Background: Actinomyces is a rare cause of esophagitis with only a handful of cases documented in the literature. It should however be kept in the differential, especially in those that are immunocompromised.
Case: We are reporting a case of a 48-year-old diabetic male who presented with dysphagia, nausea, and vomiting. Imaging showed esophagitis and subsequent esophagogastroduodenoscopy confirmed severe Grade D esophagitis. Biopsies showed Actinomyces species. He responded well to therapy.
Conclusion: It is important to keep a wide differential for esophagitis in the immunocompromised population. A high index of suspicion and obtained biopsies in these settings are vital in preventing misdiagnosis and delays in therapy.
The Actinomyces species are anaerobic gram-positive bacteria unique for their branching filamentous bacilli organization. These bacteria are relatively rare amongst certain populations but can be found in normal human genitourinary, gastrointestinal, and oropharyngeal flora [1,2]. Due to their slow growing nature, they tend to manifest as chronic indolent infections with a relatively low virulence. However, they may present as clinically significant endogenous infections, commonly emerging as facial abscesses secondary to dental caries, cervicofacial suppurative infections or pelvic inflammatory disease secondary to the utilization of intrauterine devices [1,3]. The pathogenesis of these infections is commonly preceded by the disruption of regional tissue barriers by means of infection or instrumental damage [2]. The occurrence of Actinomyces infection involving the esophagus, however, is infrequent and commonly arises concomitant to immunosuppression [4]. The occurrence of Actinomyces esophagitis in immunocompetent patients is extremely rare [5]. Here we report a rare case of Actinomyces esophagitis in a patient with diabetes mellitus, highlighting the importance of keeping Actinomyces in the differential in the immunocompromised population.
A 48-year-old male with a past medical history of diabetes mellitus and hypertension presented to the emergency department due to nausea, vomiting and hyperglycemia. He was unable to tolerate any solid foods. He denied any episodes of hematemesis, hematochezia or melena but had reported bowel movements consisting of loose stools at home. On admission his vitals were stable. He was noted to have hyperglycemia (320 mg/dL), leukocytosis (15 thousand cells/uL) and anemia (11.4 g/dL). Physical exam was only significant for left costovertebral angle tenderness which, upon a further workup, was likely secondary to a urinary tract infection (UTI) along with acute on chronic kidney injury. The patient was then started on empiric intravenous antibiotics. A non-contrast CT of the abdomen and pelvis further demonstrated distal esophageal wall thickening prompting esophagogastroduodenoscopy (EGD) for further investigation.
Esophagogastroduodenoscopy demonstrated severe Grade D esophagitis from the mid esophagus to gastroesophageal junction. Biopsies were obtained due to the atypical appearance on endoscopy (Figure1). Biopsy of the stomach and duodenum were obtained as well but was otherwise unremarkable. Analysis of the esophageal biopsies displayed evidence of extensive acute inflammation with bacterial colonies morphologically consistent with Actinomyces (Figure 2). Following the procedure, the patient was placed on pantoprazole and sucralfate with Infectious Disease consultation recommending eight months of penicillin therapy. His dysphagia symptoms subsequently improved.
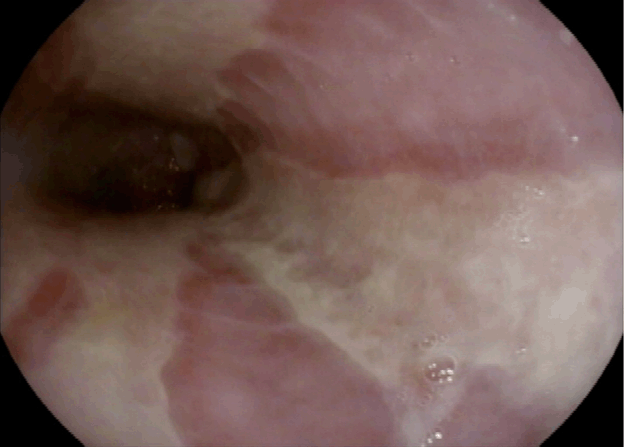
Figure 1. Endoscopic image illustrating severe esophagitis with longitudinal ulcerations extending from mid-esophagus to the gastroesophageal junction
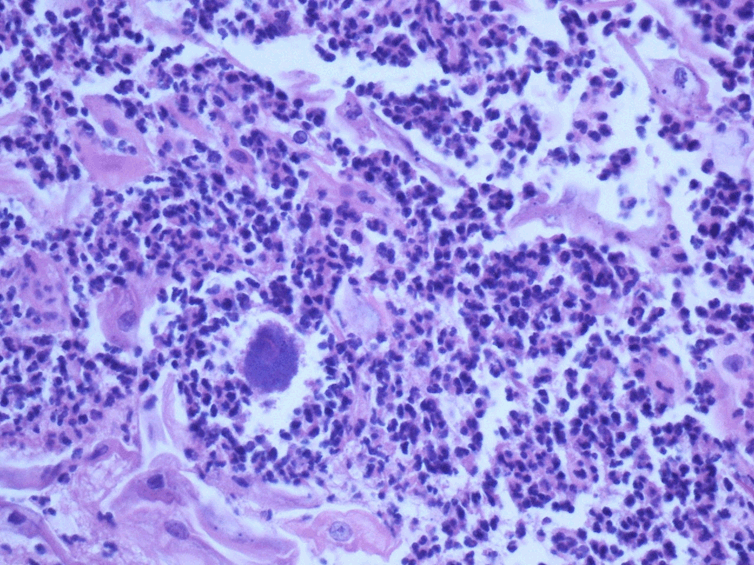
Figure 2. Histological examination showing Actinomyces colonies
Actinomyces esophagitis is a rare occurrence that has only been reported in less than 40 cases. Among these cases, less than half the number involved individuals who were immunocompetent. One trait, three of these cases share with our case is a history of diabetes [6-8]. Currently, the pathophysiology behind Actinomyces esophagitis remains unknown. While research has demonstrated tissue barrier disruption as a potential origin of infection, there was no clear history of such in this report. A case by Bella et al. reports a patient with esophageal dysmotility secondary to hiatal hernia as a plausible explanation for Actinomyces esophagitis [9]. The possibility of diabetic esophageal dysmotility predisposing diabetic patients to Actinomyces should be considered. Furthermore, esophagitis from acid reflux in patients with pre-existing hiatal hernia may predispose those that are already immunocompromised to develop Actinomyces infection.
Due to the scarcity of reported cases, the severity of Actinomyces esophagitis morbidity is also unknown. Esophagogastroduodenoscopy in this report identified severe Grade D esophagitis. However, other reports have also found Actinomyces esophagitis as a predisposing factor for the development of esophageal masses and strictures [7,10]. Due to the range of presenting morbidities, Actinomyces esophagitis mimics multiple pathologies including but not limited to, candida esophagitis and malignancy. Since this can mislead physicians, imaging and biopsy should be the gold standard for diagnosis and to rule out these differentials.
In conclusion, we report a rare case of Actinomyces esophagitis in a diabetic patient. The patient presented with severe esophagitis from the mid-esophagus to the gastroesophageal junction. Symptoms, imaging and endoscopic findings may be non-specific, and it is important to have a high degree of suspicion to biopsy in select populations to prevent misdiagnosis and delay in treatment.
- Li J, Li Y, Zhou Y, Wang C, Wu B, et al. (2018) Alimentary tract diseases: A review of its biological functions and pathology. Biomed Res Int 2018: 3820215.
- Wong VK, Turmezei TD, Weston VC (2011) Actinomycosis. BMJ 343: d6099.
- Westhoff C (2007) IUDs and colonization or infection with Actinomyces. Contraception 75(6 Suppl): S48-50.
- Valour F, Sénéchal A, Dupieux C, Karsenty J, Lustig S, et al. (2014) Actinomycosis: Etiology, clinical features, diagnosis, treatment, and management. Infect Drug Resist 7:183-197. [Crossref]
- Palmitessa V, Cuppone R, Monno R, Fumarola L, Lippolis A (2019) A case report of esophageal actinomycosis in an immunocompetent patient and review of the literature. New Microbiol 42: 55-60. [Crossref]
- Patel AL, Senuri L, Vania M, Khin Su, Schad A (2018) A rare case of invasive esophageal actinomyces in a patient with malabsorption. Am J Gastroenterol 113: S979-S980.
- Alshati A, Appleton L, Maddux JT, Almohammedawi M, Dangerfield B (2019) Esophageal actinomycosis presenting as an obstructive esophageal mass. ACG Case Rep J 6: e00140. [Crossref]
- Baig SNR, Sadia R, Daniel M, Deshpande V, Abdelsayed G, et al. (2019) Esophageal actinomycetoma masquerading as cancer in an immunocompetent patient. Am J Gastroenterol 114: S1018-S1019.
- Bella S, Saleem A, Shumeyko M (2018) Esophageal actinomyces in immunocompetent patient: That's unusual. Am J Gastroenterol 113: S998.
- Zhang AN, Guss D, Mohanty SR (2019) Esophageal stricture caused by actinomyces in a patient with no apparent predisposing factors. Case Rep Gastrointest Med 2019: 7182976. [Crossref]


