Rhabdomyomatous mesenchymal hamartoma (RMH) is a benign, rare entity that most often presents as a solitary lesion on the head or neck of a child. While the majority of affected individuals are otherwise healthy, a significant percentage of patients have coexistent developmental anomalies. We report a case of a 2-week-old male neonate with a polypoid mass on the chest that was present at birth. The mass was excised and histopathologic evaluation revealed a diagnosis of RMH. Surgical excision was both diagnostic and curative. Although our patient was otherwise healthy, due to the high rate of coincident anomalies, clinicians should perform thorough physical exams and maintain a low threshold for referral to appropriate specialists for evaluation.
rhabdomyomatous mesenchymal hamartoma, neonate, polypoid, anomaly
Rhabdomyomatous mesenchymal hamartoma (RMH) is a benign, rare entity with approximately 70 cases reported since the 1980’s [1]. This was first described in 1986 as a striated muscle hamartoma [1]. It has also been reported as congenital midline hamartoma and hamartoma of cutaneous adnexa and mesenchyme [1]. RMH most often presents as a solitary lesion on the head or neck of an infant [2]. The lesion is confined to the dermis and subcutis, and consists of mature skeletal muscle, adipose tissue, adnexae, and nerve bundles [3-5]. The clinical presentation is variable and consequently the differential diagnosis is vast, including acrochordon, accessory tragus, hemangioma, rhabdomyoma, neurofibroma, and nasal glioma [1,6-13]. Histopathologic evaluation is requisite for diagnosis. The etiology of RMH is unclear, but some postulate that it is the result of abnormal cell migration of mesodermic tissues during embryogenesis [1,4-6] or a genetic proclivity toward formation of harmatomas [2,11]. Accordingly, it follows that associated developmental anomalies may exist. Although the majority of patients diagnosed with RMH are otherwise healthy infants, many sources report congenital abnormalities. Rosenberg et al. reported as many as 40% of reported cases of RMH occur in children with coexisting developmental anomalies [11]. Described coincident findings include ocular irregularities, spinal dysraphism, thyroductal duct sinus, Delleman syndrome, amniotic band syndrome, and other limb defects [1,3-5,7-11]. Here we report a case of RMH presenting as a polypoid mass in a 2-week-old healthy infant.
A 2 week-old full-term male neonate was referred to pediatric surgery for evaluation of a polypoid mass on the right chest. The lesion had been present at birth and had been seemingly asymptomatic and unchanging. There was no overlying skin breakdown. The child’s newborn exam and screen were normal and he had been doing well since birth. The lesion on the chest was initially evaluated by ultrasound which failed to reveal any communicating sinus. There were no indications for further testing given that the child was healthy overall. The lesion was subsequently excised under local anesthesia. Histologic evaluation revealed a disordered proliferation of variably sized sebaceous glands, vascular structures, both smooth and skeletal muscle, and adnexal epithelium predominantly composed of apocrine epithelium with only occasional eccrine structures. No evidence of atypia, immature elements, or malignancy was identified (Figures 1-3). The diagnosis of rhabdomyomatous mesenchymal hamartoma was made.
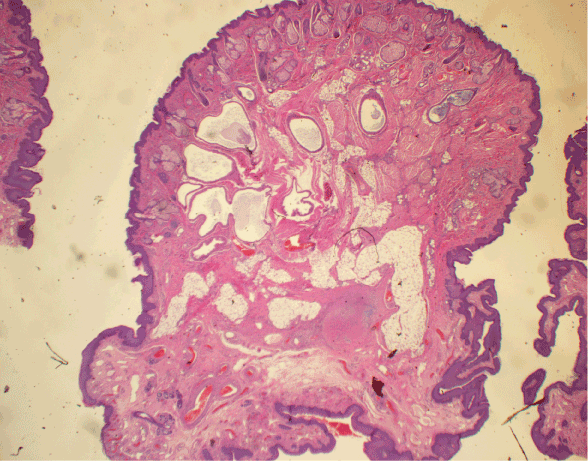
Figure 1. H&E 2x view of a polypoid mass with conspicuous adipose, adnexae, and vascular spaces
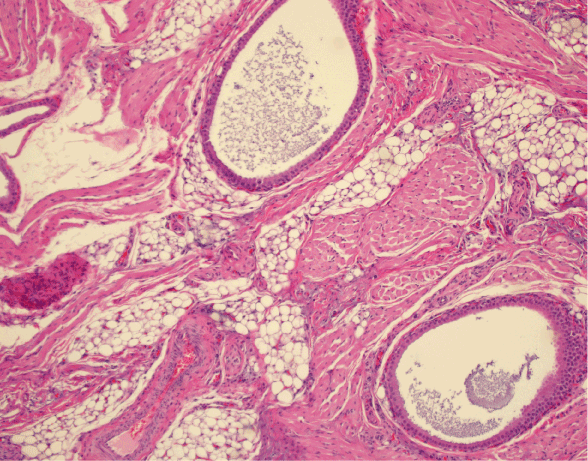
Figure 2. H&E 20x view with apocrine ducts, smooth and skeletal muscle, adipose, and blood vessel
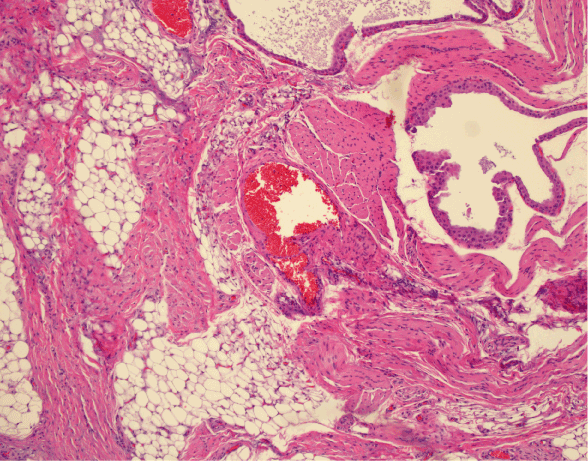
Figure 3. H&E 20x view with apocrine ducts, smooth and skeletal muscle, adipose, and vascular spaces
Rhabdomyomatous mesenchymal hamartoma is a rare lesion, most often presenting in infants and young children [9]. Although the majority of cases occur in otherwise healthy individuals, such as our patient, many cases have additional developmental anomalies [1-4,7-11]. Although RMH most often presents on the head and neck region, our report highlights that RMH can occur anywhere on the skin. Our case is also consistent with the previous observation that males are slightly more affected than females [3]. Histologic evaluation is required for diagnosis due to the myriad clinical presentations; the admixture of mature skeletal muscle, adipocytes, adnexae, and neural tissue distinguish it from other common infantile lesions such as acrochordons, hemangiomas, accessory tragi, and nasal gliomas which would not exhibit each of these microscopic features. Treatment need not be aggressively pursued unless the lesion is symptomatic, causing medical issues due to mass effect, or cosmetically disfiguring. For a small solitary lesion, surgical excision is an appropriate option for both diagnosis and definitive treatment, as with our patient. Interestingly, there have been several reports of spontaneous involution of RMH, though the mechanism for this is poorly understood. Mazza et al. recommend that clinical observation with the possibility of spontaneous regression is reasonable for 1 to 2 years, provided there are no resultant functional deficits or medical problems noted [3]. Neither metastasis nor recurrence have been reported in the literature to date [6,11]. RMH is a benign lesion; however, clinicians ought to be cognizant of the high rate of concurrent anomalies, perform thorough physical exams, and refer to ophthalmology and otolaryngology for screening in appropriate cases.
- McKinnon EL, Rand AJ, Selim, MA, Fuchs HE, Cummings TJ (2015) Rhabdomyomatous mesenchymal hamartoma presenting as a sacral skin tag in two neonates with spinal dysraphism. J Cutan Pathol 42: 774–778. [Crossref]
- Wang Y, Zhao H, Yue X, Tang X, Ma L, et al. (2014) Rhabdomyomatous mesenchymal hamartoma presenting as a big subcutaneous mass on the neck: a case report. J Med Case Rep 8: 410. [Crossref]
- Mazza JM, Linnell E, Votava HJ, Wisoff JH, Silverberg NB (2015) Biopsy-Proven Spontaneous Regression of a Rhabdomyomatous Mesenchymal Hamartoma. Pediatr Dermatol 32: 256–262. [Crossref]
- Takeyama J, Toshiaki H, Sanada T, Shimanuki Y, Saito M, et al. (2005) Rhabdomyomatous mesenchymal hamartoma associated with nasofrontal meningocele and dermoid cyst. J Cutan Pathol 32: 310-313. [Crossref]
- White LR Jr, Agrawal V, Sutton L, Balbosa AC (2015) Rhabdomyomatous mesenchymal hamartoma of the face causing trigeminal neuralgia. Am J Case Rep 16: 338-340. [Crossref]
- Hao J, Diao QC, Wang SP, Liang CP, Shi BJ (2015) Rhabdomyomatous mesenchymal hamartoma: case report and literature review. Int J Dermatol 54: 1183-1185. [Crossref]
- Argenta AE, Chen W, Davis A, Losee JE, Davit A, et al. (2015) A review of eight unusual pediatric skin and soft-tissue lesions: Diagnosis, workup, and treatment. J Plast Reconstr Aesthet Surg 68: 1637–1646. [Crossref]
- Orozco-Covarrubias L, Carrasco-Daza D, Diaz-Noriega A, Lara-Mendoza L, Ruiz-Maldonado R (2016) Rhabdomyomatous Mesenchymal Hamartoma: A Deep Subcutaneous Lesion in the Sternoclavicular Area. Pediatr Dermatol 33:e36– e37. [Crossref]
- Fontecilla NM, Weitz NA, Day C, Golas AR, Grossman ME, et al. (2016) Rhabdomyomatous mesenchymal hamartoma presenting as a skin tag in a newborn. JAAD Case Rep 2: 222-223. [Crossref]
- Solis-Coria A, Vargas-Gonzalez R, Sotelo-Avila C (2007) Rhabdomyomatous Mesenchymal Hamartoma Presenting as a Skin Tag in the Sternoclavicular Area. Pathol Oncol Res 13: 375-378. [Crossref]
- Rosenberg AS, Kirk J, Morgan MB (2002) Rhabdomyomatous mesenchymal hamartoma: an unusual dermal entity with a report of two cases and a review of the literature. J Cutan Pathol 29: 238-243. [Crossref]
- Scrivener Y, Petiau P, Rodier-Bruant C, Cribier B, Heid E, et al. (1998) Perianal striated muscle hamartoma associated with hemangioma. Pediatr Dermatol 15: 274-276. [Crossref]
- Whitaker SR, Sprinkle PM, Chou SM (1981) Nasal glioma. Arch Otolaryngol 107: 550-554. [Crossref]
2021 Copyright OAT. All rights reserv



