Abstract
Objectives: This study assessed medical students' impressions of surgery during surgical rotations and how their experience influenced career choices. An additional objective was to propose practical workplace activities to improve learning and prepare students for clinical practice.
Methods: A two-stage investigation included an anonymous electronic survey of 104 penultimate and final-year medical students followed by focus group deliberation. Participants included students and employees from an Australian metropolitan teaching hospital. Focus group members were invited from hospitals and academic institutions across Australia.
Results: Less than half of respondents found their surgical rotation useful for preparing for exams (41%) or future intern roles (48%). Students were more satisfied and more likely to consider surgical careers when made to feel welcome and when expectations were clear. When students felt welcome, 108 expressed interest in surgical careers; conversely, 83 students who did not feel welcome were dissuaded from surgery. Focus group discussion identified positive learning scenarios and proposed novel approaches to enhance educational experiences.
Conclusions: To improve engagement and promote surgery as a career path, clinical rotations must enable students to actively participate as team members, independently consult patients, and seek targeted learning opportunities. A workflow program guided by survey and focus group outcomes is underway at an Australian metropolitan hospital, emphasizing immersive team involvement, live patient encounters, practical skill development, and clear expectations. This intervention promises to stimulate interest in surgery and better utilize student rotation time.
Keywords
medical student, teaching methods, career choice, competencies
Introduction
Medical students are increasingly gaining knowledge and skills by remotely taking content, and maintaining student engagement in clinical rotations is challenging for educators. The effect of these changing attitudes on learning is yet to be felt in the clinical setting; however, it is common for students to lack confidence and feel unprepared in the initial years of hospital practice [1-3]. Students perceive the quality of education gained in lectures and clinical rotations as inferior to that gained by utilizing readily available online resources, such as OnlineMedEd, AMBOSS, and Osmosis. It appears that using these resources and self-directing learning produces non-inferior academic outcomes compared with university-led teaching, and some students claim that foregoing university lectures in favour of online resources has been a crucial part of their career advancement [4,5]. In addition, although clinicians generally see teaching as an important part of their practice, time pressure and unclear learning objectives contribute to poor student experiences [6].
There is a declining interest in surgery as a vocation worldwide, with a particular decline in general surgery [7-9]. For example, in Australia, the proportion of graduates preferring surgery as a future area of practice in 2010 was 23%. In 2023, the proportion was 12.6%, with a gradual decline across 13 years. However, the proportion of international students who moved to Australia after graduating who preferred surgery was, on average, 6.5% higher than that of domestic students between 2021 and 2023. The overall number of applications to surgical disciplines in Australia has undergone a significant decline from 1150 in 2015 to 799 in 2022 [10], but appears to be rebounding with robust interest from international medical graduates. The top three factors influencing the choices made by graduates when considering their choice of a future discipline between 2019-2023 consistently included “alignment with personal values,” “atmosphere/work culture typical of the discipline” and “experience of a specialty while on placement as a medical student” [11]. Thomas, et al. claimed that the views of medical students about general surgery as a practice are, however, prone to misconceptions and inaccurately perceive surgery as an inhospitable environment to work in [12]. Overall satisfaction among trainees also contrasts with the views of medical students, where the main drivers of dissatisfaction among trainees are related to poor lifestyle and most are content with their work environment [13,14].
The goal of this study is to explain the reasons for low engagement in surgical rotations and explore opportunities for experience-based teaching and learning. Dornan et al. demonstrated the value of experience-based learning but stressed that self-directed learning cannot substitute for mentoring and support [15]. While online environments can likely effectively provide theoretical knowledge, the fall in attendance at clinical rotations may lead to shortcomings in clinical expertise with potential consequences for patient outcomes. The COVID pandemic clearly affected the clinical rotation experience when students were unable to attend in person to engage with patients and physicians. As a result, anxiety associated with career direction has potentially led to a decrease in confidence in taking decisive steps towards gaining training positions across all fields [16].
Innovation in teaching delivery will undoubtedly be driven by advancing technology, but the measurement of student engagement shows that live patient experience outperforms game and simulation style modalities [17]. Medical students commit multiple years of working age to develop skills in an apprenticeship model. The human capital invested in these years is a potent economic resource that could be better exploited by empowering students to independently engage patients and make a direct contribution to patient care. By focusing on surgery hospital rotations, this study aimed to identify the experiences and environments that bring the highest yield to student learning, make a direct contribution to patient care, and satisfy academic and competency expectations.
Materials and methods
In the first stage, a structured electronic questionnaire was developed to obtain objective qualitative and quantitative data. The questionnaire was distributed for self-administration to penultimate and final-year medical students undergoing a postgraduate medical degree, and first- and second-year practitioners. From a survey population of 340, 104 responses were collected between October 2023 and June 2024. The electronic form allowed for anonymous responses and consisted of Likert-scale questions to measure attitudes, beliefs, opinions, and motivations. It also provided an opportunity for responses to open-ended questions.
Following analysis of the survey data, a semi-structured focus group discussion was conducted to explore the findings in greater depth and develop practical recommendations. Participants (n=8) were purposively selected through stakeholder analysis to ensure diverse perspectives, including clinical lecturers from multiple Australian centres, representatives of prevocational education and training, medical students with both expressed interest and disinterest in surgical careers, and first-year practitioners. The focus group was conducted via a combined in-person and videoconference format and lasted approximately two hours. Discussion was guided by key themes emerging from the survey data, including factors influencing rotation satisfaction, barriers to effective teaching, and strategies to enhance student engagement. The session was audio-recorded with participant consent, and thematic analysis was conducted to identify recurring themes and actionable recommendations. A transcript of the focus group discussion is available on request.
Results
The survey was designed to assess surgical rotations in achieving academic, clinically relevant, and stimulating workplace experience. In addition, the survey gained responses on how rotation influenced career decisions.
Less than half of the respondents felt that their surgical term was useful in preparing them for clinical examinations (41%) or case presentation examinations (39.8%) (Figure 1). As an activity in preparing for internships, 48.0% of the respondents agreed that their surgical rotations were useful. Respondents consistently indicated that more theatre exposure, increased involvement in ward-based tasks, and more patient interactions would improve their experiences. Of the surgical specialties, general surgery received the most favorable responses (40.8%), followed by vascular surgery (12.2%) and orthopaedics (5.1%). Respondents indicated that the optimal number of surgical rotations during medical school was two (56.2%). Only 7.3% of participants said that more than two rotations were desirable.
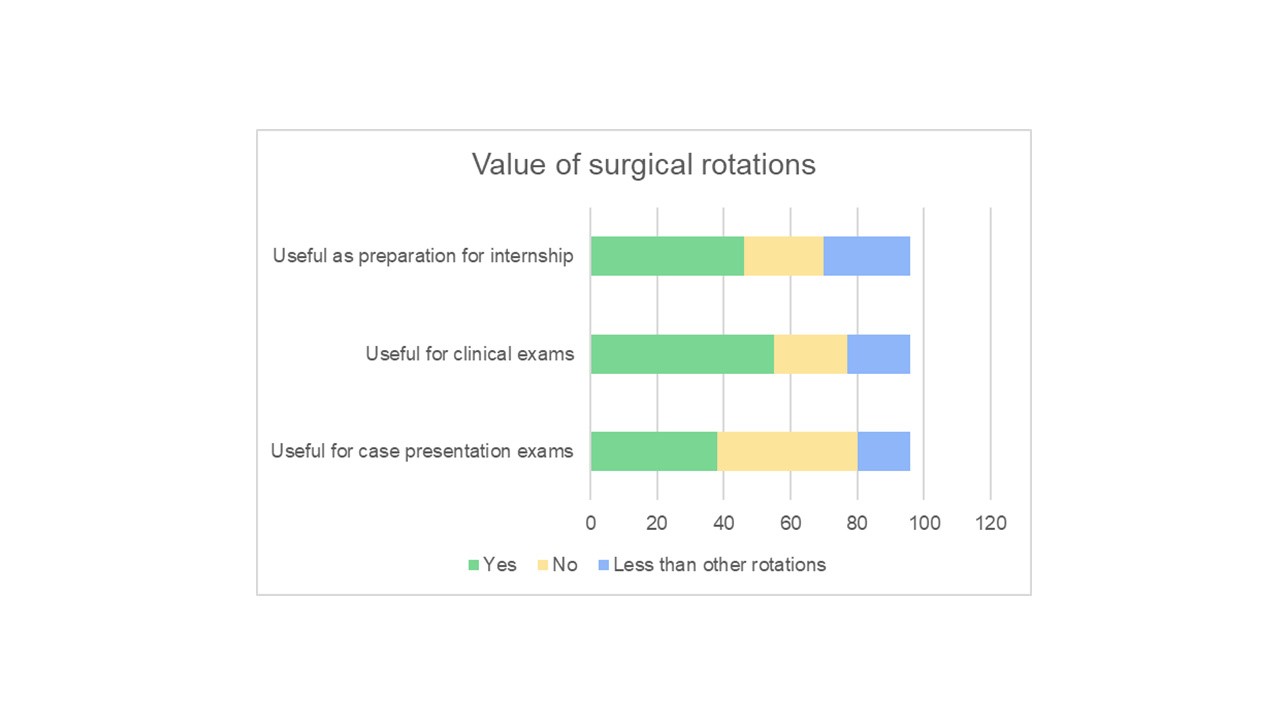
Figure 1. Students placed high value on activities such as preparing for future work and exam performance. Less than half of surveyed students felt that surgery rotations provided experiences that improved desired outcomes
The rotation experience was enhanced when students felt welcomed (57.9%) and were able to be involved as team members (29.6%) (Figure 2). Overall, responses from 350 rotations were collected, and on 108 occasions, a student who was made to feel welcome expressed interest in pursuing a career in surgery. In contrast, on 83 occasions, a student who was not made to feel welcome on the team indicated that the rotation persuaded them to reject a career in surgery. Considering that 48% of students had not made up their minds about career direction, the data suggest that simply welcoming a student to a team can be an influential component in career choice.
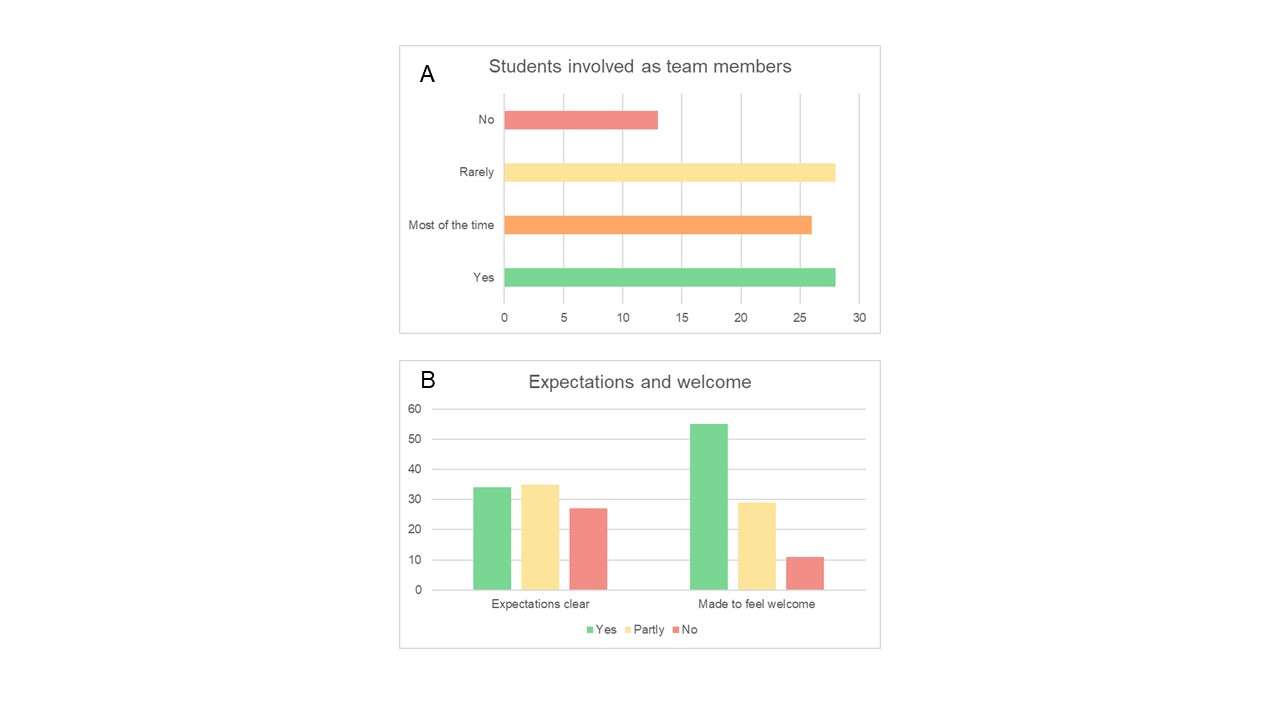
Figure 2 A/B. Students perception of team involvement, welcome and an understanding of expectations at the start of the rotation
Expectations of attendance and learning outcomes were clear for students on less than one-third of the occasions, and 65.3% of the participants felt that the surgical teams were interested in teaching. The main barrier to quality teaching during their surgical rotation was attributed to a lack of available consultants and surgical trainee time dedicated to teaching or the lack of interest in teaching. There were documented instances where students felt unwelcome, and some consultants dedicated to supervisors were unavailable for interactions with students.
Attitudes towards pursuing a career in surgery after surgical rotation were assessed. Factors that improved a student’s perception of a career in surgery included spending time in theatre, handling instruments during procedures, receiving anatomy tuition during procedures, reviewing patients independently in the emergency department or outpatient clinics, and performing bedside procedures such as suturing, intravenous cannulation, phlebotomy, and placement of indwelling catheters. Respondents consistently reported that experiences were enhanced when expectations were clear, dedicated teaching time was provided, they were made to feel part of the team, and when supervisors were responsive. The factors associated with dissuading students from a career in surgery were perceived as long working hours, impact on personal time outside of work, difficulty in gaining a training position, and poor work culture (Figure 3).
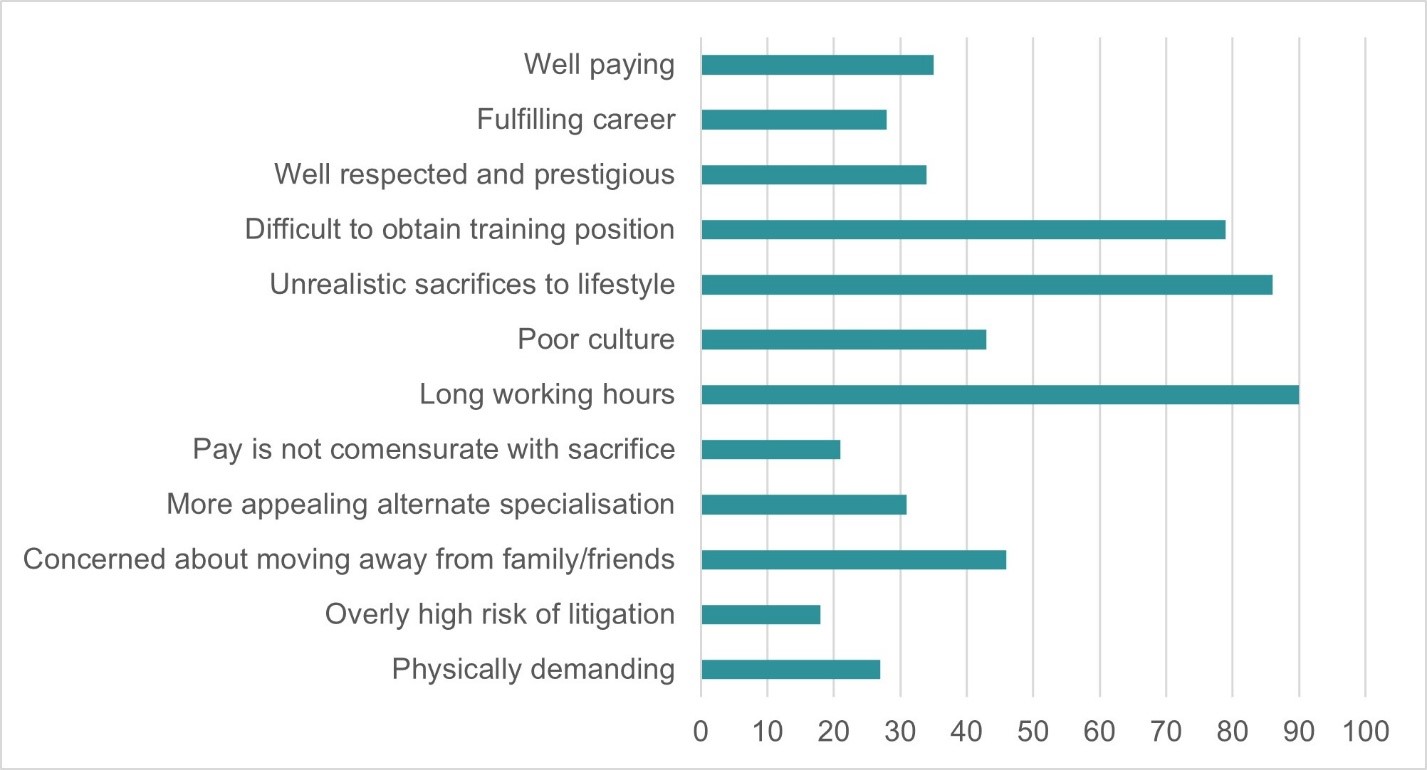
Figure 3. Perceptions of a career in surgery after surgical rotation
Focus group themes
The focus group format facilitated interactions between group members to observe the attitudes and perceptions of participants during the discussion, which are typically not apparent in other data-gathering formats [18]. In addition, the focus group format facilitates the sharing of knowledge, expertise, and experience [19].
A.Observations
- Students are quick to assess whether an environment is going to work or not, and if it is not, they quickly lose interest.
- Our medical systems are overly service driven, and the value of teaching is diminishing.
B.Situations that have brought positive outcomes
- Whether in surgery or not, it was the inclusiveness of the team that made a difference.
- Best teaching is often provided by junior staff, training surgeons, or even fellow students in later years of study.
- Inclusive teams consistently bring rich experiences.
- Upfront sharing of expectations and outcome goals enhances the experience. A common set of outcomes was set for each rotation.
C.Propositions made by focus group members
- More empowerment of junior staff, training registrars or new consultants.
- Create allowances in the weekly program. Better acknowledgement of teaching by junior doctors.
- Allow junior doctors and training registrars authority to promote immersive student activities rather than the traditional model of textbook teaching
- Students can develop their own patient lists, see outpatients in clinics, present cases, and participate in formulating management plans.
- Shift the focus to experiencing situations rather than focussing on deriving knowledge
- Immersive student behavior should be assessed. The level of engagement becomes an assessable item rather than the amount of learning taken.
- Develop a registry of requirements that students can access and take advantage of as they are made available by the team.
- Students could be paid in line with other professions, such as nursing, that have paid placements [20].
Discussion
To maintain sufficient general surgery practitioners to provide services befitting modern healthcare systems in the future, an emphasis on attracting students during medical training years is needed. Clinical rotations in surgery will require alignment with contemporary teaching methods and address the inclination of medical students to self-direct their learning and seek practical opportunities to develop skills.
According to the Royal Australasian College of Surgeons (RACS) activity statements from year 2005 to 2022, there is a steady decline in general surgery surgical education training (SET) applications since 2014, plateauing between 313 to 328 applicants per year since 2019. Similar trends were observed across all other surgical trainings, such as orthopaedics, otorhinolaryngology, plastic surgery, and paediatric surgery training. A decline in surgical training applicants was also reported by the Royal College of Surgeons of England, prompting surgical training bodies in different countries to reflect on the reasons for such a downturn in interest in surgical training [7,12].
Clinicians’ clinical time and cognitive pressure fluctuate, especially during hospital shifts, making it difficult for clinicians to consistently provide rich learning situations for students. The responses in this study suggest that recent graduates working in their first role as doctors are underutilized and valuable resources as educators. This study suggests that junior doctors can be more effective than senior clinicians in guiding medical students as they transition to the junior doctor role and can also be a vital academic resource. Students also see that junior medical officers as role models and the attitudes they display toward their work can heavily impact students, which in turn appears to shape students’ perceptions of the discipline they are placed in. Comments made in the focus group discussion suggest that medical schools could extend their recognition by rewarding the practice of teaching by junior doctors in the same way that senior teaching clinicians receive faculty positions in return for their commitment to teaching. Junior doctors should be involved in the assessment of students, as they are well placed to adjudicate on a student’s performance.
This study provides a basis for medical curriculum modification that promotes a culture where students can drive their own learning in the clinical setting by assigning patients to students who they follow throughout their hospitalization from admission to discharge, and students play an active role in providing care. This encourages students to understand the evolution of disease and management, and the interplay between various healthcare professionals, while simultaneously developing a sense of belonging in a team.
Guided by the responses from the survey and focus group conversations, a surgery rotation learning format was proposed and implemented (Table 1). The workflow was based on the key themes identified in this study: 1. Immersive involvement in the surgery team (IM), 2. Live patient encounters (LPE); 3. Practical clinical skill development (SK); 4. Clear understanding of expectations (Ex). Pilot programs at suburban and rural hospitals in Australia are underway, and although objective data are not available, the responses of the students involved have been overwhelmingly positive. The formal introduction of the program is scheduled for 2026 at a metropolitan public hospital with postgraduate students.
Table 1. The workflow for medical students on surgery rotations aligned with survey responses and focus group outcomes
Workflow item |
Key theme addressed |
Rotation introduction and expectation guide |
Ex |
Students are alerted by on-call registrars of new ED, ward or clinic consultation request |
IM |
Obtain history, physical examination, initiate bedside management (IV access, NGT, IDC etc.) |
IM, LPE, SK |
Propose and document management plan |
IM, SK |
Generate individual patient list and conduct daily ward round |
IM, SK |
Attend surgical procedures and participate in ward-based care |
IM, SK, LPE |
Propose and contribute to discharge care |
IM, SK |
Present the scientific, clinical and theoretical aspects of case to supervisors during allocated time |
IM, Ex |
Follow-up at post hospital encounter |
IM, SK, LPE |
Conclusion
The changing nature of medical education includes multimodal, self-directed, often online, and remote teaching. The value of experiential learning, however, cannot be understood, and the perspectives gained during coalface medical experiences are shown in this study to influence future career directions. Our suggested work model for clinical placements empowers students to drive their own learning, identify gaps in knowledge, and provide them with a sense of belonging and importance as future clinicians. The proposed format promises to engage students better, leaving more individuals with an impression of surgery as a fulfilling and worthwhile professional pathway. The positive outcome of retaining an interest in surgery at the medical student stage is that a greater diversity of candidates will be available to draw a surgical workforce that reflects the communities they serve.
Conflicts of interest
The authors have no conflicts of interest to declare.
Author’s contributions
YWT: Data collection, drafting, analysis, interpretation of results.
YF: Data collection, analysis.
MB: Analysis, interpretation of results, final revisions.
PW: Concept, design, data collection, analysis, interpretation of results, drafting, and final revision.
Ethics approval
Ethics approval was granted by the Australian Capital Territory Human Research and Ethics Low-Risk Sub-Committee (2025/ETH02087)
Research data for this article
Owing to the sensitive nature of the questions asked in this study, survey respondents were assured that raw data would remain confidential and would not be shared.
References
- Hawkins N, Younan HC, Fyfe M, Parekh R, McKeown A (2021) Exploring why medical students still feel underprepared for clinical practice: A qualitative analysis of an authentic on‐call simulation. BMC Med Educ 21: 165. [Crossref]
- Monrouxe LV, Grundy L, Mann M, John Z, Panagoulas E, et al. (2017) How prepared are UK medical graduates for practice? A rapid review of the literature 2009-2014. BMJ Open 7: e013656. [Crossref]
- Martin P, McGrail M, Fox J, Partanen R, Kondalsamy-Chennakesavan S (2022) Impact of the COVID-19 pandemic on medical student placements in rural Queensland: A survey study. Aust J Rural Health 30: 478-487. [Crossref]
- Doggrell SA (2020) No apparent association between lecture attendance or accessing lecture recordings and academic outcomes in a medical laboratory science course. BMC Med Educ 20: 207. [Crossref]
- Doggrell SA (2021) Quantitative study of lecture attendance and the association between this attendance and academic outcomes for nursing and nonnursing students in an introductory pathophysiology course. Adv Physiol Educ 45: 651-660. [Crossref]
- Lan NSR, Nasim S, Gan SK, Chew GT (2022) Clinicians' perceptions of medical student teaching in a tertiary hospital. Educ Health (Abingdon) 35: 16-19. [Crossref]
- Fischer JE (2007) The impending disappearance of the general surgeon. JAMA 298: 2191-2193. [Crossref]
- Hill EJR, Bowman KA, Stalmeijer RE, Solomon Y, Dornan T (2014) Can I cut it? Medical students' perceptions of surgeons and surgical careers. Am J Surg 208: 860-867. [Crossref]
- McDonald K, Sutton J (2009) Surgical workforce: An emerging crisis. Bull Am Coll Surg 94: 21-26. [Crossref]
- Surgeons RACo. RACS Activity Statements. 2007 - 2022.
- Zealand MDAN. Medical School Outcome Database, NAtional Data REport. 2010 - 2023.
- Thomas A, Murtaza AN, Michael Spiers HV, Zargaran A, Turki M, et al. (2019) Declining interest in general surgical training - Challenging misconceptions and improving access at undergraduate level. Ann Med Surg (Lond) 40: 3-8. [Crossref]
- Keegan RJ, Saw R, De Loyde KJ, Young CJ (2015) Attitudes and risk of withdrawal in general surgical registrars. N Z Med J 128: 61-68. [Crossref]
- Lennon MJ, McGrail MR, O'Sullivan B, Tan A, Mok C, et al. (2020) Understanding the professional satisfaction of hospital trainees in Australia. Med Educ 54: 419-426. [Crossref]
- Dornan T, Boshuizen H, King N, Scherpbier A (2007) Experience-based learning: A model linking the processes and outcomes of medical students' workplace learning. Med Educ 41: 84-91. [Crossref]
- Sani I, Hamza Y, Chedid Y, Amalendran J, Hamza N (2020) Understanding the consequence of COVID-19 on undergraduate medical education: Medical students' perspective. Ann Med Surg (Lond) 58: 117-119. [Crossref]
- Rohlfsen CJ, Sayles H, Moore GF, Mikuls TR, O'Dell JR, et al. (2020) Innovation in early medical education, no bells or whistles required. BMC Med Educ 20: 39. [Crossref]
- Wong LP (2008) Focus group discussion: A tool for health and medical research. Singapore Med J 49: 256-260. [Crossref]
- Kitzinger J (1995) Qualitative research. Introducing focus groups. BMJ 311: 299-302. [Crossref]
- Smith S, Smith C, Caddell M (2015) Can pay, should pay? Exploring employer and student perceptions of paid and unpaid placements. Act Learn High Educ 16: 149-164.



