“Moral Injury” is the manifestation of the psychological wounds experienced by an individual after betrayal of their morals and beliefs. The Covid-19 pandemic has acted as a catalyst for moral injury and its detrimental effects on physical and mental health can be seen in the Healthcare Workers (HCWs) battling on the frontlines. It has unmasked new ethically challenging dilemmas, which includes weighing personal risk versus duty of patient care whilst triaging an unlimited number of patients within the finite available resources. The societal narrative to portray doctors as heroes by the usage of military metaphors in media headlines has created an added pressure on HCWS to overexert themselves and meet an unreasonable demand of being self-sacrificial. The pre-existing seeds of moral injury also root from workplace cultures, where high levels of stress may be seen as an indicator of good work with no support for mental health maintenance. Moral Injury proves to have severe consequences that effect the proficiency of care delivered by HCWs. Robust counter mechanisms in place can help mitigate the effects of moral injury.
Moral injury is the functional impairment, that occurs following betrayal of one’s moral beliefs and expectations. When it comes to pointing the finger at the factors responsible for psychological distress in HCWs, burnout and inability to self-mediate are often blamed. Whilst they play a role in producing both mental and physical symptoms of exhaustion, they are only insults that add to a moral injury. It is a manifestation of the psychological, behavioural, and spiritual consequences [1]. In the context of healthcare, moral injury can be defined as “the challenge of simultaneously knowing what care patients’ need but being unable to provide it due to constraints that are beyond our control” [2].
The concept of moral injury was first derived from the symptoms expressed by military workers returning from the Vietnam war. These symptoms were characteristic of post-traumatic stress disorder (PTSD), but could not be clinically categorised as such. Prolonged exposure to morally distressing situations, was thought to be the cause of these moral wounds [2]. These symptoms are often mirrored by HCWs, due to their increased exposure to witnessing human distress and suffering.
Symptoms of moral injury have been especially prevalent during the Covid-19 pandemic [2,3]. COVID-19 due to its fast transmission and high mortality rate was officially declared as a pandemic by the World Health Organisation, on March 11th, 2020 [4,5]. Its imminent threat forced governments to instate nationwide lockdowns across the globe, resulting in most job sectors suffering a loss in working time. However, HCWs were pushed to the frontline due to playing a crucial part in global recovery [6].
During this time, HCWs were more prone to facing ethically challenging scenarios that may lead to moral injuries. With almost 40% of ICU workers reporting symptoms similar to PTSD, it is safe to say that the effects of the pandemic on the mental health of HCWs has been severe [4,6].
An example of an ethical dilemma HCWs are faced was triaging the finite resources available for patient care. Despite efforts to efficiently distribute resources, they were still inadequate to meet demands [7,8]. This could be a gateway to moral injury when making clinical decisions. For instance, choosing between maintaining ventilatory support for a critically ill patient or transferring the use of that same ventilator to a patient with a better prognosis, may lead to anxiety, fear and stress in these workers [6,9,10]. This can subsequently have a negative impact on patient care and job satisfaction, which can eventually lead to psychological disequilibrium [1].
Another ethical dilemma could arise from reweighing personal risk versus duty to patient care. The fear of not only being infected with Covid-19, but also transmitting it to family, could result in a need to reassess risk [6]. A systematic review on the infection and mortality of HCWs, highlighted that as of December 2020, there had been 1,413 deaths out of the 152,888 reported infections amongst HCWs. This suggests that the risk of mortality in HCWs after infection, is 1 in 100 [11]. This knowledge would undoubtedly be present as a formidable mental challenge in the minds of HCWs [12].
The limitation on personal protective equipment available, alongside the arguably inadequate guidelines surrounding their use, could also fuel concerns of safety. Psychological implications of this heightened fear consequently led to increased risk for stress-related disorders such, as depression and anxiety [12]. These symptoms are a prelude to psychological burnout and could ultimately result in HCWs choosing to leave the profession [13].
These scenarios may predispose HCWs to encountering an increasing number of scenarios with grieving families, in which they will not be able to say “We did all we could,” but instead, “We did our best with the resources available, but it still was not enough”. That would be the seed of moral injury [13].
However, in a pre-covid healthcare system, the baseline for facing moral injury, has always been prevalent. Delivering efficient patient care whilst contending with the duties to the institution, insurers, and even responsibility to oneself, all set this precedent [2]. Therefore, increased exposure to an environment, where it is a constant battle between the precept of doing what is in the patients best interest, whilst meeting the external demands of the double binds in healthcare can be emotionally taxing.
With the majority of workers facing these challenges on a daily basis, it is fundamental to provide support for the emotional repercussions, the job entails. Facing a combination of ethical dilemmas and psychological quests, alongside the pressure to meet patient demands, can be a burden on a medical professional’s emotional wellbeing [9]. Unfortunately, barriers to accessing the support they need, can root from the workplace itself. Internalised stigma surrounding mental illness in HCWs, has served as discouragement for professionals openly engaging in discussion to seek help for psychological problems [14].
In some workplace cultures in the healthcare sector, a high level of stress is taken as an indicator of commitment to work. The implication of this results in hesitation to seek help, due to the added factor of “professional consequences”. Fear of losing their professional reputation, as well as missing out on competitive opportunities for career advancement is constantly iterated in their minds [15]. For staff suffering with moral injury, prolonging the suffering, without addressing solutions to the symptoms, can make their symptoms gradually worsen over time. This could have adverse effects on patient care and safety. In order to overcome this, health care organisations should make conscious effort to create a common understanding between their employees, regarding the notion of working towards the same outcome of patient care. Jumping over this hurdle will lead to the desired goal, a supportive community [2].
During the Covid-19 crisis, the media was also integral in playing a part on the mental wellbeing of HCWs. Several news outlets nationally broadcasted headlines titled “health care heroes” working on the “frontlines” [16]. The fundamental qualities of a hero include integrity, bravery and selflessness. Whilst integrity and bravery to some extent are fundamental qualities of any HCW, is self-sacrifice needed to deliver effective healthcare[17]? The usage of military metaphors to portray healthcare workers with a heroic narrative, carries its consequences on their mental health, despite being used in a complementary context. It may result in the inability to distinguish between the professional standard they are expected to perform at, from the unreasonable societal demand to being self-sacrificial for the “call of duty” [16,17]. This societal pressure could be a critical factor in changing the moral compass of HCWs, forcing them to push themselves to accommodate for this public expectation. This would unquestionably have its adverse effects [2]. For example, the presence of an added factor of guilt from not being able to perform to an unrealistic standard of care. This may exacerbate the symptoms of “guilt without fault” associated with pre-existing moral injury resulting in severe psychological distress [1].
To compensate for this feeling of guilt, HCWs may overexert their efforts, by increasing their workload. This would be attainable by adopting unhealthy coping mechanisms, such as over commitment, sleep deprivation, and a work-life imbalance; all of which are associated with burnout. This in turn would drastically increase the chances of medical errors and overall reduce the quality of patient care and outcomes. Consequentially, it can cause job dissatisfaction, which can manifest into stress, mood disorders and depression. This would ultimately result in them leaving the profession or letting the cycle of psychological suffering continue [18].
It is key to note, that whilst the pandemic may have exacerbated the heroic narrative in which HCWs are portrayed, this predisposition previously existed. This shared societal opinion depicting jobs in the health sector as altruistic volunteer work, is demonstrated by the newspaper coverage of the 2001/2002 strike by mental health nurses in New Zealand [19]. These nurses were striking against the turnover of pre-existing legislations, which resulted in “eroded pay”. The specific alteration to the employment contracts, which disregarded working overtime, cost these nurses countless hours of their salary. The public depicted nurses who chose to strike for their hard-earned pay, as “greedy and lazy.” This backlash emphasises how the public may view the services that HCWs provide, as a consumer right. Correspondingly leading them to overlook the fundamental rights to protest for fair pay [19].
For the nurses who chose not to strike, an undertone of general admiration was used to portray a picture of commitment [19]. This reinstates, the organisational stigma mentioned above, consequently exacerbating symptoms of moral injury [1]. Constant exposure to poor working conditions can be detrimental to the mental health of a professional working in any field. This results in an increased margin of professional error. In a sector where human life is at stake, the risk for catastrophe becomes significant [20].
Previous pandemics and epidemics, such as Severe Acute Respiratory Syndrome (SARS), Middle East Respiratory Syndrome (MERS) and Ebola all showed a significant impact on the mental health of HCWs. Up to 73.4% of HCWs were reported to have PTSD symptoms, which are characteristic of moral injury. This should have served as the initiative to implement better resources, to prepare for the mental repercussions of any future outbreaks. Previous successful attempts at improving overall mental health of workers included development and implementation of workplace mental health policies and programmes. Psychological intervention courses with stress management were also found to have a positive impact [21].
However, raising awareness by educating individuals alone through these programmes, is not enough. Recognition of the moral distress faced not only by one person, but a work-unit, or an entire organisation, is vital into introducing a system-wide approach (Flow chart 1). It is only in this way, that any noticeable changes can be brought about. To allow organisations to be better equipped to manage adversity in unpredictable future circumstances, “organisational resilience” needs to be built. This would include employing more staff responsible for mental health management, as well as encouraging figures of authority to lead conversations which focus on emotional reflection. Through the establishments of supportive environments and programmes that alleviate work stressors, organisations can be better equipped to manage adversity during times of crisis [22] (Table 1).
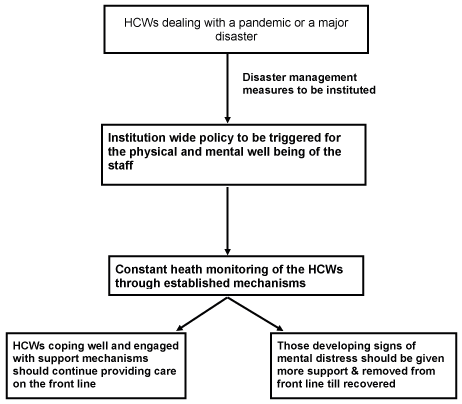
Flow chart. Proposal for dealing with HCWs during pandemics & major disasters
Table 1. Strategies to prevent moral injury

