Study design: A non-randomized control study in a rehabilitation center.
Objectives: To investigate effectiveness of RehaCom cognitive rehabilitation software compared to creative activities program in neuropsychiatric parameters in patients with cognitive deficits due to acquired central nervous system disorder.
Background: Impairment in cognitive function is common in patients with acquired brain injury and influences negatively the rehabilitation outcome.
Methods/Measures: The study included 96 subjects with different neurological conditions: cerebrovascular accident, hemiplegia, multiple sclerosis and traumatic brain injury. Fifty-six patients participated in the RehaCom cognitive rehabilitation program. Controls performed a program of creative activities. Both groups participated in a comprehensive rehabilitation program including physical therapy, occupational therapy and psychological support. In admission and at discharge a cognitive skill evaluation was performed in the patients of both groups based on the Montreal Cognitive Assessment (MoCA) psychometric screening test.
Results: The average RehaCom intervention participation time was 115 ± 70 days. It was observed that the treatment group MoCA score upon exit was statistically significantly higher than upon admission in assessment tasks of attention and concentration, reaction behavior, visuo-constructive ability, verbal memory, topological memory, visuo-motor coordination and exploration, compared with the control group (p<0.001). The sub-group that seemed to have derived the most advantage is the CVA, Right Hemiplegia.
Conclusion: Computerized cognitive rehabilitation with the RehaCom program results in improvement in cognitive function and can be used as a treatment tool beneficial to patients presenting cognitive impairment.
cognitive rehabilitation, rehacom, brain injury, montreal cognitive assessment
Cognitive rehabilitation is the collective label for a wide range of therapeutic interventions [1]. Their purpose is to reduce the adverse effects that cognitive impairments have on every aspect of a person’s life. In most countries cognitive rehabilitation is provided by psychologists and occupational therapists or their assistants, although other professionals are also involved [2]. According to the literature in subjects with brain injuries cognitive rehabilitation may improve recovery from neuropsychological impairment. From this view, neuropsychology is a part of rehabilitation procedures encompassing both assessment and treatment of sequelae [3,4]. The important issue is that cognitive impairment is common in patients with acquired brain injury and influences negatively the rehabilitation outcome. The aim of the study was to investigate effectiveness of RehaCom cognitive rehabilitation software compared to creative activities program in neuropsychiatric parameters in patients with cognitive deficits due to acquired central nervous system disorder.
The study took place in a Rehabilitation Centre and included patients (men and women, 2:1) with 4 different neurological conditions: a) cerebrovascular accident (CVA) with left hemiplegia, b) CVA right hemiplegia, c) Multiple Sclerosis (MS) and d) Traumatic Brain Injury (TBI). Subjects were divided in 2 groups: control (A) group (n=41) and RehaCom cognitive rehabilitation software intervention (B) group (n=56) (mean age: 51.7 years, range: 20-79 years) (Figure 1). The intervention group participated in the RehaCom cognitive rehabilitation software program, whilst the control group in a creative activities program. Subjects who followed creative activities program were enrolled for 40 minutes, 4 times per week, in a program based in activities including games, memory tests, reading, discussing the news, music, cooking etc. Both groups followed a rehabilitation program based on their needs (physical therapy, occupational therapy, psychological support), in addition to the creative activities or RehaCom intervention. Each subject was interviewed and clinically examined by the last author (EK) according to a baseline personal data questionnaire based on anthropometric and clinical information. The protocol was designed according to the Declaration of Helsinki and approved by the local ethics Committee. All subjects gave written informed consent to be included in this study. Upon their admission, a cognitive skill evaluation was performed in the patients of both groups based on the Montreal Cognitive Assessment (MoCA) psychometric screening test which is validated for Greek population (Figure 2) [5,6]. The MoCA test is a short in duration (10–15 min) 30-point screening test that measures a number of cognitive domains such as visuospatial abilities, executive function, short-term memory, attention/concentration, language, abstract thinking, and orientation [7-9].
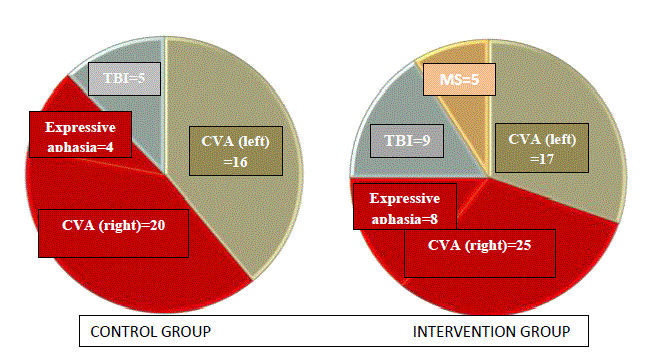
Figure 1. Participants according to diagnosis in control and intervention group
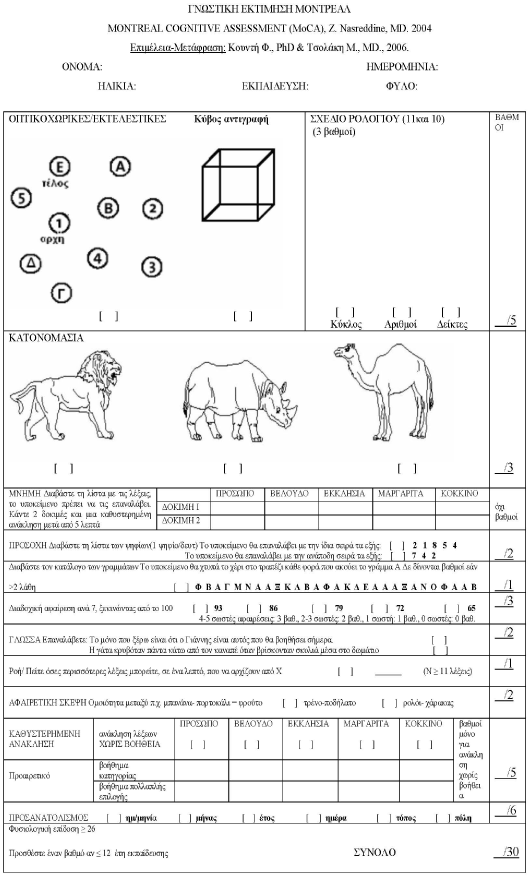
Figure 2. Greek version of Montreal Cognitive Assessment. Edited and translated in Greek by Kounti F. and Tsolaki M., Greece 2006
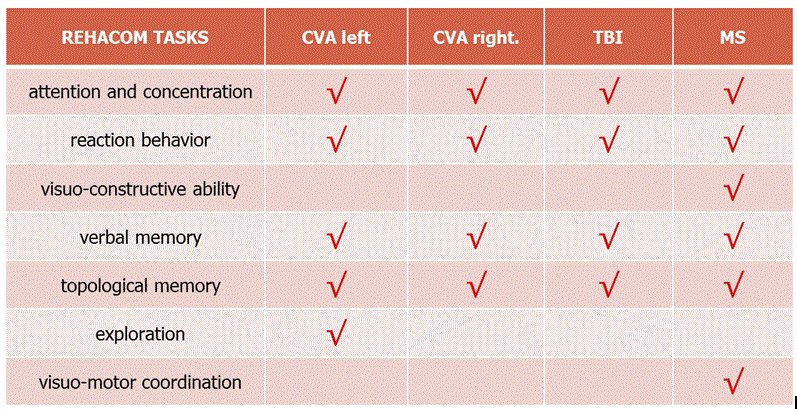
Patients included in the intervention group patients attended RehaCom program (www.rehacom.gr) sessions of neuropsychological intervention for 30 minutes, 3 times per week for >3 weeks mean 123 days (range 30-372). The RehaCom program has 20 different therapeutic activities to improve cognitive function disorders in attention, perception, memory, executive functions, etc. Specific activities were selected, depending on each patient’s deficit, as follows: attention and concentration (n=42), reaction behavior (n=45), visuo-constructive ability (n=6), verbal memory (n=30), topological memory (n=33), visuo-motor coordination (n=9) and exploration (n=30) (Table 1). For more information about these tests please see here [10]. During the first session of an activity, the patient started from minimum level of difficulty, whilst consequently, the program itself adjusted and increased automatically the level, depending on the patient’s answers in the activity tasks. In each of the following sessions, the patient would continue from the level he had reached. The software automatically adjusts the difficulty level of each session on the basis of performance and recorded numerous individual performance parameters. The therapist was case-by-case, encouraging or instructional. Finally, a psychometric reevaluation followed on, using the MoCA test by a specialized psychologist (AP). As an additional rehabilitation progress measure, the modification of the last session’s level of difficulty was evaluated compared to the one of the first session for each activity. Statistical analysis of the data was performed using the SPSS version 20.0 (SPSS, Inc., Chicago, Illinois). All subjects’ characteristics were quantitative variables and they were expressed as the mean ± standard deviation. Descriptive statistics were used (percentage, mean and standard deviation). To assess intervention effect, differences between pre- and post-training measures of attention and concentration, reaction behavior, visuo-constructive ability, topological memory, visuo-motor coordination and exploration test performance were analyzed using the Student t test. All tests were two tailed and statistical significance was considered for p<0.05.
Table 1. Rehacom tasks used in this study according to the disease.
The average RehaCom intervention participation time was 115 ± 70 days. It was observed that MoCA score in the intervention group B on discharge was statistically significantly higher than admission (p<0.001), while in controls of group A was not, presenting a 4.3-point and 1.2-point increase in their MoCA test at the end of their hospitalization, respectively. Patients reached a significantly higher level of difficulty in all tasks during the last session compared with initial appointed level by the therapist, with the highest degree of improvement found in activities of attention and concentration and exploration presenting a 5.7 and 5.2 increase respectively (p<0.05). Similar trends of improvement were found in secondary parameters (reaction time, number of mistakes, data non shown).
Regarding the intervention group evaluated with MoCA (n=48), 45 of them had at least a 1-point improvement, whilst only 1 was static and 2 patients had a -1 and -2-point decrease in MoCA score respectively, without however a change in their cognitive rating.
Patients who started with a low MoCA score benefited more from exercising with the RehaCom program. The level of difficulty that the patients reached in the last session was significantly higher than the one at the beginning, with the increase for each activity depending on the type of the patient’s cognitive disorder. A similar increase trend was observed for the separate performance parameters (ex: reaction time, number of mistakes, etc.), which are not presented in this text.
The sub-group that seemed to have derived the most advantage is the CVA, right hemiplegia (average MoCA score increase: 6 points), following the TBI (4.3-point increase). Particularly subjects with cerebrovascular accident (CVA) and right hemiplegia (and expressive aphasia) were able to follow a simple command upon entering the program (none of the 4 control group patients with CVA could follow a complex command), whereas in the end, only 1 could successfully follow a complex command, while in group B (only 1 of 8 subjects had the ability to follow a complex command upon entering the program, 12,5%) after the end of the intervention the rest 7 subjects were capable of successfully following a complex command (100%), meaning the 100% successful rate of the intervention in this group was 100% vs. 25%, p<0.001) in our study.
The increase of the difficulty level upon exit for each activity had a positive correlation with the exit MoCA difference. The highest correlation arose from the activity “attention and concentration“(matching images) (p<0.05) (Figure 3).
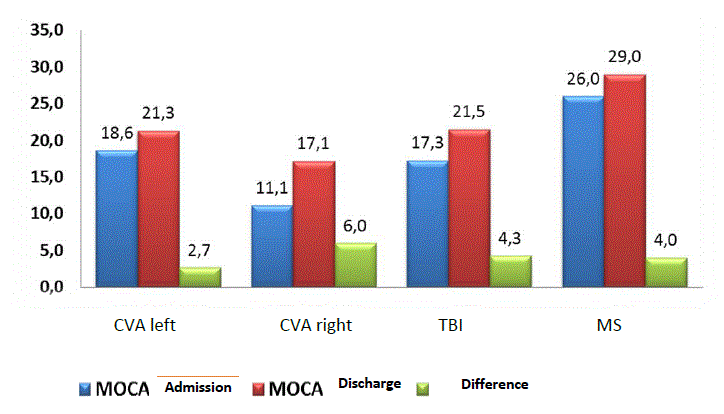
Figure 3. Statistical significance according to the disease: p<0.001 CVA (left and right), p<0.05 TBI, p<0.001 MS
All subjects were improved according to MoCA parameters after the employment of RehaCom cognitive rehabilitation software compared to creative activity program. The sub-group that seemed to have derived the most advantage is the CVA, right hemiplegia. As far as the patients with expressive aphasia are concerned, all of them managed to follow a complex order by the end of RehaCom program. The increase of the difficulty level upon exit for each activity had a positive correlation with the exit MoCA difference, meaning that a patient’s increased performance in a specific activity, accompanied the equivalent cognitive functioning increase.
The present study is in line with former studies showing that although there was no statistically significant difference in cognitive ability between the training group and control group in each test item before therapy, there was with computerized cognitive rehabilitation an improvement in cognitive assessment after therapy not only in stroke patients, but also in traumatic brain injury and multiple sclerosis [11]. However, patients with CVA, right hemiplegia seem to have a higher degree of improvement. Furthermore, its results are similar to those of Chen et al. who suggested that computerized cognitive rehabilitation is effective for recovery of cognitive function of patients presenting cognitive impairment after brain damage when conducted together with rehabilitation therapy [12].
In conclusion application of RehaCom improved the cognitive functions of patients with neurologic disorders, including highest score in psychometric assessment or improved ability to perform complex commands, finishing at discharge at a higher difficulty level than the first session for each RehaCom activity. Moreover, while monitoring of performance within the program (change of level and other individual parameters) the progress of cognitive rehabilitation was reflected. The automatic adjustment of the level of difficulty of the activities and the possibility of setting individual parameters personalizes the healing process in the context of a rehabilitation center with a maximal therapeutic benefit for the patient and the therapist. RehaCom has a statistically significant positive impact on the neuropsychiatric rehabilitation of patients with central nervous system disorders.
2021 Copyright OAT. All rights reserv
The author reports no conflict of interest.
None to disclose.
The views expressed in the article are our own and they do not belong to any founder or institution.
- Lincoln NB, Kneebone II, Macniven JAB, Morris RC (2012) Psychological management of stroke. West Sussex: John Wiley & Sons. UK.
- Bowen A, Hazelton C, Pollock A, Lincoln NB (2013) Cognitive rehabilitation for spatial neglect following stroke. Cochrane Database Syst Rev. [Crossref]
- Noreña D, Sánchez-Cubillo I, García-Molina A, Tirapu-Ustárroz J, Bombín-González I, et al. (2010) Efectividad de la rehabilitación neuropsicológica en el daño cerebral adquirido (II): funciones ejecutivas, modificación de conducta y psicoterapia, y uso de nuevas tecnologías. Rev Neurol 51: 733–44.
- Fernández E, Bringas ML, Salazar S, Rodríguez D, García ME, et al. (2012) Clinical impact of RehaCom software for cognitive rehabilitation of patients with acquired brain injury. MEDICC Rev 14: 32-5. [Crossref]
- Lyrakos G., Ypofandi M., Tzanne P (2014) Psychometric and clinometric properties of the Montreal Cognitive Assessment (MoCA) in a Greek sample. European Psychiatry, 29
- http://www.psychargos.gov.gr/Documents2/ODIGOS%20ERGALEIWN/DIADIKASIES/5.Protocol_Dementia.pdf
- Liu XY, Li L, Xiao JQ, He CZ, Lyu XL, et al. (2016) Cognitive Training in Older Adults with Mild Cognitive Impairment. Biomed Environ Sci 29: 356-64.
- Li K, Alonso J, Chadha N, Pulido J (2015) Does generalization occur following computer-based cognitive retraining? – An exploratory study. Occup Ther Health Care 29: 283-96. [Crossref]
- Yeh IC, Chang CM, Chen KC, Hong WC, Lu YH (2015) The influence of functional fitness and cognitive training of physical disabilities of institutions. ScientificWorldJournal 2015: 686498. [Crossref]
- http://issuu.com/ostracon/docs/rehacom_engish_2012/3?e=0
- Yoo C, Yong MH, Chung J, Yang Y (2015) Effect of computerized cognitive rehabilitation program on cognitive function and activities of living in stroke patients. J Phys Ther Sci 27: 2487-9. [Crossref]
- Chen SH, Thomas JD, Glueckauf RL, Bracy OL (1997) The effectiveness of computer-assisted cognitive rehabilitation for persons with traumatic brain injury. Brain Inj 11: 197-209. [Crossref]
