Abstract
Case report: Patients with Klippel-Trenaunay syndrome develop degenerative joint disease early due to abnormal bone hypertrophy. For various reasons, total knee arthroplasty is particularly challenging for these patients. This is a case report of an arthritic patient with Klippel-Trenaunay syndrome who had total knee arthroplasty.
Conclusion: For patients with Klippel-Trenaunay syndrome, total knee arthroplasty is an effective surgical procedure to treat arthritis. However, some risks must be considered, and appropriate surgical preparation must be undertaken.
Keywords
Klippel-Trenaunay syndrome, TKA, SMA
Introduction
Klippele-Trenaunay Weber Syndrome (KTWS) is a rare congenital disorder characterized by wine staining, varicose veins, bone hypertrophy, and soft tissue hyperplasia [1]. KT syndrome usually occurs at birth, early infancy or childhood. The rarity of disease makes it difficult to calculate its incidence rate. However, few studies report the incidence rate of 2-5 cases per 100 thousand [2,3]. Furthermore, evidence demonstrates that KTWS is more prevalent among males compared to females [3].
KTWS most often occurs at birth and childhood, about 95% of patients with KTWS have limb hypertrophy. Bone and soft tissue hypertrophy can cause various symptoms, such as uneven limb length, secondary pelvic tilt, joint contracture, and so forth. Asymmetry in the lower limbs and abnormal bone growth leads to knee osteoarthropathy.
One of the rarest forms of severe arthritis involves a unilateral lower extremity vascular malformation combined with the ipsilateral knee joint. In this case, total knee arthroplasty (TKA) is full of risks. Baskervillev [4] reported that 16% of KTWS patients developed deep venous thromboembolisum (VTE), and 14% of them developed pulmonary emboli. There is a risk of uncontrolled bleeding in Klippel-Trenaunay syndrome; therefore, standard practice does not recommend orthopaedic surgery.
The patient, in this case, suffers from infantile spinal muscular atrophy (SMA). Patients with SMA are usually accompanied by muscle contracture and limited activity caused by muscle weakness, resulting in increased pain, osteoporosis, and limb fracture, which significantly complicates surgery and prognosis.
Based on a literature review, limited arthroplasty cases in KTWS are available. So far, two cases involving the knee and one case involving the hip have been reported [5-7]. The patient knows and consents that case data can be published.
Case report
An elderly male aged 67, was admitted to the hospital for chronic pain in his left knee. An outpatient physical examination reveals a significantly thicker left lower limb accompanied by multiple varicose veins. The right lower limb was 2 cm short on the opposite side, and the right foot was stunted with high arch deformity. The entire body was covered in a red grape globus, which faded after pressing (Figure 1).
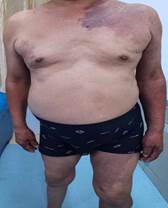
Figure 1a
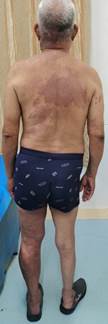
Figure 1b
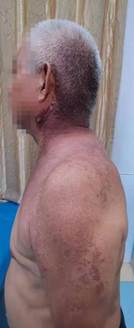
Figure 1c
Figure 1: The patient's physical examination before operation showed a large area of wine stains on the left shoulder, back and inner thigh of the affected limb
Further examination reveals that the straightening angle of the left knee was only 20°, but the flexion angle can reach 100°. The right knee joint can be improved in terms of its functional ability. Extensor dorsalis muscle strength V of the left lower extremity was normal. The extensor dorsalis muscle strength IV of the right lower limb, the pulse of the dorsalis pedis artery of both lower limbs was good, and the ends of both lower limbs can feel, blood supply and activity. Radiological examination of the left knee shows severe degenerative osteoarthritis and hypertrophic square femoral condyle and subchondral bone sclerosis (Figure 2). The preoperative coagulation index was high: plasma-d dimer: 0.63 µg/mL, plasma fibrinogen determination: 6.68 g/L, ESR: 81 mm/hr. Following consideration of the severe bleeding tendency of KT syndrome and the possibility of venous thrombosis, peripheral vascular doctors were consulted, and allogeneic blood 3U was arranged.
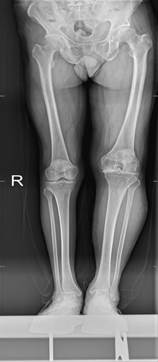
Figure 2: Preoperative X-ray showed severe degenerative osteoarthritis of the left knee, with hypertrophic and square femoral condyle and subchondral bone sclerosis
The operation was performed under combined spinal anaesthesia. A tourniquet was used during the procedure. Hemangiomas were visible during the operation, but the hemostatic effect was achieved. Synovium hyperplasia and edema were dark red, while the articular cartilage was orange. A German link bone cement prosthesis was implanted successively, followed by patella denervation. The tourniquet was used for 80 min, and intravenous injections of tranexamic acid were administered 30 min before the operation, before prosthesis implantation, and after suturing for joint cavity perfusion. Next, the drainage tube was placed, and approximately 600 mL of the drain was collected. After 24 h, the drainage tube was removed.
The patient's postoperative course was uncomplicated since there were no apparent signs of anemia and the patient did not require blood transfusions. Moreover, low molecular weight heparin was administered postoperatively to prevent venous thrombosis.
The patient began continuous passive exercise on day two and started walking using a walker. In addition, the patient was instructed to use an intermittent air pump device to prevent venous thrombosis and perform ankle pump exercises.
Ultrasonography of both lower limbs was performed five days after surgery, and no signs and symptoms of DVT were found. On the same day, the ROM was 0° - 90° and his wound healed well.
A year later, the patient reports a significant reduction in knee pain during follow up examination. In addition, the patient was able to walk normally and had found a job. Furthermore, the patient was able to travel by congested bus without external support. The patient expressed satisfaction with the postoperative outcomes (Figure 3).
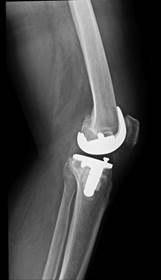
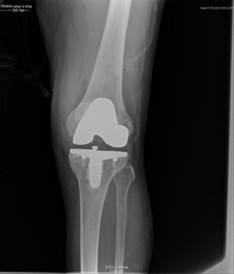
Figure 3a Figure 3b
Figure 3: One year later, X-ray showed that the prosthesis was in good position
On pathological examination, the bone and synovial tissue removed during the operation were replaced by vascular hyperplasia with lymphoplasmacyte exudates. Pathological examination further reveals a visible vascular mass with iron phagocytosis, which corresponds with the examination results of hemangiomas in Klippel-Trenaunay Weber syndrome [6].
Discussion
In patients with KT syndrome, it is difficult to perform a total knee arthroplasty because abnormal bone growth and blood vessels in the affected limb pose a risk of uncontrollable bleeding. However, the only treatment for osteoarthritis caused by KT syndrome is joint replacement.
Patients with KT syndrome have been reported to have a high risk of postoperative complications, wound complications, cardiovascular complications, and infection. In these cases, bleeding and embolism are likely to occur without adequate preoperative preparation. Therefore, a multidisciplinary consultation is necessary prior to an operation to assess its risk. However, we encountered varicose veins and vascular masses during surgery, which were burned to stop bleeding. Although the patient did not receive a postoperative blood transfusion, it is necessary to prepare allogeneic blood before the operation.
Catreetal [6] pointed out that tourniquets are useful to avoid massive bleeding during knee surgery. However, they also encountered varices and hemangiomas during the operation.
For patients with this vascular malformation undergoing joint replacement, we want to suggest the following:
1) Appropriate vascular research should be carried out prior to surgery to determine the severity of the vascular malformation.
2) If venous embolism is detected before surgery, multidisciplinary consultation is necessary, particularly with vascular surgeons.
3) As patients with KT syndrome have a severe bleeding tendency, a sufficient amount of allogeneic blood must be prepared before the operation to avoid massive bleeding.
4) Tranexamic acid should be administered during the perioperative period to reduce bleeding, and anticoagulant activity should be monitored to prevent deep vein thrombosis.
In addition, special care must be taken to ensure sterility since these patients are more vulnerable to infections. Furthermore, long-term monitoring is necessary because the progression is unpredictable. Apparently, the other side of the patient's body had weak muscles. Hence, postoperative rehabilitation exercises are essential for the follow-up to overcome muscle weakness.
Conclusion
Few studies have been conducted on joint replacement techniques in patients with KT syndrome. Due to abnormal bone hypertrophy and vascular malformation, it is risky to operate on people with KT syndrome. In this case report, we hope to provide some reference to prepare patients with KT syndrome for surgery.
Ethics statement
The studies involving human participants were reviewed and approved by research ethics committee of Department of Orthopaedics Affiliated Hospital of Shandong University of traditional Chinese Medicine. The patients/participants provided their written informed consent to participate in this study.
Author contributions
LJX designed the study. LJX and XX interpreted the data and drafted the article. YW and LJS and ZJ revised the manuscript critically and accounted for all aspects of the work.All the authors contributed equally to this manuscript.
Funding
This study was funded by a grant from the Provincal Science Foundation of China (ZR2021QH229)
Competing interests:None
References
- Asghar F, Aqeel R, Farooque U, Haq A, Taimur M (2020) Presentation and Management of Klippel-Trenaunay Syndrome: A Review of Available Data. Cureus 12: e8023. [Crossref]
- Lee A, Driscoll D, Gloviczki P, Clay R, Shaughnessy W, et al. (2005) Evaluation and management of pain in patients with Klippel-Trenaunay syndrome: a review. Pediatrics 115: 744-749. [Crossref]
- Purkait R, Samanta T, Sinhamahapatra T, Chatterjee M (2011) Overlap of sturge-weber syndrome and klippel-trenaunay syndrome. Indian J Dermatol 56: 755-757. [Crossref]
- Baskerville PA (1987) Maladie thrombo-embolique et anomalies veineuses congénitales [Thromboembolic disease and congenital venous abnormalities]. Phlebologie 40: 531-536. [Crossref]
- Letts RM (1977) Orthopaedic treatment of hemangiomatous hypertrophy of the lower extremity. J Bone Joint Surg Am 59: 777-783. [Crossref]
- Catre MG, Kolin A, Waddell JP (2005) Total knee arthroplasty in Klippel-Trenaunay syndrome. Can J Surg 48: 494-495. [Crossref]
- Willis-Owen CA, Cobb JP (2008) Total hip arthroplasty in Klippel-Trenaunay syndrome. Ann R Coll Surg Engl 90: W6-W8. [Crossref]






