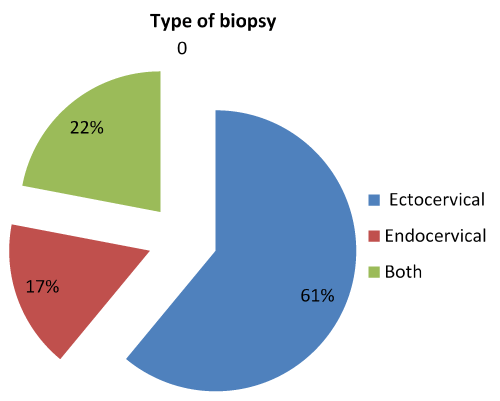Abstract
The management and follow-up of patients diagnosed with adenocarcinoma in situ (AIS) is challenging. First, complete resection is difficult and cannot be guaranteed even though resection margins are negative. Second, patients with positive margins and/or positive endocervical curettage and/or histological signs of invasive disease have a very high risk of invasive adenocarcinoma. Therefore, the optimal management of these patients remains uncertain. A 15-year retrospective study was performed of patients with AIS treated in the Unit of Gynecology of Miguel Servet University Hospital, Zaragoza, Spain. During this period, a total of 18 women were diagnosed with AIS. Initial treatment consisted of cervical conization in all patients. Histological examination of the hysterectomy specimen showed the presence of residual disease in 60% of patients with positive margins, whose treatment was completed with a hysterectomy. All patients with negative cone margins who did not receive any complementary therapy were closely monitored and currently remain disease-free.
Key words
atypical glandular cells, cervical glandular intraepithelial neoplasia, microinvasive adenocarcinoma, adenocarcinoma in situ
Abbreviations
AIS: Adenocarcinoma In situ; AGC: Atypical Glandular Cells; L-SIL: Low Grade Squamous Intraepithelial Lesion; H-SIL: High Grade Squamous Intraepithelial Lesion; ASCUS: Atypical Squamous Cells Of Undetermined Significance; HUMS: Miguel de Servet University Hospital; IACS: Aragon Institute of Health Sciences; LEEP: Loop Electrosurgical Excision Procedure
Introduction
Adenocarcinoma in situ (AIS) of the uterine cervix is a premalignant glandular condition. AIS is the only known precursor to cervical adenocarcinoma and, in many cases, invasive disease can be prevented with appropriate management [1]. The usual interval between clinically detectable adenocarcinoma in situ and early invasion is reportedly at least five years, which provides a wide scope for detection and intervention [2,3]. Glandular neoplasia in the uterine cervix is less common than squamous neoplasia, being the second most frequent histological type of lesion in the cervix. However, the incidence of adenocarcinoma in situ and invasive adenocarcinoma has increased in the last decades.
The optimal management of AIS of the uterine cervix after conservative treatment remains controversial [4]. Positive or close histopathological margins are associated with an increased risk of persistent and recurrent AIS, but whether hysterectomy should be performed as definitive treatment in margin-negative AIS remains uncertain [5-7]. To date, conflicting reports have been published regarding the rates of subsequent cervical neoplasia in these women. The main objective of this study was to evaluate the diagnostic techniques, therapeutic approaches and outcomes in patients with precursor cervical glandular lesions and endocervical adenocarcinoma in situ for a 15-year period.
Materials and methods
The study was performed in the Miguel de Servet University Hospital (HUMS), which is located in Zaragoza, the fifth largest city of Spain. HUMS is a third-level hospital serving a population of 530,510 people. It is also the reference hospital for gynecologic oncology of the Autonomous Community of Aragon. Aragon has a population of 1.277.471 inhabitants, which accounts for 2.85% of the Spanish population. The total population of Zaragoza is 917,288 (71% of the population of Aragon).
We conducted a retrospective review of patients diagnosed with AIS and treated in our hospital from January 2000 to December 2015. During the study period, a total of 18 women were diagnosed with AIS. The sample was extracted from the database of the Unit of Gynecologic Oncology, where all patients diagnosed with AIS from 2000 and treated in our Unit are registered. The clinical records of the patients included in the study were reviewed on a case-by-case basis upon request to the Service of Clinical Records.
The study included patients with cervical AIS confirmed either by initial or by cone biopsy (diathermy loop excision or cold knife). Records were reviewed for epidemiological and clinical data, diagnostic methods, therapeutical surgical procedures, and follow-up outcomes.
For statistical analysis, the data obtained were transcribed into a computerized database using the IBM Statistics Process Social Sciences 15.0 package for Windows (Copyright© SPSS Inc., 2006 license owned by the University of Zaragoza).
The level of statistical significance was set at p < 0.05.
Results
A total of 18 patients were diagnosed with AIS in our center. Notably, a significant increase was observed in the incidence of AIS in the last year of the study period (2015). Figure 1 shows the number of patients diagnosed with AIS annually. The mean age at diagnosis was 39 years, with a mode of 45 years and a 27 to 62 age range. Yet, most cases (61%) were detected in women aged 35 to 55 years. Age distribution of patients diagnosed with AIS during the study period is displayed in Figure 2.
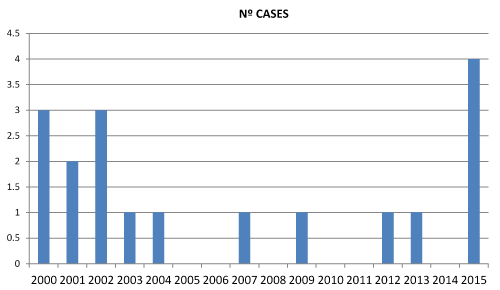
Figure 1. Evolution of the number of patients diagnosed with AIS treated in the HUMS during the study period.
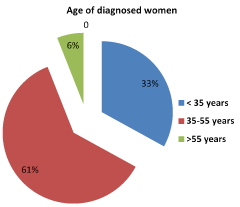
Figure 2. Age distribution of women diagnosed with AIS.
By country of origin, 17 patients (94.4%) were Spanish, whereas only a patient came from another country (5.6%).
A total of 17 patients (94.4%) were asymptomatic. In all cases AIS was confirmed following an abnormal cytological screening. Only a patient (5.6%) had clinical signs of AIS in the form of anomalous gynecological bleeding. The most common cytological findings include AGC (in half the patients) followed by H-SIL, L‑SIL and ASCUS. Figure 3 shows the cytological findings noted in the study patients.
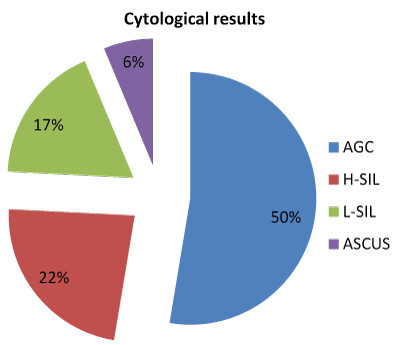
Figure 3. Citologycal results obtained in the study.
In all cases, diagnosis of AIS was confirmed histologically. Ectocervical tissue was sampled in 61% of cases, whereas endocervical and ectocervical tissue was collected in 39% of patients. The type of biopsy performed in each patient is detailed in Figure 4. Once AIS was histologically confirmed, a loop electrosurgical excision procedure (LEEP) was performed in all patients. Histopathological findings included HSIL-associated AIS in 10 patients (55.5%) and AIS alone in 8 patients (44.5%).
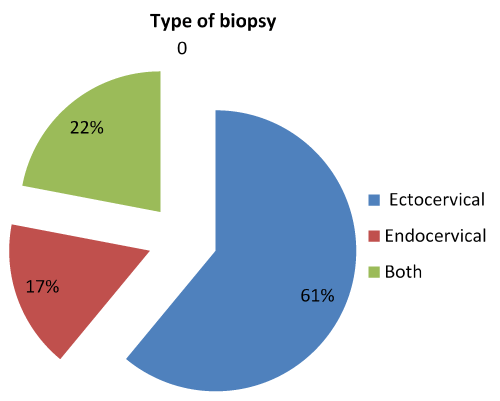
Figure 4. Type of biopsy performed for the diagnosis of AIS.
2021 Copyright OAT. All rights reserv
In most cases, cone margins were negative and only five patients (28%) had positive margins. Four of the five patients with positive margins underwent surgery. A patient had a LEEP, whereas the other three patients underwent a hysterectomy, as preserving fertility was not required (they already had children). One of the five patients with positive cone margins decided not to undergo any surgery as she wanted to become pregnant within the following months. The patient was aware of the risk that this decision entailed for her health.
Sixty percent of patients reoperated for positive cone margins had residual disease (cervical adenocarcinoma in situ). Seven of the 13 patients with free margins underwent a hysterectomy, with no residual disease. The remaining patients were closely monitored and have remained disease-free so far. Only a patient died for a cause other than cervical disease (heart disease). To date, the mean duration of follow-up has been five years (60 months), with a minimum of five months for the most recent case, and a maximum of 14.5 years (174 months) for the earliest case.
Discussion
Although the incidence of precursor cervical glandular lesions was low in the past, it is progressively increasing and occurring at an earlier age.
Special attention should be paid during screening to improve the detection of these lesions, as they are precursors to invasive endocervical adenocarcinoma, and cervical cancer screening programs have been ineffective in reducing the incidence of these lesions [8]. As this disease usually remains asymptomatic –as confirmed in our series–, it is not until abnormal cytological, clinical, or colposcopic findings suggestive of squamous cell and glandular cell carcinoma are noted that diagnosis is made.
On average, the onset of AIS occurs 13 years earlier than invasive adenocarcinoma, which is confirmed by the young mean age of the patients in our series. This is an alarming sign that AIS –and, consequently, invasive adenocarcinoma– is occurring at an increasingly younger age [9,10]. Following a diagnosis of AIS, women who want to preserve their fertility can opt for a conservative approach. Yet, it is important that these patients are aware of the potential risk for residual or recurrent cervical neoplasia, as positive or positive-close histopathological margins are associated with an increased risk of disease recurrence. However, the risk associated with histologically negative margins is less clear, as conflicting results have been reported in previous studies. It is worth noting that these studies are limited by their single-center design or the small samples employed [11].
In our series, patients younger than 35 years accounted for 33% of the sample. In Spain, many women of this age have not had any children yet and a fertility-conserving approach is of paramount importance to them. However, AIS can only be managed conservatively if patient's safety is ensured, which requires an early and accurate diagnosis.
Complete response can only be achieved by excision followed or not by a hysterectomy. In the long term, only persistent HPV and/or the associated immunosuppression can induce the invasion of other epithelia of the lower genital tract and cause a vaginal intraepithelial neoplasia (VAIN), which only occurred in two patients in our series.
Predictors of residual disease after conization have not been determined yet. Inconsistent results have been reported about the association between positive cone margins and/or positive endocervical curettage and a higher rate of residual disease Negative cone margins are correlated with the absence of residual disease, which enables a conservative approach in women of childbearing age who want to preserve their fertility [12].
Few case series studies have been performed to determine the clinical or histological features that enable that hysterectomy is delayed safely. The same occurs with the duration of the watchful waiting period. The influence of the waiting period in the risk of recurrence or progression to invasive adenocarcinoma has not been well established yet. Therefore, further studies are required to investigate whether AIS requires hysterectomy in all cases or a conservative approach based on watchful waiting is safe. The optimal management of AIS can only be determined based on objective statistical data provided by further studies [13].
All efforts should be channeled to find out for how long a conservative approach can be maintained without this entailing an increased risk of progression to invasive disease [14].
Acknowledgements
This work was supported by the IACS, the Aragon Institute of Health Sciences and Source of FEDER co-financing. Thank you for your support for our research group, Gynecology Oncology of the Miguel Servet Hospital.
References
- DeSimone CP, Day ME, Dietrich CS, Tovar MM, Modesitt SC (2011) Risk for residual adenocarcinoma in situ or cervical adenocarcinoma in women undergoing loop electrosurgical excision procedure/conization for adenocarcinoma in situ. J Reprod Med 56: 376-80. [Crossref]
- Wang J, Andrae B, Sundström K, Ström P, Ploner A, et al. (2016) Risk of invasive cervical cancer after typical glandular cells in cervical screening: nationwide cohort study. BMJ 352: 276.
- Booth BB, Petersen LK (2014) Can adenocarcinoma in situ of the uterine cervix can be treated safely by conisation in combination with endocervical curettage? Eur J Gynaecol Oncol 35: 683-687. [Crossref]
- Baalvergen A, Molijn AC, Quint WG, Smedts F, Helmerhorst TJ (2015) Conservative treatment seems the best choice in adenocarcinoma in situ of the cervix uterine. J Low Genit Tract Dis 19: 239-243. [Crossref]
- Adhya AK, Mahesha V, Srinivasan R, Nijhawan R, Rajwanshi A, et al. (2009) Atypical glandular cells in cervical smears: histological correlation and a suggested plan of management based on age of the patient in a low-resource setting. Cytopathology 20: 375‐379. [Crossref]
- Song T, Lee YY, Choi CH, Kim TJ, Lee JW, et al. (2015) The effect of coexisting squamous cell lesions on prognosis in patients with cervical adenocarcinoma in situ. Eur J Obstet Gynecol Repro Biol 190: 26-30. [Crossref]
- Diaz ES, Aoyama C, Baquing MA, Beavis A, Silva E, et al. (2014) Predictors of residual carcinoma or carcinoma in situ at hysterectomy following cervical conization with positive margins. Gynecol Oncol 132: 76‐80. [Crossref]
- Sehnal B, Driák D, Cibula D, Halaska M, Bolehovská P, et al. (2014) Tailoring surgical treatment of cervical precancerosis. Ceska Gynekol 79: 372-377. [Crossref]
- Wilbur DC (2016) Practical issues related to uterine pathology: in situ and invasive cervical glandular lesions and their benign mimics: emphasis oncytology-histology correlation and interpretive pitfalls. Mod Pathol 29(S1-S11). [Crossref]
- Cohen PA, Brand A, Sykes P, Wrede DCH, McNally O, et al. (2017) Excisional treatment in women with cervical adenocarcinoma in situ (AIS): a prospective randomised controlled noninferiority trial to compare AIS persistence/recurrence after loop electrosurgical excision procedure with cold knife cone biopsy: protocol for a pilot study. BMJ Open 7: e017576. [Crossref]
- Munro A, Codde J, Spilsbury K, Stewart CJR, Steel N, et al. (2017) Risk of persistent or recurrent neoplasia in conservatively treated women with cervical adenocarcinoma in situ with negative histological margins. Acta Obstet Gynecol Scand 96: 432-437. [Crossref]
- Costales AB, Milbourne AM, Rhodes HE, Munsell MF, Wallbillich JJ, et al. (2013) Risk of residual disease and invasive carcinoma in women treated for adenocarcinoma in situ of the cervix. Gynecol Oncol 129: 513-516. [Crossref]
- Massad LS, Einstein MH, Huh WK, Katki HA, Kinney WK, et al. (2013) 2012 updated consensus guidelines for the management of abnormal cervical cancer screening tests and cancer precursors. Obstet Gynecol 121: 829-846.
- Taylor JS, Panico V, Caputo T, Gerber D, Gupta D, et al. (2014) Clinical outcomes of patients with adenocarcinoma in situ of the cervix treated by conization. Eur J Gynaecol Oncol 35: 641-645. [Crossref]