Case report
A 64-year old pleasant man with history of gastroesophageal reflux (GERD) was planning to undergo a shoulder surgery. His preoperative ECG was abnormal with inverted Ts infero-laterally. He had no history of hypertension, hypertensive heart disease, coronary artery disease or any other significant cardiac or neurological disease. His treadmill exercise stress test did not produce any chest pressure, chest pains, palpitations, arrhythmia or any ST depression or elevation. However, his ECG showed upright T waves infero-laterally during and post-exercise (a phenomenon called 'pseudonormalization' of T waves).
After recovering from his uneventful shoulder surgery, he returned for follow up with a myocardial perfusion imaging to assess it further whether those pseudonormal T waves were representative of ischemia (perfusion defects) or simply a non-specific and benign finding. His nuclear stress test was normal and did not show any perfusion defects. His LV systolic function was preserved by Gated SPECT.

12-lead ECG at rest: Figure 1. Infero-laterally inverted Ts
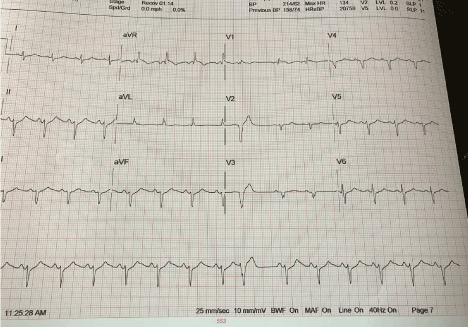
12-lead ECG during and after exercise: Figure 2. Infero-laterally upright Ts.
Introduction
In patients with inverted T waves at baseline, the evolution of an upright T waves during exercise ('Pseudonormalization') has been considered to represent ischemia by some experts [1-3], however others believe it to be non-significant [4,5].
In addition, the development of pseudonormalization of T waves after recent myocardial infarction has been controversial as well during treadmill exercise [6], during spontaneous angina [7] or while Holter monitoring [3]. It has been shown before that exercise-induced ST-segment elevation in infarct-related leads is almost invariably associated with the presence of metabolically active myocardium, however the relationship between these ST and T changes during exercise and LV function recovery is unclear [8].
In one study, low dose dobutamine stress echocardiography was performed in patients with Q-wave myocardial infarction and it was reported that the contractile reserve was higher in the area with T wave pseudonormalization or ST-segment elevation that those area without any changes on the ECG [9]. Similar findings were reported by Mobilia et al [10] stating that these ECG changes were the markers of viable myocardium and that was corroborated by PET (positron emission tomography). However, another study by Bodi et al [11] did not find any strong relationship between the ECG changes (ST-segment elevation and T wave normalization with treadmill) and functional recovery.
Therefore, the implications of these treadmill ECG changes remain controversial and inconclusive.
Discussion
Is it a sign of myocardial ischemia?
Pseudonormalization of T waves was initially described in 1970s when continuous ECG recordings became available [12]. It was 1st reported by Maseri et al [13] that the T-wave pseudonormalization was directly related to transmural myocardial ischemia. Thallium scintigraphy performed during anginal episodes at rest in patients with patients with T-wave pseudonormalization revealed a significant reduction of Tl201 activity in the myocardial region corresponding to the location of the T-wave changes [7]. Coronary angiography in similar circumstances with T-wave pseudonormalization revealed severe but reversible coronary occlusion and that was also corroborated with the perfusion defects on a nuclear scan. At times, pseudonormalization of T waves may be the only ECG change seen during acute myocardial ischemia, however it can also be an early sign of preceding ST-segment elevation as shown in a small study [14].
A study by Pizzetti et al [15] early on has shown that in patients with recent anterior myocardial infarction, exercise-induced T-wave pseudonormalization is often associated with residual perfusion to the infarct area and predicts recovery of ventricular function. In addition, if there is ST-segment elevation with exercise in these patients, it connotes the presence of myocardial viability in a region perfused by a vessel affected by a critical residual stenosis.
Mechanisms of pseudonormalization of t-waves
The exact mechanism of T-wave pseudonormalization is not fully understood. The electrophysiologic basis for its occurrence could be the superimposition of acute myocardial ischemia over chronic ischemic injury and thereby affecting the myocardial action potential and leading to these repolarization changes [16]. In addition to myocardial ischemia, it could be the passive stretching of the infarcted area by nearby viable myocardium causing these ECG changes. Alternative explanation for these T-wave changes could also be the partial denervation of the infarct area interrupting sympathetic and vagal fibres going through the necrotic area [17].
Another mechanistic issue with these T-waves: NSTEMI: that is when a patient with chest pains with NSEMI presents, he/she could have inverted Ts inferolaterally. These inverted Ts are known as 'reperfusion' T waves. Similar T waves in anterior leads are known as "Wellens' T waves." [18]. The presumed theory is that when the perfused coronary artery re-occludes, the inverted T waves can become upright.
There has been one study reporting the value of these T-wave changes and its implications to the diagnosis of apical hypertrophic cardiomyopathy [19]. There were 2 male patients otherwise asymptomatic with inverted Ts on their resting ECG, T-wave pseudonormalization on a treadmill, unremarkable echocardiography and the diagnosis finally confirmed by cardiac MRI.
Conclusion
The importance of T-wave pseudonormalization remains unclear. There are studies showing its implications in the diagnosis of ischemic heart disease, viable myocardium and re-occluded perfused coronaries. On the other hand, many studies have shown these ECG changes to be non-specific findings and having no relationship with ongoing ischemia.
There is a rare possibility of these findings leading to the clue and diagnosis of apical hypertrophic cardiomyopathy.
In summary, we need to pay very close attention to the history and the symptoms of the patients and these changes to be taken under consideration accordingly.
References
- Yu PNG, Soffer A (1952) Studies of electrocardiographic changes during exercise (modified double two-step test). Circulation 6:183-192.
- Bellet S, Deliyiannis S, Eliakim M (1961) The electrocardiogram during exercise as recorded by radioelectrocardiography: comparison with the post-exercise electrocardigram. (Master two-step test). Am J Cardiol 8: 385-400.
- Noble RJ, Rothbaum DA, Knoebel SB, McHenry PL, Anderson GJ, et al. (1976) Normalization of abnormal T waves in ischemia. Arch Intern Med 136: 391-95. [Crossref]
- Linhart JW, Turnoff HB (1974) Maximum treadmill exercise test in patients with abnormal control electrocardiograms. Circulation 49: 667-672. [Crossref]
- Aravindakshan V, Surawicz B, Allen RD (1977) Electrocardiographic exercise test in patients with abnormal T waves at rest. Am Heart J 93:706-714. [Crossref]
- Marin JJ, Heng MK, Sevrin R, Udhoji VN (1987) Significance of T wave normalization in the electrocardiogram during exercise stress test. Am heart J 114:1342-1348. [Crossref]
- Parodi O, Uthurralt N, Severi S, Bencivelli W, Michelassi C, et al. (1981) Transient reduction of regional myocardial perfusion during angina at rest with ST-segment depression or normalization of negative T waves. Circulation 63: 1238-1247. [Crossref]
2021 Copyright OAT. All rights reserv
- Margonato A, Chierchia SL, Xuereb RG, Xuereb M, Fragasso G, et al. (1995) Speficity and sensitivity of exercise-induced ST-segment elevation for detection of residual viability: comparison with fluorodeoxyglucose and positron emission tomography. J Am Col Cardiol 25:1032-1038. [Crossref]
- Lombardo A, Loperfido F, Pennestri F, Rossi E, Patrizi R, et al. (1996) Significance of transient ST-segment changes during dobutamine testing in Q-wave myocardial infarction. J Am Coll Cardiol 27: 599-605.
- Mobilia G, Zanco P, Desiseri A, Neri G, Alitto F, et al. (1998) T wave normalization in infarct-related electrocardiographic leads during exercise testing for detection of residual viability. J Am coll Cardiol 32:75-82.
- Bodí V, Sanchis J, Llàcer A, Insa L, Chorro FJ, et al. (1999) ST-segment elevation on Q leads at rest and during exercise: relation with myocardial viability and left ventricular remodeling within the first 6 months after infarction. Am Heart J 137: 1107-1115. [Crossref]
- Haiat R, Halphen C, Derrida JP, Chiche P (1977) Pseudonormalization of the repolarization during transient episodes of myocardial ischemia. Am Heart J 94:390-391. [Crossref]
- Maseri A, Severi S, Nes MD, L'Abbate A, Chierchia S, et al. (1978) Variant angina: one aspect of continuous spectrum of vasospastic myocardial ischemia, pathogenetic mechanisms, estimated incidence and clinical and coronary arteriographic findings in 138 patients. Am J Cardiol 42:1019-1035. [Crossref]
- Chierchia S, Brunelli C, Simonetti I, Lazzari M, Maseri A (1980) Sequence of events in angina at rest: primary reduction in coronary flow. Circulation 61: 759-768. [Crossref]
- Pizzetti G, Montorfano M, Belotti G, Margonato A, Ballarotto C, et al. (1998) Exercise-induced T-wave normalization predicts recovery of regional contractile function after anterior myocardial infarction. Eur Heart J 19: 420-428. [Crossref]
- Simons A, Robins LJ, Hooghoudt TE, Meursing BT, Oude Ophuis AJ (2007) Pseudonormalisation of the T wave: old wine? A fresh look at a 25-year-old observation. Neth Heart J 15: 257-259. [Crossref]
- Smith S (2009) Pseudonormalization of T waves, coronary occlusion without 1 mm ST elevation. Dr Smith's ECG blog.
- Kang S, Choi WH (2013) Pseudonormalizatrion of negative T wave during stress test in asymptomatic patients without ischemic heart disease: a clue to apical hypertrophic cardiomyopathy? Cardiology 124: 91-96. [Crossref]
- Barber MJ, Mueller TM, Davies BG, Gill RM, Zipes DP (1985) Interruption of sympathetic and vagal-mediated afferent responses by transmural myocardial infarction. Circulation 72: 623-631. [Crossref]


