Context: Despite various publications demonstrating efficacy of osteopathic manipulative therapy (OMT) in neonates, no studies have formally assessed the safety of OMT in this population.
Objective: To determine the safety of OMT in term neonates (gestational age ≥ 37 weeks) and preterm neonates (gestational age ≤ 36 6/7 weeks). Safety was assessed using two mechanisms: 1) comparison of vital signs before and after OMT, and 2) monitoring for adverse events including emesis, cyanosis, apnea or decreased level of consciousness during OMT and for 30 minutes following OMT.
Methods: A prospective observational design was used to analyze pre- and post-OMT measurements of temperature, heart rate, respiratory rate and oxygen saturation. Osteopathic physicians performed an osteopathic structural exam followed by OMT using techniques such as osteopathy in the cranial field, balanced ligamentous tension and myofascial release. Adverse events were documented by a research coordinator who observed the subject directly during OMT and for 30 minutes after OMT.
Results: Thirty term and 13 preterm infants were recruited for this study. The mean gestational age at birth for the term infants was 37.8 weeks and 32.5 weeks for the preterm infants. The mean gestational age at the time of treatment was 40.0 weeks for the term population and 34.9 weeks for the preterm population. In both term and pre-term infants, the temperature decreased by a statistically significant 0.1°C following OMT. Heart rate decreased by 4 beats per minute (bpm) in term subjects and by 5 bpm in preterm subjects. Respiratory rate was unchanged in term infants and increased slightly in preterm infants. There was no change in oxygen saturations for either term or preterm infants. There were no adverse events in either group.
Conclusion: The stability of vital signs pre- and post-OMT and absence of adverse events in this study suggest that OMT is a safe intervention to perform in healthy, term neonates. However, due to lower than anticipated recruitment of preterm neonates, safety cannot be formally declared for this population.
There is a small but growing body of evidence to support the efficacy of Osteopathic Manipulative Treatment (OMT) in preterm and term infants [1-6]. Osteopathic Medicine is a comprehensive system able to both diagnose and treat somatic dysfunctions through the refined skill of manual palpation [7]. Techniques commonly used in neonates include osteopathy in the cranial field (OCF), balanced ligamentous tension (BLT) and myofascial release (MFR) [7]. Through these techniques, OMT has been shown to improve efficiency of breast feeding [6], to reduce gastrointestinal symptoms [5], and to diminish infant colic [3]. Other studies have shown decreased length of stay (LOS) in OMT treated preterm newborns [1,4] and in a multi-center, randomized, single-blind, parallel group clinical trial in Europe, use of OMT in babies born from 29-37 weeks showed decreased hospital LOS by 3.9 days in multivariate analysis [2].
Treatments such as OMT can be considered low cost and high value given that it requires no highly specialized equipment, location or support staff, is a relatively low risk procedure, and has immense potential benefits, not limited to decreased hospital LOS. Such an intervention could be of critical importance in NICUs where cost and duration of hospitalization continue to increase. Despite these trends, the implementation and routine use of OMT is widely variable; some hospitals treat every newborn admitted [8,9], while others have no OMT program or providers.
While many of the studies have reported no adverse events during OMT, to our knowledge there has not been an investigation done that specifically addresses the overall safety of the use of OMT in newborns as a primary outcome. The goal of this study was to assess the safety of OMT as a therapeutic intervention for preterm and term infants by comparing pre- and post-OMT vital signs, as well as through careful documentation of any adverse events during and after OMT.
The study was reviewed and approved by the Maine Medical Center’s Institutional Review Board (IRB) in Portland, Maine. Written and informed consent was obtained from the subject’s parent(s) prior to enrollment by an experienced research coordinator who had completed training for protection of human subjects.
Term (≥ 37 weeks) and preterm (≤ 36 6/7 weeks) infants were identified for the study through OMT consultations which are routinely ordered on a clinical basis for infants in the newborn nursery and NICU to assess issues including poor feeding, irritability, gastrointestinal symptoms or abnormal muscle tone. Infants were excluded from eligibility in the setting of critical illness, medical instability, a suspected or confirmed genetic syndrome, hypoxic ischemic encephalopathy, high grade intraventricular hemorrhage (Grade III or IV) or cystic periventricular leukomalacia.
The primary outcome of the study was a comparison of pre- and post-OMT vital signs (temperature, heart rate, respiratory rate and oxygen saturation) to establish safety of OMT in neonates. The secondary outcome was the frequency of adverse clinical events including emesis, cyanosis, apnea, bradycardia or decreased level of consciousness during treatment and for 30 minutes thereafter. The research coordinator directly observed the infant during and after OMT for these adverse outcomes. Apnea was defined as an episode of cessation of breathing for 20 seconds or longer, or a shorter respiratory pause associated with bradycardia, cyanosis, pallor and/or marked hypoxia [10]. Bradycardia was defined as below normal heart rate for age range; specifically, a normal range for infants from birth to three months ranged from the 1st percentile of 107 bpm to the 99th percentile of 181 bpm [11].
Each infant subject received one osteopathic manipulative treatment with vital signs recorded immediately pre- and post-treatment. These vital signs were done explicitly for the purpose of the investigation. Infants may have had additional subsequent OMT; such treatments were not included in this study. Vital sign measurements, including temperature, heart rate, respiratory rate and oxygen saturation were obtained by the infant’s nurse and recorded by the research coordinator. Temperature was recorded from the infant’s axilla; heart rate was recorded from 3-lead EKG monitoring along with respiratory rate and oxygen saturation. No vitals were recorded during OMT.
Prior to OMT, an osteopathic structural exam (OSE) was performed to assess the following regions: head, cervical, thoracic, and lumbar spine, rib cage, pelvis and sacrum. The infant was then treated with standard OMT techniques including, but not limited to, MFR, BLT and OCF. These techniques were implemented as described in existing OMT literature [7,12]. OSEs and OMT for this study were performed by two board certified OMM/NMM osteopathic physicians. Following treatment, the research coordinator observed the infant for adverse events. The research coordinator worked with NICU staff to coordinate OMT with daily cares. Parents were encouraged to be present for the OMT if they desired.
Descriptive statistics were used to report the clinical characteristics of the cohort. The mean heart rate, respiratory rate, oxygen saturation and temperature pre- and post-treatment were compared using a student t-test for paired samples. Pre-and post-OMT vital signs were plotted online graphs for each participant. A power calculation was performed based on retrospective vital sign data recovered from the electronic medical record for infants treated with OMT. Based on these data, it was anticipated that there would be no statistically significant difference between the pre-treatment and post-treatment vital signs. With a sample size of 27 term infants and 27 preterm infants, a paired t-test with a 0.05 one-sided significance level would have 80% power to reject the null hypothesis that the test and standard are not equivalent (i.e., that the difference in means is one half the standard deviation, or farther from zero in the same direction) in favor of the alternative hypothesis-that the means in the two groups are equivalent (i.e., the expected mean difference is 0).
The parents of 50 infants were approached for enrollment, seven of which declined to participate (all preterm infants). Infant subjects were categorized as term (n=30) or preterm (n=13) with preterm gestation defined as less than or at 36 6/7 weeks (Table 1) at the time of OMT. Five infants in the term group were born prematurely but were term equivalent age at the time OMT was performed and thus categorized as term infants. The mean gestational age at birth for the term group was 37.8 weeks and these infants were treated with OMT at a mean gestational age of 40 weeks (GA range at birth 26.3-42 weeks, four of whom were less than 35 weeks at birth). The mean gestational age for the preterm infants was 32.5 weeks with a mean gestational age at the time of treatment of 34.9 weeks (GA range at birth 26.6-35.4weeks). Sixty percent of term infants were female and 54% of preterm infants were female (Table 1).
Table 1. Demographic characteristics and vital sign parameters of term and preterm infants
GA: Gestational Age
All data is presented as mean and standard deviation unless otherwise specified.
There were no clinically significant differences in pre- and post-treatment vital signs in either the term or preterm infants (Table 1). In both groups, the mean body temperature decreased after treatment by 0.1°C. Heart rates in both groups decreased after treatment by approximately 4 bpm in term neonates, and approximately 5 bpm in pre-term infants. Respiratory rate was unchanged in term infants and increased slightly in preterm infants. No changes in oxygen saturations were observed. Pre- and post-OMT vital signs are plotted for each participant in figures 1-4. Twenty-five infants (58%) had post-OMT temperature decreases, the most pronounced being two infants with temperatures ≥37.5°C prior to treatment (Figure 1). Three term infants had heart rates (110 bpm, 112 bpm and 113 bpm) just above the first percentile cut off 107 beats per minute prior to OMT and 2 infants had heart rates of 110 bpm after OMT (Figure 2). No patterns were evident for the respiratory rate other than preterm infants tending to have slightly higher rates than term infants (Figure 3). Oxygen saturations were similar in both groups (Figure 4). With respect to adverse events, there were no observed episodes of apnea, bradycardia, emesis or decreased level of consciousness.
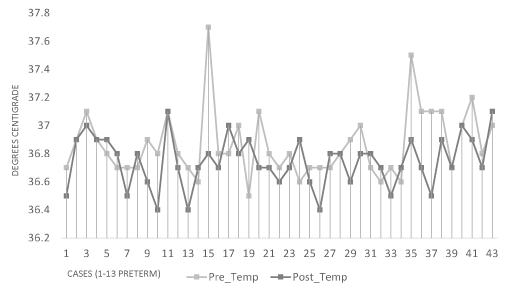
Figure 1. Temperature pre- and post- OMT
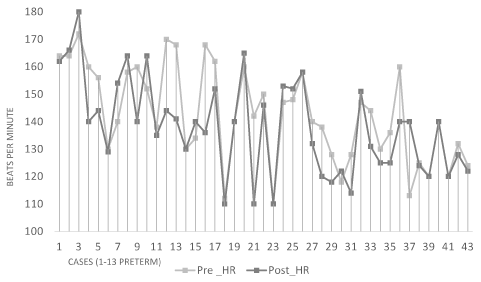
Figure 2. Heart rate pre- and post- OMT
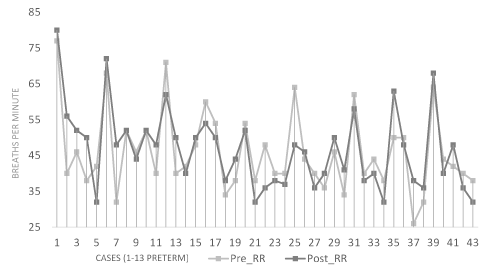
Figure 3. Respiratory rate pre- and post- OMT
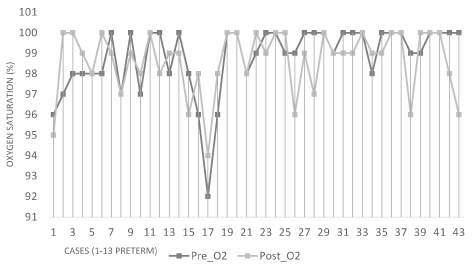
Figure 4. Oxygen saturation pre- and post- OMT
The findings of this prospective observational study suggest that OMT can be used safely in select term neonates as there were no clinically significant differences in vital signs before and after OMT, and there were no adverse events noted during or after OMT. Given the small sample size of only 13 preterm infants recruited for this study, it is not possible to state that OMT is safe in this population. However, the homogeneity of the preterm data collected does suggest that it is unlikely an additional number of infants would have altered the results in a statistically significant manner; a sufficiently powered sample size would need to be studied in order to make a more formal conclusion.
Analysis showed there was a statistically significant difference in the mean pre- and post-OMT temperature for both term and preterm infants. The mean temperature decreased by 0.1°C after OMT. While this was a statistically significant difference, we do not believe this is a clinically significant difference. It is notable that this statistical significance likely originated from the temperature measurements of two different subjects, (one from the preterm group and the other from the term group), whose pre-treatment temperatures were slightly higher than their respective cohort members but still within normal range for age (Figure 1). Regardless, it draws attention to the importance of awareness of temperature instability in the neonatal population. We would recommend that OMT providers pay careful attention to infant temperature as longer assessments and treatments could conceivably result in clinically significant temperature decreases, especially in the preterm population.
The difference of 4 bpm in heart rate for the term infant group was statistically significant, while the difference of 5 bpm in the preterm group was not. These variations were not felt to be clinically significant, especially given both mean values are well within the age-appropriate norms for pulse [11-13]. The subtle decrease in heart rate of both groups by about the same small magnitude may be attributed to the effect of OMT given the established relationship between OMT and the autonomic nervous system with a primarily parasympathetic response noted on heart rate variability after application of cervical spine myofascial release treatment [14]. The extrapolation of this hypothesis to preterm and term neonates is somewhat limited by the difference in study populations given that the study by Henley et al., was carried out in adults [14].
There were several weaknesses in this study including the use of convenience sampling (a potential source of bias) and the relatively fewer number of referrals for preterm infants; the latter led to sub-optimal recruitment of the desired study population and therefore significantly limited our ability to draw meaningful conclusions about safety in preterm infants. Additionally, detailed data about the reasons for referral and other clinical characteristics were not collected, limiting our understanding of the most common reasons for referral, medical complexity of the cohort and potentially how to improve recruitment for a future project. That said however, the results of our study represent an important contribution to the body of literature for the application of OMT in carefully selected neonates without severe illness or medical complications. To date there is only one retrospective review studying the incidence of iatrogenic events in 346 children treated with OMT which concluded that OMT “appeared to be a safe treatment modality when administered by physicians with expertise in OMT” [15]. While this study helped to address the safe use of OMT in the pediatric population, the wide age range of 1 day to 19 years limits the generalizability to term and preterm neonates. Our data, like multiple other publications, revealed no adverse events associated with OMT in either the term or preterm group [1,2,16,17]. The most comprehensive safety data found was reported in a publication by Cerritelli [7] of 695 infants looking at the effect of OMT on length of stay, in which adverse events are specifically described and notably, none were experienced by any subject.
This study demonstrates that in this stable population of term and pre-term infants, OMT was not associated with any adverse events and not associated with clinically significant vital signs changes. Though formal safety of the use of OMT in the preterm population cannot be declared due to limited number of participants in the preterm group, the results do overall illustrate OMT can be safely used in select, healthy term infants.
Authors have no disclosures of financial support or conflicts of interest to report. No grant funding was obtained for this project.
Drs. Beinlich, Beck, Bendixen and Craig provided substantial contributions to the study design, data acquisition, and analysis and interpretation of data. Dr. Beinlich drafted the article and Drs. Beck,
Bendixen and Craig revised it critically for important intellectual content. All authors have given final approval of the version of the article to be published and all authors agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
- 1. Cerritelli F, Pizzolorusso G, Ciardelli F, La Mola E, Cozzolino V, et al. (2013) Effect of osteopathic manipulative treatment on length of stay in a population of preterm infants: a randomized controlled trial. BMC Pediatr 13: 65. [Crossref]
- 2. Cerritelli F, Pizzolorusso G, Renzetti C, Cozzolino V, D'Orazio M, et al. (2015) A multicenter, randomized, controlled trial of osteopathic manipulative treatment on preterms. PLoS One 10: e0127370. [Crossref]
- 3. Hayden C, Mullinger B (2006) A preliminary assessment of the impact of cranial osteopathy for the relief of infantile colic. Complement Ther Clin Pract 12: 83-90. [Crossref]
- 4. Lanaro D, Ruffini N, Manzotti A, Lista G (2017) Osteopathic manipulative treatment showed reduction of length of stay and costs in preterm infants: A systematic review and meta-analysis. Medicine (Baltimore) 96: e6408. [Crossref]
- 5. Pizzolorusso G, Turi P, Barlafante G, Cerritelli F, Renzetti C, et al. (2011) Effect of osteopathic manipulative treatment on gastrointestinal function and length of stay of preterm infants: an exploratory study. Chiropr Man Therap 19: 15. [Crossref]
- 6. Wescott N (2004) The use of cranial osteopathy in the treatment of infants with breast feeding problems or sucking dysfunction. Aust J Holist Nurs 11: 25-32. [Crossref]
- 7. Chila AG, American Osteopathic Association (2011) Foundations of osteopathic medicine. In: 3rd ed. Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins.
- 8. Silver JH, Lorch SA, Rosenbaum PR, Medoff-Cooper B, Bakewell-Sachs S, et al. (2009) Time to send the preemie home? Additional maturity at discharge and subsequent health care costs and outcomes. Health Serv Res 44: 444-463. [Crossref]
- 9. Ettlinger H, DO, FAAO (2018) Letter from Program Director, St. Barnabas Hospital Health System, Osteopathic Neuromusculoskeletal Medicine Residency Program.
- 10. Committee on Fetus and Newborn, American Academy of Pediatrics (2003) Apnea, sudden infant death syndrome, and home monitoring. Pediatrics. 111: 914-917. [Crossref]
- 11. Fleming S, Thompson M, Stevens R, Heneghan C, Plüddemann A, et al. (2011) Normal ranges of heart rate and respiratory rate in children from birth to 18 years of age: a systematic review of observational studies. Lancet 377:1011-1018. [Crossref]
- 12. Magoun HI, Osteopathic Cranial Association (1951) Osteopathy in the cranial field. Kirksville, Mo.: Journal Printing Co.
- 13. Engorn B, Flerlage J (2015) The Harriet Lane Handbook, 20th Ed.
- 14. Henley CE, Ivins D, Mills M, Wen FK, Benjamin BA (2008) Osteopathic manipulative treatment and its relationship to autonomic nervous system activity as demonstrated by heart rate variability: a repeated measures study. Osteopath Med Prim Care 2: 7. [Crossref]
- 15. Hayes NM, Bezilla TA (2006) Incidence of iatrogenesis associated with osteopathic manipulative treatment of pediatric patients. J Am Osteopath Assoc 106: 605-608. [Crossref]
- 16. Cerritelli F, Martelli M, Renzetti C, Pizzolorusso G, Cozzolino V, et al. (2014) Introducing an osteopathic approach into neonatology ward: the NE-O model. Chiropr Man Therap 22: 18. [Crossref]
- 17. Pizzolorusso G, Cerritelli F, Accorsi A, Lucci C, Tubaldi L, et al. (2014) The Effect of Optimally Timed Osteopathic Manipulative Treatment on Length of Hospital Stay in Moderate and Late Preterm Infants: Results from a RCT. Evid Based Complement Alternat Med 2014:243539. [Crossref]




