kinra S, Chilton A (2006) Post traumatic intra thoracic spleen presenting with upper GI bleed!--a case report. BMC Gastroenterol 6: 38. [Crossref]
- Sliker CW (2006) Imaging of diaphragm injuries. Radiol Clin North Am 44: 199-211, vii. [Crossref]
- Iochum S, Ludig T, Walter F, Sebbag H, Grosdidier G, et al. (2002) MD Imaging of Diaphragmatic Injury: A Diagnostic Challenge? Mediastinum, chest wall, and diaphragm. Radio Graphics 22: S103-106.
- Mintz Y, Easter DW, Izhar U, Edden Y, Talamini MA, et al. (2007) Minimally invasive procedures for diagnosis of traumatic right diaphragmatic tears: a method for correct diagnosis in selected patients. Am Surg 73: 388-92. [Crossref]
- Karamercan A, Kurukahvecioglu O, Imren Y, Yilmaz TU, Sare M, et al. (2006) Diagnosis and Surgical Treatment of Diaphragmatic Rupture Following Blunt Abdominal Traumas. Surgery Journal 35-38.
- Chandra A, Samantaray A, Balasubramani G, Sonawane R (2006) Surgical management of diaphragmatic injuries. IJTCVS 23; 22-207.
- Khan MA, Bilal A, Aslam V, Billah M, Hadi A, et al. (2008) Muslim. Management of traumatic diaphragmatic hernias. JPMI 22:4; 281-284.
- Matsevych OY (2008) Blunt diaphragmatic rupture: four year's experience. Hernia 12(1):73-8. Epub 2007 Sep 22.
- Lee JKT, Sagel SS, Stanley RJ (1989) Computed body tomography. New York, NY: Raven 473-502.
- Rashid F, Chakrabarty MM, Singh R, Iftikhar SY (2009) A review on delayed presentation of diaphragmatic rupture. World J Emerg Surg 4: 32. [Crossref]






