Abstract
Background: Nurses play a central role in providing end-of-life (EOL) care to patients and their loved ones. Quality palliative care is essential to our healthcare system, yet nurses report inadequate training to provide patients with competent EOL care.
Objectives: This purpose of this study was to assess the perceptions of undergraduate student and professional nurses to gauge if nurses are receiving sufficient education to feel confident when caring for dying patients.
Methods: This study is a mixed blend qualitative study with a phenomenological approach. We surveyed professional nurses to appraise their perceptions and barriers when providing EOL care. Students were interviewed to elicit perspective on how baccalaureate nursing programs are incorporating EOL care. Data were evaluated for descriptive analytics and coded for thematic content.
Findings: The study revealed student nurses have an expectation that EOL patient care will be incorporated in their curriculum. While some nurses noted formal training in their undergraduate studies, most cited experiential training and knowledge from their peers as their primary source for palliative care education. 97% of the professional nurses surveyed expressed interest in EOL education if it were offered by their institutions.
Conclusion: This study supports the need for undergraduate nursing programs to integrate more robust EOL and palliative care training into their curriculum in order to adequately prepare competent and assertive future nurses when providing EOL care.
Keywords
end-of-life nursing care, nursing curriculum, end-of-life nurse education, palliative care education
Undergraduate Nursing Education for End-of-Life Care: A Mixed Phenomenology Study
End-of-life (EOL) patient care is a complex, yet inevitable domain in the healthcare continuum. All players in this triangle of care- the dying patient, their families and caregivers, and the medical teams supporting them- require unique and individualized consideration of their EOL needs. The U.S. population continues to age and become more medically complicated, prompting an upsurge to our palliative and EOL care needs [1]. It is estimated by 2030 that 9 million Americans will be over the age of 85, many living with serious medical conditions [2]. Nurses are key players in providing sensitive, quality EOL care to patients and their families. Yet nurses consistently report feeling inadequately prepared or educated to provide sensitive palliative and EOL care, despite this escalating demand [1,3].
Research Question
Are undergraduate nursing curriculums adequately preparing novice nurses to provide competent end-of-life care?
Problem Statement
The lack of palliative training for nurses is not a new phenomenon and many reputable organizations recognize this deficit in nursing education. The Institute of Medicine (IOM) recommends educational institutions should include palliative care education amongst clinicians in all disciplines of healthcare, particularly in nursing [2]. The American Association of Colleges of Nursing (AACN) and the American Nurses Association (ANA) have acknowledged the gaps in nursing programs and have called upon nursing academia and healthcare institutions to incorporate more vigorous training and education for both student and professional nurses alike [4].
There is evidence of some progress, with the development of the End-of-Life Nursing Education Consortium (ELNEC) and the Competencies and Recommendations for Educating undergraduate nursing Students (CARES) document. These tools offer learning modules and EOL clinical guidelines for undergraduate nursing programs [5]. However, many nurses currently in practice received their education prior to the development of these resources, and still lack the knowledge and expertise in EOL care. Further, despite the availability of the ELNEC and CARES recommendations, nursing students continue to report the limitation of palliative care instruction within their academic programs [2,4]. By incorporating evidence-based guidelines and expanding current curricula, nursing programs and healthcare institutions are capable of empowering nurses to provide high-quality and sensitive care and support the increasing demand for EOL patients.
Aims and Goals
This study examines the insights of undergraduate nursing students and professional nurses regarding their education and training for end-of-life patient care. The aim of the study is to determine if undergraduate nursing programs are incorporating EOL and palliative care into their curricula, thus preparing nurses to confidently provide EOL care. Our goal was to compare our findings with the current literature to determine if perceived inadequacies in nursing education and training are influencing the quality of palliative patient care. The findings of this study may support the need for undergraduate nursing programs to modify their curricula and incorporate more comprehensive EOL education in order to yield more competent nurses.
Nursing Theorist
Dr. Patricia Benner’s Novice to Expert theory provided a framework for this research. Benner’s theory [6] was developed based on the Dreyfus Model of Skill Acquisition and suggests that nursing competence is cultivated from a novice to expert capacity through continued clinical experiences and gained knowledge. The theory states that nurses acquire skills and confidence in a continuum of five stages: Novice, Advanced Beginner, Competent, Proficient, and Expert. Benner explains that the skills gained through actual experience and shared knowledge are essential to becoming an expert nurse [7].
The Novice nurse represents nursing students with limited or no clinical experience who rely on theoretical and abstract concepts to guide their clinical decision making. The Advance Beginner characterizes a new graduate nurse in their inaugural clinical role who is able to apply their academic foundations to make connections with concrete scenarios [8]. The Competent nurse has a few years of professional experience and demonstrates preliminary mastery in their skills and clinical decision making but may lack the speed and conviction of a more seasoned nurse. A Proficient nurse relies on their in-depth clinical experience to predict outcomes and exemplifies confidence and proficiency with clinical judgment to provide more holistic patient care [7,8]. An Expert nurse has cultivated the skills and knowledge through innumerous clinical experiences and no longer relies on guidelines to determine actions; but rather their clinical decision making has become innate and second nature to them [7]. They are experts in their field and provide confidence and proficiency in care. Thus, they are an invaluable resource of knowledge to their aspiring peers.
The Benner model suggests nursing proficiency is not something that is developed overnight, but rather is cultivated over time through foundational knowledge, shared wisdom from peers, and experiential learning. When applying Benner’s theory to end-of-life nursing, it is probable that a novice nurse would only have their academic background combined with any personal experiences with death as the foundation for their EOL understanding. However, research shows that veteran nurses feel inadequately prepared to provide quality palliative care, despite their clinical proficiency.
Review of the Literature
A comprehensive review of relevant nursing and healthcare literature was conducted to investigate nursing education and preparedness related to EOL and palliative care. The following keywords were utilized, both singularly and in combination: nursing education, end-of-life nursing care, nursing curriculum, nursing preparedness, end-of-life, and palliative care. The search included databases of CINAHL, PubMed, Google Scholar, and EBSCO through the Simmons University library. The search was limited from 2017 to present, including peer-reviewed publications printed in English to elicit relevant literature.
The World Health Organization (WHO) issued a directive that all individuals dying from life-limiting illnesses are entitled to quality care across a range of settings when approaching death (World Health Organization, 2021) [9]. Published reports by the National Hospice and Palliative Care Organization (2021) [10] noted 1.61 million Medicare beneficiaries were enrolled in hospice care for one day or more in 2019, nearly a 4% increase from the previous year. The global need for palliative care will continue to grow as a result of the aging population. The terms end-of-life (EOL), palliative care, and hospice are used interchangeably within the context of this paper.
It has been widely recognized that palliative care training for health professionals is limited or non-existent. Despite the obvious need for palliative and end-of-life care, the focus is often on improved EOL access for certain disease groups or on the development of hospice qualification guidelines. Although these are relevant aspects of palliative care, the lack of EOL nursing education still persists. Nonetheless, nurses who receive ample education in palliative care feel better equipped to care for their dying patients.
Since nurses spend more time with patients and families than any other health professional, the importance of proper end-of-life training is crucial [1,12]. Caring for palliative and hospice patients requires nurses to be well-prepared for multidimensional needs of the ailing patient and their family, including pain and symptom management, cultural considerations, and nonpharmacological needs [3]. Literature supports that few pre licensure nurse education programs have formal training focused on palliative and EOL care. Novice nurses reported they felt inadequately prepared to care for a dying patient based on their shortage of structured training [12].
Many themes were identified during the review of the literature. In addition to overall lack of education, additional barriers in providing quality EOL care were reported including nurses’ attitudes toward caring for the dying patient, poor communication, and limitation of necessary palliative clinical skills. Novice nurses reported they felt poorly prepared to care for a dying patient based on their insufficient EOL care training.
Limited Palliative Education in Curricula
The ability to incorporate EOL care into academic curricula presents a challenge amongst universities, as most nursing programs are saturated with content to begin with. However, when considering factors such as our aging and multimorbid population and the COVID-19 pandemic, the need for adequately trained nurses in EOL care is essential [11]. It is important to include this education early on and consistently within nursing curriculums. In order to implement changes, nursing programs must determine where the educational gaps exist before they can be corrected.
Four studies identified limited or lack of specific courses on palliative care within undergraduate programs. A cross-sectional study by Lippe et al. [13] evaluated the curriculum of baccalaureate nursing programs in the southern United States. The Context, Input, Process, and Product (CIPP) model was used as a method to evaluate this program. The curriculum consisted of 22 courses, though a formal course on palliative or end-of-life care was not included.
A multi-site feasibility study by Lippe [12] was conducted within three accredited nursing universities in an unnamed southern state. The End-of-Life Nursing Education Consortium (ELNEC) curriculum served as the standard of measurement of palliative content. Findings showed that although most of ELNEC’s content was covered within each program, faculty expertise or experience was limited, resulting in inadequately prepared students. This data supports an important point, that faculty preparation and knowledge can directly influence students’ learning outcomes.
A randomized control study of registered nurses from ambulatory and acute-care settings was conducted to further highlight that nursing curricula lack adequate palliative education. Less than 25% of participants reported they received palliative care education during their time in nursing school, and 45% of subjects did not receive any EOL care training in the previous two years [1].
Despite the efforts of The American Association of Colleges of Nursing (AACN) and ELNEC, it has been found that only 25% of nursing schools in the United States are utilizing student-based modules [11]. Content that has been created to provide palliative education to students and practicing nurses should be incorporated into curricula early on in an effort for nurses to be more comfortable and prepared when they are faced with caring for a terminally ill patient.
Nurse Attitudes and Perceptions Toward EOL Patients
Several articles examined nurses’ attitudes and perceptions towards caring for palliative and EOL patients, underscoring the need for enhanced palliative care education. Beckstrand et al. [14] used a quantitative descriptive survey of 104 ICU nurses to gather an understanding of obstacles faced during end-of-life care. The study found major barriers in providing care were directly related to miscommunication between physicians and nurses. Common themes included physician behavior, lack of resources, and insufficient EOL education. One nurse felt that “not being educated in EOL care, I found myself feeling left out---I didn’t know what to do.”
A quasi-experimental study by O’Shea and Mager [2] highlighted nurse attitudes toward EOL care. The researchers utilized the Palliative Care Quiz for Nursing (PCQN) to measure palliative care knowledge in 134 nurses from one county in Connecticut. The PCQN consists of 20 measurable items concerning palliative care, with a higher score correlating a greater knowledge of palliative care. Approximately 80% of nurses reported they had palliative experience and utilized palliative care methods in their work; yet mean pre-PCQN scores indicated this sample was lacking knowledge in the care they were providing. An intervention of a 6-week, 12-hour ELNEC educational program was implemented. After completion of the program, there was a significant improvement in post-PCQN scores.
Harrington et al. [15] conducted a quality improvement study in the U.S. that included 32 nurses from a dedicated palliative care unit. The study found that nurses' perceptions of caring exclusively for palliative patients resulted in emotional stress. The quality improvement project incorporated a three-step process to assess the benefit of the intervention, a series of seven palliative care workshops completed over one month. Pre workshop reflective activities were completed by nurses. Participants were asked to write a letter to loved ones as if they were a patient receiving palliative care. Nurses were able to discuss the emotional process in writing the letter but did not have to share what they wrote. They worked in small groups to discuss real-life case studies that focused primarily on the emotional component of caring for the dying patient. The Quality of Dying and Death (QODD) and Frommelt Attitudes Toward Care of the Dying (FATCOD) scales were used to measure the emotional experience. Post-intervention FATCOD scores were increased when compared with pre-intervention scores. Overall findings found the educational intervention improved attitudes and perceptions. Approximately 28% of nurses who participated reported they felt there is a valid need for increased training in palliative care.
The lack of palliative care knowledge in nursing is not unique to the United States. In India, a qualitative study was conducted to assess nursing students’ attitudes toward caring for dying patients. Of the 146 students in the study, only 39% of participants had a positive attitude toward caring for dying patients. A correlation was noted between students who had participated in palliative care during their clinical experience and improved perceptions toward dying patients [16]. The data is congruent with the findings of similar studies and reflects increased knowledge of palliative care results in improved nurse attitudes and higher quality EOL care for patients.
Communication
Palliative care must extend beyond clinical needs and include therapeutic communication with patients, caregivers, and the interprofessional team. The role of a nurse often involves having difficult and sensitive conversations with patients and families. When a nurse is faced with a challenging case and has little knowledge or experience on a matter, communication may be poor.
Broaching a palliative care conversation requires adequate knowledge of the subject. A study by Desanto-Madeya et al. [17] incorporated segments from the ELNEC model to address communication. Topics ranged from the difference between palliative care and hospice to addressing advanced directives. Knowledge was assessed by the means of the End-of-Life Professional Caregiver Survey (EPCS) and ELNEC training post-tests. Nurses who participated in this module noted the importance of assessing patient and family knowledge and feelings before initiating a conversation about EOL care. The implications of this study reflect that lack of communication training can result in a delay in palliative care.
Interventions and Training Modalities
To bridge the gap of knowledge concerning EOL care, several training modalities have been implemented across various settings. The End-of-Life Nursing Education Consortium curriculum has been adopted by many agencies. The goal of ELNEC is to provide evidence-based education initiatives to improve end-of-life care. The core curriculum includes eight didactic modules addressing pain and symptom management, and ethics. This curriculum has been used internationally and has proven to have successful outcomes for nurses.
EOL simulation modules have provided positive interactive learning experiences for nursing students. Carvalho et al. [4] conducted a qualitative descriptive study among junior and senior nursing students (n=32) which included live simulation scenarios and post-simulation reflections. Students reported the greatest knowledge was gained from participating in a live simulation and noted that emotions and discomfort were triggered during the virtual interaction. Students who participated were able to gain a better understanding of the role of the nurse in EOL care and how being prepared resulted in better patient outcomes.
A similar study by Byrne et al. [18] included 54 nursing students who participated in an EOL simulation combined with a lecture. The lecture incorporated modules from the ELNEC curriculum and focused on palliative care, caring for the dying patient, grief and loss, bereavement, and communication. A pre-course survey was conducted to gather perceptions of students before the educational component. The findings showed nurses felt unprepared when caring for a dying patient, specifically in an emotional manner. Students completed a post-intervention survey on their perceptions, and results were measured using a paired t-test. The findings showed a statistically significant difference between pre-test and post-test scores, suggesting that attitudes improved after incorporation of a formal palliative care training.
One study focused on the option for online training as a means of improving accessibility to EOL and palliative care education for students. Maznec et al. [19] implemented an ELNEC online curriculum to advanced practicing registered nursing (APRN) students. While this study focused on graduate level students, the results still support the convenience and value of online training interventions. The online ELNEC is available at a low cost, offering flexibility of remote learning and ensuring students can obtain palliative care education away from the traditional classroom setting. Overall findings from participants reflected a 95-100% satisfaction score when evaluating the online course. Content that was measured focused on the satisfaction of material relevance, ease of use, and clarity of the material. In addition to offering this intervention to students, this study initiated a faculty palliative care education development plan as well.
A large midwestern university piloted an elective palliative care class for nursing students, including 18 undergraduate and five graduate students. Before the start of the course, a survey was sent to all students to gather perceptions and comfort levels in caring for EOL patients. Toward the end of the 15-week class, students participated in a reflection paper and were asked to describe their learning experience. Results suggested an increased understanding of clinical skills, patient advocacy, and improved attitudes in caring for a patient as a result of their increased knowledge [20].
A qualitative study with a pragmatic approach explored the value of online training in improving health professionals’ capacity to provide end-of-life care. Authors Morgan et al. [21] conducted 30 semi-structured interviews with allied health professionals after completing three EOL essentials online modules. Several important themes emerged from the interviews: the information provided reinforced their current practice; the increased ability to recognize when the end of life is approaching; importance of strengthened interprofessional teamwork; and paradigm shifts in broaching EOL discussions. Although there is a need to integrate EOL care in academic curricula, this study reinforces that EOL education is still lacking even for experienced health care workers.
This extensive review of literature supports the notion that limited palliative and EOL education in nursing curriculums is a lead reason why novice nurses are inadequately prepared to provide quality care to dying patients. The literature reviewed illustrates that incorporating formal palliative care and EOL education into nursing curricula will enhance nurses’ attitudes toward caring for this population and ultimately improve patient care outcomes.
Methodology
The study utilized a mixed blend of qualitative data and focus group interviews to gain a better understanding of student and professional nurses’ competence and attitudes towards caring for EOL patients. Institutional review board approval, as well as endorsement from nurse management and university leadership, were respectfully obtained prior to recruitment of participants (see Appendix A). All subjects volunteered and provided informed consent to participate in the study. This mixed methodology allowed researchers to ascertain a better understanding of educational needs and potential barriers for nurses providing EOL care. Professional nurses from three diverse medical units in a Boston hospital were surveyed to appraise their experiences with palliative care. While baccalaureate nursing students from a Boston university were interviewed to capture the student perspective on how their current curriculum was preparing them to provide EOL care in their future nursing roles.
These two sample populations were intended to represent nurses from novice to expert competence, providing a broad spectrum of proficiency and education in EOL care. Professional nurses completed an electronic survey, incorporating four demographic questions, an abbreviated version of the End-of-Life Professional Caregiver Survey (EPCS), and three open-ended questions to elicit insight on providing palliative and EOL patient care (see Appendix B). The EPCS survey incorporates the eight domains of the national palliative care guidelines and has been proven to be psychometrically valid as a scale to evaluate EOL and palliative care educational needs among healthcare professionals [22]. The student nurse population was recruited from a mixed cohort of nursing students, with seven students volunteering for final interviews. Audio-only interviews were recorded via Zoom with consent from participants, omitting identifying information to eliminate bias and maintain confidentiality. Researchers asked participants an identical set of open-ended questions to elicit responses related to their personal and professional EOL experience and their nursing curriculum (see Appendix C). All data collected for this study has been securely locked and stored for up to three years in the lead researcher’s possession.
Data Analysis
The professional nurse survey was emailed via hospital distribution lists to all nurses on the preassigned units, allowing three weeks for submission of responses. The institution’s REDCap software was utilized to capture the data and results were exported to SPSS for coding and statistical analysis. Descriptive analytics from the demographic and modified EPCS contents of the survey were coded for frequency distribution. Open-ended responses were read and re-read by the researchers and coded for common paradigms and phenomena that emerged within the context of the statements. Student focus group interviews were transcribed verbatim from the audio recordings. Transcripts were read multiple times and coded by the research team, identifying commonly stated phrases, and extracting thematic content for descriptive analysis of the data.
Results
Professional Nurse Demographics
Thirty-six professional nurses from the selected units submitted the electronic survey, with 33 completed in its entirety. The majority of nurses were between the ages of 18-34 years old (66.6%) and the remainder over the age of 35. All but one nurse had a bachelor’s degree in nursing (n=35), with the other having an associate degree (n=1). The years of experience varied widely, with the majority of respondents having 1-3 years (33.3%) or more than 10 years (38.9%) of professional nursing experience (see Table 1).
With regards to EOL and palliative care education and training, 20 nurses reported having had a course or lecture as part of their nursing curriculum; seven completed an online EOL course at some point, seven reported having formal training as part of their job, and seven completed a continuing education (CE) course on EOL or palliative care. In contrast, nine nurses reported they never received any formal education or training on EOL or palliative care (see Table 2).
Confidence in Providing EOL Care
Nurses were asked to rate their confidence and comfort levels in various aspects of providing EOL care to patients, using a modified End-of-life Professional Caregivers Survey (EPCS). Two thirds of nurses reported feeling “quite a bit” (48.5%) or “very much” (18.2%) comfortable talking to patients and families about personal choice and self-determination. While more than half felt comfortable discussing code status (“not at all” (6.1%), “a little bit” (24.2%) or “somewhat” (24.2%)). The majority of nurses reported they were able to recognize impending death in patients (56.3% “quite a bit”; 34.4% “very much”) and know how to use non-drug therapies to manage patient symptoms (45.5% “quite a bit”; 18.2% “very much”). More than half of the nurses surveyed were only “somewhat” (36.4%) or less familiar with palliative care principals and national guidelines (6.1% “not at all”; 15.2% “a little bit”). A comprehensive analysis of the EPCS findings is detailed in Table 3.
Nurse Perceptions and Barriers
Professional nurses were asked two open-ended questions to elicit their opinions on EOL care-giving from a professional standpoint, with 26 nurses (72%) providing responses. The first question inquired how their education and training has prepared them to provide quality end-of-life care for patients and families. From the 26 unique responses, four significant themes emerged. Seven nurses referenced having lectures, preceptorships and/or simulation training as part of their undergraduate nursing curriculum. Eight nurses alleged the content for EOL education provided in nursing school as inadequate and limited. Thirteen nurses stated they gained the most EOL and palliative training from their peers and through their own personal patient care experiences. While three nurses mentioned having received formal training through hospital in-services and online modules at their place of employment.
The second question asked what the biggest challenges or barriers nurses experience are when providing end-of-life or palliative care to patients. Eight themes emerged from data: (1) ineffective communication among patient care teams (n=7), (2) disagreement between patient wishes and plan of care (n=7), (3) not keeping the dying patient comfortable/ineffective comfort measures (n=6), (4) family disagreements regarding patient wishes (n=8), (5) cultural barriers (n=2), (6) delayed initiation of palliative care or advanced care planning (n=8), (7) lack of support for grieving families (n=4), and (8) lack of support for the health care team (n=2). A frequency analysis of these themes in relation to years of nursing experience can be further examined in Table 4.
The final survey question asked nurses if their institution were to offer a formal educational program or training on end-of-life care, would they be interested in this training; 30 responded “yes,” while only one person responded “no.”
Student Nurse Perceptions
Baccalaureate student nurses were recruited from a nursing elective course, and 20 students initially expressed interest in participating in the focus group interviews. From this cohort, eight students provided written consent to volunteer and seven students ultimately participated in the individual interviews. The sample included five first-year students and two second-year students. The second-year students (n=2) reported having started some clinical hours through their nursing curriculum, while the remaining students (n=5) had no clinical or direct patient care experience at the time of interviews. None of the students had received any lectures or coursework as part of their nursing curriculum directly related to EOL patient care. However, three students reported having some element of death and dying referenced in non-nursing electives, including ethics and philosophy courses. Four students reported having personal EOL experiences with family or loved ones. Upon reviewing the transcripts from interviews, five major themes emerged from the student interviews: (1) the expectation that their nursing school curriculum and clinical experiences would include EOL context, (2) the importance of family involvement in EOL patient care, (3) the fear of feeling unprepared to care for dying patients, (4) the importance of sensitive communication with dying patients and their families, and (5) the importance of nursing presence to provide support for palliative patients and families (Figure 1).
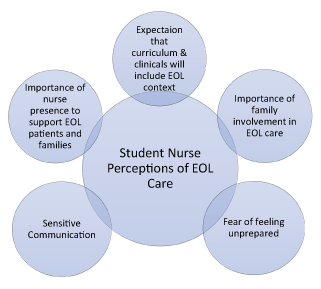
Figure 1: Thematic Analysis from student interviews
Limitations
Interpretation of the results was performed with mindful consideration of internal and external validity factors, avoiding bias or conflict of interest from the research team. A rigorous analyzation of the data supports the aim of the study, investigating if academic institutions are adequately incorporating palliative and EOL patient care into the curriculum. Both sample groups voluntarily participated and provided informed consent, and all responses remained anonymous through data collection. Convenience sampling for both populations limited our findings to potential bias. The professional nurses surveys were distributed on three hospital units with critically ill patients, potentially narrowing the variety of professional nurse representation. Future research would benefit from including nurses from various specialties to diversify professional nurse perspectives. A second limitation is small sample size. While we met our goal for number of participants from both populations, larger samples would help to achieve data saturation. A third limitation was the level of education from the nursing students. The majority of the students were first-year students with limited nursing classes and/or clinical exposure to patient care. Thus, student perceptions and outcomes may lack representative data. Future focus groups with third and fourth-year nursing students would add valuable student insight to this research.
Discussion
The goal of our research was to investigate if undergraduate nursing programs are preparing future nurses to confidently provide EOL care to patients and their families. Themes that emerged from the representative populations of student and professional nurses assert the current literature that nurses desire more robust EOL and palliative care education, specifically as part of their undergraduate studies. Responses from the nursing students suggest there is an expectation that they will receive both didactic and clinical training in EOL care prior to graduating. Yet the professional nurses surveyed implied the EOL education provided in nursing school is superficial and limited, lacking practical preparation for real-life patient care. One nurse stated, “I feel there is a gap in knowledge about caring for the dying patient in a bachelors program.” Previous research from Bishop et al. (2019) supports this inadequacy in nursing programs. Their study found that only a quarter of their subjects received comprehensive palliative care education during their time in nursing school, and nearly half did not receive any EOL care training as part of their undergrad program.
During student interviews, undergraduates expressed a fear of feeling unprepared to care for palliative patients. A study by Stokman et al. [11] endorses that when novice nurses receive formalized end-of-life and palliative training, they enter the workforce with a sense of confidence, knowledge, and skills, providing improved attitudes and perceptions towards EOL patient care. Our data showed nurses with three years or less of professional experience mentioned having some degree of EOL education while in school that helped them to feel more confident in caring for dying patients. One nurse stated, “Because of the experiences I had in nursing school, I have felt more comfortable caring for [palliative] patients as a nurse, and I feel as though these experiences have helped me provide better quality end-of-life care.” Meanwhile, five nurses with ten or more years of experience reported inadequate or nonexistent EOL education in their previous nursing studies. Perhaps this insight from newer nurses points to a promising paradigm shift that nursing programs are beginning to include more EOL training in their curriculum.
The nurses in our study emphasized that the majority of palliative and EOL knowledge is gained from professional or personal experience, rather than classroom curriculum. Thirteen of the nurses surveyed (36%) stated their palliative knowledge came “at the hand of my peers” and from on-the-job patient care experience, while only six nurses (16%) commented on having formalized training. Previous studies have found that more structured training in palliative care improved nurses perceptions and attitudes when caring for dying patients, resulting in better quality care for patients (Beckstrand et al., 2021; Harrington et al., 2021; O’Shea & Mager, 2019; Paul et al., 2019). Our findings suggest that nurses are confident in the physiological aspects and are comfortable being present with dying patients. However, the data indicates that nurses lack confidence in the cultural, ethical, and emotional needs of palliative patients and their families. Nurses may be well-versed in providing medical management for dying patients, yet they lack the confidence when providing the psychological side of palliative care. Formal education that addressed these unique and individualized needs of dying patients would enable nurses with knowledge and confidence when providing these sensitive yet predominant aspects of palliative care.
The importance of communication resonates in both the current literature and the findings from our study. Student nurses cited their desire to learn sensitive communication when dealing with dying patients and family members. Professional nurses in our study found poor communication to be a significant barrier to quality EOL care. Specifically, nurses mentioned the delay in discussing advanced care plans, misinterpretation of patient wishes between the patient and family members, and overall miscommunication between the healthcare team to be the prevalent barriers in EOL patient care. Desanto-Madeya et al. [17] published a quality-improvement study where nurses completed modules of the ELNEC focused on effective communication. Following the intervention, nurses reported improved confidence when approaching advanced care planning discussions and improved knowledge in sensitive patient communication. This highlights the value of end-of-life care training for nurses that promotes compassionate communication, the need for timely advanced care planning, and open discussion among patients, families, and the healthcare team.
While many of the nurses in this study have indicated their palliative care training to be mainly driven from patient care experience, 97% reported they would be interested in formal EOL and palliative care training if offered by their institution. Student nurses voiced the expectation that their undergraduate studies will enable them to care for palliative patients at a novice level. The desire to learn is there. Academic and medical institutions are tasked to provide learning opportunities for both student and professional nurses alike to promote confident end-of-life patient care.
Nursing Implications
Themes that emerged from this study validate nurses’ longstanding feeling that they have been denied adequate EOL and palliative training. While first-hand patient experience is immeasurable, there is an obligation for professional development that falls in the hands of both academic and healthcare organizations. The End-of-Life Nursing Education Consortium (ELNEC) modules, the Competencies and Recommendations for Educating undergraduate nursing Students (CARES) document, and simulation labs are options available for instruction. These programs have proven successful in studies and offer a variety of accessibility in-person and online, without institutions having to reinvent the wheel. Future studies would benefit from including student perspectives from all academic levels, including graduate-level nurses. It would be valuable to research what strategies nursing programs have utilized to successfully incorporated EOL care into their curriculum.
End-of-life nursing education should embrace advanced practice nurses as well. Advanced practice registered nurses (APRNs) can play a unique and valuable role in end-of-life patient care. As the data showed, ineffective communication contributes to poor coordination among the multidisciplinary team, misinterpretation of patient wishes between family members, and delayed initiation of palliative care. APRNs can facilitate improved communication and act as a liaison between the patient, family members, and care team. They can initiate advanced care planning discussions with terminally ill patients and advocate for patients’ self-determination and care preferences to disagreeing family members. APRNs can also support staff nurses by providing continued EOL education, ultimately leading to improved quality palliative care.
Conclusion
Nurses are at the helm of providing quality end-of-life and palliative care to patients. Yet they have historically relied on on-the-job and empirical training to acquire the necessary skills for compassionate EOL care. Our research, compared with the most recent literature, shows that gaps still exist in undergraduate nursing curriculums. Institutions are not offering formal training or education, which may be impacting current practicing nurses in their EOL proficiency. The findings of this study support the need for undergraduate nursing programs to modify their curriculum to incorporate more comprehensive EOL education in order to cultivate competent nurses. Further, medical organizations must offer continued education to practicing nurses to meet the growing demands on our healthcare systems for quality end-of-life and palliative patient care.
References
- Bishop CT, Mazanec P, Bullington J, Craven H, Dunkerley M, et al. (2019) Online end-of-life nursing education consortium core curriculum for staff nurses: An education strategy to improve clinical practice. Journal of Hospice and Palliative Nursing. 21(6), 531–539. [Crossref]
- O’Shea ER, Mager D (2019) End-of-life nursing education: Enhancing nurse knowledge and attitudes. Appl Nurs Res 50: 151197. [Crossref]
- Manning J, Creel A, Jones N (2020) Effectiveness of an end-of-life nursing education consortium training on registered nurses’ educational needs in providing palliative and end-of-life patient care. J Hospice Palliat Nurs 23:1 [Crossref]
- Carvalho LG, Hamilton HM, Burke ME, McDonald C, Griggs S (2020) End-of-life nursing knowledge among nursing students. Journal of Nursing Education 59: 154. [Crossref]
- Ferrell B, Malloy P, Mazanec P, Virani R (2016) CARES: AACN’s new competencies and recommendations for educating undergraduate nursing students to improve palliative care. J Prof Nurs 32: 327–333. [Crossref]
- Benner P (1982) From novice to expert. American Journal of Nursing, 82(3), 402-407. [Crossref]
- Petiprin A (2020) From novice to expert. Nursing Theory. https://nursing-theory.org/theories-and-models/from-novice-to-expert.php
- Mennella H, Schub T (2021) Benner’s model of professional advancement. CINAHL Nursing Guide.
- World Health Organization (2021) Implementing world health assembly resolution on palliative care. https://www.who.int/news/item/12-10-2021-implementing-world-health-assembly-resolution-on-palliative-care
- National Hospice and Palliative Care Organization (2021) NHPCO facts and figures: 2021 edition. https://www.nhpco.org/hospice-facts-figures/ https://www.nhpco.org/hospice-facts-figures/
- Stokman AI, Brown SL, Seacrist MJ (2021) Baccalaureate nursing students’ engagement with end-of-life curriculum: A grounded theory study. Nurs Educ Today, 102: 104914. [Crossref]
- Lippe M (2019) Assessment of primary palliative care content within prelicensure nursing education: A multisite feasibility study. J Hosp Palliat Nurs 21: 373–381. [Crossref]
- Lippe M, Volker D, Jones T, Carter P (2017) Evaluating end-of-life care education within nursing programs: A method for targeted curriculum evaluation. J Hospice Palliat Nurs 19: 266–274.
- Beckstrand RL, Willmore EE, Macintosh JLB, Luthy KEB (2021) Critical care nurses’ qualitative reports of experiences with physician behaviors, nursing issues, and other obstacles in end-of-life care. Dimensions of Critical Care Nursing 40: 237–247. [Crossref]
- Harrington KJ, Affronti ML, Schneider SM, Razzak AR, Smith TJ (2019) Improving attitudes and perceptions about end-of-life nursing on a hospital-based palliative care unit. J Hosp Palliat Nurs 21: 272–279. [Crossref]
- Paul S, Renu G, Thampi P (2019) Creating a positive attitude toward dying patients among nursing students: Is the current curriculum adequate? Indian Journal of Palliative Care, 25: 142–146. [Crossref]
- DeSanto-Madeya S, Darcy AMG, Barsamian J, Anderson A, Sullivan L (2020) An innovative application of end-of-life nursing education consortium curriculum to increase clinical nurses’ palliative care knowledge. J Hosp Palliat Nurs 22: 377–382. [Crossref]
- Byrne D, Overbaugh K, Czekanski K, Wilby M, Blumenfeld S, Laske RA (2020) Assessing undergraduate nursing students’ attitudes toward the dying in an end-of-life simulation using an ACE.S unfolding case study. Journal of Hospice & Palliative Nursing, 22: 123–129.
- Mazanec P, Ferrell B, Malloy P, Virani R, Cormack C (2021) Preparing advanced practice registered nursing students to provide primary palliative care. Nurse Educator, 46: 221–224. [Crossref]
- Mason H, Burgermeister D, Harden K, Price D, Roth R (2020) A multimodality approach to learning. J Hospice Palliat Nurs 22: 82–89.
- Morgan DD, Litster C, Winsall M, Devery K, Rawlings D (2021) “It’s given me confidence”: A pragmatic qualitative evaluation exploring the perceived benefits of online end‐of‐life education on clinical care. BMC Palliative Care 20. [Crosserf]
- Lazenby M, Ercolano E, Schulman-Green D, McCorkle R (2012) Validity of the End-of-Life Professional Caregiver survey to assess for multidisciplinary educational needs. J Palliat Med 4: 427-431. [Crossref]

