Context: Subacute combined degeneration (SCD) is a rare cause of myelopathy and is classically due to vitamin B12 deficiency. The typical pathological changes associated with SCD include axonal loss selectively involving the dorsal columns as well as the anterolateral pyramidal pathways.
Findings: We report a 22-year old Chinese woman who initially presented with progressive numbness and recurrent falls. Patient was subsequently diagnosed with subacute combined degeneration involving the thoracic and cervical cord based on imaging findings and low vitamin B12 levels. With careful and empathetic interviewing the patient admitted to intermittent self-induced vomiting after periods of compulsive eating consistent with a diagnosis of Bulimia Nervosa.
Conclusion: To our knowledge, this is the first case report of subacute combined degeneration due to B12 deficiency secondary to bulimia nervosa.
subacute combined degeneration, B12 deficiency, bulimia nervosa
Here we present a 22-year-old female of Chinese origin who initially began experiencing numbness and tingling in her hands and feet. This later progressed to weakness primarily in her lower extremities to the point where she began falling repeatedly. Patient was quite reserved and not forthcoming with here history however with gentle questioning regarding her eating habits she finally admitted to periods of binge eating followed by self-induced vomiting or purging. She admitted to doing this on a “on and off” basis over the 6 months prior to the onset of her symptoms.
Her exam revealed a well-developed female who initially was quite reserved and withdrawn. Cranial nerve exam was normal and strength in the upper extremities was 4/5 while strength in bilateral lower extremities was 3/5. There were horizontal linear abrasions immediately below her knees which she attributed to repeated falls. She had impaired sensation to light touch in bilateral upper and lower extremities and proprioception and vibration sensation were also both impaired. She was unable to stand up from a laying position without significant assistance and was unable to ambulate even for a few steps (Table 1).
Table 1: Patient Demographics and baseline characteristic.
Age |
22 |
Sex |
F |
Ethnicity |
Chinese |
Duration of Bulimia |
6 months |
Symptoms |
Numbness and weakness – 4 extremities
Recurrent falls |
Neurologic Exam |
Cranial nerve exam: normal; quadriparesis; Decreased proprioception, vibration and light touch in bilateral upper and lower extremities; Unable to ambulate; Linear abrasions below knees bilaterally due to repeated falls |
Initial investigations included an electrocardiogram which showed normal sinus rhythm, computerized tomography scan of the head which was normal. Her laboratory workup was remarkable for a markedly low serum B12 level together with markedly elevated methylmalonic acid and homocysteine levels. To investigate the potential etiology of the low B12 levels, we obtained testing for anti-parietal cell, anti-intrinsic factor antibodies and Immunochemical fecal occult blood all of which were negative. A Gastroenterology consult was obtained, and a computerized tomography of the abdomen was performed together with testing for fecal calprotectin (an intestinal inflammatory biomarker used to screen for inflammatory bowel disease) [1] both of which were normal. A full psychiatric assessment was then obtained, and patient was screened for possible drug abuse including the possibility of exposure to nitrous oxide (known to impair B12 metabolism) [2]. Patient met all diagnostic and statistical manual (DSM) criteria for Bulimia Nervosa – Purging Type. Lab and imaging workup is shown in Table 2.
Table 2: Lab and imaging workup.
Lab Name |
Value |
Normal Range |
WBC |
5.3 |
4.0 - 11.0 10*3/µL |
RED BLOOD CELL |
3.53 (L) |
3.63 - 5.04 10*6/µL |
HEMOGLOBIN |
11.4 (L) |
12.0 - 15.3 g/dL |
HEMATOCRIT |
34.5 (L) |
34.7 - 45.1 % |
MCV |
97.9 |
80.0 - 100.0 fL |
PLATELET |
200 |
150 - 450 10*3/µL |
GLUCOSE |
97 |
70 - 99 mg/dL |
SODIUM |
140 |
133 - 144 mmol/L |
POTASSIUM |
3.7 |
3.5 - 5.1 mmol/L |
CHLORIDE |
109 (H) |
98 - 107 mmol/L |
BUN |
20 |
7 - 25 mg/dL |
CREATININE |
0.6 |
0.6 - 1.2 mg/dL |
CALCIUM |
9.4 |
8.6 - 10.3 mg/dL |
AST (SGOT) |
17 |
13 - 39 U/L |
ALT (SGPT) |
14 |
7 - 52 U/L |
ALKALINE PHOSPHATASE (ALP) |
53 |
34 - 104 U/L |
TSH |
3.573 |
0.270 - 4.200 u[IU]/mL |
CRP |
1.3 (H) |
0.0 - 0.5 mg/dL |
CERULOPLASMIN |
222.0 |
180.0 - 580.0 mg/L |
Syphilis Treponemal AB |
Nonreactive |
Nonreactive |
HIV-1/HIV-2 Ag/Ab |
Nonreactive |
Nonreactive |
IGG SYNTHESIS RATE CSF |
<0.0 |
<=8.0 mg/d |
IGG/ALB RATIO CSF |
0.17 |
0.09 - 0.25 {ratio} |
IgG Index |
0.61 |
0.28 - 0.66 {ratio} |
ALBUMIN INDEX |
3.8 |
0.0 - 9.0 {ratio} |
OLIGOCL.BAN.CSF |
Negative |
Negative |
Urine Drug Screen |
Negative |
Negative |
VITAMIN B1 |
4 |
4 - 15 |
VITAMIN E (ALPHA TOCO) |
7.7 |
5.5 - 18.0 mg/L |
VITAMIN E (B-GAMMA TOCO) |
0.9 |
0.0 - 6.0 mg/L |
VITAMIN B12 |
88 (L) |
180 - 914 pg/mL |
VITAMIN B12
(3 weeks post- treatment |
790 |
180 - 914 pg/mL |
FOLIC ACID |
23.6 |
5.9 - 24.8 ng/mL |
HOMOCYSTEINE |
60.3 (H) |
3.7 - 13.9 umol/L |
METHYLMALONIC ACID |
4.49 (H) |
0.00 - 0.40 umol/L |
PARIETAL CELL AB |
<1:20 |
<1:20 |
INTRINSIC FACTOR AB |
Negative |
Negative |
Immunochemical fecal occult blood |
Negative |
Negative |
CT Abdomen with contrast |
Unremarkabme |
Unremarkabme |
MRI Brain |
Unremarkabme |
Unremarkabme |
MRI C and T spine |
hyperintensity within the bilateral
posterior columns |
|
A magnetic resonance imaging of the brain was unremarkable however magnetic resonance imaging of the cervical and thoracic spine revealed an abnormal signal hyperintensity within the bilateral posterior columns of the thoracic cord, most apparent below T7 and a similar extensive signal hyperintensity within the posterior columns of the spinal cord extending from the craniocervical junction through C6-C7 (Figure 1A and 1B). With cyanocobalamin replacement and concurrent rehabilitation, the patient improved markedly where she was then able to ambulate with minimal assistance within the first 2 weeks after treatment.
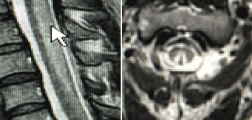
Figure 1: Imaging findings of subacute combined degeneration. Magnetic resonance imaging showing degeneration of the dorsal columns of the cervical spine as revealed through a hyperintense signal change on sagittal T2-weighted imaging (A, arrow) and axial T2-weighted imaging (B).
To our knowledge, this is the first case report describing subacute combined degeneration of the spinal cord due to B12 deficiency in a patient with bulimia nervosa. A previous report described a case of SCD of the spinal cord in an adolescent male afflicted with avoidant/restrictive food intake disorder who was found to be deficient in vitamins A, E, K, D, B12, and folate [3]. In this condition, sufferers avoid only specific types of food or food groups. The Diagnostic and Statistical Manual of Mental Disorders distinguishes this condition from Bulimia Nervosa where patients typically suffer from periods of binging followed by self-induced vomiting or purging. Interestingly, a medline search with the terms “bulimia” AND “’B12” revealed 4 articles, one of which directly addressed the prevalence of B12 deficiency in bulimic patients [4-7]. The study found a prevalence of 5.1% of vitamin B12 levels below the “normal range”. They concluded that this prevalence was no different than psychiatric controls [4]. In our case however, our investigations revealed no other plausible cause for the severe B12 deficiency leading to SCD of the spinal cord. Our patient presented with significant weakness in all extremities as can be expected from a patient presenting with subacute combined degeneration. Imaging revealed a definitive abnormality within the dorsal columns of the spinal cord known to subserve fine touch, proprioception and vibration sensations. While it is not easy to distinguish specific ascending or descending spinal cord tracts on magnetic resonance imaging, it is likely that at least the lateral corticospinal tract, which is immediately lateral to the dorsal column, was involved as well in our patient. In addition, it is also likely that the patient had a concomitant neuropathy related to her B12 deficiency which would also account for her weakness. Patient was scheduled for an electromyography and nerve conduction study exam but was marked as a “no show” for her appointment as she had returned to spend her summer vacation with her family in China. Prior to her departure, she did however undergo rather extensive inpatient rehabilitation but had already improved dramatically even within the first 2 weeks after cyanocobalamin replacement therapy.
Subacute combined degeneration has also been described in association with multiple conditions such as total gastrectomy for early gastric cancer [8], infective endocarditis [9], occult celiac disease with copper deficiency [10], helicobacter pylori-induced gastritis with anti-intrinsic factor antibodies [11] and in the setting of nitrous oxide abuse (N2O, laughing gas) which is thought to impair vitamin B12 metabolism [2]. In our case, the patient was very reluctant to admit self-induced vomiting following periods of binging or compulsive eating. Only after careful and empathetic interviewing was the patient forthcoming regarding her eating patterns.
This case highlights the need for careful screening for conditions such as bulimia nervosa when SCD secondary to B12 deficiency is encountered.
Patient provided consent for the publication of this manuscript, acknowledge that they cannot be identified via the paper and all efforts were made to de-identify the patient.
- Fagerhol MK (2000) Calprotectin, a faecal marker of organic gastrointestinal abnormality. Lancet 356: 1783-1784. [Crossref]
- Gowdappa HB, Mahesh M, Murthy KV, Narahari MG (2013) Helicobacter pylori associated vitamin B12 deficiency, pernicious anaemia and subacute combined degeneration of the spinal cord. BMJ Case Rep 2013. [Crossref]
- Chandran JJ, Anderson G, Kennedy A, Kohn M, Clarke S (2015) Subacute combined degeneration of the spinal cord in an adolescent male with avoidant/restrictive food intake disorder: A clinical case report. Int J Eat Disord 48: 1176-1179. [Crossref]
- Gendall KA, Bulik CM, Joyce PR (1999) Visceral protein and hematological status of women with bulimia nervosa and depressed controls. Physiol Behav 66: 159-163. [Crossref]
- Tasegian A, Curcio F, Dalla Ragione L, Rossetti F, Cataldi S, et al. (2016) Hypovitaminosis D3, Leukopenia, and Human Serotonin Transporter Polymorphism in Anorexia Nervosa and Bulimia Nervosa. Mediators Inflamm 2016: 8046479. [Crossref]
- Connelly JJ, Golding J, Gregory SP, Ring SM, Davis JM, et al. (2014) Personality, behavior and environmental features associated with OXTR genetic variants in British mothers. PLoS One 9: e90465. [Crossref]
- Schlosser BJ, Pirigyi M, Mirowski GW (2011) Oral manifestations of hematologic and nutritional diseases. Otolaryngol Clin North Am 44: 183-203, vii. [Crossref]
- Hwang CH, Park DJ, Kim GY (2016) Ataxic gait following total gastrectomy for gastric cancer. World J Gastroenterol 22: 8435-8438. [Crossref]
- Huang XJ, He J, Qu WS, Tian DS (2015) A Case of Subacute Combined Degeneration of the Spinal Cord with Infective Endocarditis. Case Rep Neurol Med 2015: 327046. [Crossref]
- Cavallieri F, Fini N, Contardi S, Fiorini M, Corradini E, et al. (2017) Subacute copper-deficiency myelopathy in a patient with occult celiac disease. J Spinal Cord Med 40: 489-491. [Crossref]
- Buizert A, Sharma R, Koppen H (2017) When the Laughing Stops: Subacute Combined Spinal Cord Degeneration Caused by Laughing Gas Use. J Addict Med 11: 235-236. [Crossref]
2021 Copyright OAT. All rights reserv

