Abstract
The case of a young child with duodenal heterotopia in the ileum is reported and the relevant Literature on the topic is briefly reviewed.
Key words
perforation, peritonitis, laparotomy, brunner’s glands
Introduction
"Heterotopia" refers to the presence of a particular tissue type at a non-anatomical site, usually co-existing with original tissue in its correct anatomical location [1,2]. In other words, it implies the presence of histologically normal tissue, but at an abnormal site, in addition to presence of the original tissue at its original site.
Gastrointestinal heterotopias are rare disorders which have been identified throughout the entire length of the gastrointestinal tract. Gastric and pancreatic heterotopia has been well documented at various sites in the gastrointestinal tract, with a reported incidence of 1- 13% [1]. Pancreatic heterotopia is mostly seen in the stomach, whereas combined (gastric and pancreatic) heterotopia is most commonly seen in the duodenum and jejunum. Involvement of other organs (esophagus, terminal ileum, Meckel’s diverticulum, colon, gallbladder, spleen, mesentery, liver, bile ducts, omentum and urinary bladder) is rare but has been previously reported [1,2].
Duodenal heterotopia is an extremely uncommon form of heterotopia. Despite an exhaustive search of available Literature, we could come across only a few reports of duodenal heterotopia [3-7]. We report a case of a young 8 year old girl who presented with peritonitis and was found to have duodenal heterotopia in the resected part of the ileum.
Case report
An 8 years old female presented to our emergency with abdominal pain and distension for 6 days. She was dehydrated, with signs of peritonitis on abdominal examination. Chest x-ray revealed the presence of free gas under the diaphragm, and after adequate resuscitation, she was taken up for exploratory laparotomy.
On opening the abdomen via midline, bilio-purulent fluid was drained. Further exploration revealed a small perforation of the ileum, approximately 50 cms proximal to the ileo-cecal junction. The part of the ileum around this was unhealthy. After a thorough lavage, resection of the unhealthy, perforation bearing segment of the ileum was performed and an end to end primary (ileo-ileal) anastomosis performed in two layers using polygalactin 000.
The postoperative period was uneventful and the child was discharged with advice to follow up in OPD. The histopathological examination of the resected ileum showed foci of heterotopic Brunner’s glands in the mucosa and submucosa (Figure 1) with a surprising diagnosis of duodenal heterotopia.
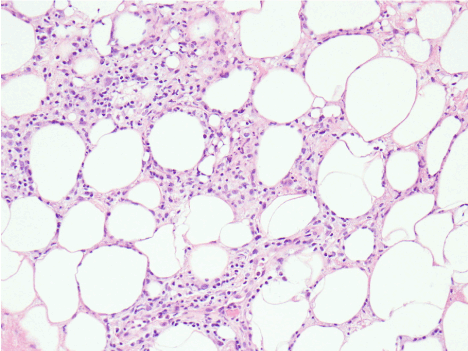
Figure 1. Photomicrograph of resected ileum showing foci of Brunner’s glands in muscularis mucosa and submucosa (H& E ×100)
Discussion
The aetiology of GI heterotopias remains incompletely understood; they are believed to be congenital, arising either due to abnormalities during rotation of the foregut or due to metaplasia [1,2].
The clinical presentation of GI heterotopia is variable, and depends on the nature of primary tissue, its size, location and associated complications. Gastric and pancreatic heterotopia usually becomes clinically symptomatic when they reach large size (more than 1 cm) or due to the sequelae of acid secretion and/ or polyp formation [1]. In cases where pancreatic and gastric heterotopias have been reported together, the clinical presentations result from a combination of these symptoms [1]. When heterotopic tissue causes intestinal inflammation or injury secondary to acid secretion, pancreatic enzyme activation and tissue digestion, patients present with symptoms like obstruction, intussusception and perforation [1,2].
Unfortunately, although gastric and pancreatic heterotopias are well documented, there is very little Literature available to comment on the significance of duodenal heterotopia and its presentations. In the earliest reported case that we could come across, duodenal heterotopia was diagnosed in a patient with pyloric obstruction secondary to gastric adenomyoma [3]. In another, duodenal heterotopia was diagnosed on histopathology in a patient suspected to be suffering from gastric malignancy [5]. By and large, the stomach has been the site, albeit infrequent, for heterotopic duodenal tissue, and other sites such as the ileum rare [3-8].
In our patient, the diagnosis of duodenal heterotopia was made by visualizing Brunner’s glands in the mucosa and submucosa of the ileum (Figure 1). In other reported cases of Brunner’s gland pathology (hyperplasia, hamartoma or adenoma), the disease is mostly confined to the duodenum, and occasionally to the stomach [3-8]. Presentation of these glands that are confined primarily to the submucosa of the proximal duodenum at other places in the GI tract is extremely uncommon, and to the best of our knowledge, has not been reported in the ileum before. In our patient, it is quite likely that duodenal heterotopia in the ileum was an incidental finding that was diagnosed only because she presented with ileal perforation. The clinical significance of this heterotopia is still not clear, but the patient remains on follow up to see how this unfolds as she grows up.
References
2021 Copyright OAT. All rights reserv
- De Castro Barbosa JJ, Dockerty MB, Waugh JM (1946) Pancreatic heterotopia; review of the literature and report Of 41 authenticated surgical cases, of which 25 were clinically significant. Surg Gynecol Obstet 82: 527-42. [Crossref]
- Al-Zahem A, Arbuckle S, Cohen R (2006) Combined ileal heterotopic pancreatic and gastric tissues causing ileocolic intussusception in an infant. Pediatr Surg Int 22: 297-9. [Crossref]
- Crossman LW, Kidder JH (1941) Adenomyoma of the Stomach. Heterotopia of Brunner’s Glands producing Pyloric Obstruction. Case Report. Am J Surg 54: 395-402.
- Scott HW, Payne TPB (1947) Diffuse Congenital Cystic Hyperplasia of the Stomach, Clinically Simulating Carcinoma. Bull Johns Hopkins Hosp 81: 448. [Crossref]
- Oberman HA, Lodmell JG, Sower ND (1963) Diffuse Heterotopic Cystic Malformation of the Stomach. N Engl J Med 269: 909-911. [CrossRef]
- Berant M, Aviad I, Jacobs J (1965) Heterotopic duodenal mucosa in the stomach. Am J Dis Child 110: 566-569. [CrossRef]
- Johnson CD, Bynum TE (1976) Brunner Gland Heterotopia presenting as Gastric Antral Polyps. Gastrointest Endosc 22: 210-11. [Crossref]
- Stolte M, Sticht T, Eidt S, Ebert D, Finkenzeller G (1994) Frequency, Location and Age and Sex Distribution of Various Types of Gastric Polyp. Endoscopy 26: 659-65. [Crossref]

