An increased risk of testicular cancer in men with infertility and poor semen quality has been reported. Our aim is to present a patient who was being studied for infertility and incidentally found a testicular nodule, discuss management and prevalence of small testicular masses.
Historically testicular masses have presented as palpable lesions, but scrotal Ultrasound (US) has rapidly become the preferred modality to detect scrotal pathology with sensitivity approaching 100% for testicular masses [1,2]. Now with increasing use and availability of US technology we are seeing an increase in incidental masses in other organs such as the testes and we are faced with the question of how to act upon these findings without compromising patient care [3,4]. The current literature on long-term follow up and safety data on nonpalpable small testicular masses (STMs) is lacking [5].
The prevalence of germ cell neoplasia in situ (GCNIS) is increased in non-obstructive azoospermia (NOA) [6] and increases with the degree of spermatogenic impairment [7].
GCNIS is a precursor lesion that eventually becomes malignant [8].
Histologic evaluation of the testicular biopsy is considered the gold standard for diagnosis of GCNIS [9]. Additional use of the immunohistochemical tumor markers PLAP and OCT3/4 enhances the accuracy of histologic evaluation [10,11]. However, when only a standard testicular biopsy (3x3 mm) is performed, a false-negative result is possible due to the focal distribution of GCNIS [12,13].
A 42-year-old male patient presented with secondary infertility. Physical exam was unremarkable. US showed right testis with multiple calcifications and hypoechogenic oval images with poor vascular peripheral signal measuring 6 to 8 mm (Figure 1). Spermogram showed NOA. Laboratory workup revealed normal tumor markers. He was submitted to a Magnetic resonance (MR) that showed in lower pole of the right testis pseudonodular images without contrast enhancing (Figure 2).
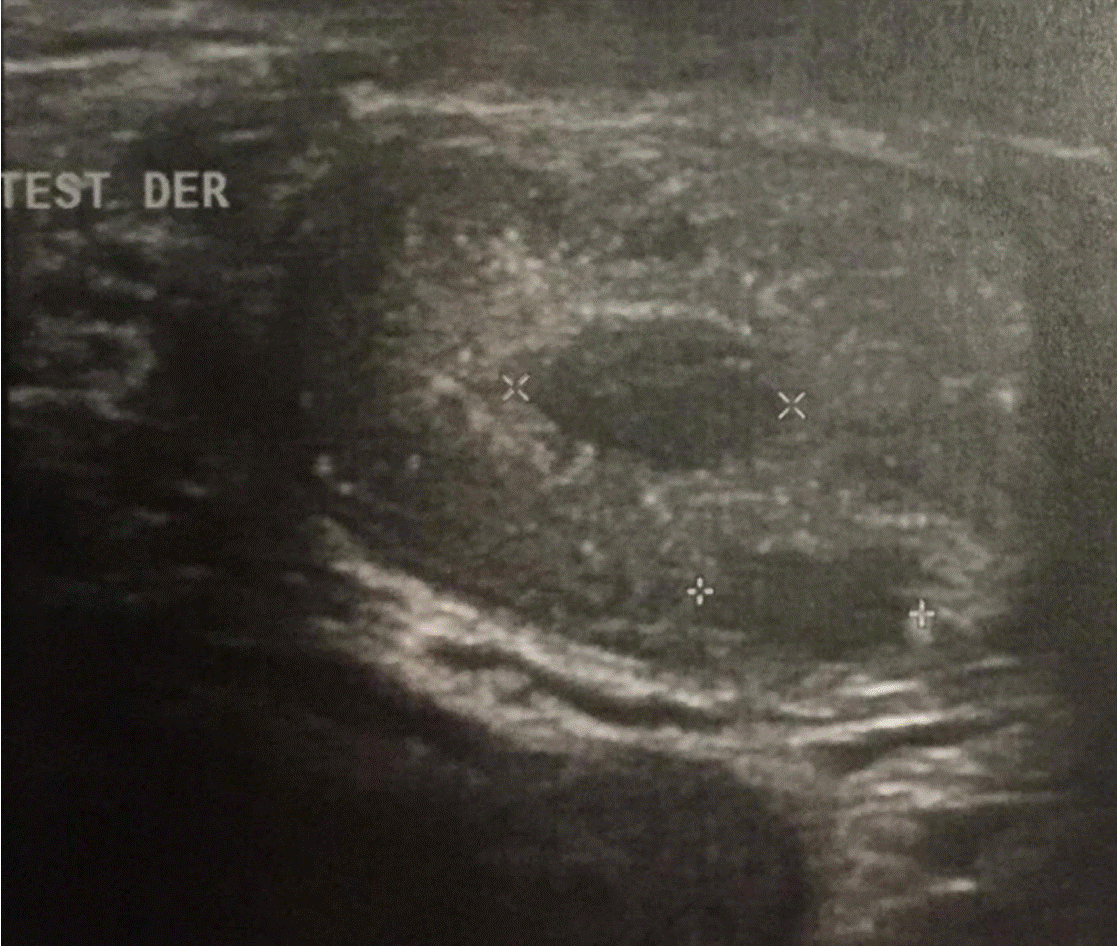
Figure 1. US showed right testis with multiple calcifications and hypoechogenic oval images with poor vascular peripheral signal measuring 6 to 8 mm.
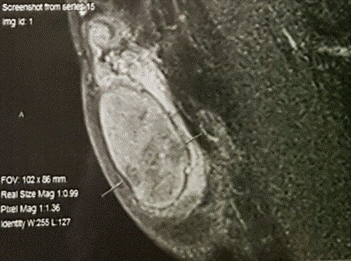
Figure 2. Magnetic resonance (MR) that showed in lower pole of the right testis pseudonodular images without contrast enhancing.
The patient was scheduled for testicular sperm extraction (TESE) and biopsy of lower pole. Intraoperative biopsy showed azoospermia and seminoma. Therefore, he underwent right orchiectomy (Figure 3). The postoperative period was uneventful, and the patient exited the hospital the next day.
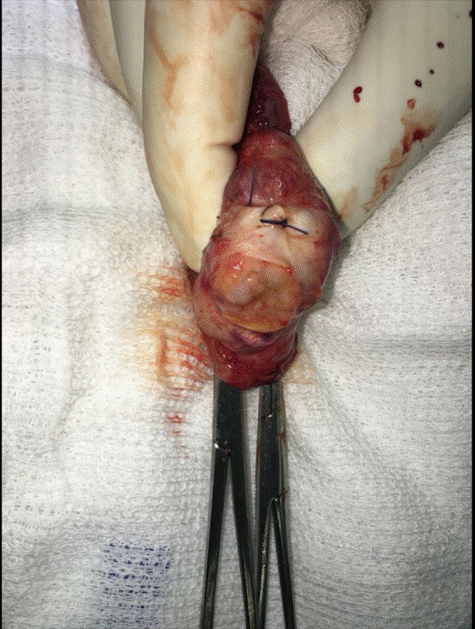
Figure 3. Right orchiectomy.
Histopathological evaluation of the specimens revealed GCNIS. Tumor cells stained positive for OCT ¾. Chest abdomen pelvis Computed Tomography (CT) scan showed multiple nodules smaller than 5 mm and mediastinal lymph nodes (Figure 4). Biopsy of mediastinal lymph nodes revealed Sarcoidosis.
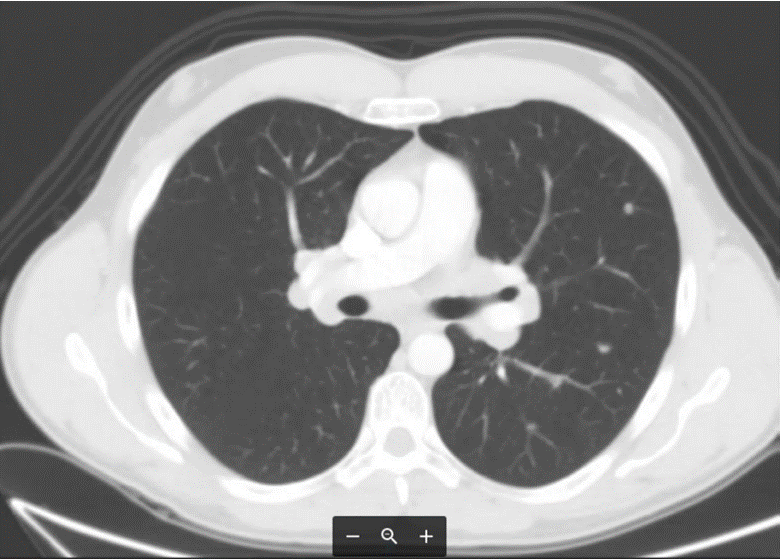
Figure 4. Chest abdomen pelvis Computed Tomography (CT) scan.
Infertility and testicular cancer have been linked, with germ cell tumors found in up to 0.5% of men with infertility, a nearly 20-fold greater prevalence than in the general population [14,15].
Classic teaching about the treatment of solid testicular lesions is extirpative surgery with radical orchiectomy due to the risk of germ cell tumor [5]. However, this dogma is changing as experience has demonstrated that many incidentally discovered small masses prove to be benign [5]. Bieniek et al. [5] reported 120 infertile men that were diagnosed with incidental sub centimeter hypoechoic testicular masses. Average follow up was 1.3 years and 18 men underwent surgical exploration.Malignant seminoma was found in 6 patients, comprising 5% of the overall cohort [5]. Eifler et al. [6] discovered 49 testicular abnormalities, including 20 that were hypoechoic, in a total of 145 men undergoing scrotal US to evaluate nonobstructive azoospermia [16]. At sperm retrieval 14 men with hypoechoic masses 1 cm or less underwent excision and all showed benign pathology.
Novel biomarkers and imaging techniques may eventually help define the malignant risk in men found to have incidental STMs (Figure 5) [5]. Routine staging CT appears unnecessary for these lesions [17].
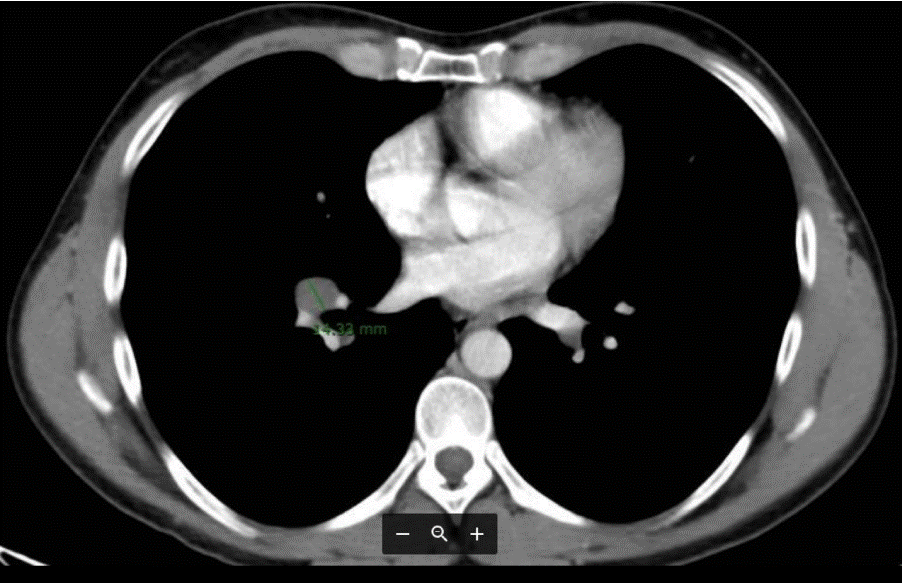
Figure 5. Incidental STMs.
A high number of non-palpable testicular nodules may be found by the combined use of testicular ultrasound and biopsy in azoospermic men examined for infertility [18]. Mancini, et al. evaluated 145 azoospermic patients. Testicular ultrasonographic nodules were found in 11 out of 145 patients (7.5%). Ninety-seven, including the 11 with testicular nodules, where asked to submit to TESE and biopsy to search for spermatozoa. Nine out of the 11 subjects with testicular nodules underwent a more extensive microsurgical exploration and they found one seminoma, one embryonal carcinoma, three Leydig cell tumours and four Leydig hyperplasias. The biopsies which were routinely performed during TESE detect two additional GCNIS [18]. In azoospermic patients TESE must be accompanied by anatomopathological study, not only for define the cause of infertility but to discard also associated serious diseases, such as tumors of germ cells and GCNIS [19] (Figure 6).
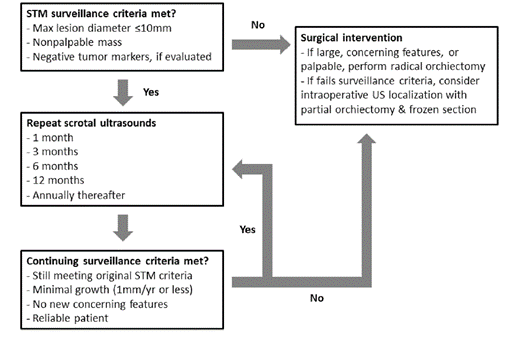
Figure 6. Suggested small testicular mass surveillance algorithm.
Small, nonpalpable, hypoechoic lesions with negative tumor markers detected incidentally during evaluation
for infertility can be safely follow up with serial ultrasound. Before TESE, in azoospermic patients it should be mandatory to submit the patient to scrotal US based on the high prevalence of non-palpable testicular nodules detected as small cancer upon surgery.
- Appelbaum L, Gaitini D, Dogra VS (2013) Scrotal ultrasound in adults. Semin Ultrasound CT MR 34: 257-273. [Crossref]
- Winter TC (2009) There is a mass in the scrotum what does it mean? Evaluation of the scrotal mass. Ultrasound Q 25: 195-205. [Crossref]
- Silverman SG, Israel GM, Herts BR, Richie JP (2008) Management of the incidental renal mass. Radiology 249: 16-31. [Crossref]
- Conti A, Santoni M, Sotte V, Burattini L, Scarpelli M, et al. (2015) Small renal masses in the era of personalized medicine:Tumor heterogeneity, growth kinetics, and risk of metastasis. Urol Oncol 33: 303-309. [Crossref]
- Bieniek JM, Juvet T, Margolis M, Grober ED, Lo KC, et al. (2018) Prevalence and Management of Incidental Small Testicular Masses Discovered on Ultrasonographic Evaluation of Male Infertility. J Urol 199: 481-486. [Crossref]
- Rørth M, Rajpert-De Meyts E, Andersson L, Dieckmann KP, Fossa D, Grigor KM, et al. (2000) Carcinoma in situ in the testis. Scand J Urol Nephrol 205:166–86.
- Mancini M, Carmignani L, Gazzano G, Sagone P, Gadda F, et al. (2007) High prevalence of testicular cancer in azoospermic men without spermatogenesis. Hum Reprod 22: 1042–1046. [Crossref]
- Dohle GR, Elzanaty S, van Casteren NJ (2012) Testicular biopsy: clinical practice and interpretation. Asian J Androl 14: 88–93. [Crossref]
- Hessel M, Ramos L, D'Hauwers KWM, Didi DMBraat, Hulsbergen-van de Kaa CA (2016) Beneficial value of testicular sperm extraction-AgarCyto in addition to the standard testicular biopsy for diagnosis of testicular germ cell tumors in nonobstructive azoospermia. Fertility and Sterility 105: 0015-0282.
- Dieckmann KP, Kulejewski M, Heinemann V, Loy V (2011) Testicular biopsy for early cancer detection—objectives, technique and controversies. Int J Androl 34: e7–e13. [Crossref]
- Van Casteren NJ, de Jong J, Stoop H, Steyerberg EW, de Bekker-Grob EW, et al. (2009) Evaluation of testicular biopsies for carcinoma in situ: immunohistochemistry is mandatory. Int J Androl 32: 666-674. [Crossref]
- Van Casteren NJ, Boellaard WPA, Dohle GR, Weber RFA, Kuizinga MC, et al. (2008) Heterogeneous distribution of ITGCNU in an adult testis: consequences for biopsy-based diagnosis. Int J Surg Pathol 16: 21–24. [Crossref]
- Oosterhuis JW, Stoop H, Dohle G, Boellaard W, van Casteren N, et al. (2011) A pathologist's view on the testis biopsy. Int J Androl 34: e14–e9. [Crossref]
- Pierik FH, Dohle GR, van Muiswinkel JM, Vreeburg JT, Weber RF (1999) Is routine scrotal ultrasound advantageous in infertile men? J Urol 162: 1618-1620. [Crossref]
- Carmignani L, Bozzini G (2006) Re: Increased incidence of testicular cancer in men presenting with infertility and abnormal semen analysis. J. D. Raman, C. F. Nobert and M. Goldstein. J Urol 175: 1574. [Crossref]
- Eifler JB Jr, King P, Schlegel PN (2008) Incidental testicular lesions found during infertility evaluation are usually benign and may be managed conservatively. J Urol 180: 261-264. [Crossref]
- Toren PJ, Roberts M, Lecker I, Grober ED, Jarvi K, et al. (2010) Small Incidentally Discovered Testicular Masses in Infertile Men—Is Active Surveillance the New Standard of Care? J Urol 183: 1373-1377. [Crossref]
- Mancini M, Carmignani L, Gazzano G, Sagone P, Gadda F, et al. (2007) High prevalence of testicular cancer in azoospermic men without spermatogenesis. Human Reprod 22: 1042–1046. [Crossref]
- Gomisa C, Sarquella J, Arcec Y, José Ignacio V (2017) Neoplasia intratubular testicular e infertilidad:azoospermia asociada a neoplasia intratubulartesticular bilateral. Rev Int Androl 15: 165-168.






