This report summarises a case of S. lugdunensis infective endocarditis in an 86-year-old woman presenting with a 3-week history of increasing confusion and multiple falls. Although rare, the inherent properties of this bacteria mean that it can lead to a rapidly progressive endocarditis, and so the requirement for surgical intervention in addition to antimicrobial therapy is higher than when compared to other pathogens. Also, the presentation of infective endocarditis is often non-specific in elderly. These combination of factors mean that it is crucial to maintain a high index of suspicion for this disease. If S. lugdunensis is isolated from a blood culture, this should be regarded as a pathogen and prompt workup via transoesophageal echocardiography and Cardiology assessment should be done.
An 86-year-old woman was admitted following a 3-week history of increasing confusion and multiple falls. Past medical history included vascular dementia, ischaemic stroke and severe mitral regurgitation. The patient was disorientated with respiratory rate of 22 breaths/min, oxygen saturations of 93%, pulse of 80 bpm, blood pressure of 96/77 mmHg, temperature of 37.3C and NEWs score 7. Cardiovascular-respiratory examination demonstrated vesicular breath sounds with a loud pansystolic murmur. Her blood tests showed haemoglobin 124 g/dL, white cell count 25.8 10^9/L, C - reactive protein 186 mg/L, and platelets 121 10^9/L. Chest X-ray and abdominal ultrasound were normal, with sinus rhythm on ECG. Blood cultures were sent. She was commenced on intravenous fluids and antibiotics i.e. Teicoplanin and Gentamicin.
By Day 3 of admission, blood cultures grew S. lugdunensis sensitive to flucloxacillin. Cardiology opinion was sought, and a transthoracic echocardiogram showed mitral valve vegetations consistent with infective endocarditis. She was deemed not fit for surgical intervention in view of her frailty and medical comorbidities (Figure 1).
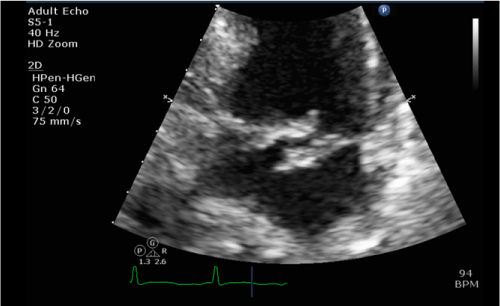
Figure 1. Transthoracic echocardiogram showing mitral valve vegetations.
Her clinical condition improved initially on medical management, however, she later developed fast atrial fibrillation with flash pulmonary oedema secondary to acute deterioration of mitral valve functioning. The patient was managed with appropriate diuretics and discharged to a nursing home for palliation within the community as agreed with her family. She passed away four weeks later.
Staphylococcus lugdunensis is a coagulase negative staphylococcus whose pathogenic potential should not be underestimated. Although a commensal of human skin, it is rarely a contaminant in blood culture and should be regarded as a pathogen [1-4]. Infective endocarditis (IE) caused by S. lugdunensis is a rare disease [2]. Its ability to bind directly to von Willebrand factor and adhere firmly to vessels and valves, makes it resistant to shearing forces and leads to a rapidly progressive endocarditis, with abscess formation and development of congestive heart failure [3], as was seen in this case. Surgical treatment is often necessary, particularly in left-sided infective endocarditis, in addition to antimicrobial therapy [4] – indeed, the requirement for valve replacement was higher for S. lugdunensis when compared with other pathogens [1].
S. lugdunensis IE has a higher mortality rate than other pathogens and often affects the elderly. Diagnosis can be delayed as presentation is usually non-specific with confusion, weight loss or fatigue [5]. Early diagnosis and treatment are therefore essential. It is important to have a high index of suspicion and blood cultures should be reviewed and acted on. Valve replacement in addition to antimicrobial therapy should be strongly considered. Finally, it is crucial to actively monitor for complications such as valve destruction and congestive cardiac failure as these significantly contribute to mortality.
- Liu PY, Huang YF, Tang CW, Chen YY, Hsieh KS, et al. (2010) Staphylococcus lugdunensis Infective Endocarditis: A Literature Review and Analysis of Risk Factors. J Microbiol Immunol Infect 43: 478-484. [Crossref]
- Ishiekwene C, Ghitan M, Kuhn-Basti M, Chapnick E, Lin YS (2017) Staphylococcus lugdunensis endocarditis with destruction of the ventricular septum and multiple native valves. ID Cases 7: 14-15. [Crossref]
- Anguera I, Del Río A, Miró JM, Matínez-Lacasa X, Marco F, et al, (2005) Staphylococcus lugdunensis infective endocarditis: description of 10 cases and analysis of native valve, prosthetic valve, and pacemaker lead endocarditis clinical profiles. Heart 91: e10. [Crossref]
- Flores Umanzor EJ, San Antonio R, Jimenez Britez G, Caldentey G (2016) Staphylococcus lugdunensis: an unusual and aggressive case cause of infective endocarditis. Case Reports 2016: bcr2016217156. [Crossref]
- Forestier E, Fraisse T, Roubaud-Baudron C, Selton-Suty C, Pagani L (2016) Managing infective endocarditis in the elderly: new issues for an old disease. Clin Interv Aging 11: 1199-1206. [Crossref]

