Plantar fasciopathy (PF) is a common pathology with an incidence of 10% in adults [1,2]. With a 7.9% incidence in runners, PF is the third most common overuse running injury with an estimated financial burden of $376 million per year in the United States of America [3,4]. Despite a wealth of research PF is still considered a difficult condition to treat.
Currently, it is not clear which intervention, physiotherapy, podiatry, pharmacological treatment, or surgery best stimulate a healing response. While there is no consensus among orthopaedic clinicians regarding the best treatment for PF, many authors recommend exhausting conventional treatment options typical of Physiotherapy and Podiatry (exercise, orthotics, manual therapy, tape, acupuncture, night splints) before proceeding to extracorporeal shockwave therapy (ESWT), injection therapy or surgery [5]. The advantages of a conventional approach include lower associated costs and less risk of complications such as infection, rupture, fat pad atrophy, osteomyelitis or nerve damage when compared to injection or surgery [6,7].
Symptoms of PF are plantar heel pain on first steps after waking, pain on sustained loading and pain on palpation of the medial calcaneal tubercle [8]. Historically, this condition has been referred to as plantar fasciitis which would suggest an inflammatory pathology. This may be inappropriate as the underlying pathophysiology of this condition is not fully understood. Structural changes consistent with degeneration [9], associated plantar intrinsic muscle atrophy [10,11], softening of the plantar fascia [12], hypertonic muscle patterns [13] and a failed healing response have been reported rather than inflammation. The term plantar fasciopathy is therefore more reflective of this condition.
A number of narrative and systematic reviews have been conducted regarding conventional treatments for PF. A search of MEDLINE, AMED, EMBASE, Cochrane and PEDro databases between 2007 and September 2017 identified six systematic reviews of conservative treatments for plantar fasciopathy. These included tape [14, 15], stretching [16], acupuncture [17] and orthotics [18]. One review considered a limited range of modalities [19]. To the authors’ knowledge no review has exclusively looked at high quality evidence (randomised controlled trials) of conservative treatments alone. As PF is considered difficult to treat, interventions that are considered in the normal scope of Physiotherapy and Podiatry are usually recommended as the first line of management, the aim of this systematic review was to evaluate the efficacy of these treatments.
Data source
The electronic databases of MEDLINE, EMBASE, Cochrane and PEDro were searched. The keywords used for the search are presented in Table I. The inclusion and exclusion criteria for the review are listed in table 2. The period for the review was from the beginning of the databases until March 2018.
Table 1. Keywords used in the search, “$” indicating a truncated search term.
1 |
plantar fasciitis OR plantar fasciosis OR plantar fasciopathy OR heel pain |
2 |
Tap$ OR electro$ OR la$er OR LLLT OR cryo$ OR heat OR stretch$ OR physiotherap$ OR exercise$ OR physical therap$ OR podiatr$ OR ultrasound OR orthotic$ OR insole$ OR night splint$ OR acupuncture |
3 |
Exploded terms: plantar fasciitis, physical therapy modalities, exercise therapy, orthotic devices, acupuncture |
|
1 AND (2 OR 3) |
Table 2. Eligibility criteria.
Inclusion |
Exclusion |
Randomised Controlled Trials |
Aged under 18 years old |
English Language |
Use of injection therapies |
Treatments considered by author consensus to be within the normal scope of practice for Physiotherapists or Podiatrists |
Use of ESWT |
Chronic PF (duration of symptoms over 3 months)
(if this was not explicitly stated studies were included) |
Use of invasive techniques |
Human subjects |
Pilot studies |
Study identification
Two reviewers (AL and AMH) independently reviewed all titles and abstracts that were identified against the eligibility criteria. Full-text manuscripts were requested when eligibility could not be assessed from the abstract and title.
Data extraction
The reviewer (AL) performed data extraction for each eligible paper. Data extraction included population characteristics (sample size, mean age, gender, and duration of symptoms), clinical diagnostic criteria, investigations, treatment interventions, outcomes, results, follow-up period, country of study and athletic population (involvement in sport) (table 3).
Table 3. Data extraction included population characteristics (sample size, mean age, gender, and duration of symptoms), clinical diagnostic criteria, investigations, treatment interventions, outcomes, results, follow-up period, country of study and athletic population (involvement in sport).
Author year |
Modality |
Country of study |
Mean age, SD, range |
No. subjects, No. fascias |
Gender male / female |
Population sporting / sedentary |
Minimum symptom duration / mean |
Diagnosis Radiological or clinical |
Outcome Measures |
Treatments |
Main between groups result |
Follow-up |
PEDro score /10 |
(months) |
(months) |
(* If calculated by authors) |
Alotaibi 2015 |
Exercise |
USA |
49.3, NR, NR |
44 / NR |
22 / 22 |
NR |
NR / 12 |
clinically |
VAS |
4 weeks monophasic pulsed current (MPC) vs MPC and plantar fascia stretch |
Nil difference |
1 |
5 |
PPT |
ADL |
FAAM |
U/S thickness |
DiGiovanni 2003 |
Exercise |
USA |
46, 7.5, 23-60 |
82 / 82 |
24 / 58 |
NR |
10 / NR |
Clinically |
Modified FFI |
Calf stretch vs plantar fascia stretch |
Plantar stretch better than calf stretch |
2 |
4 |
DiGiovanni 2006 |
Exercise |
USA |
NR |
66 / 66 |
NR |
NR |
10 / NR |
clinically |
Modified FFI |
Calf stretch vs plantar fascia stretch |
Nil difference |
24 |
3 |
Engkananuwat |
exercise |
Thailand |
49.8, 6.5, NR |
50 / 50 |
18 / 32 |
NR |
1 / 7.25 |
clinically |
VAS-FA |
Achilles stretch |
Improved PPT in plantar stretch at 1 month only |
1 |
8 * |
2017 |
ROM |
Vs |
3 |
| |
PPT |
Plantar fascia stretch |
|
| |
VAS |
|
|
Kamonseki 2016 |
Exercise |
Brazil |
45.8, NR, NR |
83 / 83 |
18 / 65 |
NR |
1 / 18.3 |
clinically |
VAS |
Stretching |
Nil difference |
2 |
6 * |
FAOS |
Vs |
SEBT |
Stretching & foot strength |
| |
Vs |
| |
Stretch & foot & hip strength |
Radford 2007 |
Exercise |
Australia |
50, 11, NR |
92 / 92 |
36 / 56 |
NR |
1 / 13 (median) |
clinically |
FHSQ |
Sham U/S & stretch vs Sham U/S |
Nil difference |
2 weeks |
8 * |
VAS 1st step |
Rathleff 2014 |
Exercise |
Denmark |
46, 8, NR |
48 / 48 |
16 / 32 |
NR |
03-Jul |
Clinically & ultrasound |
FFI |
Insoles and stretches vs insoles and strength training |
Strength training better at 3 months only |
1 |
6 * |
U/S thickness |
3 |
| |
6 |
| |
12 |
Abigail 2017 |
Manual therapy |
India |
NR, NR, NR |
30 / 30 |
NR |
NR |
NR / NR |
clinically |
NPRS |
U/S |
Manual better |
10 days |
7 * |
FFI |
Vs |
| |
U/S & frictions |
Ajimsha 2014 |
Manual therapy |
Qatar |
41.5, NR, NR |
65 / 65 |
17 / 48 |
sedentary |
NR / 4 |
clinically |
FFI |
Myofascial release vs sham U/S |
Myofascial better |
3 |
6 |
PPT |
| |
Cleland 2009 |
Manual therapy |
USA and New Zealand |
48.4, 8.7, NR |
54 / 54 |
Oct-44 |
NR |
NR / 8.7 |
clinically |
LEFS |
U/S, ice and iontophoresis vs |
Manual better than electrotherapy |
1 |
7* |
FAAM |
soft tissue and rear foot mobs with mobs to hip, knee, ankle, foot as required |
6 |
NRS |
|
|
Dimou 2004 |
Manual therapy |
United Kingdom |
NR, NR, |
20 / 20 |
13-Jul |
NR |
NR / 23.2 |
clinically |
PSW |
foot and ankle joint mobilisations with stretches |
Mobs better at 1 month |
1 |
6* |
23-59 |
PSL |
Vs |
No difference at 2 months |
2 |
| |
FSP |
insoles |
|
|
| |
PPT |
|
|
|
| |
HPL |
|
|
|
Ghafoor 2016 |
Manual therapy |
Pakistan |
47.4, 9.1, NR |
60 / 60 |
Dec-48 |
NR |
NR |
clinically |
FAAM |
standard vs standard & |
Manual better |
3 weeks |
6 |
LEFS |
soft tissue and joint mobs to the foot and calf |
|
NRS |
|
1.5 |
Am 2010 |
Manual therapy |
India |
35.5, NR, NR |
60 / 60 |
35 / 25 |
NR |
3 / NR |
clinically |
FFI |
Standard vs positional release |
No difference |
10 days |
4 |
VAS |
Kuhar 2007 |
Manual Therapy |
India |
43, NR, 28-62 |
30 / 30 |
15 / 15 |
NR |
4.5 / NR |
clinically |
VAS |
Standard (U/S, cryotherapy, strength) |
Myofascial release better |
10 days |
7 * |
FFI |
Vs |
| |
Standard * myofascial release |
Renan-Ordine 2011 |
Manual therapy |
Brazil |
44, 10, NR |
60 / 60 |
15 / 45 |
NR |
NR / 4.6 |
clinically |
Modified SF-36 |
Stretching vs stretching & trigger point therapy (TPT) |
TPT better |
1 |
7* |
PPT |
| |
| |
Shashua 2015 |
Manual therapy |
Israel |
51.3, 12.6, |
56 / 56 |
14 / 32 |
NR |
NR / 5.91 |
clinically |
NRS |
Standard vs standard with sub-talar, talocrural, mid-foot mobs |
No difference |
2 ½ |
8 |
23-73 |
LEFS |
| |
PPT |
| |
ROM |
Wynne 2006 |
Manual therapy |
USA |
NR, NR, 20-66 |
20 / 20 |
Apr-16 |
NR |
NR |
Clinically |
P&DQ |
Osteopathic counterstrain vs placebo |
Counterstrain better immediately, no difference at 6 days |
Immediate |
2 |
Stretch reflex |
6 days |
H reflex |
|
| |
electrotherapy |
USA |
NR, NR, 26-64 |
28 / 31 |
Jul-24 |
NR |
1 / median 6.5 |
clinically |
Distance |
LLLT vs placebo |
No difference |
1 |
7 |
Basford 1998 |
VAS |
| |
Windlass |
Brook 2012 |
electrotherapy |
USA |
52, NR, NR |
70 / 70 |
18 / 52 |
NR |
NR / 12.4 |
Clinically and x-ray |
VAS |
Pulsed radiofrequency electromagnetic field therapy vs placebo |
PRFE better than placebo |
1 week |
9* |
Cinar 2017 |
electrotherapy |
Turkey |
45.5, 9.9, |
49 / 49 |
Sep-40 |
NR |
1 / NR |
clinically |
AOFAS |
Insoles and stretch |
LLLT better at 3 months only |
3 weeks |
7 * |
12-minute walk |
Vs |
|
VAS |
Insole, stretch, LLLT |
3 months |
Crawford 1996 |
electrotherapy |
United Kingdom |
NR, NR, NR |
19 / 26 |
15-Nov |
NR |
NR / NR |
Clinically |
VAS |
U/S |
No difference |
1 |
8 * |
X-ray |
Vs |
| |
Sham U/S |
Gudeman 1997 |
electrotherapy |
USA |
42.1, 13.6, NR |
36 / 40 |
Jul-32 |
NR |
NR |
Clinically and x-ray |
MFS |
Iontophoresis and standard vs placebo and standard |
Iontophoresis better than placebo at 2 weeks, no difference at 6 weeks |
½ |
6 |
1.5 |
Kiritsi 2010 |
electrotherapy |
Greece |
40, NR, NR |
25, 25 |
15-Oct |
NR |
1.5 / NR |
Clinically and U/S |
VAS |
LLLT vs placebo |
LLLT better |
1.5 |
7 |
U/S thickness |
Marcias 2015 |
electrotherapy |
USA |
56.7, NR, 31 -75 |
69 / 69 |
17 / 42 |
NR |
3 / 12.2 |
Clinically |
FSP |
LLLT vs placebo |
VAS better for LLLT at 2 months only |
1 week |
9* |
U/S |
FFI |
2 weeks |
| |
U/S thickness |
3 weeks |
| |
|
1 |
| |
|
1.5 |
| |
|
2 |
Osbourne 2006 |
electrotherapy |
Australia |
51.1, 10.6, NR |
31 / 42 |
28 / 34 |
NR |
NR / 11.8 |
Clinically |
VAS |
Iontophoresis with: |
Acetic acid better |
½ |
9* |
X-ray |
stiffness |
Acetic acid |
U/S |
|
Dexamethasone |
| |
|
placebo |
Straton 2009 |
electrotherapy |
USA |
41, NR, NR |
26 / 26 |
NR |
NR |
¼ / 3.5 |
clinically |
ADL |
Standard vs standard with low frequency electrical stimulation |
No difference |
1 |
5 |
FAAM |
3 |
VAS |
|
Hyland 2006 |
tape |
USA |
39.5, NR, NR |
41 / 41 |
21 / 20 |
NR |
NR |
clinically |
PSFS, |
Stretching vs tape vs sham tape vs control |
Tape better for VAS |
1 week |
4 |
VAS 1st step |
Khatavkar 2015 |
tape |
India |
31.5, NR, NR |
30 / 30 |
Sep-21 |
NR |
NR / NR |
Clinically |
VAS |
Intrinsic foot exercises & cryotherapy |
Tape better all measures |
1 week |
7 * |
U/S |
U/S thickness |
Vs |
| |
PFPS |
kinesiotape |
Radford 2006 |
tape |
Australia |
50, 14, NR |
92 / 92 |
37 / 55 |
NR |
1 / 9 (median) |
clinically |
FHSQ, |
Sham U/S and tape |
Tape better for 1st step VAS only |
1 week |
9* |
VAS 1st step |
Vs |
| |
Sham U/s |
Tsai 2010 |
tape |
Taiwan |
NR, NR, NR |
52 / 57 |
19 / 33 |
NR |
Less than 10 / 4 |
Clinically |
FFI |
U/S & TENS vs U/S TENS & kinesiotape |
Tape better |
1 week |
5 |
U/S |
McGill |
| |
U/S thickness |
Vishal 2010 |
tape |
India |
38.4, NR, NR |
60 / 60 |
35 / 25 |
NR |
NR |
clinically |
VAS |
Stretch, U/S & calcaneal tape |
Plantar fascia tape better than calcaneal |
1 week |
4 |
FFI |
Vs |
| |
Stretch, U/S and plantar fascia tape |
El Salam 2010 |
Tape and orthotics |
Saudi Arabia |
53, NR, NR |
30 / 30 |
23-Jul |
NR |
1 / NR |
clinically |
VAS average, |
Standard and tape |
Orthotic better than tape |
3 weeks |
7 |
MFPDS |
Vs |
| |
Standard and pre-fab orthotic |
Baldassin 2009 |
Orthotics |
Brazil |
47.4, NR, NR |
105 / 105 |
25 / 80 |
sedentary |
NR / 17.9 |
clinically |
Modified FFI |
Pre-fabricated vs custom insole |
No difference |
2 |
8 |
Pressure pain |
Fong 2012 |
Orthotics |
China |
50.6, 5.3, NR |
15 / 15 |
03-Dec |
NR |
NR / 11 |
clinically |
VAS first step |
Barefoot vs normal shoes with flat insoles (NSF) vs normal shoes with custom insoles (NSC) |
All better than barefoot, |
immediate |
6* |
Plantar pressure in-shoe |
Vs rocker shoe flat insoles (RSF) vs rocker shoe custom insole (RSC) |
|
| |
|
Rocker better than normal |
| |
|
|
| |
|
Custom insoles better than flat |
Landorf 2006 |
Orthotics |
Australia |
48.3, NR, NR |
135 / NR |
46 / 89 |
NR |
NR / 12 (median) |
clinically |
FHSQ |
Orthotics: |
3 months |
3 |
9 |
Sham |
Custom & pre-fab better than sham |
12 |
Vs |
No difference custom vs pre-fab. |
|
Pre-fab |
12 months |
|
Vs |
No difference |
|
Custom |
|
|
Oliviera 2015 |
Orthotics |
Brazil |
50.5, NR, NR |
74 / NR |
Aug-66 |
NR |
NR / 4 |
clinically |
VAS |
Custom Insole |
Improved 6 min walk for custom. |
3 |
8 |
6 min walk test |
Vs |
No other difference |
6 |
FFI |
Flat control insole |
|
|
FHSQ |
|
|
|
SF-36 |
|
|
|
Likert |
|
|
|
Pfeffer 1999 |
Orthotics |
USA |
NR, NR, 23-81 |
200 / 200 |
65 / 135 |
NR |
NR |
clinically |
FFI |
Stretch vs |
Pre-fab better than custom or stretching alone |
2 |
5 |
Stretch silicone heel pad vs |
Stretch felt insert vs |
Stretch heel cup vs |
Stretch custom |
Ryan 2009 |
Orthotics |
Canada |
40.3, NR, |
20 / 21 |
NR |
NR |
Jun-21 |
Clinically and x-ray |
VAS |
Ultra-flexible shoe |
No difference |
3 |
4 |
NR |
Vs |
6 |
| |
Conventional running shoe |
|
Winemiller 2003 |
Orthotics |
USA |
41.3, NR, NR |
101 / 101 |
21 / 80 |
NR |
1 / 100 |
Clinically |
Likert |
Magnetised insoles vs placebo insoles |
No difference |
2 |
10 |
VAS |
Wrobel 2015 |
Orthotics |
USA |
49.6, 12.7, 23-75 |
69 / 69 |
26 / 43 |
NR |
Less than 12 / 5.2 |
X-ray and U/S |
FFI |
Orthotics: |
Custom orthotic increased activity. |
3 |
9* |
FSP |
Sham |
No other difference |
SF-36 |
Vs |
|
Physical activity |
Pre-fab |
|
| |
Vs |
|
| |
Custom |
|
Batt 1996 |
Night Splint |
USA |
45.7, NR, 20-74 |
32 / 33 |
Nov-21 |
NR |
NR / 12.7 |
Clinically and X-ray |
VAS |
Standard vs standard with night splint |
standard 6/17 healed at mean 8.8 weeks |
3 |
4 |
| |
|
Number self reported as healed |
night splint 16/16 healed at mean 12.5 weeks |
Lee 2012 |
Night Splint |
Hong Kong |
44, NR, 31-54 |
28 / 28 |
Feb-26 |
NR |
NR / 7.3 |
clinically |
FFI |
Orthosis |
No difference |
½ |
6* |
VAS |
Vs orthosis and night splint |
2 |
Martin 2001 |
Night Splint |
USA |
47, NR, 21-70 |
193 / 193 |
68 / 125 |
NR |
NR / 5 |
clinically |
VAS |
Custom orthotic |
no difference |
3 |
3 |
vs |
pre-fab orthotic |
Vs |
night splint |
Powell 1998 |
Night Splint |
USA |
48, NR, 22-72 |
37 / 49 |
Aug-29 |
NR |
6 / NR |
Clinically and X-Ray |
MCSS |
Night splint for 4 weeks (crossover) |
Better with night splint |
6 |
2 |
AHRS |
Probe 1999 |
Night Splint |
USA |
46, 11, NR |
116 / 146 |
35 / 81 |
NR |
NR / 5 |
Clinically & X-Ray |
Pain 4-point scale |
stretches, piroxicam vs stretches, piroxicam and night splint |
No difference |
1 |
4 |
| |
2 |
SF-36 |
3 |
| |
|
Roos 2006 |
Night Splint |
Sweden |
46, NR, 22-63 |
34 / 34 |
Jul-27 |
40% “active in sports” |
>1 / 4.2 |
clinically |
FAOS |
Custom Orthosis vs night splint vs both |
no difference |
3 |
6 |
Wheeler 2017 |
Night splints |
United Kingdom |
52.1, NR, NR |
40 / 40 |
Nov-29 |
NR |
4 / 25.2 |
Clinically & either U/S or MRI |
FFI |
Exercises |
Nil difference |
1.5 |
7 * |
MOXFQ |
Vs |
3 |
EQ-5D-5L |
Exercises and night splint |
|
HADS |
|
|
PSQI |
|
|
Cotchett 2014 |
acupuncture |
Australia |
56, 122, NR |
84 / 84 |
44 / 40 |
NR |
Jan-14 |
clinically |
VAS |
Dry needling vs sham dry needling |
Dry needling better |
1 ½ |
9 |
FHSQ |
Kumnerddee 2012 |
acupuncture |
Thailand |
53, NR, NR |
24 / 24 |
NR |
NR |
6 / NR |
clinically |
VAS |
Conventional vs conventional and electro acupuncture |
Electro acupuncture better |
1 ½ |
6 |
FFI |
Zhang 2011 |
acupuncture |
Hong Kong |
48, NR, NR |
53 / 53 |
14 / 39 |
NR |
Mar-34 |
clinically |
Pressure pain |
Acupuncture vs control acupuncture |
Acupuncture better at 1 & 6 month |
1 |
8 |
VAS |
3 |
| |
6 |
Legend of terms
Outcome Measures: AHRS – Ankle Hind foot Rating Scale, DF ROM – dorsiflexion range of movement, FAAM – Foot and Ankle Ability Measure, FAOS – Foot And Ankle Outcome Score, FFI – Foot Function Index, FHSQ – Foot Health Status Questionnaire, FSP – First Step Pain, HPL – Heel pain Leisure, LEFS – Lower Extremity Functional Scale, McGill – McGill Medlnack pain questionnaire, MCSS – Mayo Clinical Scoring System, MFDPS – Manchester foot pain & disability Schedule, MFS – Maryland Foot Score, NRS – Numerical Rating Scale, P&DQ – Pain and Dysfunction Questionnaire, PFPS – Plantar fasciopathy pain / Disability Scale score, PPT – Pressure Pain Threshold, PSFS – Patient Specific Functional Scale, PSL – Pain Scale Least, PSW – Pain Scale Worst, SF-36 – Medical Outcomes Study Short Form-36, VAS – Visual Analogue Scale
F/u – follow-up, LLLT – low light laser therapy, Mobs – mobilisations, MRI – Magnetic resonance imaging, NR – not reported, NSAIDs – Non-Steroidal Anti-Inflammatory Drugs, Rx – Treatment, U/S – ultrasound
Critical appraisal
The methodological quality of each article was assessed using the Physiotherapy Evidence Database (PEDro) score. This scoring system was selected as it was developed to assess the internal validity of randomised controlled trials (RCTs) investigating Physiotherapy modalities [20]. The PEDro score is an 11-point scale rating the internal validity of a study’s method. It was developed using a Delphi approach with one measure of external validity not contributing to the total score [20]. Reliability and validity of this approach have been established [21,22] where a PEDro score of 0 represents a study with poor internal validity and a score of 10 a high internal validity. When a study had yet to be reviewed by PEDro this was performed by the authors, indicated by * on table 3. Using the PEDro score, studies were considered excellent quality (≥8/10), good quality (5-7/10) or poor quality (≤4/10) [21,23]. The quality and number of studies were combined for each modality to establish the strength of supporting evidence against criteria proposed by van Tulder et al. [24](table 4).
Table 4. Criteria for strength of evidence (RCTs – randomised controlled trials, CCTs – case-control trials)
Level of evidence |
Criteria |
Strong |
Consistent findings among multiple high-quality RCTs |
Moderate |
Consistent findings among multiple low-quality RCTs and/or CCTs and/or one high-quality RCT |
Limited |
One low-quality RCT and/or CCT |
Conflicting |
Inconsistent findings among multiple trials (RCTs and/or CCTs) |
No evidence |
No RCTs or CCTs |
Search strategy
A total of 1941 articles were identified by the initial search, following removal of duplicates 1102 remained for review of which 1034 studies were excluded from their title and abstracts against the inclusion and exclusion criteria leaving 68 articles requiring review of the full-texts. Five articles were unobtainable, in these cases the lead authors were contacted via e-mail. One author replied and was included; the remaining four did not reply and therefore were not included in the review. Seven studies were excluded based on the eligibility criteria (two were not RCTs, three reported mean symptom duration of less than 3 months, one used non-steroidal anti-inflammatory medication, one used cortisone injections). In seven studies only the abstracts had been published leaving 50 eligible articles (Figure1). A meta-analysis could not be performed due to the extensive heterogeneity in methodology, follow-up and outcome measures used. As a result, an in-depth narrative review was conducted.
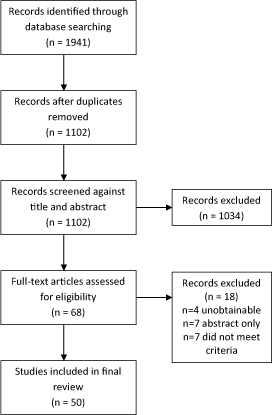
Figure 1. Flow chart showing the search results
Population characteristics
The gender distribution of 45 studies (not reported by 5 studies) was 67% females and 33% males with a mean age (reported in 41 studies) of 46.9 years, a range of 20 – 81 and mean symptom duration of 16.0 months (reported in 26). This is similar to a recent meta-analysis of ESWT for PF with a 65% : 35% female to male ratio, mean age of 50.7 years and mean duration of 16.2 months based on 9 studies and 935 patients [25].
The 50 studies were conducted in 19 countries (USA n=17, Australia n=5, India n=5, Brazil n=4, United Kingdom n=3, Hong Kong n=2, Thailand n=2 and n=1 for China, Canada, Denmark, Greece, Israel, Pakistan, Qatar, Saudi Arabia, Sweden, Taiwan and Turkey with a multi-national study in New Zealand and USA). Racial differences in foot morphology have been demonstrated [26] potentially affecting the ability to generalise these results to a specific population group.
Clinical diagnosis and investigations
To the authors’ knowledge, no clinical tests have been investigated for accuracy in diagnosing PF so the reliability and validity of the tests used within the studies are not known. Only 8 studies employed imaging to support the diagnosis, 7 used ultrasound [27-33] and one study used either ultrasound or MRI [34].
Critical appraisal
Findings of the critical appraisal are presented in table 3. Whilst only the highest level of evidence, namely RCTs, were chosen for this review widespread methodological limitations were seen. Only studies considered high quality (PEDro ≥8/10) or medium-quality (PEDro 5-7/10) were included in the final analysis however all studies were included in table 3 for completeness. Sample sizes of studies were frequently small with a range of 15 to 200 patients and a mean sample size of 59 patients. The internal validity as assessed by the PEDro score showed substantial variability ranging from 2/10 to 10/10 with a mean of 6/10. Only 15 of the 50 studies achieved a high PEDro score (≥8/10) and a further 24 achieved a medium PEDro score (5-7/10).
The review identified 50 RCTs that tested the efficacy of conservative treatments for PF. Seven categories of treatments were identified; exercise (n=7), manual treatment, (n=10), electrotherapy (n=9), tape (n=6), orthotics (n=8), night splints (n=7), and acupuncture (n=3).
Exercise (n=7)
Seven studies investigated exercise therapy; five were medium or high quality. Five reviewed the efficacy of stretching [35-39] and two reviewed strengthening [30,40]. Two studies found short term benefits of exercise, DiGiovanni et al. [35] found a plantar fascia specific stretch to be more effective than a calf stretch after eight weeks treatment and Rathleff et al. [30] found strengthening (weighted heel raises with maximum metatarsal phalangeal joint dorsiflexion) superior to stretching at 12 weeks. Kamonseki et al. [40] found no benefit of adding either foot or foot and hip strengthening to stretching. Whilst a within-group benefit was demonstrated with exercise, no one exercise was found to be superior to another beyond 3 months.
When evidence was combined based on the criteria proposed by van Tulder et al. (table 4) stretching was not useful in either the short term defined as ≤1 month (strong evidence) or the mid-term defined as <6 months (moderate evidence). Strengthening was not useful in the short or long term defined as ≥6 months (moderate and limited evidence respectively) with conflicting evidence in the mid-term.
Manual therapy (n=10)
Ten studies investigated the efficacy of manual therapy techniques including joint mobilisations, soft tissue mobilisation or a combination of both [41-50]. Different manual therapy techniques were investigated in each study and inconsistencies in results were demonstrated. Joint mobilisations were investigated in two studies [41, 48] with neither finding benefit at 2 months. Soft tissue therapy was investigated in six studies finding no benefit of positional release or counterstrain techniques [42,45] however benefit was shown with local frictions at 10 days [50], myofascial release at 10 days and 3 months [43,47] and trigger point therapy at 1 month [46]. A combination of soft tissue and joint techniques were supported by both investigating studies. Joint mobilisations to the foot with soft tissue mobilisations to the foot and calf were beneficial at 3 and 6 weeks [49]. Soft tissue and rear-foot joint mobilisations combined, as required, with mobilisations to the hip, knee and ankle joints were beneficial at 4 weeks and 6 months [44].
When evidence was combined joint mobilisations have limited support in the short term with moderate evidence of no effect in the mid-term. Soft tissue mobilisations were useful in the short term (moderate evidence) and mid-term (limited evidence). A combination of joint and soft tissue techniques were beneficial during the short, mid and long-term (moderate evidence).
Electrotherapy (n= 9)
Nine articles investigated five different forms of electrotherapy including Low Light Laser Therapy (LLLT), Pulsed Radiofrequency Electromagnetic Field Therapy (PRFE), Low Frequency Electrical Stimulation (LFES), ultrasound and iontophoresis. LLLT was investigated in four studies with conflicting results [51, 28, 32, 52]. A PRFE device worn for 7 days was significantly better than a placebo at day 7 [53]. LFES was superior at 4 weeks however at 3 months there was no benefit over a placebo [54]. Ultrasound was of no benefit at 1 month [55]. Comparing iontophoresis with three different chemicals (acetic acid, dexamethasone or placebo) found acetic acid significantly more effective for pain relief and stiffness at 2 weeks [27]. Iontophoresis was significantly better than placebo iontophoresis at 2 weeks but not at 6 weeks [56].
When evidence was combined LLLT was not effective in the short term (strong evidence) however was effective in the mid-term (strong evidence). PRFE was effective in the short term only (moderate evidence), there was conflicting evidence for iontophoresis in the short-term and not effective in mid-term (limited evidence).
Tape (n=5)
Five studies investigated the efficacy of tape [57-59,29,31]. All studies found a significant improvement at a one week follow up, however the tape was applied differently in each study. Non-stretch tape applied to either the longitudinal arch or calcaneus was better than sham [57,58]. Non-stretch tape was more effective when applied to the longitudinal arch than the calcaneus [59]. Kinesio-tape on the calf and plantar surface was more effective than electrotherapy [29] and when applied to the plantar surface was more effective than intrinsic foot exercises [31].
Tape vs orthotics (n=1)
Non-stretch tape was compared to a pre-fabricated (pre-fab) orthotics for 3 weeks with the orthotic more effective [60]. The location of taping was not described.
When evidence was combined tape was effective in the short term (strong evidence) regardless of how applied. There was also limited evidence that an orthotic was more effective than tape in the short-term.
Orthotics (n=8)
Comparing shoe type, one study found both rocker shoes and normal shoes better than barefoot with a rocker better than normal shoes with immediate re-testing only [61], a second study found no difference between a normal running shoe and an ultra-flexible shoe [62].
Studies comparing pre-fabricated (pre-fab) and custom insoles found conflicting results. No difference in any outcomes were found at 2, 3 and 12 months [63,64]. In contrast a pre-fab was better than a custom insole at 2 months [65]; Oliveira et al. and Wrobel et al. found a custom insole increased activity only at 3 and 6 months respectively with no effect on pain [66,33]. On immediate re-testing only a custom insole was better than a flat insole [61].
Studies investigating a “true” insole (either a custom or pre-fab) against a sham insole, found a true insole better at 3 months with no difference at 12 months [63] and a magnetised insole was no better than a placebo insole [67].
When evidence was combined shoe type was effective in the short-term only (limited evidence). Comparing a custom and pre-fab insole there was conflicting evidence in the short term, no difference in the mid-term (strong evidence) or long term (moderate evidence). A “true” orthotic was more effective in the mid-term (moderate evidence) with no difference in the long term (moderate evidence).
Night splints (n=7)
Night splints were investigated in seven studies with conflicting results. No difference was found at 12 weeks between custom orthoses, night splints and a combination of both [68]. Similarly, no difference was detected between custom orthoses, prefabricated orthoses and night splints at 12 weeks [69]. No benefit was found by adding a night splint to calf stretches and NSAIDs at 4, 8 and 12 weeks [70]. No benefit was found by adding a night splint either to an exercise programme [34] or to an orthotic [71]. In contrast, 1 month of night splint use led to a significant improvement that was maintained at 6 months [72]. Also, night splinting gave a significant improvement when added to ibuprofen, calf stretches and a heel cushion at 12 weeks [73]. The quality of studies in this group was the lowest with a mean PEDro of 4/10 and only 3 studies of medium or high quality.
When evidence was combined night splints were ineffective in both the short term (limited evidence) and mid-term (moderate evidence)
Acupuncture (n=3)
Three studies investigated acupuncture [74], electro-acupuncture [75] or dry needling [76]. All demonstrated positive results although all had a relatively short follow-up period. 6 weeks of dry needling to myofascial trigger points was significantly more effective than sham dry needling at 6 and 12 weeks [76]. A specific acupuncture point (PC 7) was more effective than a control point (LI 4) at both 1- and 6-month follow-up [74]. A 5-week multimodal approach (analgesics, shoe modification, stretches to calf and plantar fascia) was compared to the same approach and twice weekly electro-acupuncture. After 6 weeks the electro-acupuncture group were significantly better [75]. The acupuncture group had the highest methodological quality with a mean PEDro of 7.7/10.
When evidence was combined acupuncture was effective in the short term (moderate evidence), mid-term (strong evidence) and long term (moderate evidence).
The aim of this review was to determine the efficacy of conservative modalities considered by author consensus to be within the normal scope of practice for Physiotherapists and Podiatrists treating plantar fasciopathy, termed conventional treatment. This review included only RCTs with their internal validity assessed against the PEDro tool. A range of treatments are currently used reflecting either the difficulty in treating this condition, the poor efficacy of current treatments, or a lack of understanding of this pathology.
ESWT has become more common as an intervention for plantar fasciopathy and tendinopathies. Despite the increase in use, ESWT is still not widely available due to the high equipment cost and additional training required to deliver this modality. A literature search of ESWT for PF identified four recent meta-analyses of RCTs [77-80]. Due to these recent high-level reviews and its use as a second line modality (after initial conservative treatment has failed) ESWT was not included in this review by author consensus.
The studies included in this review highlight a lack of high-quality research in conventional modalities for this pathology. Only 15 of the 50 included studies were deemed of high quality (PEDro ≥8/10). A common limitation of the studies was a short follow-up period with only 3 studies following their patients for one year or longer and two studies only investigating an immediate effect of treatment. No data were provided in any study on symptom recurrence.
This review demonstrated inconsistencies in the ability of conventional treatments to reduce pain and function with no single treatment being found to be superior at all time points. No adverse outcomes were reported for stretching or strengthening programs. In contrast, long-term use of orthotics was found to reduce intrinsic plantar muscle strength [81] which has been linked to PF [10,11].
Only one study reported their patient group included a sporting population [68]. No study exclusively examined the athletic population, so this group is under-represented both in this review and the current literature. Differences in the rate, repetition and duration of plantar fascia loading are expected between, for example, high-mileage runners and sedentary groups. As such the findings of this review should be applied to this group with caution.
No study has investigated the accuracy (reliability and validity) of clinical diagnostic tests for PF. It was therefore surprising to find that only 8 of the 50 studies employed radiological imaging to support their clinical diagnosis (US n=7, US or MRI n=1). Findings by McMillan et al. [82] demonstrated a fascial thickening greater than 4mm and hypoechoic areas detected on US were 100 and 200 times respectively more likely to confirm the presence of PF. A number of differential diagnoses for PF exist including Baxter’s nerve compression, tarsal tunnel syndrome, calcaneal stress fracture and plantar fascia rupture [83,84] with 15% of plantar heel pain suggested to be neural in origin [85]. It is therefore possible that in the trials that did not use radiological investigations patients may have been included who did not have PF. The validity of these studies is therefore questionable, and this should be considered in any interpretation.
A meta-analysis of included studies was not possible as 22 different outcome measures were used. The most common outcome measures were versions of the Visual Analogue Scale / Numerical Rating Scale (n=7). The substantial variation in outcome measures as well as the lack of validated instruments for assessing the efficiency of treatments for PF makes this an area of priority for future research.
Efficacy of individual treatments is difficult to conclude as only 14 studies assessed interventions against a placebo and 16 against a control intervention. The remaining 20 studies compared two or more interventions. When interventions are compared without a control, between-group and within-group differences are difficult to interpret. For example, Rathleff et al. [30] compared stretching to strengthening with no between group difference at 1-year follow-up however both groups showed a within group difference. Either this may represent the natural time course of PF or that both treatments were equally effective.
Moderate or strong evidence from medium and high quality RCTs (PEDro ≥5) were collated. Supported modalities in the short-term (up to 1 month) were manual therapy, PRFE, tape and acupuncture. In the mid-term (less than 6 months) manual therapy, LLLT, an orthotic and acupuncture were beneficial. In the long term (6 months or longer) only manual therapy and acupuncture were supported. Using strong evidence only, a very limited number of modalities were supported. In the short term only tape was supported, in mid-term LLLT and acupuncture were supported, no modalities were supported in the long term based on strong evidence alone.
Interestingly, a survey of 457 UK Physiotherapists’ and Podiatrists’ perception of the most effective treatment for PF does not correlate with the findings of this review [86]. Both professions advocated calf stretches, Podiatrists advocated custom orthotics, arch support orthotics and night splints, while Physiotherapists advocated electrotherapy (specifically ultrasound), manual therapy and acupuncture.
This systematic review was limited by the inability to perform a meta-analysis as 22 different outcome measures were used. Only RCTs were included in the review to enhance the validity of conclusion however robust cohort studies may have added to the evidence base available to review.
This review has highlighted no major safety concerns of the conventional treatments for plantar fasciopathy. The research is generally of low to medium quality with poor sample sizes and short follow-up making definitive conclusions difficult to formulate. Based on strong evidence alone tape was supported in the short term (≤1 month), low light laser therapy (LLLT) and acupuncture were supported in the mid-term (<6 months) and there was no strong evidence for any modality in the long term (≥6 months). Further well-designed multi-centre RCTs that include accurate clinical diagnostic criteria as well as valid and reliable outcome measures are required to help guide therapists to the optimal conservative treatments for this condition.
- Riddle DL, Schappert SM (2004) Volume of ambulatory care visits and patterns of care for patients diagnosed with plantar fasciitis: a national study of medical doctors. Foot & ankle international 25: 303-310. [Crossref]
- Riddle DL, Pulisic M, Sparrow K (2004) Impact of demographic and impairment-related variables on disability associated with plantar fasciitis. Foot & ankle international 25: 311-317. [Crossref]
- Taunton JE, Ryan MB, Clement DB, McKenzie DC, Lloyd-Smith DR, et al. (2002) A retrospective case-control analysis of 2002 running injuries. British journal of sports medicine 36: 95-101. [Crossref]
- Tong KB, Furia J (2010) Economic burden of plantar fasciitis treatment in the United States. Am J Orthop 39: 227-231. [Crossref]
- National Institute for Clinical Excellence (NICE) (2009) Extracorporeal shockwave therapy for refractory plantar fasciitis. Guidance 2009b.
- Acevedo JI, Beskin JL (1998) Complications of plantar fascia rupture associated with corticosteroid injection. Foot Ankle Int. 19: 91-97. [Crossref]
- Tatli YZ, Kapasi S (2009) The real risks of steroid injection for plantar fasciitis, with a review of conservative therapies. Curr Rev Musculoskelet Med 2: 3-9. [Crossref]
- Bartold SJ (2004) The plantar fascia as a source of pain—biomechanics, presentation and treatment. J bodywork and movement therapies 8: 214-226.
- Lemont H, Ammirati KM, Usen N (2003) Plantar fasciitis: a degenerative process (fasciosis) without inflammation. J Am Podiatr Med Assoc 93: 234-237. [Crossref]
- Chang R, Kent-Braun JA, Hamill J (2012) Use of MRI for volume estimation of tibialis posterior and plantar intrinsic foot muscles in healthy and chronic plantar fasciitis limbs. Clin Biomech 27: 500-505. [Crossref]
- Cheung RTH, Sze LKY, Mok NW, Ng GYF (2015) Intrinsic foot muscle volume in experienced runners with and without chronic plantar fasciitis. J Sci Med Sport 19: 713-715. [Crossref]
- Lee SY, Park HJ, Kwag HJ, Hong HP, Park HW, et al. (2014) Ultrasound elastography in the early diagnosis of plantar fasciitis. Clin Imaging 38: 715-718. [Crossref]
- Huang YC, Wei SH, Wang HK, Lieu FK (2010) Ultrasonographic guided botulinum toxin type A for plantar fasciitis: an outcome-based investigation for treating pain and gait changes. J Rehabil Med 42: 136-140. [Crossref]
- Van de Water AT, Speksnijder CM (2010) Efficacy of taping for the treatment of plantar fasciosis: a systematic review of controlled trials. J Am Podiatr Med Assoc 100: 41-51. [Crossref]
- Podolsky R, Kalichman L (2015) Taping for plantar fasciitis. J Back Musculoskelet Rehabil 28: 1-6. [Crossref]
- Garrett TR, Neibert PJ (2013) The effectiveness of a gastrocnemius-soleus stretching program as a therapeutic treatment of plantar fasciitis. J Sport Rehabil 22: 308-312. [Crossref]
- Clark RJ, Tighe M (2012) The effectiveness of acupuncture for plantar heel pain: a systematic review. Acupunct Med 30: 298-306. [Crossref]
- Lee SY, McKeon P, Hertel J (2009) Does the use of orthoses improve self-reported pain and function measures in patients with plantar fasciitis? A meta-analysis. Phys Ther Sport 10: 12-18. [Crossref]
- De Vera Barredo R, Menna D, Farris JW (2007) An evaluation of research evidence for selected physical therapy interventions for plantar fasciitis. J Physical Therapy Science 19: 41-56.
- Verhagen AP, de Vet HC, de Bie RA, Kessels AG, Boers M, Bouter LM, et al. (1998) The Delphi list: a criteria list for quality assessment of randomized clinical trials for conducting systematic reviews developed by Delphi consensus. J Clin Epidemiol 51: 1235-1241. [Crossref]
- Maher CG, Sherrington C, Herbert RD, Moseley AM, Elkins M (2003) Reliability of the PEDro scale for rating quality of randomized controlled trials. Physical therapy 83: 713-721. [Crossref]
- De Morton NA (2009) The PEDro scale is a valid measure of the methodological quality of clinical trials: a demographic study. Aust J Physiother 55: 129-133. [Crossref]
- Rowe V, Hemmings S, Barton C, Malliaras P, Maffulli N, et al. (2012) Conservative management of midportion achilles tendinopathy. Sports med 42: 941-967. [Crossref]
- Van Tulder M, Furlan A, Bombardier C, Bouter L, Editorial Board of the Cochrane Collaboration Back Review Group (2003) Updated method guidelines for systematic reviews in the cochrane collaboration back review group. Spine 28: 1290-1299. [Crossref]
- Sun J, Gao F, Wang Y, Sun W, Jiang B, et al. (2007) Extracorporeal shock wave therapy is effective in treating chronic plantar fasciitis: A meta-analysis of RCTs. Medicine 96: 1-7. [Crossref]
- Golightly YM, Hannan MT, Dufour AB, Jordan JM (2012) Racial differences in foot disorders and foot type. Arthritis Care Res 64:1756-1759. [Crossref]
- Osborne HR, Allison GT (2006) Treatment of plantar fasciitis by LowDye taping and iontophoresis: short term results of a double blinded, randomised, placebo controlled clinical trial of dexamethasone and acetic acid. Br J Sports Med 40: 545-549. [Crossref]
- Kiritsi O, Tsitas K, Malliaropoulos N, Mikroulis G (2010) Ultrasonographic evaluation of plantar fasciitis after low-level laser therapy: results of a double-blind, randomized, placebo-controlled trial. Lasers med sci 25: 275-281. [Crossref]
- Tsai CT, Chang WD, Lee JP (2010) Effects of short-term treatment with kinesiotaping for plantar fasciitis. J Musculoskeletal Pain 18: 71-80.
- Rathleff MS, Mølgaard CM, Fredberg U, Kaalund S, Andersen KB, et al. (2015) High‐load strength training improves outcome in patients with plantar fasciitis: A randomized controlled trial with 12‐month follow‐up. Scand J Med Sci Sports 25: 292-300. [Crossref]
- Khatavkar AV, Palekar TJ, BASU S (2015) Comparative study of kinesiotaping versus intrinsic muscle strengthening and cryotherapy in the treatment of chronic plantar fascitis. Int J Pharm Bio Sci 6: 486-497.
- Macias DM, Coughlin MJ, Zang K, Stevens FR, Jastifer JR, et al. (2015) Low-level laser therapy at 635 nm for treatment of chronic plantar fasciitis: a placebo-controlled, randomized study. J Foot Ankle Surg 54: 768-772. [Crossref]
- Wrobel JS, Fleischer AE, Crews RT, Jarrett B, Najafi B (2015) A randomized controlled trial of custom foot orthoses for the treatment of plantar heel pain. J Am Podiatr Med Assoc 105: 281-294. [Crossref]
- Wheeler PC (2017) The addition of a tension night splint to a structured home rehabilitation programme in patients with chronic plantar fasciitis does not lead to significant additional benefits in either pain, function or flexibility: a single-blinded randomised controlled trial. BMJ open sport exerc med 3: 1-11. [Crossref]
- Digiovanni BF, Nawoczenski DA, Lintal ME, Moore EA, Murray JC, et al. (2003) Tissue-specific plantar fascia-stretching exercise enhances outcomes in patients with chronic heel pain: a prospective, randomized study. J Bone Joint Surg Am 85: 1270-1277. [Crossref]
- Digiovanni BF, Nawoczenski DA, Malay DP, Graci PA, Williams TT, et al. (2006) Plantar fascia-specific stretching exercise improves outcomes in patients with chronic plantar fasciitis: a prospective clinical trial with two-year follow-up. J Bone Joint Surg Am 88: 1775-1781. [Crossref]
- Radford JA, Landorf KB, Buchbinder R, Cook C (2007) Effectiveness of calf muscle stretching for the short-term treatment of plantar heel pain: a randomised trial. BMC musculoskeletal disorders 8: 36-44. [Crossref]
- Alotaibi AK, Petrofsky JS, Daher NS, Lohman E, Laymon M, et al. (2015) Effect of monophasic pulsed current on heel pain and functional activities caused by plantar fasciitis. Med Sci Monit 21: 833-839. [Crossref]
- Engkananuwat P, Kanlayanaphotporn R, Purepong N (2018) Effectiveness of the simultaneous stretching of the Achilles tendon and plantar fascia in individuals with plantar fasciitis. Foot Ankle Int 39: 75-82. [Crossref]
- Kamonseki DH, Gonçalves GA, Liu CY, Júnior IL (2016) Effect of stretching with and without muscle strengthening exercises for the foot and hip in patients with plantar fasciitis: a randomized controlled single-blind clinical trial. Man ther 23: 76-82. [Crossref]
- Dimou ES, Brantingham JW, Wood T (2004) A randomized, controlled trial (with blinded observer) of chiropractic manipulation and Achilles stretching vs. orthotics for the treatment of plantar fasciitis. J American Chiropra Assoc 41: 32-42.
- Wynne MM, Burns JM, Eland DC, Conatser RR, Howell JN (2006) Effect of counterstrain on stretch reflexes, hoffmann reflexes, and clinical outcomes in subjects with plantar fasciitis. J Am Osteopath Assoc 106: 547-556. [Crossref]
- Kuhar S, Subhash K, Chitra J (2007) Effectiveness of myofascial release in treatment of plantar fasciitis: A RCT. Indian J Physiotherapy and Occupational Therapy-An Internat J 1: 3-9.
- Cleland JA, Abbott JH, Kidd MO, Stockwell S, Cheney S, et al. (2009) Manual physical therapy and exercise versus electrophysical agents and exercise in the management of plantar heel pain: a multicenter randomized clinical trial. J Orthop Sports Phys Ther 39: 573-585. [Crossref]
- AM H, Kage Vijay B, Basavaraj C (2010) Comparison of myofascial release and positional release therapy in plantar fasciitis–a clinical trial. Indian Journal 4: 8-11.
- Renan-Ordine R, Alburquerque-SendÍn F, Rodrigues De Souza DP, Cleland JA, Fernández-de-las-Peñas C (2011) Effectiveness of myofascial trigger point manual therapy combined with a self-stretching protocol for the management of plantar heel pain: a randomized controlled trial. J Orthop Sports Phys Ther 41: 43-50. [Crossref]
- Ajimsha MS, Binsu D, Chithra S (2014) Effectiveness of myofascial release in the management of plantar heel pain: a randomized controlled trial. The Foot 24: 66-71. [Crossref]
- Shashua A, Flechter S, Avidan L, Ofir D, Melayev A, et al. (2015) The effect of additional ankle and midfoot mobilizations on plantar fasciitis: a randomized controlled trial. J Orthop Sports Phys Ther, 45: 265-272. [Crossref]
- Ghafoor I, Ahmad A, Gondal JI (2016) Effectiveness of routine physical therapy with and without manual therapy in treatment of plantar fasciitis. Rawal Medical Journal 41: 2-6.
- Abigail AJ, Kamalakannan M (2017) Effectiveness of cyriax friction massage along with ultrasound therapy in patients with plantar fasciitis. Int J Pharm Bio Sci 8: 841-848.
- Basford JR, Malanga GA, Krause DA, Harmsen WS (1998) A randomized controlled evaluation of low-intensity laser therapy: plantar fasciitis. Arch Phys Med Rehabil 79: 249-254. [Crosref]
- Cinar E, Saxena S, Uygur F (2018) Low-level laser therapy in the management of plantar fasciitis: a randomized controlled trial. Lasers Med Sci 33: 949-958. [Crossref]
- Brook J, Dauphinee DM, Korpinen J, Rawe IM (2012) Pulsed radiofrequency electromagnetic field therapy: a potential novel treatment of plantar fasciitis. J Foot Ankle Surg 51: 312-316. [Crossref]
- Stratton M, McPoil TG, Cornwall MW, Patrick K (2009) Use of low-frequency electrical stimulation for the treatment of plantar fasciitis. J Am Podiatr Med Assoc 99: 481-488. [Crossref]
- Crawford F, Snaith M (1996) How effective is therapeutic ultrasound in the treatment of heel pain? Ann Rheum Dis 55: 265-267. [Crossref]
- Gudeman SD, Eisele SA, Heidt RS, Colosimo AJ, Stroupe AL (1997) Treatment of Plantar Fasciitis by lontophoresis of 0.4% Dexamethasone: A Randomized, Double-Blind, Placebo-Controlled Study. Am J Sports Med 25: 312-316. [Crossref]
- Hyland MR, Webber-Gaffney A, Cohen L, Lichtman SW (2006) Randomized controlled trial of calcaneal taping, sham taping, and plantar fascia stretching for the short-term management of plantar heel pain. J Orthop Sports Phys Ther 36: 364-371. [Crossref]
- Radford JA, Landorf KB, Buchbinder R, Cook C (2006) Effectiveness of low-Dye taping for the short-term treatment of plantar heel pain: a randomised trial. BMC musculoskeletal disord 7: 64-71. [Crossref]
- Vishal B, Santosh M, Ganesh BR (2010) Effectiveness of plantar fasciitis taping and calcaneal taping in plantar heel pain-A randomized clinical trial. Indian Journal 4: 86-90.
- El Salam MSA, ELhafz YNA (2011) Low-dye taping versus medial arch support in managing pain and pain-related disability in patients with plantar fasciitis. Foot Ankle Spec 4: 86-91. [Crossref]
- Fong DTP, Pang KY, Chung MML, Hung ASL, Chan KM (2012) Evaluation of combined prescription of rocker sole shoes and custom-made foot orthoses for the treatment of plantar fasciitis. Clin Biomech 27: 1072-1077. [Crossref]
- Ryan M, Fraser S, McDonald K, Taunton J (2009) Examining the degree of pain reduction using a multielement exercise model with a conventional training shoe versus an ultraflexible training shoe for treating plantar fasciitis. Phys Sportsmed 37: 68-74. [Crossref]
- Landorf KB, Keenan AM, Herbert RD (2006) Effectiveness of foot orthoses to treat plantar fasciitis: a randomized trial. Arch Intern Med 166: 1305-1310. [Crossref]
- Baldassin V, Gomes CR, Beraldo PS (2009) Effectiveness of prefabricated and customized foot orthoses made from low-cost foam for noncomplicated plantar fasciitis: a randomized controlled trial. Arch Phys Med Rehabil 90: 701-706. [Crossref]
- Pfeffer G, Bacchetti P, Deland J, Lewis AI, Anderson R, et al. (1999) Comparison of custom and prefabricated orthoses in the initial treatment of proximal plantar fasciitis. Foot Ankle Int 20: 214-221. [Crossref]
- Oliveira HAV, Jones A, Moreira E, Jennings F, Natour J (2015) Effectiveness of total contact insoles in patients with plantar fasciitis. J Rheumatol 42: 870-878. [Crossref]
- Winemiller MH, Billow RG, Laskowski ER, Harmsen WS (2003) Effect of magnetic vs sham-magnetic insoles on plantar heel pain: a randomized controlled trial. JAMA 290: 1474-1478. [Crossref]
- Roos E, Engström M, Söderberg B (2006) Foot orthoses for the treatment of plantar fasciitis. Foot Ankle Int 27: 606-611. [Crossref]
- Martin JE, Hosch JC, Goforth WP, Murff RT, Lynch DM et al. (2001) Mechanical treatment of plantar fasciitis: a prospective study. J Am Podiatr Med Assoc 91: 55-62. [Crossref]
- Probe RA, Baca M, Adams R, Preece C (1999) Night splint treatment for plantar fasciitis. A prospective randomized study. Clin Orthop Relat Res 368: 190-195. [Crossref]
- Lee W, Wong WY, Kung E, Leung A (2012) Effectiveness of adjustable dorsiflexion night splint in combination with accommodative foot orthosis on plantar fasciitis. J Rehabil Res Dev 49: 1557-1564. [Crossref]
- Powell M, Post WR, Keener J, Wearden S (1998) Effective treatment of chronic plantar fasciitis with dorsiflexion night splints: a crossover prospective randomized outcome study. Foot Ankle Int 19:10-18. [Crossref]
- Batt ME, Tanji JL, Skattum N (1996) Plantar fasciitis: a prospective randomized clinical trial of the tension night splint. Clin J Sport Med 6:158-162. [Crossref]
- Zhang SP, Yip TP, Li QS (2011) Acupuncture treatment for plantar fasciitis: a randomized controlled trial with six months follow-up. Evid Based Complement Alternat Med 1:1-10. [Crossref]
- Kumnerddee W, Pattapong N (2012) Efficacy of electro-acupuncture in chronic plantar fasciitis: a randomized controlled trial. Am J Chin Med 40: 1167-1176. [Crossref]
- Cotchett MP, Munteanu SE, Landorf KB (2014) Effectiveness of trigger point dry needling for plantar heel pain: a randomized controlled trial. Physical therapy 94:1083-1094. [Crossref]
- Aqil A, Siddiqui MR, Solan M, Redfern DJ, Gulati V, et al. (2013) Extracorporeal shock wave therapy is effective in treating chronic plantar fasciitis: a meta-analysis of RCTs. Clin Orthop Relat Res 471: 3645-3652. [Crossref]
- Dizon JNC, Gonzalez-Suarez C, Zamora MTG, Gambito ED (2013) Effectiveness of extracorporeal shock wave therapy in chronic plantar fasciitis: a meta-analysis. Am J Phys Med Rehabil 92: 606-620. [Crossref]
- Yin MC, Ye J, Yao M, Cui XJ, Xia Y, et al. (2014) Is extracorporeal shock wave therapy clinical efficacy for relief of chronic, recalcitrant plantar fasciitis? A systematic review and meta-analysis of randomized placebo or active-treatment controlled trials. Archives physical med rehabilitation 95:1585-1593.
- Lou J, Wang S, Liu S, Xing G (2017) Effectiveness of extracorporeal shock wave therapy without local anesthesia in patients with recalcitrant plantar fasciitis: a meta-analysis of randomized controlled trials. Am J Phys Med Rehabil 96: 529-534. [Crossref]
- McClinton S, Collazo C, Vincent E, Vardaxis V (2016) Impaired Foot Plantar Flexor Muscle Performance in Individuals With Plantar Heel Pain and Association With Foot Orthosis Use. J orthop sport phys ther 46: 681-688. [Crossref]
- McMillan AM, Landorf KB, Barrett JT, Menz HB, Bird AR (2009) Diagnostic imaging for chronic plantar heel pain: a systematic review and meta-analysis. J Foot Ankle Res 2:1-11. [Crossref]
- Hossain M, Makwana N (2011) Not Plantar Fasciitis: the differential diagnosis and management of heel pain syndrome. Orthopaedics and trauma 25:198-206.
- Lareau CR, Sawyer GA, Wang JH, DiGiovanni CW (2014) Plantar and medial heel pain: diagnosis and management. J Am Acad Orthop Surg 22: 372-380. [Crosref]
- Alshami AM, Souvlis T, Coppieters MW (2008) A review of plantar heel pain of neural origin: differential diagnosis and management. Man Ther 13: 103-111. [Crossref]
- Ferdinand NC, Smith GD, Smith S (2014) A survey comparing the perceptions of physiotherapists and podiatrists in the management of plantar fasciitis. Int J Ther Rehabi 21: 526-538.

