Abstract
Autoimmune disorders are may be seen together with the other autoimmune diseases. However multiple autoimmune diseases are rare to be seen in a patient. Coeliac disease, systemic lupus erythematosus (SLE) and familial Mediterranean fever having (FMF) the common clinical symptoms, are the diseases that are related with severe inflammatory disorder. In this case, it is talked about a patient who was followed initially with coeliac and later was diagnosed with SLE and FMF. It is not reported in the literature before that these three diseases have been seen together.
Key words
coeliac disease, systemic lupus erythematosus, familial Mediterranean fever
Introduction
Coeliac disease (CD) also known as gluten enteropathy is immune-mediated inflammatory disease of the small intestine caused by gluten sensitivity in genetically predisposed people. The most common symptoms are chronic diarrhea, anorexia, weight loss, abdominal distention and pain. CD is diagnosed with positive serological tests and small bowel biopsy findings which they are intraepithelial lymphocyte, crypt hyperplasia, and villous atrophy. Systemic lupus erythematosus (SLE) is a chronic inflammatory disease of unknown cause that can affect each organ. Clinical manifestations of this disease is variable, it varies from mild joint and skin involvement to life-threatening renal, hematological, and central nervous system involvement. Familial Mediterranean fever (FMF) is autosome-recessive inherited disease, associated with failure of inflammation control in Mediterranean origin communities like Turkish, Jewish, Arab and Italians. This case is about a patient who followed by a coeliac disease and afterwards was diagnosed with the FMF and SLE. The association of these three diseases has not been published in the literature before.
Case
Fifteen years ago 28-year-old woman was admitted complaining of diarrhea, abdominal pain and weight loss. Iron-deficiency anemia and hypocalcemia was determined in her tests. The vitamin D levels were checked. Malabsorption etiology was investigated since the patient had low levels of vitamin D and iron deficiency anemia. Anti-gliadin IgA and anti-endomisium antibodies were positive. Patient was diagnosed with CD according to finding of the infiltration of intraepithelial lymphocytes, crypt hyperplasia and mild villous atrophy in small bowel biopsy and a gluten-free diet was started (Figure 1). After that the patient's complaints were regressed. The patient was admitted to our hospital with fever, abdominal pain, arthritis of hand joints (recurrent attacks, lasting between 1 and 3 days) and lesions on the face a year later. Physical examination revealed AT 110/65 mmHg and pulse 77/min. Cardiovascular system, respiratory and abdominal examinations were normal. Malar rash, discoid lesions on arms were observed. Complete blood count was: Hb 12.3 g/dL, Hct 40.6%, Wbc 4770/ mm, Lymphocite 980/mm, Plt 378 000, CRP 3.95 and ESR 81 (0-20). Urea 38 mg/dL (17-43), creatinine 0.91 mg/dL (0.67-1.17), total bilirubin 1.1 mg/dL (0.3-1.2), direct bilirubin 0.1 mg/dL (0.1-0.2), AST 32 U/L (5-50), ALT 16 U/L (5-50), ALP 92 U/L (30-120), GGT 26 U/L (10-55). There was no specific finding in urine microscopy. Immunological markers were: C3 0.73 (0.9-1.8), C4 0.145 (0.1-0.4), ANA 1/640, ASMA (+), anti-SM(+), anti-dsDNA 62.9 (0-20). The patient was diagnosed with SLE according to the 2012 SLICC SLE criteria and steroid and hydroxychloroquine therapy was initiated. According to the criteria developed by Tel-Hashomer the patient was diagnosed with FMF since m694v mutation was positive while analyzing the FMF gene homozygote mutation. Treatment was started with colchicine therapy. In this case follow-up as well as treatment is being continued.
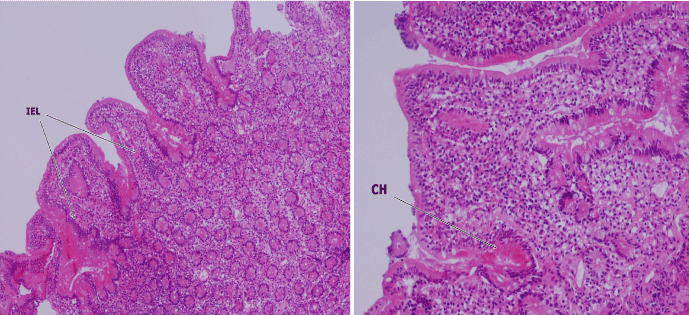
Figure 1. Infiltration of intraepithelial lymphocytes (IEL), lymphohistiositic infiltration of lamina propria, crypt hyperplasia (CH) and mild villous atrophy and rare eosinophils in small bowel biopsy.
Discussion
The diagnosis of SLE is based on a combination of clinical findings and laboratory evidence. Systemic Lupus International Collaborating Clinics (SLICC) group revised and validated the ACR SLE classification criteria in 2012; they classified a person as having SLE in the presence of biopsy-proven lupus nephritis with ANA or anti-dsDNA antibodies or if 4 of the diagnostic criteria, including at least 1 clinical and 1 immunologic criterion, have been satisfied [1]. Our patient had acute cutaneous lupus, arthritis, serositis and positive ANA, Anti-DNA antibodies. SLE may develop due to such drugs, like procainamide, hydralazine, quinidine, however we did not consider that it was developed as a result of the drugs since the patient did not take those pills and his anti-histone antibodies were negative.
The diagnosis of familial Mediterranean fever is based upon three factors: typical clinical manifestations, a positive response to colchicine therapy and genetic testing, although currently available tests do not detect all mutations associated with FMF [2]. Our patient had recurrent febrile episodes associated with peritonitis and synovitis, favorable response to daily colchicines and positive history of familial Mediterranean fever in a first degree relative. The diagnosis of coeliac disease based on typical gastrointestinal symptoms, such as weight loss, chronic diarrhea, abdominal distention and poor growth; atypical symptoms, such as dermatitis herpetiformis, iron deficiency anemia, osteoporosis; abnormal serological tests; abnormal intestinal biopsy findings; clinical improvement with gluten free diet [3]. Our patient had gastrointestinal symptoms, iron-deficiency anemia, positive anti-gliadin IgA and anti-endomysium antibody, finding of villus atrophy in small bowel biopsy and clinical improvement with gluten-free diet.
Clinical symptoms of FMF and SLE are seen as a result of autoimmune inflammation of serous membranes. FMF is an autosome-recessive disease characterized by fever and polyserositis. Gastrointestinal involvement is observed in 20-40% of patients and abdominal pain due to peritoneal inflammation, vasculitis, pancreatitis, malabsorption, pseudo-obstruction as well as paralytic ileus may occur too. Arthritis is the most common symptom in FMF attacks. Knees, ankles, and wrists are the joints most commonly affected. An arthritis that resembles seronegative spondyloarthritis may also occur. The most common musculoskeletal outcome of the SLE is the arthritis of the proximal interphalangeal (PIP) and metacarpophalangeal (MCP) joints of the hands. SLE and FMF occur together very rarely. Until now, 10 cases were reported of SLE and FMF association [4-6].
Coeliac disease may be associated with autoimmune diseases such as insulin-dependent DM, autoimmune thyroid disease. SLE and coeliac disease association is rare. HLA-B8 and HLA-DR3 may be seen in both diseases. Furthermore, there are publications which indicate the availability of transglutaminase antibodies in SLE and positive antidsdna antibodies in 23% cases in coeliac disease.
13 cases of SLE and coeliac disease association were reported in between 1966-2005 years in adult and children medical literature [7]. Diarrhea and weight loss is the most common symptoms in these cases. In a study of Tursi et al. [7] 57.14% of patients with coeliac disease represent with gastrointestinal complaints. 42.86% is silent/subclinical. Iron deficiency anemia is the most common extraintestinal symptoms in silent form. The study done by Hugh J 246 patients followed for 25 year and in 2.4% of these patients developed to SLE later. The study done by Utiyama et al. [8] in 8.9% of CD patients ANA will be positive. FMF and coeliac disease association is rare and the relationship has not been shown. A study completed by Kuloglu et al. [9] MEFV mutation was observed in 23% coeliac patients.
Conclusion
As a result, SLE and FMF are two different multisystem chronic inflammatory disorders that may be seen together and coeliac disease may accompany them. If the patient diagnosed one of these diseases, should be kept in mind other diseases can be seen in the same patient.
References
- Petri M, Orbai AM, 2021 Copyright OAT. All rights reservJT, et al. (2012) Derivation and validation of the Systemic Lupus International Collaborating Clinics classification criteria for systemic lupus erythematosus. Arthritis Rheum 64: 2677-2686. [Crossref]
- Berkun Y, Eisenstein EM (2014) Diagnostic criteria of familial Mediterranean fever. Autoimmun Rev 13: 388-390. [Crossref]
- Hopper AD, Hadjivassiliou M, Butt S, Sanders DS (2007) Adult coeliac disease. BMJ 335: 558-562. [Crossref]
- Lidar M, Zandman-Goddard G, Shinar Y, Zaks N, Livneh A, et al. (2008) Systemic lupus erythematosus and familial Mediterranean fever: a possible negative association between the two disease entities-report of four cases and review of the literature. Lupus 17: 663-669. [Crossref]
- Schreiber BE, Lachmann HJ, Mackworth-Young CG (2008) Possible familial Mediterranean fever in a Caucasian patient with systemic lupus erythematosus. Lupus 17: 752-753. [Crossref]
- Bakir F, Saaed B (1989) Systemic lupus erythematosus and periodic peritonitis (FMF). Br J Rheumatol 28: 81-82. [Crossref]
- Tursi A, Giorgetti G, Brandimarte G, Rubino E, Lombardi D, et al. (2001) Prevalence and clinical presentation of subclinical/silent celiac diseases in adults: an analysis on a 12 year observation. Hepato-gastroenterol 48: 462-464. [Crossref]
- da Rosa Utiyama SR, da Silva Kotze LM, Nisihara RM, Carvalho RF, de Carvalho EG, et al. (2001) Spectrum of autoantibodies in celiac patients and relatives. Dig Dis Sci 46: 2624-2630. [Crossref]
- Kuloglu Z, Ozçakar ZB, Kirsaçlioğlu C, Yüksel S, Kansu A, et al. (2008) Is there an association between familial Mediterranean fever and celiac disease? Clin Rheumatol 27: 1135-1139. [Crossref]

