During Muammar al-Gaddafi`s sovereignty, only little has been reported about the level of care, Libyan pediatric surgeons are able to provide to their patients and families. Thus, soon after the revolution, stakeholder families in Benghazi decided to invest more in their community health care by funding a cooperation with Western World -namely German- experts. Here, their main goal was to bring German medical standards and expertise to Benghazi, especially to their newly built and just opened up “Libyan German Hospital” (LGH) (Figure 1).

Figure 1. Entrance of the newly opened up Libyan German Hospital
Initially, no one has been considering the speciality of >>Pediatric Surgery<< to be in any way part of the agenda. Why. Because it has always been considered as being too “special” or too “complex” by all national experts and the public. However, I, the German consultant pediatric surgeon, joined the group for the first time in September 2012 with the clear attempt to provide a CHANCE to make a substantial CHANGE.
Like in all other surgical or non-surgical disciplines the initial plan has been to organize repeated short term visits on honorary basis. During these visits, daily OPD services, consultant ward rounds and pediatric surgical operations should be provided. Since the LGH is a non-governmental, fully private hospital, the treatment of accident & emergencies has not necessarily been a part of the agenda. The main focus instead should lie on elective and scheduled cases and consultations. It is in full contrast to the daily praxis in the governmental or the majority of our German children`s hospitals.
The LGH itself is a newly built and well-furnished hospital hosting a strictly separated male and female ward on the 2nd, 3rd floor, respectively. Within the female ward, next to the obstetrical department, the “baby unit” (= newborn suite) is located. This “baby unit” covers several cribs and one (transport) incubator. It is equipped with an extra heating source and a dressing table with integrated bath tab for diaper changes and newborn nursing. Through the big window on the front side, the proud parents and relatives enjoy the whole day long to have a closer look on their “new arrivals” (Figure 2). On the first floor, the central theatre area (3 major, 1 minor OR), an ICU/Recovery Room (6 beds, 1 ventilator) and the endoscopy unit (gastro- & colonoscopy) are located. In the left wing of the basement the x-ray department (CT and US availability) is found, while the right wing hosts the laboratory and the pharmacy. The OPD area in the middle is surrounded by several (specialists) consultation rooms and only a small emergency room (ER). Like in any other private hospitals in Libya, there is no defined trauma bay, ambulance car lane or triage point.

Figure 2. Welcome to the “BABY-UNIT”

Figure 3. Skills workshop accessible for all staff.
At that time, the speciality of >>Pediatric Surgery<< in Benghazi has been provided exclusively in 2 governmental institutions. Namely, the “Benghazi Children`s Hospital” and the “Benghazi Medical Center (BMC)”. The Benghazi Children`s Hospital is quite an old building out of the 60s, the BMC, indeed, is a three tower complex out of the 80s. The BMC is the official University Hospital and located within the campus of the University of Benghazi. The “Children`s Hospital” is the teaching affiliate, located right in the same street on the opposite site of the road. There is a constant exchange of staff, patients, equipment and disposables between these 2 institutions. But, for several reasons, admissions in both institutions are extremely limited in numbers and usually do not match the real needs of the Benghazi children. In the public the general reputation of both institutions and their medical staff is considered quite low in comparison to any foreign institution or foreign doctor (for whatever reason).
Regularly, Libyan pediatric surgeons work under a fixed contract in a governmental institution in the morning, while in the afternoon and evening they provide their services either in private praxis or in one or even more private hospitals. These schedules and appointments are flexible, especially for the department head and the senior consultants, making it sometimes difficult to have a fixed plan for the individual child`s surgery.
Within the private hospital sector, the necessary work permit and liability insurance coverage for the foreign doctor will be issued exclusively by the owner of the hospital himself! For the governmental sector, no verified licensing process is visible. The foreign applicant has to deal permanently with unannounced changes, and therefore the foreign doctors` applications are always in the “still pending” mode.
Libyan junior pediatric surgeons are eager to find funding and support for electives abroad, bringing them most preferably to Germany. But, they seem to be completely unaware of what they will have to face inside Germany: the language and educational barriers, the different culture and attitudes, the different health care system, and last but not least, the loss of their family and family support for quite a long time.
In comparison to Germany, >>Pediatric Surgery<< is seen different by the Libyan medical board, institutions, the associations and your colleagues. In the first instance, >>Pediatric Surgery<< is seen as the equivalent to “newborn- and visceral surgery”, exclusively. Our common subspecializations like “Pediatric Urology”, “Pediatric Orthopedics”, or “Pediatric Neurosurgery” do not even exist; neither within the Libyan pediatric surgeon nor the Libyan adult (organ) specialist associations. And, not even this already mentioned “traditional core specialization” for pediatric surgeons is well established. Even more, no rules and regulations do exist, when and how to transfer the little patient to the (adult) organ specialist. Or, what to do, when two or more organ systems, or different “specialties” seems to be “involved”. To the best of my knowledge, no standardized training curriculum or logbook has been released by any of the Libyan Surgical Associations so far.
The hierarchy within the department of pediatric surgery is unidirective: head of department, consultant surgeon, senior registrar and house officer.
Within the institution all male and female doctors should be treated and promoted equally. But, it is the Islamic tradition which rules out. Every female has to ask her (even so far only proposed) husband for permission first for any (even personal) decision she intends to make in her life! It in fact means, that none of our female doctors has been able to participate in extra teaching lessons, I offered to the candidates on a public holiday in front of their exams on personal request of the chief pediatric surgeons of the BMC. Because none of their husbands has given permission! Thus, only the male candidates finally got the benefit.
Most of the Libyan female nursing or health care staff fail to come in at the right time in the morning. And, they will even have to leave the hospital quite early in the afternoon, because their fathers and heads of family still think, that they are “unsafe in town” after Gaddafi`s sudden dismiss. And this is despite the fact, that they are always picked up or dropped at the front door by the same drivers of their families like every day before in the past. Almost all families express such a feeling of “unsafeness”, when being asked for the times before the revolution. But nobody was able or willing to explain or to discuss this in more details.
Right from the beginning, all Libyan colleagues constantly assured us, that “Libyan doctors are never ever “envious” or “emulous” of someone of their colleagues”, and that they are “eager to learn and always cooperative and compliant”. However, I personally have had a different feeling based on the following examples.
A honourable visiting German ENT professor intended to perform a complex larynx tumor resection in our LGH. One of our Libyan junior doctors has been offered to assist him with this case. But the junior doctor refused completely, because he did not want “to be asked any questions during the procedure”. And, he has been totally self-convinced to “already know everything about such cases!”. In addition, he told us, that he “aspires specialization in ophthalmology”, meaning that he “did not want to waste time with ENT cases ……”. (NB: Later on his dream became true. After he has (been) separated (via SMS) from his former girl friend, he could get engaged with the single daughter of the one and only Libyan professor of ophthalmology !).
Despite all personal “invitations”, none of the LGH house officers never ever joined me during my daily ward rounds. The only action they have been taken was to tell the nurses to call me in, if they intended to face a “problem”, or, even more likely, just because of the insisting request of the child`s parents and relatives “to see the German doctor”.
In due course several pediatric fracture cases have been presented in the ER and finally admitted to the ward. For sure, I would have been the most senior experienced person in these cases, but the chief orthopedic surgeon did not allow any interprofessional discussion to be started. He rejected any advice, and relied strictly on the (antiquated) Medical Association`s professional code of conduct: “pediatric fracture treatment is NOT within the scope of pediatric surgeons in Libya!” Thus, the only thing I could do is to take care of a good pain relief, make prescriptions for appropriate infusion regimens and keep on trying “to prevent doctors from doing things, that should better not be done”.
In conclusion, during my entire 2 years of service there has never been the right time or CHANCE for an open interprofessional discussion to make a substantial CHANGE on these traditional and cultural based (medical) issues and attitudes.
The general attitude of Lybian patients and parents towards medical decision making is driven by the dogma: “never trust in medical systems and medical doctors”. The worth of, respectively the right for a second opinion is completely unknown. Medical education and (individual) body knowledge within the families are still only rudimentary. And, “everything” is deeply influenced by “inschallah” and their muslimic culture and not by “Western medical science”. Their real personal insight into common illnesses and diseases, possible treatment options or plans, as well as their natural courses is still extremely low. And, last but not least, any final decision about treatment or non-treatment of a family member or child will be made exclusively by the patriarch and never ever by the patient or his/her parents alone like in our society. However, even in real emergencies this can take quite a long time and might not be even straight forward and conclusive from our point of view!
Like anytime in the past, treatment in governmental hospitals in general has been free of charge respectively has been paid for by the government in almost all cases. In a private hospital and private practice, on the other hand, the family have to pay for everything in “cash” and “well in advance”!
Nevertheless, there is an overall constant and never ending complaining about everybody and everything within the Libyan health care sector. Most likely due to the fact, that so far >>health care<< has just been “provided” by the authorities, making it “unnecessary” and maybe “impossible” for the individual to develop his or her individual responsibility for his or her personal health and well-being.
Therefore, the majority of Libyan families are (still) in big favour for “medical tourism” to their neighbouring Arabic speaking countries like Egypt, Jordan or Tunesia. From my point of view, much too often they returned back with highly questionable results, inappropriate (not - documented, even fake-!) surgeries done, and obviously unmet patient`s/parents` expectations. Not to forget, the already fixed but “unnecessary” follow-up visits in the future, meaning in fact the complete loss of their money for all the charges! In addition, quite often the medical report has been written in French and not Arabic language (mother tongue!) creating another (unnecessary) costs for re-translation back home, because Libyan authorities still do accept only Arabic or English paperwork!
However, and as already mentioned above, the Libyans keep on going to expect from any of their “acting“ government the provision of medical care free of charge for everybody and everything. Most preferable, including the private sector as well! Like it has been in the past, no matter if it has been during Gaddafi`s regimen or after the revolution.
That´s why the Libyan public has forced their acting “government” and politicians to set up a program, that will cover all treatment costs in general. Regardless, if a civilian or military personal or just an innocent child will be the insurant. Because, they still live in the understanding, that “everything” regarding their medical problems has its roots in the civil war and its sequelae. Thus, once their “diagnosis” will be “covered by this program”, the Libyan Health Government will have to release money (out of Gaddafi`s treasure) for all the insurant`s treatment costs, the family expenses and a surplus. Most preferable abroad! Then, from the Libyan perspective most Western countries did it the same by organizing thousands of med evacs of “warriors/patients” into their countries and by treating them like “VIPs and for free” there. All financed by money, that has been taken from Gaddafi`s treasures hidden wisely abroad after his dismiss and death. For sure, the Libyans might not be able to understand the real insight and the background of such Western actions, but of course, they would like to have the benefits out of such a “program”. Regardless of the reasons! And they are all still believe, that “Gaddafi`s hidden treasures” have to be considered as “their” money.
The once and only requirement for participation in this program has been the presentation of an expert letter signed in favor for it by a “Western doctor”. None on either side, of course, should have a closer look, if indication, diagnosis, history and cause are checked and approved! In fact this means, that all parents and relatives have been approaching me, the German pediatric surgeon, insisting that their beloved child have to enter this governmental program to be protected and finally a 100% cure in Germany. Regardless of the underlying (from the Western viewpoint) “correct” diagnosis like ie. congenital malformation, common illness and/or acute or secondary surgery. And, last but not the least, we all know for sure, that they are hoping for a surplus on the foreign treatment costs, a surplus this family might have to live from for quite a longer time after returning to Libya!
This complete trust and their overall expectations in us, German doctors, and the German healthcare system, are out of any reach and totally excessive. Never ever they could be met by a sincere medical doctor. But how could you educate your patients/parents and their families about such medical facts? Like, ie. that not in every case a 100% cure is possible, regardless of the surgeon, regardless if he or she is from Germany or from somewhere else. Why the Western countries have undertaken these med evacs, and what have been the real results out of such a/their own “medical tourism”? Especially, when considering the fact, that in the past every medical treatment has just been “provided for free”, and any “decision” has just been made by a non-medical official instead of the individual himself. And, last but not the least, the political situation and cultural issues in the past did not allow for any self-education of these families.
Trying to educate all the parents and families of my little patients about the “Western point of view” and its medical and scientific background have been the most challenging task of this (my) project. The key issue has been enableing them to make their real own and unbiased decisions. However, to be pretty honest, I am not able to say how successful and sustainable it finally was.
In the second half of the year 2013 a “new health insurance system” has been launched in the Benghazi region. But only the employees of big oil companies or foreign entrepreneurs could be coveredand the insurance proceeds and benefits have been reported as being too less transparent. Vice versa, according to the insurers party payment of the contribution rates by their insurants have been missing or have been too unreliable most frequently as well. And, last but not the least, the hospital accountant has been complaining constantly, that definitive payment of the hospital bill by the partnering insurance company after complex surgeries has never been for sure, despite a confirmed calculation as well. However, regardless if happening in the “old” or “new” (health care) system, when it comes to reality every medical treatment outside the governmental sector still has to be paid in cash, anyway.
In summary, it means that actually the needs of the majority of Benghazi`s children have not been met and that only a very small and pre-selected minority have appropriate access to modern and progressive pediatric surgery.
Every medical education, specialist training or the use of advanced technologies have been restricted over the last decades for all Libyan doctors due to their political situation and various cultural issues. The majority of nursing and physician assistance staff, indeed, is usually hired abroad and therefore “multinational”, “multilingual” and “multicultural” with a lot of different training curricula, medical standards and cultural issues involved. And, last but not least, “issues” regarding the group of senior consultant specialists from Germany have to be taken into consideration as well. To overcome all these issues and starting a CHANGE have been a (my) major task of this project.
Despite the skepticism of the local hospital management I promoted and engaged right from the beginning in a continuous and well adapted educational program in nursing essentials accessible to all staff (Figure 3). This lecture series has been covering topics like “hygiene”, “catheters and iv lines”, “assessing patients” or “dressing wounds”, among others. Shortly thereafter, a more specialized and focused program for the nurses signing in for the pediatric patients either on the ward or in the OT followed. After participation each participant received credits and his/her certificate out of the hands of the board of directors. This program has been highly appreciated by the patriarchs of the families as well. They often attended the handing over ceremony of the certificates and asked proudly for the individual progress of their daughters.
Since we all had a different mother tongue, all translators and interpreters have been involved right from the beginning in “patient assessment” as well (Figure 4). Some of them did have a medical background already (final year medical students), others did not (linguistic or art students). For the non-medical ones a brief introduction in medical terminology has been provided. At this stage I have to learn the lesson, that informed consent of the patient is gender-sensitive in the Arabic culture. Meaning in fact, that a female translator is not allowed to deliver several medical facts to a male patient and vice versa. Or, that delivering certain (“bad”) diagnoses to the patient directly instead of delivering them first to the patriarch of the family is inappropriate as well. New perspectives that I have had to consider immediately in my present and future counselling and communication with my little patients and their parents!

Figure 4. Aisha (r), final year medical student & translater, Nasreen (m) pediatric nurse, Dr Fette (l) pediatric surgeon = the Pediatrics TEAM
For sure it takes a lot of efforts to bring all these different learning attitudes together and to build up a new culture of learning together and from each other. But, we succeded and it deemed to come out as a success. But real sustainability could not be achieved, since I has been the only one who has been “constantly” engaged in this training and educational program.
After my first personal contact with the heads of the 2 local governmental pediatric surgical centers, we decided to start a “new” pediatric surgical collaboration.
First, a list about their most interesting cases have been submitted by all senior pediatric surgeons to enable all junior doctors to have a closer look or to attend these surgeries or consultations or rounds on a rotational basis. Regardless of the hospital the patient has been admitted to.
Second, whenever possible all complex cases out of the Benghazi area have been seen and operated on by all chief pediatric surgeons together in a TEAM-approach. Regardless of the hospital the individual patient has been admitted to.
Last but not the least, I designed and provided a lecture and bed side teaching series to enable a group of registrars to prepare for their master exams. The aim was to held these exams in Benghazi again after several years of civil war in order to give the candidates the opportunity to make the next step in their professional career. The teaching period as well as the exam has been divided in a theoretical and practical part like in many other countries. In addition, each candidate`s surgical logbook listing all procedures he/she has already done so far has been considered in detail, too.
As a member of the board of examiners, I am proud to say that all candidates have passed their exam with remarkable results. However, I have had to learn my lesson how to pick up the individual candidate in a culture-sensitive manner based on his/her personal background while still providing a fair and constant examination process for the entire group.
The chief anesthetist of Benghazi area has had some training in a German Heart Center recently and therefore a lot of experience in anesthetizing even small infants safely. This enabled us to do (scheduled) newborn surgery in a private hospital in Libya for the first time ever, starting even straight from my first visit (Figure 5).
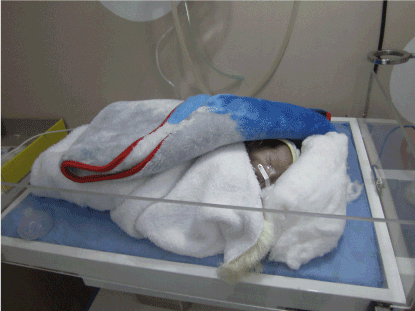
Figure 5. First newborn surgery performed in the private sector (in the LGH)
In due course we started to perform laparoscopic pediatric surgery (ie. appendicitis, inguinal hernia repair) in good cooperation within the LGH, after borrowing the instruments from the general surgery department. The main problem has been the maintenance of the laparoscopic equipment and the higher charges which have to be paid for this type of surgery within the private health care sector. However, all kinds of modern minimal invasive techniques have been highly appreciated in general within the public and among all staff.
Since >>pediatric surgery<< has been the “orphan speciality” within the medical system and the mind of the public in Libya in the past decades, many children have just been presented because of the (physical) presence of the “German doctor” and with no surgical problem at all. With long lasting patience and step by step education of, first, the hospital staff and second, the patients` families more and more (Western style) informed consent has been possible and more and more families could have been convinced to undergo and trust in their necessary surgeries. It in fact means that the number and ratio of pediatric patients with a clear indication for a surgery = “real” pediatric surgical patient out of all pediatric patients increased gradually and constantly. And that the number and ratio of these “real” pediatric surgical patients finally undergoing their particular surgery increased gradually and constantly over the time, too (Figure 6, Graph 1). In due course, more and more children with diagnoses out of the pediatric surgical subdisciplines could have been treated and operated on as well. For details see Graph 2.
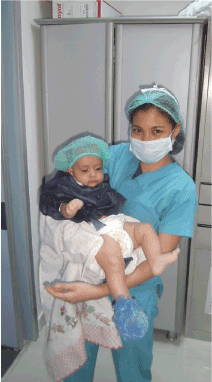
Figure 6. Inguinal hernia patient awaiting his surgery.
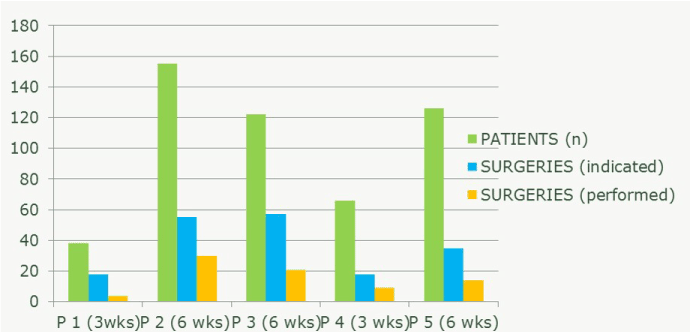
Graph 1. Correlation between number of pediatric surgical patients, indicated and performed surgeries.
2021 Copyright OAT. All rights reserv
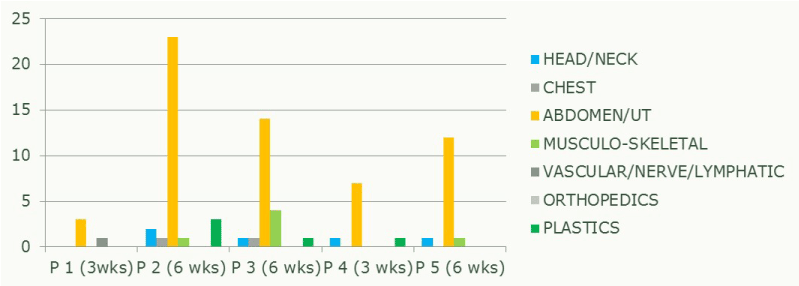
Graph 2. Numbers of surgeries performed in the pediatric surgical subdisciplines.
Performing ultrasound bedside to make the findings more visible has been of great value for all patients, parents and the medical staff. Occasionally, our lady radiologist joined us in these investigations to get more experience herself. When there have been no patients waiting, several staff members became interested in having a “secret” look in their own bodies.
After quite a long time, contrast enema diagnostics of the intestine has been re-invented in Benghazi`s pediatric medicine making specific diagnosis of constipation or large bowel disorders possible again. Despite a numerous potential patients providing this investigation for the Benghazi children has only been possible, when you have been willing to keep supplies coming. It in fact means bringing them in your own hand luggage from Germany. Because none of the locals is willing to organize ie. barium or the necessary disposables. Nursing staff usually has been flinching in providing any care in this field. Training and skills have only been rudimentary. However, our better diagnostic options and results have been the reason for our increasing number of surgeries out of these subspecialties. For details see Graph 2. This trend has been substantial throughout all my visits.
Shortly after the hospital staff and their families learned more and trusted more in the big portfolio (Western style) general pediatric surgery could offer, a real CHANGE could be observed. The “new” information has been shared and discussed extensively within the families and the CHANCE for a better pediatric surgical care of their kids by utilizing it is highly appreciated.
As soon as everybody recognized how important “transparency” and “respect” are, a (my) transparent and respectful leadership formed the basis for a CHANGE in the interprofessional attitude of communication among all staff. By living it, this CHANCE for better team formation has been highly appreciated.
These two points should also be seen as a CHANCE for better “medical compliance” and more “systematic medical decision making”. However, no significant CHANGE in attitude could be observed.
In conclusion: within my approximately 2 years of providing German pediatric surgery service in Benghazi, a lot of CHANGES have been seen. But, since some have been more sustainable than others, we have been preparing to go a long way for a final success. However, due to the sudden resurgence of fighting, no further engagement has been made possible.








