Phyllodes are uncommon fibroepithelial breast tumours. Here, we present the case of a 42-year-old woman who presented to our breast centre with a palpable breast mass, which was initially suspected and treated as fibroadenoma but was finally revealed to be a phyllodes tumour. Histopathological examination identified ductal carcinoma in situ (DCIS) within the entire volume of the fibroepithelial tumour. The literature on these transformations is still limited, and the treatment is not standardised.
breast, phyllodes tumour, ductal carcinoma, fibroepithelial neoplasm, DCIS, case report
Phyllodes tumours are uncommon fibroepithelial breast tumours that are capable of a wide range of biological behaviours, from benign to malignant [1]. They can appear at any age, with a median age of presentation of 42 to 45 years, and are often misdiagnosed as fibroadenomas [2,3]. Phyllodes tumours account for less than 1% of all breast tumours, and they rarely undergo a malignant epithelial transformation. Due to their rarity, data are limited, and diagnosis and treatment are not yet standardised [4].
We report the case of a patient who was diagnosed with noninvasive ductal carcinoma growing within the entire volume of a borderline phyllodes tumour of the breast.
A 42-year-old multiparous woman attended a consultation at the breast centre of our hospital for a growing palpable left breast mass, previously confirmed as fibroadenoma with a core needle biopsy. The patient had a positive family history of breast cancer (two maternal aunts). During clinical examination, the B-sized breast was palpated, and a mass measuring 5 cm was identified in the left upper outer quadrant. The mass was mobile and had a firm consistency and well-defined margins, with no skin alterations and normal axilla examination. The contralateral breast was normal. On ultrasound imaging, we observed a well-circumscribed hypoechoic mass measuring 45 × 22 × 41 mm (Figure 1).
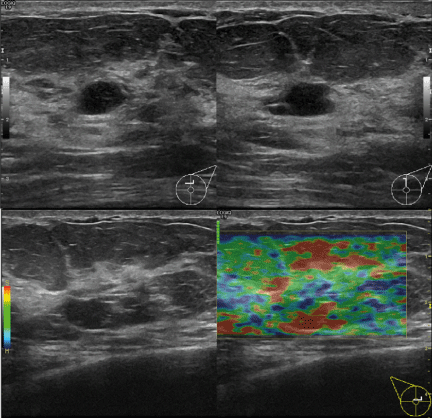
Figure 1. Ultrasound results
On the complementary mammography, nodular opacity is confirmed in correspondence with the non- magnetic clip positioned at the previous biopsy (Figure 2).
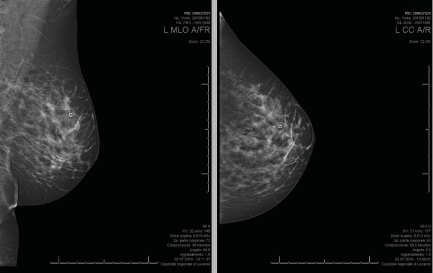
Figure 2. Mammography results
The patient underwent an excisional biopsy, which revealed a 5-cm borderline phyllodes tumour with associated ductal carcinoma in situ (DCIS) widespread throughout the preparation (Figure 3). The epithelial cells presented nuclear atypia up to important and frequent mitotic figures (up to 6 for 10 HPF) leading to a histological grading G3 for the entire 5-cm diameter of the DCIS. The surgical excision margins were positive for DCIS at several points (Figure 4). The epithelial cells were strongly positive for oestrogen and progesterone receptors (both 95%) and had a Ki-67 index of 15–20% and a c-erbB2 score of 2+.
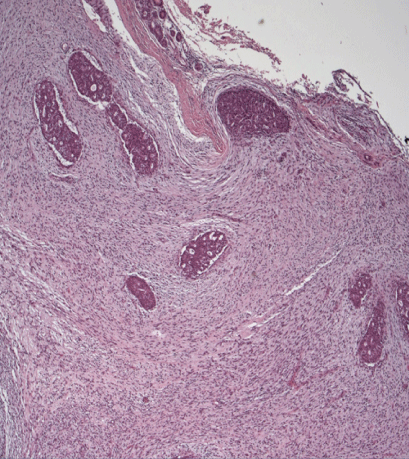
Figure 3. Histopathology analysis (H&E stain, 50×) showing a circumscribed mass with biphasic morphology. An epithelial component and an expanded stromal compartment can be observed
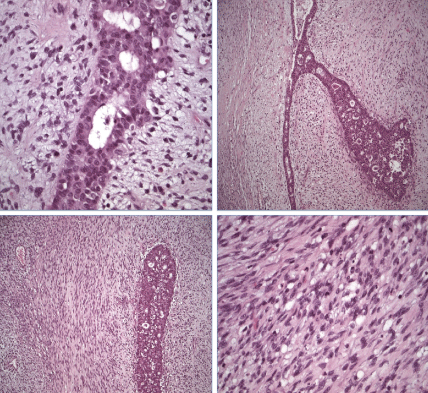
Figure 4. Histopathology analysis (H&E stain, 100–400×) showing the epithelial component of the tumour. A high-grade comedoductal carcinoma in situ with necrotic debris in the central duct space can be observed
Considering the size and histological grade of the tumour, the eventual need for reoperation to achieve clear margins and an aesthetic result, and the patient’s stress related to her family history, we opted for a bilateral mastectomy with pose of tissue expanders. The final histopathological findings were negative for malignancy. No metastasis was detected in the dissected sentinel lymph nodes. Neither chemoendocrine therapy nor irradiation were performed postoperatively.
Phyllodes are uncommon tumours, comprising less than 1% of primary breast neoplasms. They are composed of an epithelial and a stromal component. Based on their stromal characteristics, phyllodes are classified as benign, borderline or malignant to prognosticate their clinical course [5]. Most phyllodes tumours are classified as benign (50–70%). Locally recurrence is common, even in benign tumours, and those with positive or close margins are significantly associated with recurrence [6]. The malignant transformation of the epithelial component of phyllodes tumours is very rare (less than 1% of all phyllodes tumours) [7]. Over the past 20 years, only 17 cases of carcinoma arising in a phyllodes tumour have been described [8]. Since the stromal component takes up most of the tissue, it is very difficult to detect the presence of carcinoma within the tissue [9]. In most cases, phyllodes tumours occupy a larger area than the carcinoma. However, in the case of our patient, the epithelial component was evenly distributed over the entire stromal component, with no evidence of transition.
The presence of a carcinoma within a phyllodes tumour is clinically relevant as it may change the clinical management. Moreover, preoperative diagnosis of stromal degeneration is very difficult, and it is usually an incidental finding [10]. It is important to conduct an exhaustive histopathologic examination when evaluating a phyllodes tumour, keeping in mind the possibility of a coexisting carcinoma.
Surgical excision is the first treatment offered to patients with a phyllodes tumour. As malignant phyllodes tumours are usually spread through the hematogenous route, axillary lymph node dissection is generally not recommended [11]. Furthermore, no standard adjuvant therapy is currently recommended [12]. The survival of patients with a phyllodes tumour is excellent, even those with a coexisting carcinoma [13,14].
The patient signed an approval for the publication of thecase.
The authors declare that the research was conducted in the absence of commercial orfinancial relationships that could be construed as a potential conflict of interest.
FM and IFV conceived of the presented idea and wrote the manuscript with support from APand ESL. AF, SA and MNDA supervised the findings of this work. All authors discussedand Contributed to the finalmanuscript.
The authors thank Dr. Ulrike Perriard at the Cantonal Institute of Pathology of Locarno forproviding the histologicalimages.
- Telli ML, Horst KC, Guardino AE, Dirbas FM, Carlson RW (2007) Phyllodes tumors of the breast: natural history, diagnosis, and treatment. J Natl Compr Canc Netw 5: 324-330. [Crossref]
- Zhang L, Yang C, Pfeifer JD, Caprioli RM, Judd AM, et al. (2020) Histopathologic, immunophenotypic, and proteomics characteristics of low-grade phyllodes tumor and fibroadenoma: more similarities than differences. NPJ Breast Cancer 6: 27. [Crossref]
- Lee AH, Hodi Z, Ellis IO, Elston CW (2007) Histological features useful in the distinction of phyllodes 109 tumour and fibroadenoma on needle core biopsy of the breast. Histopathology 51: 336-344.
- Saimura M, Koga K, Anan K, Mitsuyama S, Tamiya S (2018) Diagnosis, characteristics, and treatment of breast carcinomas within benign fibroepithelial tumors. Breast Cancer 25: 470-478. [Crossref]
- Tan BY, Tan PH (2018) A diagnostic approach to fibroepithelial breast lesions. Surg Pathol Clin 11: 17-42. [Crossref]
- Tan BY, Acs G, Apple SK, Badve S, Bleiweiss IJ, et al. (2016) Phyllodes tumours of the breast: a consensus review. Histopathology 68: 5-21. [Crossref]
- Parker SJ, Harries SA (2001) Phyllodes tumours. Postgrad Med J 77: 428-435. [Crossref]
- İlhan B, Emiroğlu S, Türkay R (2021) Report of two cases with simultaneously detected tubular carcinoma and phyllodes tumor of the breast. Eur J Breast Health 17: 80-84. [Crossref]
- Giri D (2009) Recurrent challenges in the evaluation of fibroepithelial lesions. Arch Pathol Lab Med 133: 713-721.
- Padmanabhan V, Dahlstrom JE, Chong GC, Bennett G (1997) Phyllodes tumor with lobular carcinoma in situ and liposarcomatous stroma. Pathology 29: 224-226. [Crossref]
- Chaney AW, Pollack A, McNeese MD, Zagars GK, Pisters PW, et al. (2000) Primary treatment of cystosarcoma phyllodes of the breast. Cancer 89: 1502-1511. [Crossref]
- Pandey M, Mathew A, Kattoor J, Abraham EK, Mathew BS, et al. (2001) Malignant phyllodes tumor. Breast J 7: 411-416.
- Co M, Tse GM, Chen C, Wei J, Kwong A (2018) Coexistence of ductal carcinoma within mammary phyllodes tumor: a review of 557 cases from a 20-year region-wide database in Hong Kong and Southern China. Clin Breast Cancer 18: e421-425. [Crossref]
- Ditsatham C, Chongruksut W (2019) Phyllodes tumor of the breast: diagnosis, management and outcome during a 10-year experience. Cancer Manag Res 11: 7805-7811. [Crossref]




