splenic artery rupture, ECMO, TRALI, pregnancy
A 29-year old woman was admitted to hospital for acute pancreatitis (Balthazar grade A) at 38 weeks of her second pregnancy (gravida 2 para 1). One day before planned caesarean section at 39+1 week, she collapsed in shower bath. Due to profound hypotension, she was rushed to the operating theatre where alive but severely asphyxiated infant (2,900 g) was delivered. Large pools of clotted and fresh blood were found in abdominal cavity, deteriorated blood pressure required catecholamine support (norepinephrine 0.18-0.27 µg/kg/min) and massive transfusion protocol was applied because of profound blood loss within surgical exploration. Bleeding originated from ruptured splenic artery aneurysm which was uneasily controlled by its ligation and fibrin sealant patch (Figure 1) [1]. She received a total of 40 units of packed red blood cells, 32 units of fresh frozen plasma, 24 units of platelets, 12 g of fibrinogen, 4500 units of prothrombin complex, and 540 µg of recombinant f VIIa (90 µg/kg). Within 4 hours after surgery, severe respiratory failure developed under the picture of non-cardiac pulmonary oedema (transfusion-related acute lung injury) with drop of hypoxemic index (PaO2/FiO2) to 56.3 mm Hg despite aggressive mechanical ventilation and recruitment trials (Figure 2a). She was put on veno-venous extracorporeal membrane oxygenation (femoro-jugular) and successfully weaned off 60 hours later (Figure 2b) [2,3]. Being awaken with no neurological sequelae, she was extubated 5 days after the surgery and discharged home 26th post-operative day (Figure 2c). One year after the surgery, she is well and looks after her baby presenting with moderate psychomotor disability. She denied interventional closure (coiling) of ecstatic proximal part of splenic artery preventing the risk of its rupture (Figure 1).
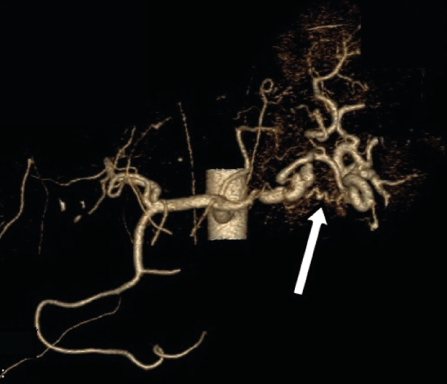
Figure 1. Post-operative CT reconstruction of dysplastic splenic artery with “a gap” where aneurysm was surgically ligated (arrow)
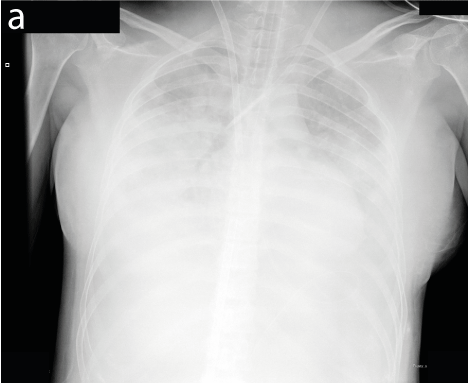
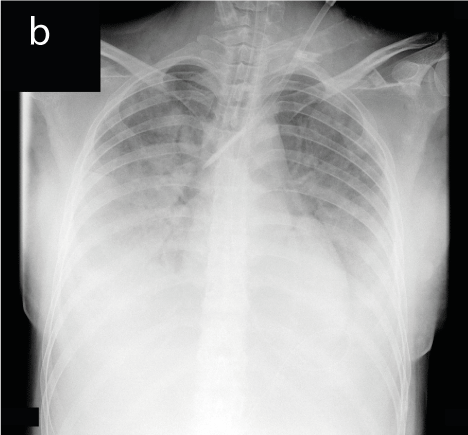
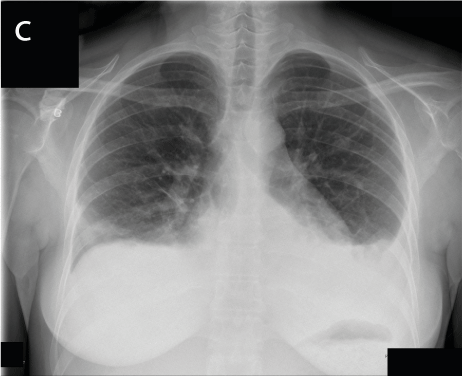
Figure 2. a-c. Chest x-ray shows bilateral patchy infiltrates “white out” of non-cardiac pulmonary oedema (a), partial resolution of oedema after 60 hours of ECMO support (femoro-jugular cannulation) allowing extracorporeal support weaning (b), complete resolution at the time of discharge (c)
Authors declared obtaining of patient consent for publication of the case.
Supported by MH CZ – DRO (FNOl, 00098892).
- Parrish J, Maxwell C, Beecroft JR (2015) Splenic Artery Aneurysm in Pregnancy. J Obstet Gynaecol Can 37:816-818.
- Lee AJ, Koyyalamudi PL, Martinez-Ruiz R (2008) Severe transfusion-related acute lung injury managed with extracorporeal membrane oxygenation (ECMO) in an obstetric patient. J Clin Anesth 20:549-52.
- Munshi L, Telesnicki T, Walkey A, Fan E (2014) Extracorporeal life support for acute respiratory failure. A systematic review and metaanalysis. Ann Am Thorac Soc 11:802-10.
Editorial Information
Editor-in-Chief
Article Type
Clinical Image Article
Publication history
Received: December 17, 2021
Accepted: January 17, 2022
Published: January 20, 2022
Copyright
©2022 Obare LP. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation
Obare LP, Simek M, Halama J, Dzvincuk P (2022) Extracorporeal membrane oxygenation for severe transfusion-related acute lung injury after splenic artery aneurysm ruptures in pregnancy. Glob Imaging Insights 7: DOI: 10.15761/GII.1000219
Corresponding author
Martin Simek, MD, PhD
Department of Cardiac Surgery, University Hospital, I.P.Pavlova 6, 77900 Olomouc, Czech Republic
E-mail : bhuvaneswari.bibleraaj@uhsm.nhs.uk




