Aims: Stercoral perforation is a relatively rare life-threatening condition. The aim of this study was to investigate and compare the clinical characteristics and outcomes of patients with stercoral colonic perforation and patients with perforated colonic diverticulum.
Methods and results: This retrospective cohort study analyzed data via chart reviews from patients who received treatment at our institution between 1989 and 2018. Patients were divided into the stercoral colon perforation group (stercoral, 20 patients, 13.5%) and perforated colonic diverticulum group (diverticulum group, 40 patients, 27%). There were no significant differences in patient background information between the groups. Patients in both groups had a high rate of chronic constipation (80% vs. 53%). The final diagnosis was confirmed by CT scan in over 80% of all patients and the most common site of perforation was the sigmoid colon in both groups (80% vs. 90%, respectively). The most performed surgical procedure in both groups was the Hartmann procedure, and the implementation of planned second-stage surgery was significantly higher in the stercoral group (40% vs. 13%, respectively, p=0.04) than the diverticulum group. Although no significant differences in the postoperative mortality rates (20% vs 15% respectively, p=0.9), the duration of hospital stay was significantly longer in the stercoral group (60.2 days vs. 36.6 days, respectively, p < 0.05).
Conclusion: In the increasingly aging population, stercoral perforation should be suspected in elderly and chronically constipated patients with unexplained abdominal pain, although stercoral colonic perforation and perforated colonic diverticulum showed no significant differences in clinical characteristics or treatment outcomes in our study. Prompt diagnosis and optimal surgical intervention should be warranted to overcome this perilous pathology.
stercoral perforation, perforated colonic diverticulum, hartman’s procedure, open abdominal management, mortality
Stercoral colon perforation is defined as a perforation caused by compression necrosis of the intestinal wall due to stagnant feces or fecal stones in the large intestine. The condition is common in elderly patients who tend to be constipated [1]. This is a relatively rare disease; therefore, few case reports and review articles describing this condition are available [1-6]. It is difficult to determine the precise incidence of this condition. However, stercoral perforation is potentially life-threatening with an overall postoperative mortality rate of 35–50% mainly due to a high level of intra-peritoneal contamination, delayed diagnosis, and inappropriate surgical intervention [1,5,6]. Until 1990, only 11% of cases were correctly diagnosed before surgery because of nonspecific vague symptoms, especially in elderly patients [5]. A current meta-analysis revealed that 90% of cases were diagnosed by computerized tomography (CT) scan preoperatively. As such, clinical suspicion and early CT scan became the primary method of early diagnosis and led to improvement in the survival rate [6]. In addition, colonic free perforation itself leads to severe peritonitis and septic multi-organ failure and requires emergency laparotomy regardless of etiology [7]. To our knowledge, there have been no studies reporting clinical differences between stercoral perforation and other etiologies (especially the most frequent etiology of diverticula perforation) within colon perforation. The purpose of this study was to investigate and compare the clinical characteristics and treatment outcomes of patients with stercoral colonic perforation and patients with perforated colonic diverticulum who underwent surgical treatment at our facility.
Using data from chart reviews, we conducted a retrospective cohort study from patients who underwent surgical treatment at our hospital between 1989 and 2018. We initially reviewed all patients with chart-documented colon perforation. Those with colon perforation treated by non-operative therapy were excluded. A total of 148 patients with colonic perforation underwent surgical treatment at our facility during this period. We further excluded those patients with perforation caused by trauma, foreign body, malignancy, bowel obstruction, ischemic colitis, inflammatory bowel disease, and iatrogenic procedures. Finally, patients with idiopathic colon perforations were excluded by intraoperative and pathological findings.8,9 For this study, we used diagnostic criteria by Huttunen et al., in which stercoral conic perforation is defined as a condition that satisfies the following criteria: “sudden abdominal pain that develops during defecation,” “rounded colonic perforation with no other clear cause,” “the presence of hard stools in the abdominal cavity or intestine,” and “the exclusion of colonic diverticulosis.”1
This search was narrowed to identify two subsets of patients: 20 stercoral colon perforation (stercoral group, 13.5%) and 40 perforated colonic diverticulum (diverticulum group, 27%). Standard demographic and descriptive data were collected for all patients including age, sex, underlying disease (cerebrovascular disease, cardiovascular disease, respiratory disease, liver disease, acute/chronic renal failure, diabetes, psychiatric disease, steroid, and immunosuppressant usage), history of constipation, abdominal pain at defecation, vital signs on admission, physical examination on admission, diagnostic modalities and results, timing and findings of operations, type of operation, postoperative management, postoperative complications, hospital length of stay, and cause of death, if applicable. The study population was stratified according to etiology (stercoral group and diverticulum group). Clinical characteristics, operative management, and outcomes were compared. Statistical analysis was performed using unpaired Student’s t-test to compare means, and chi-squared analysis was used to compare proportions. A comparison was declared to be statistically significant if the p-value was <0.05.
Patient backgrounds of both groups are shown in Table 1. The patients in the stercoral group had a higher average age (72.8 vs. 69 years, respectively) and a higher number of female patients (75% vs. 58%, respectively). These differences were not significant. Regarding underlying diseases, the number of patients on dialysis was higher (25% vs. 10%, respectively) in the stercoral group; however, the difference was not significant. In addition, there was no significant difference in the number of steroid and immunosuppressant users between the two groups. Chronic constipation was recognized in 80% of patients in the stercoral group and 53% in the diverticulum group, a nonsignificant difference. Abdominal pain during defecation was recognized in 75% of patients in the stercoral group, and 23% of those in the diverticulum group. The final diagnosis was confirmed by abdominal CT scan in over 80% of all patients and the most common site of perforation was the sigmoid colon in both groups (80% vs. 90%, respectively).
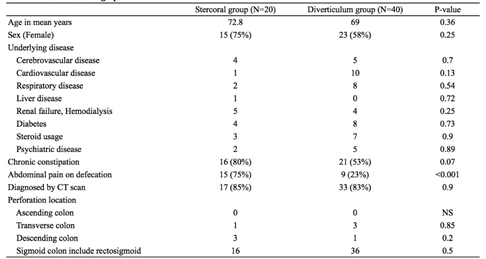
Table 1. Patient demographics
The surgical procedures performed in both groups are shown in Table 2. The most commonly performed procedure in both groups was the Hartmann procedure, which was performed on approximately half the patients. Meanwhile, exteriorization, simple suture closures, and temporary ileostomy were performed in the diverticulum group, but they were rarely performed in the stercoral group. Furthermore, we only performed a resection of the causative lesion, intraperitoneal lavage, and drainage during the initial surgery in patients with unstable intraoperative vital signs and colonic perforation with significant intraperitoneal contamination. These patients underwent “planned second-stage surgery” [10-12]. involving multiple intraperitoneal lavages or colostomy depending on their general condition. The implementation of this repeated surgery was significantly higher in the stercoral group (40% vs. 13%, respectively, p=0.04).

Table 2. Surgical procedures
The characteristics of postoperative management are shown in Table 3. All patients in the stercoral group required postoperative ICU management, with 75% of patients needing postoperative intubation. The sequential organ failure assessment (SOFA) score 24 hours after surgery was significantly higher in the stercoral group (6.6 vs. 4.5, respectively, p<0.05). However, there was no difference between the two groups in the use of vasopressor agents and those requiring postoperative dialysis or endotoxin absorption therapy. The treatment outcomes are shown in Table 4. The incidence of complications related to infection such as postoperative wound infection and intraperitoneal abscesses was similar (around 50%) in both groups. No significant differences in the postoperative mortality rates were observed between the two groups (20% and 15% in the stercoral and diverticulum groups, respectively), but the duration of hospital stay was significantly longer in the stercoral group (60.2 days vs. 36.6 days, respectively, p<0.05).

Table 3. Characteristics of postoperative management

Table 4. Postoperative outcomes
In this study, we recognized clinical features of stercoral perforation and found that stercoral colonic perforation and perforated colonic diverticulum showed no significant differences in terms of clinical characteristics or treatment outcomes.
Huttunen et al. defined stercoral colonic perforation as a “perforation that occurred due to compression necrosis of the intestinal wall due to hard stools or fecal stones [1].” The existence of tumors or diverticula that are generally thought to be the cause of the perforation cannot be confirmed. Instead, hard stools are observed in the large intestine with relatively large circular or elliptical perforations. Histological findings include compression necrosis of the mucosa near the perforation site, and the loss, non-thinning, and inflammation of the muscular layer [1,5]. Idiopathic colonic perforation is a differential diagnosis with many similarities to other diagnoses, and preoperative diagnosis is difficult [8,9]. However, stercoral colonic perforations are either circular or elliptical, while idiopathic colonic perforations are slit-like. Furthermore, based on the intraoperative and postoperative pathological findings, the latter reveals a histologically milder inflammation and a normal perforation perimeter, allowing for differentiation from the former [1,5]. Only those patients in whom the above-mentioned diagnostic criteria were met and where differentiation from idiopathic colonic perforation was possible were used as subjects in this study.
Regarding the background of the patients, most patients with stercoral perforation show a tendency for constipation including patients of older age, females, those on dialysis, and those who are bedridden for long periods of time [1-6]. Similar tendencies were observed among the patients of the stercoral group in this study, but there were no significant differences in the patient background between the two groups. In other words, these risk factors could also result in a perforated colonic diverticulum. As described above, the main cause of stercoral perforation of the large intestines is compression necrosis; on the other hand, perforation of the diverticulum is caused by the inflammatory spread of diverticulitis [7]. Interestingly, there is no difference in patient backgrounds despite these completely different pathological conditions. However, it is reported that a chronic increase in intestinal pressure due to constipation is involved in the occurrence of diverticulum of the large intestines [13], which may be a reasonable result.
Abdominal CT scan is essential for the diagnosis of stercoral perforation [6], the final diagnosis was confirmed by abdominal CT scan in over 80% of all patients in our study. The CT findings of stercoral perforation include discontinuity of the bowel wall, presence of faecal material either protruding through the colonic wall or lying free within the peritoneal cavity, and extraluminal free air [14]. The sigmoid colon was the most common perforation site in both groups, which was in line with the findings of various reports [1,5,6,13,15]. It seems likely that the watershed region of blood supply on the antimesenteric border of the colon where anastomosis between the vasa recta longa is poor, may explain the stercoral mass exerting its greatest pressure necrosis at this site [5].
In our study, the Hartmann procedure was selected for both groups, which is considered a standard surgical procedure for the safe management of colonic perforation [5,6,16,17]. Furthermore, resection/anastomosis and temporary colostomy were performed only in the diverticulum group. This is because these procedures were only performed in patients with generalized purulent peritonitis (Hinchey class III perforations), not in patients with generalized fecal peritonitis (Hinchey class IV perforations) [17]. Additionally, as a consequence of this high level of intraperitoneal contamination, a significantly higher proportion of patients from the stercoral group were selected for a “planned second-stage surgery.” Planned second-stage surgery is the application of damage control concepts in traumatic surgery for severe peritonitis [10,11,12]. This method involves rapidly removing the source of infection during the initial surgery and implementing open abdominal management. Subsequently, 24–48 hours after the patient’s general condition has stabilized, a re-laparotomy is conducted, and the intraperitoneal lavage and other processes are repeated. Although this strategy has the advantages of early detection and elimination of persistent contamination or latent infection, it can also lead to unnecessary laparotomies in severely ill patients. Furthermore, there is no consensus on the effectiveness of re-laparotomy procedures [10,11]. In this study, only those patients with unstable intraoperative vital signs and those with significant intraperitoneal contamination were selected for this procedure. We considered the shortened duration of the initial surgery and the simplicity of the repeated intraperitoneal lavage as its main advantage. However, the efficacy of this method in improving the treatment outcomes is yet to be proven. Moreover, a second-staged surgery increases the chances of postoperative intubation and the duration of ICU management. Thus, the indications for a second surgery should be carefully evaluated, and it should be selectively performed so as not to become an easy “escape surgery.”
Finally, stercoral colonic perforation often occurs in older people with underlying diseases and can easily lead to multi-organ failure. Hence, the mortality rate was once reported to be around 50%, and the pathology was associated with an extremely poor prognosis [4]. However, current advances in diagnosis, surgery, and perioperative management have reduced the mortality rate to around 34% [5,6]. Our research revealed similar postoperative outcomes. Furthermore, no other report has described the mortality rate for each cause of perforation. It is worth noting that despite the small sample size, our study demonstrated that there was no difference in the mortality rates between the diverticulum and stercoral groups despite a higher level of intraperitoneal contamination in the stercoral group. Basically, stercoral perforation results in fecal peritonitis [1,5]. Alternatively, perforation of the diverticulum includes purulent peritonitis and fecal peritonitis [17]. Therefore, considering the degree of intra-abdominal contamination, stercoral perforation is highly contaminated presumably resulting in poorer prognosis; interestingly, that there is no difference in these prognoses. However, the rate of infection-related complications in the stercoral group was high at 50%, and the duration of hospitalization was prolonged due to these complications.
Several limitations of the present study warrant mention. First, there may be potential residual confounders owing to unavailable information in the dataset due to the retrospective nature of the study design. Second, our sample numbers are relatively small because of the infrequency of this disease. Finally, it may be very difficult to differentiate stercoral perforation from idiopathic colonic perforation completely despite our definition and differential diagnosis methods based on intraoperative and pathological findings. Therefore, future large multi-institutional prospective cohort studies must work towards further refining perioperative management techniques in addition to the previously described surgical procedures for stercoral perforation of the colon.
In this study, we recognized clinical features of stercoral perforation and found that stercoral colonic perforation and perforated colonic diverticulum showed no significant differences in terms of clinical characteristics or treatment outcomes. Moreover, the constipation-induced pathology predisposing to high mortality rates was similar between the two groups. For societies with a sizable aging population, it will become extremely important in the future to adequately recognize this perilous pathology and master its perioperative management as well as create awareness about the importance of preventing constipation in the elderly.
None.
Funding: The funding source had no role in the design, practice, or analysis of this study.
Conflict of interest: Authors declare no Conflict of Interest for this article.
Author contribution: Study conception and design: TM; Acquisition of data: MK, MI; Analysis and interpretation of data and Drafting of the manuscript: TM, TK; All authors read and approved the final manuscript.
- 1)Huttunen R, Heikkinen E, Larmi TKI (1975) Stercoraceous and idiopathic perforation of the colon. Surg Gynecol Obstet 140: 756-760. [Crossref]
- 2) Hakami M, Mosavy SH, Tadaiion A (1975) Stercoral perforation of the sigmoid colon. Report of two cases. Dis Colon Rectum 18: 512-513. [Crossref]
- 3) Lasser A, Conte M, Solitaire GB (1975) Stercoraceous perforation of the caecum. Report of two cases. Dis Colon Rectum 18: 410-412. [Crossref]
- 4)Shatila AH, Ackerman NB (1977) Stercoraceous ulcerations and perforations of the colon Report of cases and survey of the literature. Dis Colon Rectum 20: 524-527. [Crossref]
- 5) Serpell JW, Nichollus RJ (1990) Stercoral perforation of the colon. Br J Surg 77: 1325-1329.
- 6) Chakravartty A, Chang A, Nunoo-Mensah J (2013) A systematic review of stercoral perforation. Colorectal Dis 15:930-5. [Crossref]
- 7) Brown CV (2014) Small bowel and colon perforation. Surg Clin North Am 94: 471-475. [Crossref]
- 8)Lyon DC, Sheiner HJ (1969) Idiopathic rectosigmoid perforation. Surg Gynecol Obstet 128: 991-1000. [Crossref]
- 9)Kasahara Y, Matsumoto H, Umemura H, Shiraha S, Kuyama T (1981) Idiopathic perforation of the sigmoid colon in Japan. World J Surg 5: 125-130. [Crossref]
- 10) Van Goor H (2002) Interventional management of abdominal sepsis: when and how. Langenbecks Arcj Surg 387: 191-200.
- 11) Van Ruler O, Mahler CW, Boer KR, Reuland EA, Gooszen HG, Opmeer BC (2007) Comparison of on-demand vs planed relaparotomy strategy in patients with severe peritonitis: a randomized trial. JAMA 298: 865-872. [Crossref]
- 12) Kirkpatrick AW, Coccolini F, Ansaloni L, Roberts DJ, Tolonen M, McKee JL, et al. (2018) Closed or open after source control laparotomy for severe complicated intra-abdominal sepsis (the COOL trial): study protocol for randomized control trial. World J Emer Surg 13: 26. [Crossref]
- 13) Heise CP (2008) Epidemiology and pathogenesis of diverticular disease. J Gastrointest Surg 12: 1309-11. [Crossref]
- 14) Kumar P, Pearce O, Higginson A (2011) Imaging manifestations of fecal impaction and stercoral perforation. Clin Radiol 66: 83-88. [Crossref]
- 15) Ngyuen GC, Sam J, Anand N (2011) Epidemiological trends and geographic variation in hospital admissions for diverticulitis in the United States. World J Gastroenterol 17: 1600-1605. [Crossref]
- 16) Hughes ESR, Cutherbertson AM, Killingback MK (1983) Colorectal Surgery. Edinburgh: Churchill Livingstone.
- 17) Lumpkin ST, Chaumont N (2019) Management of freely perforated diverticulitis. Dis Colon Rectum 62: 1153-1156. [Crossref]




