Right-sided, congenital diaphragmatic hernia is not common but accounts for about 20% of all congenital diaphragmatic hernia. It sometimes has serious complications, such as intrathoracic kidney and hepatic pulmonary fusion.
Here we report a rare case of right-sided diaphragmatic hernia, complicated by intrathoracic kidney and hepatic pulmonary fusion. Repair of the diaphragm via the abdominal approach was difficult and the disease recurred. The second operation was through a right thoracotomy and was successful. The biopsied specimen of the diaphragm contained hepatocytes and bile duct cells which strongly suggested the close relationship between liver and the diaphragm in this case.
Right-sided, congenital diaphragmatic hernia (R-CDH) is rare compared to left-sided CDH and accounts for about 20% of the disease [1,4]. R-CDH is sometimes difficult to diagnose prenatally and Duess et al. reported that prenatal diagnosis and patch closure may be risk factors for increased mortality [4].
Furthermore, R-CDH may be complicated by some specific pathophysiological states, such as intrathoracic kidney [5,6] and hepatic pulmonary fusion [7-18], which is rare but causes complicated and difficult problems for the surgical repair of the diaphragm.
In this report, we describe a rare case with the combination of intrathoracic kidney and hepatic pulmonary fusion in R-CDH and discuss the etiology of the disease and surgical treatment.
hepatic pulmonary fusion, intrathoracic kidney, congenital diaphragmatic hernia
Abbreviations
R-CDH: right-sided congenital diaphragmatic hernia
The patient’s mother was referred to our institute at 33 weeks of gestation because her baby was suspected to have a right congenital diaphragmatic hernia. Fetal ultrasonography and fetal MRI (Figure 1a, b) were taken; R-CDH was confirmed with right intrathoracic kidney and careful follow-up was initiated. At 38 weeks and 4 days of gestational age the female patient was born at 2,780 g birth weight and intensive care was started by the neonatologists in the neonatal care unit. A plain chest X-ray showed that the right thoracic space was occupied by the right lobe of the liver and the right lung was severely compressed (Figure 1c). Ultrasound examination revealed that the right lobe of the liver was prolapsed into the right thoracic space, the hepatic veins were draining directly into the right atrium and the inferior vena cave was defective at the retro-hepatic part. The first operation was performed at 1 day old, using an abdominal approach with a right upper transverse incision. The ventral rim of the diaphragm was formed by muscle but the postero-lateral rim was composed of a very thin membrane. This part of the membrane was biopsied, the right lobe of the liver was maneuvered into the abdominal cavity and the membranous diaphragm was taken in by non-absorbable sutures. The severe pulmonary hypertension gradually subsided but artificial respiratory care was needed for one month. The liver prolapsed again into the right thorax and a chest CT was taken to confirm recurrence of the hernia and the conformation of the great vessels around the liver. The right hepatic vein drained directly into the right atrium at the level of the 9th rib (Figure 1d) and the right lobe of the liver and right kidney had again prolapsed into right thoracic space (Figure 1e). We decided to operate again to repair the hernia using a right thoracotomy. Thoracotomy was performed at the seventh intercostal space. Severe adhesion was seen between the upper and middle lobes of the right lung and the prolapsed liver (Figure 2a). After dissecting these adhesions, one striated connection was seen between the right lung and the postero-lateral part of diaphragm (Figure 2b) and a massive air leak was detected after its dissection. This structure was the right lower bronchus and airless lung tissue was found just above the postero-lateral membranous diaphragm (Figure 2c). The adhesion of this structure was severe but was dissected bluntly and a right lower lobectomy was carried out. After this procedure, the right lobe of the liver and intrathoracic kidney were easily maneuvered into the abdominal cavity. The repair of the diaphragm was carried out using Gore-texR sheet (Figure 1f). The postoperative course was uneventful and the patient was extubated.
2021 Copyright OAT. All rights reserv
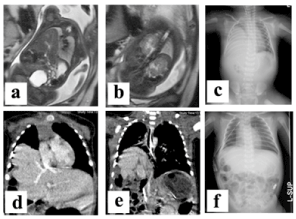
Figure 1. Images of the patient
a. Fetal MRI showing the prolapse of the right lobe of the liver into the right thoracic space.
b. Fetal MRI also shows prolapse of right kidney into the right thoracic space.
c. The chest roentgenogram taken shortly after birth. The right lung was severely compressed by the herniated liver. Mediastinal deviation was not apparent.
d. A chest CT taken when one month old shows recurrence of the right diaphragmatic hernia. The right lobe of the liver was herniated and the hepatic vein drained directly into the right atrium.
e. The right kidney also was prolapsed into the right thoracic space at one month old, by chest CT.
f. After the second operation the right diaphragm was constructed with a patch at the level of the ninth rib.
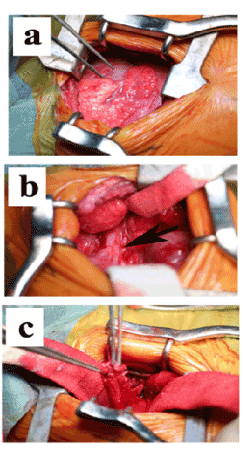
Figure 2. Operative views obtained by right thoracotomy
a. The right upper and middle lobes of the lung showed severe adhesion to the postero-lateral membranous diaphragm.
b. One striated connection was seen between the right lung and diaphragm. After dissection, an air-leak ocurred in the right lower bronchus.
c. Some tissues connecting to right lower bronchus was resected after dissecting the severe adhesion to the postero-lateral membranous diaphragm.
The final diagnosis of the patient was right-sided congenital diaphragmatic hernia with intrathoracic kidney and hepatic pulmonary fusion. Pathological examination of the biopsied membranous diaphragm revealed no detectable muscle tissue but nests of Hep-1 positive hepatocytes and keratin-7 positive bile duct cells were seen (Figure 3a, b, c). These findings suggest that some hepatic tissues had migrated into the pleuroperitoneal membrane during the early gestational age. The resected right lower lung had collapsed but was composed of a normal bronchus and lung tissues and no liver tissue was detected (Figure 3d, e, f).
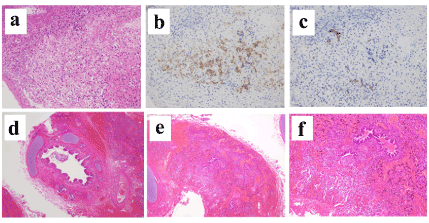
Figure 3. Pathological findings
a, Membranous diaphragm biopsied at the first operation. There was no muscular tissue but it contained some spherical cells. (HE stain, 200X)
b, The nest of Hep-1 positive cells was demonstrated by immunohistochemical staining. These cells were hepatocytes. (200X)
c, Keratin-7 positive cells were also apparent by immunohistochemical staining, which suggested the existence of bile duct cells. (200X)
d, The cut edge of the resected air-collapsed tissue was composed of bronchial cartilage and bronchial epithelium. (HE stain 100X)
e, Resected tissue at the second operation was lung tissue with air-collapsed bronchioles and alveoli. (HE stain, 100X)
f, The stronger view of the resected tissues showed bronchioles and alveoli but the invasion of the inflammation cells was not detected. (HE stain, 200X)
R-CDH is relatively rare but some characteristics, including its mortality and morbidity rates, were reported recently [1-4]. As seen in this case report, R-CDH may sometimes have rare and problematic complications.
Hepatic pulmonary fusion was first reported by Katz et al. in 1998[7] and 17 cases have been reported in the English literature [7-18]. Among these, 6 patients died and the prognosis is poor [7,8,10,13,18]. Recurrence of the hernia was experienced in many cases and well planned treatment may be needed [11-13]. Pulmonary resection or partial hepatectomy were required in some cases [8,9,11,13,16]. The absence of a mediastinal shift or ipsilateral mediastinal shift was reported as a characteristic feature of some cases [8,9] but this depends on the right diaphragmatic formation and right pulmonary hypoplasia and is not always seen [17]. Airway connection of the affected lung tissue to the right bronchus or trachea was reported in some papers [7,8,10] and, in our case, airway injury occurred in the second operation. In these complicated cases, lobectomy of the right lung or total right lung resection is mandatory to prevent postoperative complications. In addition, aberrant arteries or veins related to the right lung were seen in some cases, which suggests abnormal lung development, similar to pulmonary sequestration. In our case, the hepatic veins drained directly into to the right atrium and this suggests a close relationship between the liver tissue and the intrathoracic and mediastinal viscera. The biopsied membranous diaphragm contained small nests of hepatocytes and bile duct cells in our case and this finding was never reported before and strongly suggests the close connection of the diaphragm and liver at the early gestational age. It is quite difficult to diagnose this situation prior to surgery but several characteristics mentioned above may provide a reason to suspect the problem. In some cases, MRI or CT were helpful to detect this anomalous adhesion [9,13,14,16]. Hepatic pulmonary fusion sometimes needs pulmonary resection and, if possible, it is recommended to repair the hernia via the thoracic or thoraco-abdominal approach to attain a good operative field [11,13-15,17].
Intrathoracic kidney also is a rare variation and is sometimes seen in diaphragmatic hernia [5,6]. Right-sided hernia is more frequently complicated with this situation than left-sided hernia. This variation is usually asymptomatic and, when encountered during repair of the diaphragmatic hernia, the reduction of the kidney to the abdominal space is not difficult and usually causes little problem [5,6].
The combined complication of hepatic pulmonary fusion and intrathoracic kidney is rare and our case is the first report. In this case, the ventral rim of the diaphragm was formed by muscle tissue but the postero-lateral diaphragm was composed only of a very thin membrane and this suggested poor development of the dorsal part of diaphragm, in other words, poor development of pleuroperitoneal fusion. This malformation may have caused prolapse of both the liver and kidney into the dorsal thoracic space and finally resulted in intrathoracic kidney and hepatic pulmonary fusion at the same time, early in the gestational period.
TT, MN, KO, KT, OM, KT, TW, TH, AF contributed surgical treatment of the patient after birth, MM, OM reported pre- and post-natal image findings, HF, TF, YI treated the patient in the neonatal intensive care unit, RS, KO, SW, HS contributed the prenatal diagnosis of the patient and treatment of patient’s mother, RI, TY reported the pathological findings of the specimens obtained at surgery, YK is a corresponding author.
- Collin M, Trider S, Minutillo C, Rao S, Dickinson J, Samnakay N (2016) A modern era of right versus left sided congenital diaphragmatic hernia outcome. J Pediatr Surg 51: 1409-1413.
- Partridge EA, Peranteau WH, Herkert L, Rendon N, Smith H, Rintoul NE, Flake AW, Adzick NS, Hedrick HL (2016) Right- versus left-sided congenital diaphragmatic hernia: a comparative outocomes analysis. J Pediatr Surg 51: 900-902. [Crossref]
- Akinkuotu AC, Cruz SM, Cass DL, Cassady CI, Mehollin-Ray AR, et al. (2015) Revisiting outcomes of right congenital diaphragmatic hernia. J Surg Res 198: 413-417. [Crossref]
- Duess JW1, Zani-Ruttenstock EM, Garriboli M, Puri P, Pierro A, et al. (2015) Outcome of right-sided diaphragmatic hernia repair: a multicentre study. Pediatr Surg Int 31: 465-471. [Crossref]
- Juricic M, Cambon Z, Baunin C, Abbo O, Puget C, et al. (2016) Prenatal diagnosis of right-sided diaphragmatic hernia and ipsilateral intrathoracic kidney in a female fetus: a rare observation. Surg Radiol Anat 38: 419-423.
- Jeong BD, Ahn SH, Song JW, Shim JY, Lee MY, et al. (2016) Impaction of an intrathoracic kidney acted as a shield against herniation of the abdominal viscera in a case of right congenital diaphragmatic hernia. Obstet Gynecol Sci 59: 58-61. [Crossref]
- Katz S, Kidron D, Litmanovitz I, Erez I, Dolfin Z (1998) Fibrous fusion between the liver and the lung: An unusual complication of right congenital diaphragmatic hernia. J Pediatr Surg 33: 766-767. [Crossref]
- Slovis TL1, Farmer DL, Berdon WE, Rabah R, Campbell JB, et al. (2000) Hepatic pulmonary fusion in neonates. AJR Am J Roentgenol 174: 229-233. [Crossref]
- Keller RL1, Aaroz PA, Hawgood S, Higgins CB (2003) MR imaging of hepatic pulmonary fusion in neonates. AJR Am J Roentgenol 180: 438-440. [Crossref]
- Robertoson DJ, Harman CM, Goldberg S (2006) Right congenital diaphragmatic hernia associated with fusion of the liver and the lung. J Pediatr Surg 41: E9-10. [Crossref]
- Tanaka S, Kubota M, Yagi M, Okuyama N, Ohtaki M, et al. (2006) Treatment of a case with right-sided diaphragmatic hernia associated with an abnormal vessel communication between a herniated liver and the right lung. J Pediatr Surg 41: E25-28. [Crossref]
- Gander JW, Kadenhe-Chiweshe A, Fisher JC, Lampl BS, Berdon WE, et al. (2010) Hepatic pulmonary fusion in an infant with a right-sided congenital diaphragmatic hernia and contralateral mediastinal shift. J Pediatr Surg 45: 265-268. [Crossref]
- Khatwa U, Lee EY (2010) Multidetecter computed tomography evaluation of secondary hepatopulmonary fusion in a neonate. Clin Imaging 34: 234-238. [Crossref]
- Taide DV1, Bendre PS, Kirtane JM, Mukunda R (2010) Hepatic pulmonary fusion: a rare case. Afr J Paediatr Surg 7: 28-29. [Crossref]
- Castle SL, Naik-Mathuria BJ, Torres MB (2011) Right-sided congenital diaphragmatic hernia, hepatic pulmonary fusion, duodenal atresia, and imperforate anus in an infant. J Pediatr Surg 46: 1432-1434. [Crossref]
- Chandrashekhara SH1, Bhalla As, Gupta AK, Sharma PK, Agarwala S, et al. (2011) Hepatic pulmonary fusion: case report with review of literature. J Pediatr Surg 46: e23-27. [Crossref]
- Olenik D, Codrich D, Gobbo F, Travan L, Zennaro F, et al. (2014) Hepatopulmonary fusion in a newborn. An uncommon intraoperatory finding during right congenital diaphragmatic hernia surgery: case description and review of literature. Hernia 18: 417-421. [Crossref]
- Laamiri R, Belhassen S, Ksia A, Salem AB, Kechiche N, et al. (2016) Right congenital diaphragmatic hernia associated with hepatic pulmonary fusion: A case report. J Neonat Surg 5: 35 [Crossref]



