Abstract
Purpose:
Review of literatures reveals that there are an abundance of information discussing the pathology and many different treatments for the shoulder impingement and rotator cuff dysfunction however, to the clinician designing the treatment regimen based on biomechanical approach to shoulder dysfunction is vital.
Case presentation:
A 49 year-old male patient complained insidious type of left shoulder pain. The pain was sharp on elevation of the left shoulder away from the body. The pain was triggered by lying on left side, lifting and reaching overhead functional activities with the left arm and his doctor referred him to physical therapy with a diagnosis of frozen shoulder.
Discussion:
The patient underwent six weeks rehabilitation physical therapy interventions by carefully analyzing the shoulder biomechanics in related to painful and stiff shoulder due to impingement and rotator cuff disease. Conclusion:
The purpose of this case report was to present the biomechanics approach of the entire shoulder region associated with shoulder impingement and rotator cuff disease for fitting course of physiotherapy interventions in order to effectively accomplish and coming back to regular activities of daily livings.
Key words
Subacromial impingement syndrome, Rotator cuff dysfunction, Biomechanics
Introduction
Shoulder pain is a collective musculoskeletal illness in the overall population. Shoulder impingement syndrome and rotator cuff dysfunction are among the most common origins of shoulder pain and diseases and consequently seen in primary care practices. The frequency of shoulder pain and rotator cuff dysfunction occur with aging. The shoulder dysfunction symptomatology and number of findings are various also overlap each other however; successful outcomes of impingement syndrome are dependent on accurate diagnosis. It is attained by knowledge of the regional anatomy, the biomechanics analysing of shoulder movements and the precise understanding of the pathology determined through a detailed history, comprehensive physical examination and diagnostic studies. A study shows that conservative management of shoulder impingement syndrome was recovered the problem in 70-90% of patients, although in certain cases, surgical intervention is required [1]. This brief case study example is discussed by motion based normal biomechanics approach.
Case Presentation
Subjective examination
Case report illustrated a 49-year-old man who works as an automobile (three wheeler) driver over the last 12 years, which involves repetitive forceful left shoulder movements and stooped position prolong time during the ride. He complained a five month history of left shoulder pain and also on the left lower neck; middle area of scapula region. His symptoms appear gradual onset, with no any previous reported trauma to left upper limp, no any history of pins and needles or paraesthesia pain type (red flags) to left upper limb; however symptoms had worsen. The pain was sharp on abduction and flexion of the left shoulder and changed to a dull pain which lasted for several hours. It was aggravated by lying on the shoulder, reaching and lifting with the left arm overhead functional activities. His doctor referred him to physical therapy with a diagnosis of frozen shoulder. Pain was eased to certain extent with medication also the patient has comorbidity history of dyslipidaemia and diabetes mellitus but was under controlled by the medications [2-6].
Physical examination
The left shoulder examination was accomplished by a systemic approach. It contains inspection, palpation, range of motion, strength testing, neurologic assessment, and performance of special shoulder tests [7]. In addition to that assessment of the proximal region of cervical spine and distal region of elbow joint were examined because of the frequent referred pain in the shoulder region. Manual Muscle Testing (MRC scale) revealed weakness in abduction, elevation, and external rotation. The joint play movement pattern of restriction was described by Cyriax, external rotation is the most restricted motion in the early stages of shoulder stiffness as the capsular pattern of the shoulder then abduction and finally internal rotation [8]. The passive motion performed to ensure absence of adhesive capsulitis. Pain and functional assessment was measured by VAS and DASH tool respectively. The initial assessment, at plump line standing posterior to anterior view, left side acromion process of scapula slightly was elevated and also during the arm motion; shoulder shrug initiates movement without significant lateral translation of inferior angle of scapula away from midline. Plump line at lateral view, slightly kyphosis of thoracic spine with forwarded upper cervical spine and scapula was displaced ventrally over the top of the thoracic His left upper tapezius presented with jumping sign, infraspinatus, subscapularis and pectoralis major muscles were spasmodic and tender upon soft tissue inspection and also tenderness of bicepital, supraspinatus tendon. Moreover, left coracoid process, acromioclavicular joint tender compare to right bony and soft tissue inspection left side pain remarkably noticed. There was severe tenderness on the left deltoid insertion. Left glenohumaral motions limited in all aspects. His active left glenohumeral ROM was; flexion110º, abduction was painful at 70º with multi diagonal plane instead of coronal/plane of scapula, external rotation 30º and internal rotation 40º. The left glenohumeral joint passive ROM was much more achievable compare to active ROM; however their all inner range were stiff and painful in each direction. Pain and soft tissue tightness were the limiting factors at the end of all ranges. Passive mobility testing of the glenohumeral joint indicated gliding restricted in the anterior and inferior directions. The manual muscle testing of left glenohumeral joint flexion, abduction, internal and external rotations indicated all gross movement shoulder girdle muscular imbalances with weakness and tightness between agonist and antagonist as well as stabilizers. Limited in inferior and medial movements of scapular mobilization was identified. Active and passive cervical spine all directions end range of motion was slightly limited however, the left shoulder pain could not be reproduced by the neck examinations because the continuing cervical orthopaedic and neurological tests were within normal limits, more over all elbow joint movements and functional capabilities were normal. Patient pointed a VAS of 7/10 and DASH score 28.4. Special tests such as Apple’s scratch test, Empty can test, Speed’s test and Hawkins Kennedy impingement test were positive [7,9].
Investigation
Hematological tests revealed normal ESR level. Plain radiograph of the left shoulder revealed narrowing subacromial space associated with superior migration of the humeral head and subchondral sclerosis found left humeral head area (Figure 1) [10]. Ultrasound scan of left shoulder found that there was evidence of mild thickening with few tiny calcifications in the supraspinatus and bicipital tendon, subsequently were tendinitis (Figure 2) [10].
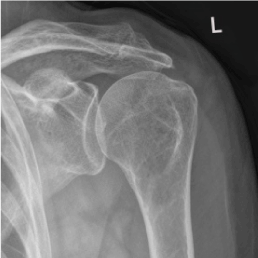
Figure 1. X-ray of left shoulder
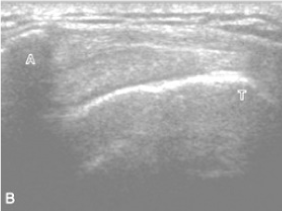
Figure 2. Ultrasound scan of left shoulder
Clinical diagnosis
This patient was present with a history of insidious type shoulder pain that had converted progressively more limiting root causes for normal daily livings. The pain was usually aggravated by overhead functional activities, worse at night and slightly reduced with anti-inflammatory drugs. The history and the clinical examination findings suggested left subacromial impingement of suprapinatus, bicipital tendenitis associated with posterior capsule tightness it had resulted to minimize the functional abilities of the patient. This secondary impingement was resulted from the patient occupation in the long run, developed muscular imbalance in left gleno humeral girdle, tightness in pectoralis major restricted posterior clavicular motion and pectoralis minor shortened to lead anteriorly tilt the scapula due to it attachment to coracoid process both affected normal scapular movement.
Out comes
The patient was seen two times per week in physical therapy for six weeks. The treatment was designed to three phases two weeks in each phase. The phase I focused to reduce pain and inflammation of soft tissues. This was achieved by applying superficial heat, soft tissue mobilization to the left upper trapezius and phonophoresis to left bicipital and supraspinatus tendinopathy by using ultrasound for first two weeks. Then phase II emphasized to gentle oscillation grade 1 and 2 were performed at the left glenohumeral joint to promote mechanoreceptor activity and reduce pain followed by a home exercises program implemented, which consisted pain free passive and active assisted exercises and gentle sustained stretching demonstrated for tight muscles of left shoulder girdle such as upper trapezius, pectoralis major, minor and supscapularis. Finally the phase III more aggressive techniques were initiated as the pain was subsided left glenohumeral joint long axis distraction, anteroposterior and postero inferior manual grade 3and 4 manipulation, capsular stretches, scapular strengthening exercises by using 0.5 kg dumbbells in all planes of glenohumeral ROM and with multi angle functional exercises were introduced. Patient’s left shoulder movements, strength and pain were markedly improved after the rehabilitation. There was a marked improvement in pain VAS score 1/10 as well as DASH score 45.6 and the range of motion at the left glenohumeral with flexion ROM was 150°, abduction 130°, external rotation 60° and internal rotation 60°. The patient could perform mostly pain free all his activities of daily living.
Discussion
Anatomy
The human shoulder is an elegant piece of machinery and the most mobile joint in the body. This mobility provides the upper extremity with marvelous range of motion such as adduction, abduction, flexion, extension, internal rotation, external rotation, and circumduction. However, this large range of motion can cause to joint problems. Moreover, the shoulder permits for scapular protraction, retraction, elevation, and depression. These broad movements also lead to unstable of the shoulder joint. This instability is reinforced by rotator cuff muscles, tendons, ligaments, and the glenoid labrum. Knowledge of anatomy arrangements of different layers of the shoulder and how they are built and connected to each other to allow greatest range of motion and also how it can be injured, and how challenging recovery can be when the shoulder is injured. The deepest layer of the shoulder includes the bones and the joints. Then the layer is made up of the ligaments of the joint capsule. Finally, the tendons and the muscles are arranged [11-13].
Biomechanics approach
The biomechanical analysis of the shoulder emphasizes the synchronized movement of four joints: glenohumeral, scapulothoracic, sternoclavicular, and acromioclavicular. As the humerus moves into elevation, movement must occur at all four joints [14]. This joint movement has been described as the joint arthrokinematics, or the intricate movement of the joint surfaces. Shoulder elevation is defined as the movement of the humerus away from the side, and it can result from arthrokinematics of the glenohumeral joint [15]. Arthrokinematic describes rolling, spining, and sliding in different directions at the joint surfaces, as the bone moves through the body planes. Normal arthrokinematic movements take place only in the incidence of normal periarticular connective tissue, extensibility, and integrity and normal tension relationship muscle function [16]. The rotator cuff muscles allow dynamic stabilization to the humeral head onto glenoid fossa, forming a force couple with the deltoid to permit elevation of the arm. This force couple is in control for 45% of abduction strength and 90% of external rotation strength [17]. Static stabilizers are made up of articular morphology, glenoid labrum, joint capsule, glenohumeral ligaments and inherent negative pressure of the joint. Dynamic stabilizers contain the rotator cuff muscles, long head of the biceps tendon and other shoulder girdle muscles such as pectoralis major, minor, latismusdorsi and serratus anterior [18]. A stiff shoulder has inadequate capsular flexibility and changed muscle function in order to reestablish harmonious movement within the shoulder complex the therapist must rehabilitate the connective tissue by restoring it extensibility and restore normal muscles balance.
Pathophysiology of Impingement syndrome
Shoulder impingement syndrome is reflected to be the most recurrent cause of shoulder pain and disability. Impingement in the shoulder happens when the soft tissues such as supraspinatus, long head of biceps brachii tendon, sub acromial bursitis and superior joint capsule occupying the subacromial space are encroached upon by the coracoacromial arch. Disorders involving shoulder impingement and can consequence in chronic symptoms with functional impairments. It is often refractory to conservative treatments including mainly physical therapy instead of surgical intervention. A number of subacromial impingement categories have been identified including external impingement and internal impingement [19]. Research was carried out by Neer on impingement based on cadaveric dissections, clinical and surgical experience. He established a classification system that defines three stages in the spectrum of rotator cuff impingement that follow a pattern of severity.3 Stage 1 is described by acute inflammation, oedema and hemmorrage in the rotator cuff. In stage 2, the rotator cuff tendon developments to fibrosis and tendinitis. As this condition progresses, it may principal to mechanical disturbance of the rotator cuff tendon and to alter in the coracoacromial arch with osteophytes along anterior acromion in stage 3. Moreover, he described external impingement as the compression and abrasion of the bursal side of the rotator cuff beneath the anterior acromion, and lead to anterior acromioplasty as a treatment. External impingement is now agreed as a much wider understanding than that defined by Neer, and could take in compression or abrasion of the tendon of the long head of biceps brachii beneath any aspect of the coracoacromial arch [20]. The coracoacromial arch includes not just the acromial undersurface, but also the coracoacromial ligament, and the undersurface of the acromioclavicular joint. Internal impingement is depicted to be contact or entrapment of the articular side of the supra or infraspinatus tendons with the posterior/superior glenoid labral complex in a position of glenohumeral abduction and external rotation [21]. Articular surface contact of the cuff with the glenoid labral complex can occur anteriorly and also superiorly [22]. Involvement of the subscapularis tendon between the coracoid process and lesser tuberosity of the humerus to cause for shoulder pain has also been identified as an impingement category, but few literatures are enlightening it. [23]
Intervention
The therapeutic interventions for shoulder impingement and rotator cuff disease vary, because it is determined by the individual patient subjective complaints and the objective evaluations. As per many studies revealed, the conservative treatment protocol and meticulous rehabilitation based on biomechanical evaluation is important for effective results in the long run of pain free functional activities of individual patient approach. Majority of the patients have shoulder pain with painful restriction of the range of motion of the shoulders and thus boundaries in activities of daily living. Brox, et al. who carried out study to conclude that exercise supervised by a physical therapist was superior to placebo and was as effective as a surgical subacromial decompression with postoperative rehabilitation in the treatment of patients with stage I primary impingement [24]. This recent randomize controlled study reported better ROM, reduce pain, and improving functional abilities in patients with shoulder pain. These patients received an individualized physical therapy program consisting of muscle stretching, strengthening, and retraining. Physical therapists have advocated the use of passive joint mobilization, soft tissue mobilization, and muscle stretching as an effective means of treating shoulder dysfunction. Passive joint mobilization is considered to be an effective treatment for enhancing ROM in the patient with shoulder impingement. Brier reported significant improvement with passive shoulder abduction in patients with adhesive capsulitis who received joint mobilization combined with active exercise [25]. The influence of thoracic spine mobility and curvature on shoulder ROM and scapular position the prevalence of significant forward head posture in subjects with shoulder overuse injuries and increased lateral rotation of the shoulder following joint mobilization to the cervical spine in patients with suspected capsular contractures of the glenohumeral joint are examples of the interdependence among joints in the shoulder girdle. The complexity of joint function in the shoulder may require treatment of shoulder impingement to extend beyond the glenohumeral and subacromial joints. Bang’s reported the purpose of our investigation was to compare the effectiveness of physical therapy treatment approaches to shoulder impingement syndrome a shoulder exercise program supervised by a physiotherapist and a shoulder exercise program supervised by a physical therapist combined with manual physical therapy to the upper quarter [26]. In a study carried out by Myers, the success rate of conservative management in patients with impingement syndrome was 73.8% regardless of the acromial morphology present. If the patient remains significantly disabled and has no improvement after conservative treatment, surgical treatment may be considered. Early therapeutic goals include the reduction of the inflammation and pain. Cryotherapy is particularly beneficial during the acute inflammatory stage or chronic recurrent exacerbation. Stretching and strengthening of the rotator cuff muscles shoulder should be performed while avoiding the impingement positions and once pain and inflammation have reduced, active and passive ROM exercise should be incorporated with gentle oscillation and mobilization [27]. One recent study shows, for the first time, that adducting muscle forces lead to a significant increase of subacromial space width compared with abducting muscle activity. Thus, future physical therapy protocols should focus on increasing the depressor effect of adducting muscles in the postoperative and conservative treatment of impingement syndrome of the shoulder. This early rehabilitative activity allows for neurological reintegration of neuromuscular structures [28].
Prognosis
The rehabilitation of the shoulder must follow a comprehensive approach. In analysis of the bio mechanical collected works revealed that glenohumeral motion and scapulothoracic rotation must occur simultaneously. This synchronized movement establishes the scapulohumeral rhythm. This movement occurs in conjunction with sufficient mobility of the acromioclavical and sternoclavicular joints. The combined movements of the glenohumeral, scapulothoracic, acromioclavical, and sternoclavicular, can only be accomplished by a dynamic combination of muscle function, periarticular flexibility, stability, and proper arthrokinematics. The study has demonstrated that muscle and joint tissues both contribute to the total joint stiffness [29]. There is no evidence that the changes in one are more dominant concealing the changes in the other. Therefore, the therapist must treat all aspects of joint stiffness it is important to incorporate mobilization, strengthening and stretching exercises, and pain releasing electro physical agents into the rehabilitation program of a stiff and painful shoulder [30].
Conclusion
Conservative treatments are acclaimed by number of authors for subacromial impingement syndrome associated with rotator cuff dysfunction. However many findings of these various conditions overlap, therefore accurate diagnosis and analyzing individual biomechanics lead to design effective rehabilitation regimen which is emphasized range of motion, joint mobilization and muscular imbalance therapy to consistency of ideal scapular thoracic rhythm to prevent the possibility of evolving adhesive capsulitis. Physiotherapy interventions will remain to have a vital role in treating patients with shoulder pain to recovery of pain free functional capability in day to day livings and recreational life.
Abbreviations
VAS – Visual Analog Scale
DASH - Disabilities of the Arm, Shoulder and Hand
ROM – Range of Motion
SAIS – Subacromial Impingement Syndrome
RC – Rotator Cuff
References
- Morrison Ds, Frogameni AD, Woodworth P (1997) Non-operative treatment of subacromial impingement syndrome. J Bone Joint Surg Am 79:732-737. [Crossref]
- Lin JC, Weintraub N, Aragaki DR (2008) Nonsurgical Treatment for rotator cuff injury in the elderly. J Am Med Dir Assoc 9: 626-632. [Crossref]
- Neer CS 2nd (1972) Anterior acromioplasty for chronic impingement syndrome in the shoulder: A preliminary report. J Bone Joint Surg 54: 41-50. [Crossref]
- Cofeild RH (1985) Rotator cuff disease of the shoulder. J Bone Joint Surg 67: 974-979. [Crossref]
- Breazeale NM, Craig EV (1997) Partial-thickness rotator cuff tears pathogenesis and treatment. Orthop Clin of N Am 28: 145-155. [Crossref]
2021 Copyright OAT. All rights reserv
- Soslowsky LJ, Carpenter JE, Bucchieri JS, Flatow EL (1997) Biomechanics of the rotator cuff. Orthop Clin of N Am 28: 17-30. [Crossref]
- Miniaci A, Salonen D (1997) Rotator cuff evaluation: Imaging and diagnosis. Orthop Clin of N Am 28: 43-58. [Crossref]
- Cyriax J (1975) Diagnosis of Soft Tissue Lesions. Baltimore: Williams and Wilkins, Textbook of Orthopaedic Medicine 180-228.
- Barr KP (2004) Rotator cuff disease. Phys Med Rehab Clin N Am 15: 475-491. [Crossref]
- Werner DS, Macnab I (1970) Superior migration of the humeral head: a radiological aid in the diagnosis of tears of the rotator cuff. J Bone Joint Surg 52:524-527. [Crossref]
- Ludewig PM, Phadke V, Braman JP, Hassett DR, Cieminski CJ, et al. (2009) Motion of the shoulder complex during multiplanar humeral elevation. J Bone Joint Surg Am 91: 378–389. [Crossref]
- Lucas D (1973) Biomechanics of the shoulder joint. Arch Surg 107:425- 432. [Crossref]
- Clark JM, Harryman DT (1992) Tendons, ligaments, and capsule of the rotator cuff: Gross and microscopic anatomy. J Bone Joint Surg 74: 713-725. [Crossref]
- Kent BE (1971) Functional anatomy of the shoulder complex, a review. Phys Ther 51: 867-887. [Crossref]
- Warwick R, Williams P (1973) Gray's Anatomy, 35th British Ed. Philadelphia: WB Saunders Co, 399-407.
- Sarrafian SK (1983) Gross and functional anatomy of the shoulder. Clin Orthop Relat Res 19: 173. [CrossRef]
- Kapanji IA (1970) Upper Limb. New York: Churchill Livingstone, The Physiology of the Joints 24-76.
- Evans PJ, Maniac A (1997) Rotator cuff tendinopathy: many causes, many solutions. J Musculo Med 14: 47-61.
- Edelson Gm Teitz C (2000) Internal impingement in the shoulder. J Shoulder Elb Surg 9: 308-315.
- Paley KJ, Jobe FW, Pink MM, Kvitne RS, ElAttrache NS (2000) Arthroscopic findings in the overhand throwing athlete: Evidence for posterior internal impingement of the rotator cuff. Arthroscopy 16: 35–40. [Crossref]
- Saha AK (1983) Mechanism of shoulder movements and a plea for the recognition of "zero position" of glenohumeral joint. Indian J Surg 12: 153-165. [Crossref]
- Poppen NK, Walker PS (1976) Normal and abnormal motion of the shoulder. J Bone Joint Surg Am 58: 195-201. [Crossref]
- Okroro T, Reddy VR, Pimpelnarkar A (2009) Coracoid impingement syndrome: A literature review. Curr Rev Musculoskelet Med 2: 51–55. [Crossref]
- Brox I, Staff PHI Ljunggren AE, Brevik JI (1993) Arthroscopic surgery compared with supervised exercises in patients with rotator cuff disease (stage II impingement syndrome). Br Med J 307: 899-903. [Crossref]
- Brier SR (1992) Rotator cuff disease: current trends in orthopaedic management. J Manipulative Physiol Ther 15: 123-128. [Crossref]
- Bang MD, Deyle GD (2000) Comparison of supervised exercises with and without manual physical therapy for patients with shoulder impingement syndrome. J Orthop Sports Phys Ther 30: 126-137. [CrossRef]
- Myers JB (1999) Conservative management of impingement syndrome in the athletic population. J Sports Rehab 8: 230-254.
- Breazeale NM, Craig EV (1997) Partial-thickness rotator cuff tears pathogenesis and treatment. Orthop Clin North Am 28: 145-155. [Crossref]
- Wirth MA, Basamania C, Rockwood CA (1997) Nonoperative management of full-thickness tears of the rotator cuff. Orthop Clin of North Am 28: 59-67. [Crossref]
- Shrode LW (1994) Treating shoulder impingement using supraspinatus synchronization exercise. J Manipulative Physiol Ther 17: 43-53. [Crossref]


