Surgical site infections are important cause of morbidity, mortality and prolonged hospital stay after surgical procedures. It complicates around 2% of surgeries done in the United States each year. Several preventive measures were suggested by World Health Organization (WHO) to decrease the rate of surgical site infections. Of the most important is preoperative antibiotics and optimal skin preparation with chlorhexidine and alcohol prior to the incision. During the COVID-19 pandemic more strict infection control measures were taken to decrease the risk of transmission. Applying Contact and droplet isolation and strict hand hygiene were implemented. The above measures as well as limiting visitors in the surgical wards all resulted in decrease in the rate of surgical site infection in a report by losurdo et al. A similar observation was found in King Faisal Specialist Hospital & Research Centre, Riyadh. The rate of SSI in liver transplant surgeries was reduced by 5-8% as compared to 2018 and 2019 respectively. The rate however was more in renal transplant surgeries that might be related to decrease in the overall number of surgeries.
Surgical, Infections, COVID-19, Transplant, Liver, Kidney
COVID-19: Coronavirus disease 2019; KFSH&RC: King Faisal Specialist Hospital and Research Center; SSI: Surgical Site Infections; WHO: World Health Organization
Surgical site infection (SSI) is defined as an infection that occurs within 30 days after the operation involving the skin and subcutaneous tissue (Superficial SSI), deeper soft tissue e.g., fascia and muscle (Deep incisional SSI) or involve organ and body spaces (organ/space SSI) [1]. SSI contributes to major morbidity, mortality, and length of stay post operatively [2]. It is estimated to complicate 2% of the 80 million surgeries done in the United States each year and is the commonest health care associated infection in patients undergoing surgery [3]. SSI is an important complication in the early post-transplant period with the highest rates seen in small bowel and multivesicular transplants followed by liver and pancreas transplant surgeries [4]. Several preventive measures have been studied to decrease the rate of SSI. Pre-operative antimicrobial prophylaxis is among the most effective ones. Preparing the skin with chlorohexidine and alcohol has also shown benefit [5]. During the COVID-19 (Coronavirus disease-2019) pandemic the World Health Organization (WHO) recommended measures to limit the transmission in healthcare facilities including applying contact and droplet precautions and further emphasis was put on adequate hand hygiene [6]. A report by losurdo et al has shown significant reduction in the incidence of both superficial and deep surgical site infection during the COVID-19 year as compared to the previous COVID-19 free years [7]. We aim at this study to see the difference in SSI rate before and after the COVID-10 pandemic.
Single center observational cohort study. We retrospectively analyzed patients who underwent liver and kidney transplant surgeries in King Faisal Specialist Hospital & Research Centre (KFSH&RC), Riyadh during the period January 2018- October 2020. SSI infection rate was obtained from the department of Infection control and hospital epidemiology.
The rate of SSI was calculated by dividing the number of total SSI over the total number of liver or kidney transplant surgery per year and it was divided into quarters. A comparison was made between the rates before and after the COVID-19 pandemic and the infection control measures that was implemented by the hospital.
The total number of liver transplant surgeries done in 2018 was 156 surgeries, rate of surgical site infection was 19/156 (12.2%) during 2018. Klebsiella pneumoniae and Candida spp. were the most frequently isolated organisms. In 2019 a total of 186 liver transplant surgeries were performed, SSI occurred in 28 (15%) of the cases. Commonest isolated organisms were Candida spp., Enterococcus faecium and coagulase negative Staphylococcus. A total of 114 liver transplant surgeries were done in 2020, SSI was reported in 8 (7%), again Candida spp. was the commonest isolated organism, Stenotrophomonas maltophilia was isolated in two of the cases.
On the other hand, there were 211 kidney transplant surgeries were conducted in 2018 with a surgical site infection rate of 3/211 (1.4%). Klebsiella pneumoniae, Candida krusei, Pseudomonas aeruginosa and Enterobacter cloacae were isolated from these patients. In 2019 a total of 196 renal transplant surgeries were performed, SSI was reported in 6 (3%) of the cases. Escherichia coli, Pseudomonas aeruginosa and Enterococcus faecalis were isolated in the reported cases. During 2020 a total of 101 renal transplant surgeries were done, SSI was reported in 6 (5.9%) of the cases. Escherichia coli and Pseudomonas aeruginosa were most frequently isolated. Results summarized in figure 1.
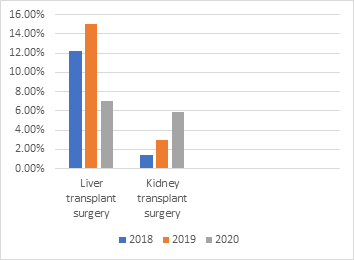
Figure 1: Rate of SSI liver and kidney transplant surgeries 2018-2020.
Liver Transplant Surgery SSI rates:
The rate of SSI was calculated in each quarter of the year.
In 2018, the rate of SSI was as follow 2/38 (5.3%), 6/40 (15%), 6/33 (18.2%) and 5/45 (11.1%) in the 1st, 2nd, 3rd, and 4th quarters respectively. The overall rate of SSI was 19/156 (12.2%). In 2019 the rate of SSI was as follow 3/36 (8.3%), 9/53 (16.98%), 8/51 (15.7%), 8/46 (17.4%) in the 1st, 2nd, 3rd, and 4th quarters respectively. The overall rate of SSI was 28/186 (15%). In 2020 SSI occurred in 1/43 (2.3%), 1/24 (4.2%), 1/27 (3.7%) in the 1st, 2nd, and 3rd quarters respectively, results summarized in figure 2. The overall rate of SSI in 2020 was 8/114 (7%).
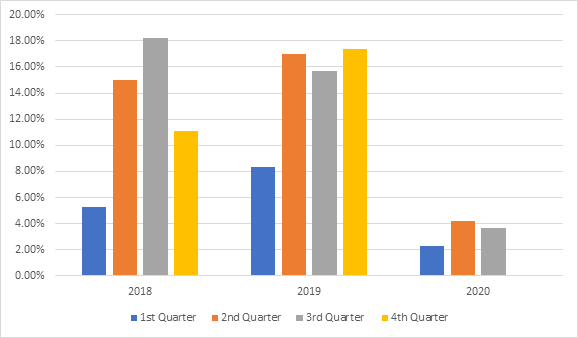
Figure 2: SSI rates in liver transplant surgeries in quarters 2018-2020.
Kidney Transplant Surgeries:
In 2018, the rate of SSI was as follow 1/54 (1.9%), 2/61 (3.3%), 0/53, 0/44 in the 1st, 2nd, 3rd and 4th quarters respectively. The overall rate of SSI was 3/211 (1.4%). In 2019, the rate of SSI was as follow 2/58 (3.5%), 1/20 (5%), 0/52, 3/66 (4.6%) in the 1st, 2nd, 3rd, and 4th quarters respectively. The overall rate of SSI was 6/196 (3%). In 2020, 5/49 (10.2%), 0/8, 1/24 (4.2%) in the 1st, 2nd, 3rd quarters respectively, results summarized in figure 3. The overall rate of SSI in 2020 6/101 (5.9%).
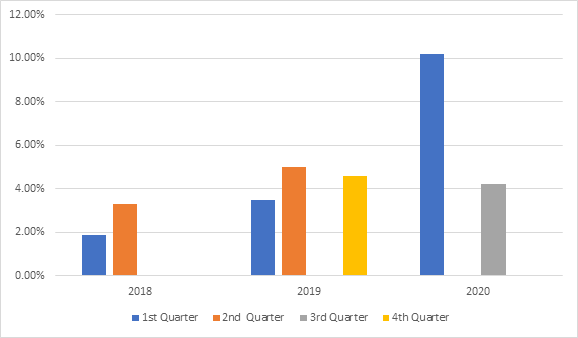
Figure 3: SSI rates in kidney transplant surgeries in quarters 2018-2020.
KFSH&RC has implemented several infection controls measures to decrease the risk of COVID-19 transmission. On March 22nd all patients were only allowed to have one sitter if the patient’s condition necessitate and as directed by the treating physician. No visitors were allowed in all patient care areas. On April 5th the hospital implemented universal masking policy for all staff when inside hospital premises, it also stressed on strict adherence to proper hand hygiene.
Surgical site infection remains a major cause of morbidity and mortality and increased cost following surgical intervention. It estimated that hospital stay will increase by 9.7 days. The estimated costs from SSI are 900 million US$ 8It is thus crucial to find ways to decrease the rate of SSI and burden of financial cost on the healthcare system. Prevention o SSI requires control of pre-operative, intraoperative and post-operative factors. Of the recommended methods is to treat any infection prior to the surgical procedure, hair removal at the site of surgical incision, pre-operative antimicrobial prophylaxis given 60 minutes prior to the surgery. Perioperative glycaemic control and oxygenation has also shown to decrease the rate of SSI [8,9]. The findings of this study further highlight the importance of infection control measures in preventing SSI. We postulate that the universal masking and strict hand hygiene as well as limiting the number of sitters in our institute since the start of COVID-19 has helped decrease the rate of surgical site infection in liver transplant surgeries. Although the overall rate of SSI in 2020 was higher in renal transplant surgeries, there was only one reported case after the implementation of the precautionary measures which further support that adherence to infection control measures has clearly resulted in decrease in the rate of SSI. Also, the increase in the overall rate might partially be related to the lower number of surgeries done during the COVID-19 pandemic. These findings are like what was reported by losurdo et al where the rate of SSI was 7.2% prior to the COVID-19 era compared to 3.3% during the COVID-19 pandemic. The reduction in the rate was contributed to the mandatory wearing of surgical mask and the restriction of visitors in the surgical words [7] like the measures taken in our institute. To our knowledge this is the first observational study that shows the rates of SSI in transplant surgeries during the COVID-19.
There are several limitations to the study including the relatively small number of cases and the short period that was evaluated. It is also a single center observation which limits its generalizability. A larger population study over a longer period needs to be done to further support the current results.
SSI remains an important cause of morbidity, mortality, prolonged length of hospital stays and increase financial burden in patient undergoing surgeries. Strict infection control measures implemented during the COVID-19 pandemic has resulted in lesser rate of SSI. Compliance and continuation on the current measures might result in enhance patient’s outcome and decreased cost on the healthcare system.
The authors of this manuscript have no conflicts of interest to disclose.
- ECDC (2012) European Centre for Disease Prevention and Control. Surveillance of Surgical Site Infections in European Hospitals – HAISSI Protocol. Version 1.02. Stockholm: ECDC; 2012.
- Sartelli M, Kluger Y, Ansaloni L, Coccolini F, Baiocchi GL, et al. (2018) Knowledge, awareness, and attitude towards infection prevention and management among surgeons: Identifying the surgeon champion. World J Emerg Surg 13: 4-9. [Crossref]
- Borchardt RA, Tzizik D (2018) Update on surgical site infections: The new CDC guidelines. J Am Acad Physician Assistants 31: 52-54. [Crossref]
- Abbo LM, Grossi PA (2019) Surgical site infections: Guidelines from the American Society of Transplantation Infectious Diseases Community of Practice. Clin Transplant 33: 1-19. [Crossref]
- Itani KMF (2015) Care bundles and prevention of surgical site infection in colorectal surgery. J Am Med Asso 314: 289-290. [Crossref]
- World Health Organization (2020) Laboratory biosafety guidance related to coronavirus disease (COVID-19). Interim guidance 1-5.
- Losurdo P, Paiano L, Samardzic N, Germani P, Bernardi L, et al. (2020) Impact of lockdown for SARS-CoV-2 (COVID-19) on surgical site infection rates: a monocentric observational cohort study. Updates Surg 72: 1263-1271. [Crossref]
- Leaper DJ, Edmiston CE (2017) World Health Organization: global guidelines for the prevention of surgical site infection. J Hosp Infect 95: 135-136. [Crossref]
- Soule BM (2018) Evidence-Based Principles and Practices for Preventing Surgical Site Infections.



